Abstract
Background. Currently, the only effective method to control the spread of the COVID-19 pandemic is social distancing. The lockdown measures during the epidemic may have an impact on the presentation of diabetes and may disturb metabolic control.
Objectives. In order to address the hypothesis that the COVID-19 lockdown affected the incidence rate (IR) of type 1 diabetes (T1D) in the pediatric population of Lower Silesia and the patients’ clinical status, the incidence of T1D during the COVID-19 pandemic was analyzed.
Material and methods. Incidence estimates were obtained from the T1D pediatric registry for Lower Silesia which has been maintained since January 1, 2000. The observation was completed on April 30, 2020.
Results. A total of 1961 cases were diagnosed (1054 boys, 53.72%). An increase in the T1D IR was observed, from 10.43/100,000/year in 2000 to 22.06/100,000/year in 2019. The seasonality of T1D incidence was also observed, with the highest IR appearing in January and February. There were half as many cases of T1D in March and April 2020 as in the same months in 2019 (p > 0.05). Diabetic ketoacidosis (DKA) occurred in 31.75% of patients in years 2000-2019, comparably (p > 0.05) to 2020 (36.67% patients), including March and April (50% of patients). The duration of hyperglycemia symptoms was 20.2 ±25.4 days, which was comparable to 2020 (13.1 ±10.96 days; p = 0.1675) and March and April of 2020 (9.67 ±5.63 days; p = 0.0831). Glycated hemoglobin (HbA1c) level was 11.79 ±2.63%, which was comparable to March and April of 2020 (13.06 ±2.35%; p = 0.1171), while in all of 2020 it was 13.41 ±2.50% (p = 0.0003).
Conclusions. The IR of T1D in Lower Silesian children in the months of the COVID-19 pandemic was comparable to previous years, while their clinical condition at the time of diagnosis was worse than in previous years.
Key words: type 1 diabetes, COVID-19 pandemic, incidence rate
Background
Spread by droplet transmission, severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) causes respiratory coronavirus disease (COVID-19). The first reports of SARS-CoV-2 viral infections in the Chinese province of Hubei appeared in the last months of 2019. The high infectivity of this pathogen caused a rapid spread of the COVID-19 disease and an unprecedented outbreak, first in many cities of China and then globally. On January 30, 2020, the World Health Organization (WHO) announced a global health emergency; on March 11, 2020 it was declared a pandemic.
The classic clinical symptoms of COVID-19, in addition to high fever and flu-like symptoms (including muscle pain), relate to the respiratory tract and include fatigue, dry cough, severe interstitial pneumonia, and acute respiratory distress syndrome (ARDS), often requiring the use of respiratory support with mechanical ventilation. Disorders of smell and taste, gastrointestinal symptoms (diarrhea) and neurological symptoms (headache, disturbance of consciousness, and confusion) have also been reported. In severe cases, SARS-CoV-2 infection can cause complications such as renal and circulatory failure. On the other hand, asymptomatic infections seem to be quite common (up to 80% of cases).1 The risk of a serious course of the disease applies primarily to the elderly and to those with comorbidities, including diabetes.
Because SARS-CoV-2 is a new virus for humanity, only those who have suffered COVID-19 now have adaptive immunity against this coronavirus. It can therefore be concluded that all humanity is susceptible to infection. Since it is a new pathogen, vaccination against it is still unavailable. Unfortunately, there is also no causal treatment.
The reproduction ratio (R0) of this virus is estimated to be between 2 and 3, which means that every patient with COVID-19 infects 2 to 3 people on average, and that the number of affected people therefore doubles every week.2 Currently, the only effective method of controlling the spread of the COVID-19 epidemic is social distancing. Therefore, governments of many countries, including Poland, decided to close borders, limit travel and introduce quarantine for people returning from abroad. Large gatherings – cultural, sport and religious events – were cancelled. Schools and universities were closed, which affected more than 90% of students globally.3
Medical facilities proved to be critical places for the development of the epidemic, and the protection of medical personnel against infection is a priority. Access to medical care has become limited, not only because of the cancellation of planned services, but also because of the closure of health centers due to diagnoses of COVID-19 among staff and/or patients of wards beyond those dedicated to treating the infection. In addition, even in urgent situations, patients delay contacting healthcare providers, as they are afraid of being infected with SARS-CoV-2.
Objectives
With this in mind, the aim of the research was to determine whether the restrictions introduced due to the SARS-CoV-2 epidemic have affected the incidence of type 1 diabetes (T1D) in the pediatric population of Lower Silesia (a region in southwest Poland) or the clinical status of children and adolescents hospitalized because of newly diagnosed T1D.
