Abstract
Clinical skills refresher courses focusing on competence are essential for enhancing the clinical performance of healthcare providers. These courses play a pivotal role in nursing and midwifery education, offering students initial exposure to clinical environments and preparing them for subsequent internships. This systematic review aimed to assess the effectiveness of clinical skills refresher courses on clinical performance, particularly focusing on competency-based supplementary clinical skills courses.
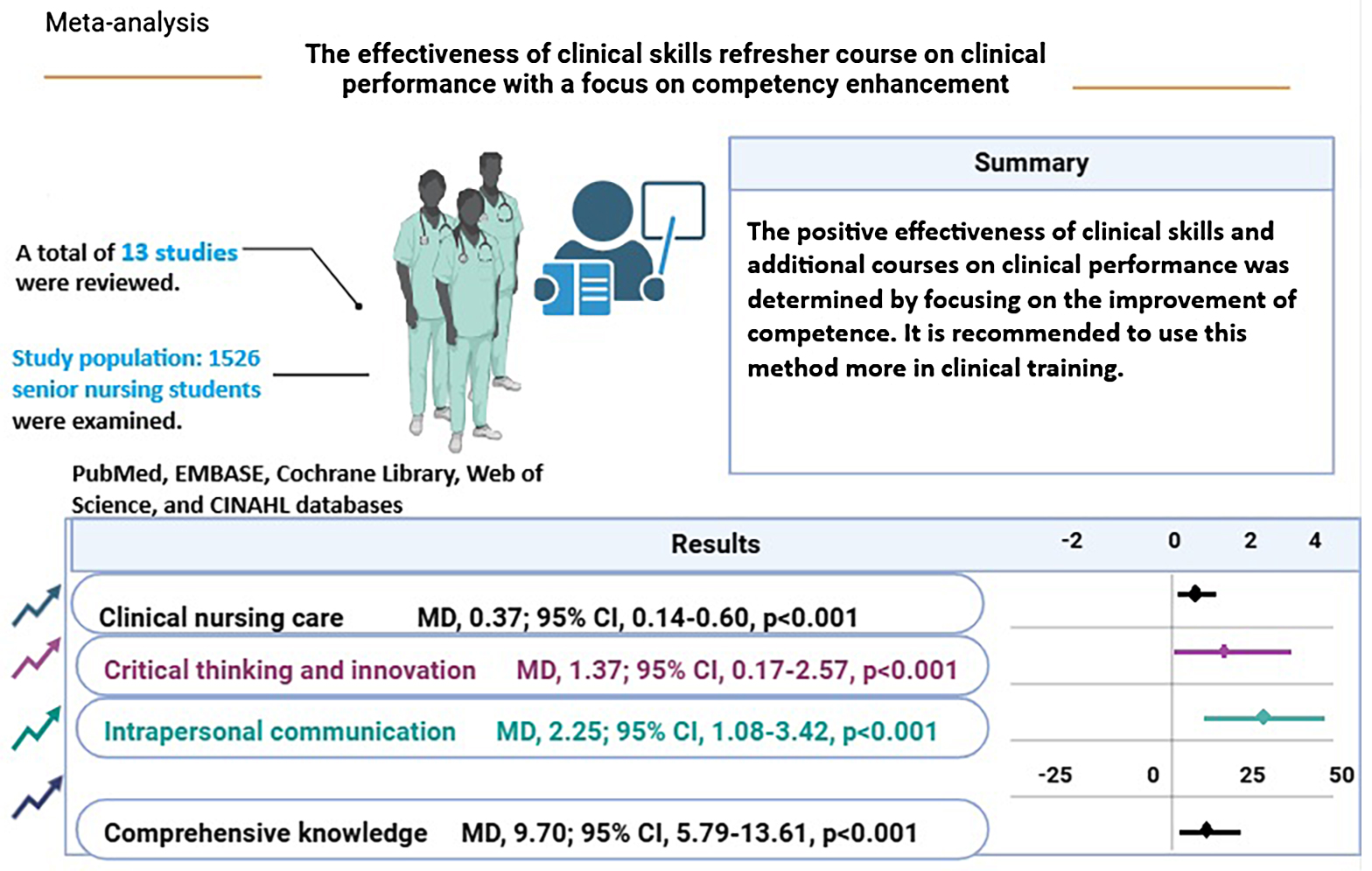
A comprehensive literature search was conducted across articles published in the last 15 years, utilizing PubMed, Embase, Cochrane Library, Web of Science, and Cumulative Index of Nursing and Allied Health Literature (CINAHL) databases with specific keywords. This extensive search yielded 1,751 records, of which 13 were selected based on strict inclusion and exclusion criteria. Of these, 5 studies examined the effect of competency-based education (CBE) on the quality of clinical skills, 5 studies assessed clinical skills in detail, and 3 studies discussed other variables related to nursing skills, such as anxiety. The results indicate that CBE significantly enhances clinical skills and self-efficacy among nursing students, addressing gaps in practical training and psychological readiness for clinical internships.