Material and methods
The incidence of T1D and the clinical status of children and adolescents with T1D diagnosed in the first 4 months of 2020 were compared to historical data. The analysis covered a reference period from January 1, 2000 to December 31, 2019, and an examined period from January 1, 2020 to April 30, 2020. All new cases of T1D in children aged 0–18 years were recorded. All patients were treated in the same reference Center for Pediatric Endocrinology and Diabetology for Lower Silesia. The diagnoses of diabetes were made based on the WHO criteria, with the date of onset defined as the day of the first insulin administration.4 The incidence rate (IR) was expressed as the number of new cases of T1D per 100,000 people in the general population of a given age group per year. The demographic data was obtained from the Statistical Yearbooks of the Lower Silesian Voivodeship. For the years 2019 and 2020, demographic data from 2018 was used because the statistical data had not been updated yet. The IR was assessed for each year and for individual months of the year.
In addition, the clinical status of children with T1D at the time of diagnosis was analyzed by assessing the presence of diabetic ketoacidosis (DKA) and pH at presentation, the duration of hyperglycemia symptoms before the diagnosis of diabetes, and the glycated hemoglobin (HbA1c) level. Diabetic ketoacidosis was diagnosed according to International Society for Pediatric and Adolescent Diabetes (ISPAD) recommendations.5
The statistical measures presented herein are the arithmetic mean (M) and standard deviation (SD). The distribution of the quantitative variables in the analyzed sample was compared with the normal distribution using the Shapiro–Wilk test. When the distribution of the compared samples did not differ significantly from the normal distribution with statistically equal variance, Student’s t-test was used to assess the differences. When the assumptions required for Student’s t-test were not met, the Mann–Whitney U test was used. A comparison of the frequencies between groups was performed using the χ2 test. In the case of small sample sizes (i.e., a total <20 or a total <40 and the smallest sample <5), Yates’s correction or Fisher’s exact test were applied. In all statistical tests, a significance level of α = 0.05 was assumed.
Results
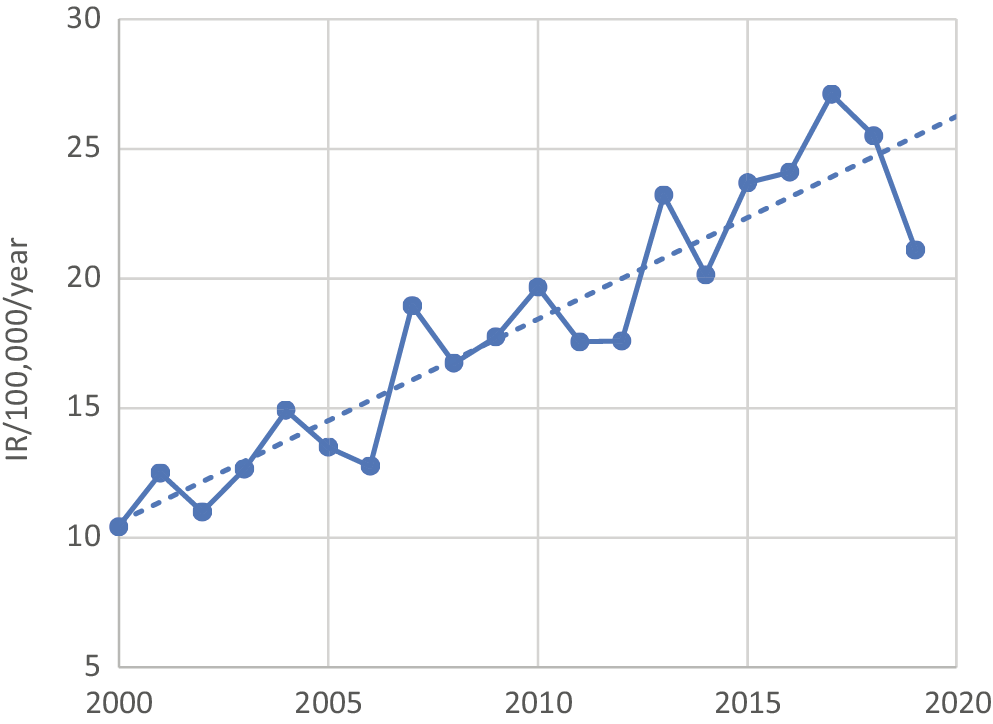
In the period 2000–2019 in Lower Silesia, T1D was diagnosed in 1961 children and adolescents, including 1054 boys (53.72%). The overall IR in the study period was 17.51/100,000/year. An increase in the IR was observed – from 10.43/100,000/year in 2000 to 22.06/100,000/year in 2019, with a peak in 2017 (27.10/100,000/year) (Table 1, Figure 1).
Due to the lack of statistically significant differences between IRs in five-year intervals (Table 1), further analyses were carried out jointly for individual intervals (period I – 2000–2004, period II – 2005–2009, period III – 2010–2014, and period IV – 2015–2019). It should be noted that the IR for T1D in from 2015 to 2019 was twice as high as from 2000 to 2005. The forecast of the IR for T1D in 2020, based on the IR in the first 4 months, is 17.27/100,000/year, which is significantly lower (p = 0.0016) than the IR in the previous period (2014–2019), but comparable to the IR in 2019 (p = 0.0808).
From 2000 to 2019, the IR of T1D among boys (M) was higher than among girls (F) (M: 18.60/100,000/year, F: 16.40/100,000/year; p = 0.0053); however, this result was influenced by the significant difference in the IRs for the period 2010–2014 (M: 21.26/100,000/year; F: 16.27/100,000/year; p = 0.0031), because in the remaining period, the IR for both sexes was comparable. Also, in 2020, the T1D IR was comparable for both sexes (p = 0.5506).
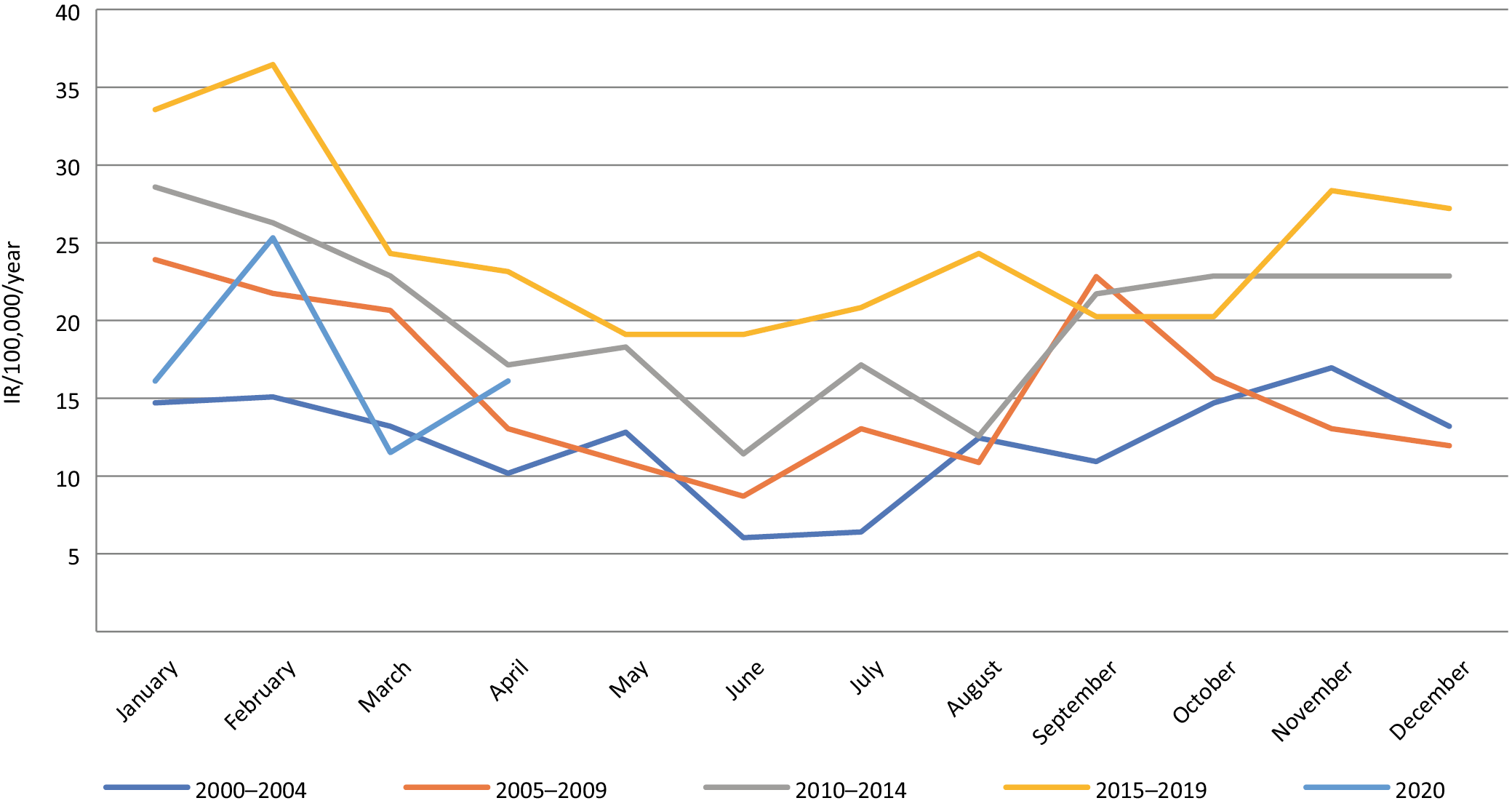
A degree of seasonality in T1D incidence was observed in the study period. Most often, T1D was diagnosed from September to February, with the highest IR being observed in January and February. Starting in March, the T1D IR decreased, with the minimum being observed in June and July, followed by an increase in the autumn. Detailed data is presented in Table 2 and Figure 2. There were half as many cases of T1D in Lower Silesian children in March and April 2020 than in the same months in 2019, but the difference between the IRs was not statistically significant; this was also true when compared with the whole study period (for March p = 0.2788; for April p = 0.8843), as well as for period IV (p = 0.1059 and p = 0.3741 for March and April, respectively). Surprisingly, T1D IRs in March and April 2020 were also comparable to those calculated for January and February this year (p > 0.05).
The clinical status of children was evaluated in five-year clusters: 2000–2004, 2005–2009, 2010–2014, and 2015–2019. In addition, the clinical condition of children diagnosed with T1D in 2019 and 2020 was compared, with a separate group for children diagnosed with T1D in March and April of 2020.
Over the entire study period, DKA occurred in 31.75% of patients with newly diagnosed T1D, statistically significantly less often (p = 0.0210) in period I (23.65%), while in subsequent years, there was a comparable percentage of children (34.23% in period II, 35.59% in period III and 36.71% in period IV; p = 0.9298). In the first 4 months of 2020, DKA was associated with the diagnosis of diabetes in 36.67% of patients, similarly to previous years (p = 0.6874), including 2019 (p = 0.9396). Diabetic ketoacidosis was present in 50% of patients diagnosed with T1D in March and April 2020; nevertheless, its incidence was comparable to previous years (p = 0.3635), including 2019 (p = 0.7450).
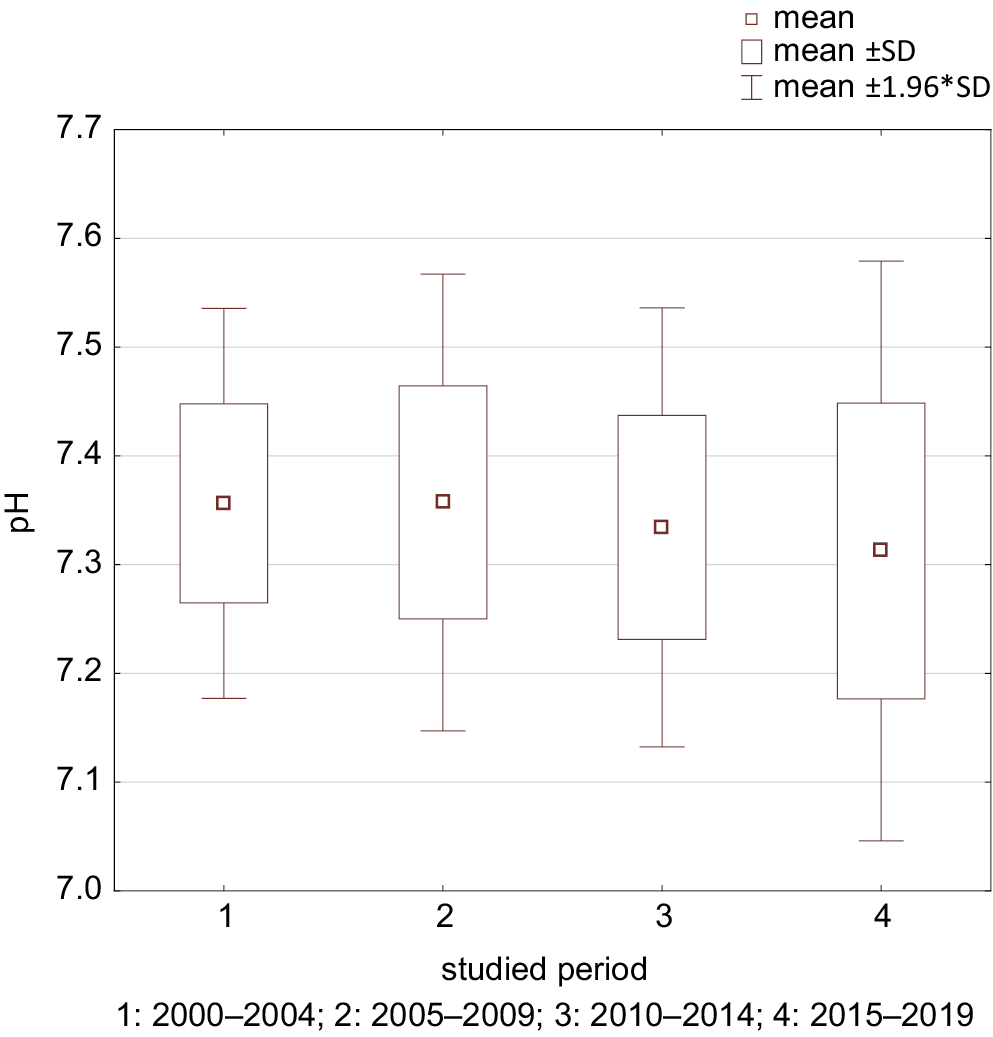
The mean pH upon admission to the Department was 7.34 ±0.11. This differed significantly over the study period: from 2015 to 2019, the mean pH was 7.31 ±0.14, significantly lower than in other years (Figure 3); in period I, the pH was 7.36 ±0.09; in period II, it was 7.36 ±0.11; and in period III, it was 7.33 ±0.10. Metabolic disorders in children diagnosed with T1D in 2020 were even more severe, as the mean pH was 7.26 ±0.19 (p = 0.0169). Moreover, the mean pH in children hospitalized in March and April 2020 (7.19 ±0.24) was lower than in previous years (p = 0.0199).
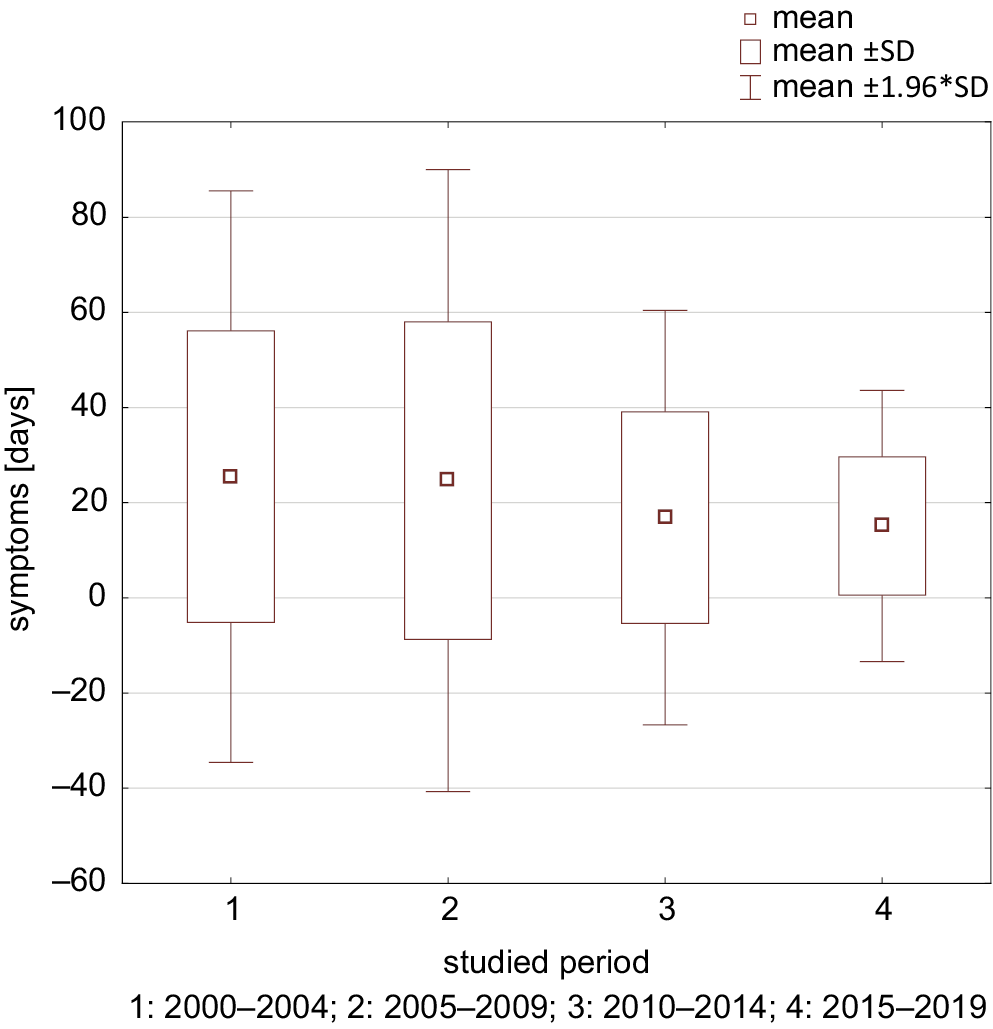
The mean duration of symptoms of hyperglycemia, as declared by the patient or legal guardian, was 20.2 ±25.4 days throughout the whole study period. It was the longest in period I (25.5 ±30.6 days) and the shortest in period IV (15.1 ±14.5 days) (p < 0.0001). In period II, it was 24.7 ±33.3 days and in period III – 16.9 ±22.2 days (Figure 4). In 2020, the mean declared duration of symptoms was 13.1 ±10.96 days, which was similar to that observed in previous years (p = 0.1675). It should be emphasized that the mean duration of symptoms in patients hospitalized in March and April of 2020 was 9.67 ±5.63 days, though it was comparable both to the previous years (p = 0.0831), to the year 2019 (p = 0.8031), and to January and February of 2020 (p = 0.6149).
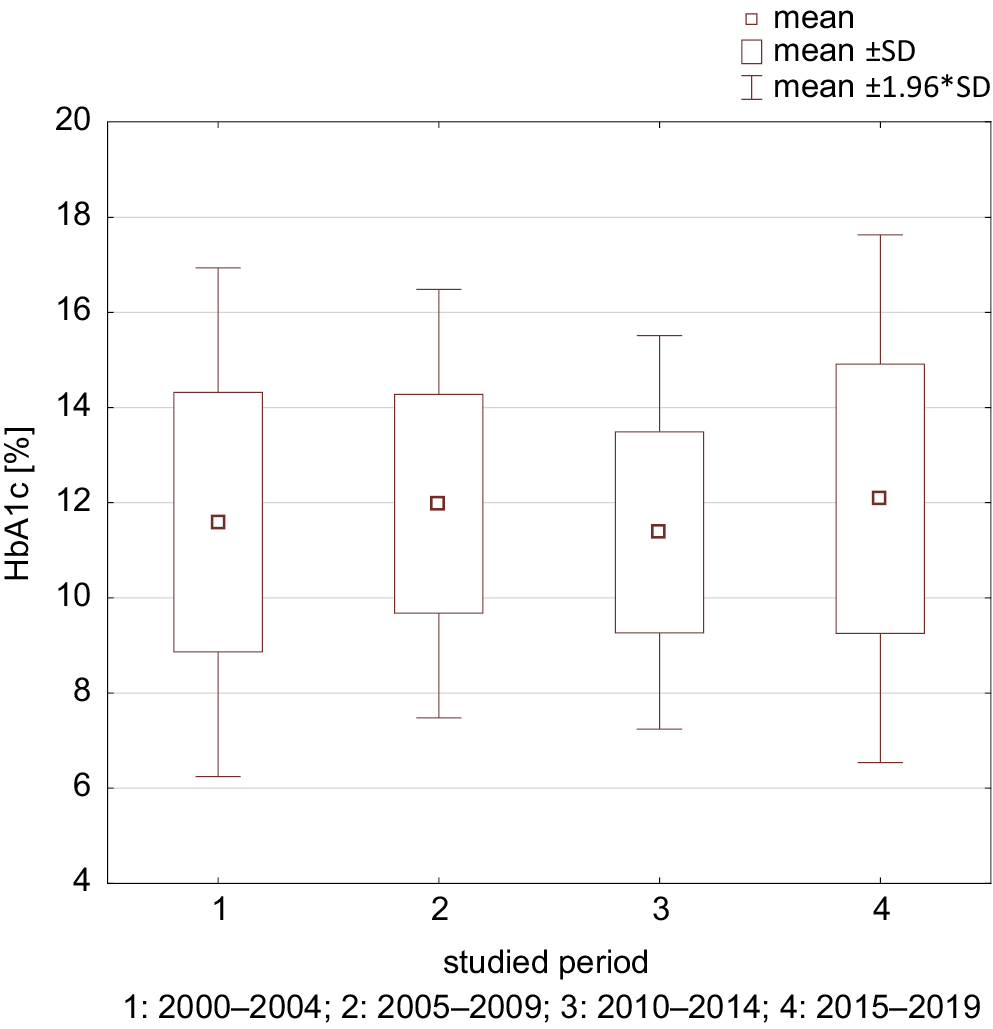
The mean HbA1c level in the study group was 11.79 ±2.63%. The highest percentage of HBA1c was found in children with T1D diagnosed between 2015 and 2019 (12.08 ±2.83%), while the lowest in patients hospitalized from 2010 to 2014 (11.37 ±2.11%) (p = 0.0013). In patients with T1D diagnosed in period I, HbA1c level was 11.59 ±2.72%, while for those diagnosed in period II, it was 11.99 ±2.30% (p = 0.0391). The mean HbA1c levels between periods I and III, as well as between periods II and IV were comparable (p > 0.05), while the mean HbA1c level between periods II and III and between periods I and IV differed significantly (p = 0.0125 and p = 0.0032, respectively) (Figure 5). The mean HbA1c level in patients diagnosed with T1D in 2020 was 13.41 ±2.50%, which was higher than in previous years (p = 0.0003), including the HbA1c level of patients diagnosed in 2019 (12.17 ±3.0%; p = 0.0234). On the other hand, the HbA1c level in patients in whom T1D was confirmed in March and April of 2020 was 13.06 ±2.35% and did not differ from the mean HbA1c in patients diagnosed in previous years (p = 0.1171), including 2019 (p = 0.3620) and the period of 2020 before the COVID-19 pandemic was announced (p = 0.2915).
Discussion
Numerous studies have indicated an increase in the incidence of T1D at a rate of about 3% per year.6 Epidemiological studies carried out in Poland have also confirmed this trend, with the T1D IRs for some regions of the country being comparable to data from Western Europe and North America.7, 8 Also, the current study found a twofold increase in the IR of T1D in children and adolescents in Lower Silesia over the last 20 years. It is noteworthy, however, that in the last 2 years, the IR has decreased: in 2019, it was the lowest in the last 5 years, and the forecast for 2020 is also lower than in previous years. The trend towards stabilization or even a slowdown in the growth of new cases of T1D has been observed in recent years in other countries, not only European ones. Recent reports have also indicated a certain cyclical incidence of diabetes and a periodic decrease in the IR.6, 8 It is therefore possible that the current decrease in the incidence of T1D among Lower Silesian children, especially the lower IR in the current year, may be due to cyclical fluctuations, as previously described by Chobot et al.9 On the other hand, the “silence” observed at our center regarding the diagnosis of new cases of T1D in children may be the result of avoiding contact with healthcare providers out of fear of being infected with the new coronavirus, together with the seasonality of the incidence of T1D.
The role of environmental factors in the pathogenesis of diabetes is indisputable and has been confirmed by the fact that the incidence of T1D – especially among older children – changes seasonally, decreasing significantly in the summer months.10 The seasonality of the presentation of new cases of T1D was previously observed in the Lower Silesian population.11 Data from 20 years of observation confirms this trend. In the winter months, there are significantly more new cases of T1D in children and adolescents than in summer, and the IR in January and February covered, on average, 1/5 of all new diagnoses in a given year. In absolute numbers, the number of new cases of T1D in our center has been steadily decreasing since March; however, the IR for March was comparable to the IR for January and February, while the IR for April was significantly lower. A similar relationship can be observed this year, although the IR for March 2020 is half that of the previous months and the lowest value for the month of March in the last 20 years.
On March 4, 2020 the first case of SARS-CoV-2 infection in Poland was diagnosed in a man travelling from Germany. On March 20, 2020, an epidemic was announced in the country; however, some restrictions were introduced a few days earlier, including the cancellation of mass events, the closure of national borders and obligatory quarantines for returnees. International rail and air transportation was suspended, domestic transportation was restricted, and schools, colleges, preschools, and nurseries were closed. On March 24, 2020, significant restrictions on movement were introduced: only trips to work, to grocery stores or pharmacies, or to help others were allowed. Children and adolescents up to 18 years of age could only leave home under adult supervision. We were constantly reminded of the need for social distancing.
At the same time, access to the healthcare system was limited, as all planned hospital admissions and surgical procedures were cancelled, and the activities of specialist outpatient clinics were limited to telemedicine consultations. Primary healthcare providers also carried out telemedicine consultations whenever possible. All of these measures were aimed not only at limiting gatherings of people, but also at protecting healthcare workers and securing hospitalization in the situation of an uncontrolled outbreak.
Social distancing is the most important intervention in the case of an epidemic of a disease for which there is no cure or vaccination, as it aims to reduce the possibility of infection. It seems that – at least so far – the actions taken have had the intended effect, because in Poland there was no rapid increase in infections comparable to that seen in Italy, Spain or Great Britain.12 On the other hand, public opinion is that contact with the healthcare system has become associated with a high risk of infection, and as such, is limited and delayed.
However, the appearance of T1D in children usually takes a rapid course and has symptoms that are difficult to overlook, which (in a way) forces families to seek help from the healthcare system. Therefore, it was expected that the incidence of T1D in children in 2020 would be comparable to that in previous years. According to the statistical comparison of IRs, this is indeed the case.
On the other hand, if parents and caregivers have deferred contact with the healthcare system for fear of infection with the new virus, the effect should be a deterioration of the children’s condition at presentation (e.g., DKA) and a longer duration of hyperglycemia symptoms and higher HbA1c levels. Our study found that DKA was present in half of the children diagnosed with T1D during the pandemic. The pH of these children was significantly lower than that of children diagnosed in previous years and in the months preceding the COVID-19 pandemic. One of the children was in a diabetic coma, which had not been seen in our center since 2000. However, the declared duration of symptoms was shorter and the level of HbA1c lower than in previous years, which would contradict the thesis that parents are postponing contact with healthcare providers and, consequently, delaying diagnosis and treatment; it would rather indicate a more rapid course of the disease.
As with Middle East Respiratory Syndrome (MERS) infection, diabetes is one of the factors determining a severe course and increased mortality in COVID-19. Data from the Centers for Disease Control and Prevention (CDC) registers indicate that patients with diabetes have a 50% higher risk of dying from SARS-CoV-2 infection than those without carbohydrate disorders.13 This is due to the fact that hyperglycemia alters the immune response, phagocytosis, neutrophil chemotaxis, and cell-mediated immunity. Angiotensin 2 converting enzyme (ACE2) has been identified as the receptor for the main protein of SARS-CoV-2 and is necessary for it to enter the host cell. The ACE2 molecule was proven to be anti-inflammatory and to protect against AH5N1 influenza infection. Acute hyperglycemia has been shown to increase ACE2 cell expression, facilitating SARS-CoV-2 infection. However, after the virus enters the cell, ACE2 expression decreases, resulting in increased susceptibility to the development of an excessive immune response and the occurrence of acute respiratory distress syndrome. It should be emphasized that a lower expression of anti-inflammatory ACE2 is also observed because of long-lasting poor metabolic control of diabetes. This may result in an excessive inflammatory response of the body and cell damage. Then, even a mild COVID-19 infection in patients with chronic hyperglycemia may cause excessive secretion of interleukin 6 (IL-6), IL-1b and tumor necrosis factor α (TNF-α), monocyte chemotactic protein 1 (MCP-1), and other cytokines, thus causing cytokine release syndrome, a “cytokine storm” that leads to rapid deterioration of the patient’s health.14, 15, 16
The expression of ACE2 on pancreatic β cells may potentially lead to β cell damage by the virus and result in insulin deficiency.17, 18 In addition, it should be underlined that inflammation itself is a factor which causes a decrease in insulin sensitivity, and thus an increase in insulin demand. Therefore, in insulinopenic conditions, this will result in a deterioration of metabolic control or faster diabetes manifestation, and potentially its more rapid course. Italian studies have indicated a higher incidence of DKA and of the severe form of the disease.19
Patients admitted to our center during the ongoing pandemic did not have any infections. This includes COVID-19, though due to the lack (at that time) of reliable serological tests for SARS-CoV-2, we could not determine whether our patients were infected before the presentation of diabetes. This is undoubtedly a limitation of this study. While a shorter duration of symptoms and a lower percentage of HbA1c indicate a worse clinical condition when diagnosing diabetes, the higher rates of DKA and the significantly lower blood pH could indicate a more rapid course of the disease in these patients. Whether it was due to a COVID-19 infection, needs to be determined in the future.
It should also be remembered that a viral infection trigger an autoimmune reaction, leading to the presentation of T1D, as has already been seen with the coincidence of the outbreak of Coxsackie B5 virus in Jefferson County, Alabama in 1983 and an increase in T1D IR.20 However, to test this hypothesis, an analysis of the IR of T1D in the following months and years needs to be performed.
Conclusions
The IR of T1D in Lower Silesian children in the months of the COVID-19 pandemic was comparable to previous years, while their clinical condition at the time of diagnosis was worse compared to previous years.