This review recommends the implementation of well-organized competency-based training courses in nursing and midwifery education. By bridging the gap between theoretical knowledge and practical experience, this approach equips nurses and midwives to effectively address contemporary healthcare challenges, ultimately improving patient outcomes, enhancing professional confidence and ensuring adherence to healthcare standards.
Key words: nurses, midwives, clinical skills, competency-based education, refresher course
Introduction
Learning is the fundamental foundation of human progress in today’s world. Literacy improves people’s attitudes and performance, and it is further enhanced through new, practical methods in learning curriculum design. The curriculum is a cornerstone of educational sciences, and its pivotal role in educational practices cannot be overlooked.1 Improving the quality of education by aligning educational goals with performance and activities is essential for developing educational programs that meet societal health needs. To address these demands, both the theoretical and practical components of an effective educational system must be continuously updated.2, 3, 4
The “Clinical Skills” foundational course is designed to introduce nursing and midwifery students to real-world clinical experiences. It is essential to assess both existing practices and ideal benchmarks across theoretical, practical and clinical aspects of education within this course. This serves as students’ initial exposure to the clinical environment, helping to prepare them for future internships.5, 6 Alternatively, nursing students receive clinical skills training in the nursing school’s clinical laboratory during their 1st semester. Following this, they participate in a range of supervised exercises in hospitals and other clinical settings. In preparation for their final year, students engage in a 2-semester internship, in addition to part-time, unsupervised classes. The goal of this internship program is to help students transition from an academic setting to a clinical setting.7
Unfortunately, some students do not fully experience all the necessary clinical nursing abilities, and some may gradually deviate from standard practice procedures due to inadequacies and issues inherent in various clinical environments.8 Accordingly, improper learning in clinical courses was identified by Aein et al. as a major issue in clinical nursing education programs.9 Numerous studies from Iran, China, Australia, and the UK have demonstrated that nursing students lack psychological readiness for clinical internships. Senior nursing students and recently graduated nurses are acutely aware of their clinical incapacity, which causes them to feel anxious and lack confidence. A student’s last year of study may be less educationally beneficial if they join an internship program with such uncertainty and worry.10, 11, 12
To ensure a seamless transition into professional practice, final-year nursing students should enhance their clinical skills by participating in competency-based supplementary training courses. In other words, the final year serves as a preparatory phase that helps nursing students solidify their clinical abilities while cultivating favorable work attitudes and professional traits. To support final-year clinical students, several educational approaches and initiatives have been proposed in the form of competency-based supplementary courses. These instructional strategies positively impact students’ approaches and clinical abilities by reducing their sense of inadequacy.13, 14, 15
Short-term supplemental courses designed to enhance clinical skills can help students feel less anxious before starting their internships. The primary cause of stress among newly graduated nurses is the perception of their clinical incapacity to perform clinical duties.16 Throughout the final year of the nursing bachelor’s program, feelings of inadequacy in performing professional nursing tasks, along with associated anxiety, often lead to considerations of leaving the profession. These emotions are frequently triggered when students become aware of their limitations and upcoming legal responsibilities.17 In many countries, nursing students inevitably encounter unsuitable role models in clinical settings. Therefore, it is crucial for students to have an opportunity to refresh their clinical knowledge before graduation.
Short, additional courses on clinical skills, based on competence, can help nursing students become more proficient in the field, feel more confident in their abilities and experience less anxiety.7, 18 Ongoing challenges in healthcare education, particularly those highlighted by emerging medical issues such as the COVID-19 pandemic, have made competency-based education (CBE) a timely and relevant approach. Competency-based education addresses many limitations of traditional educational models by emphasizing flexibility, personalized learning, alignment with workforce demands, and mastery of skills.19 As healthcare systems adapt to new realities, CBE provides a pathway for preparing competent professionals to effectively meet future challenges.
As mentioned above, CBE provides a valuable approach that focuses on improving specific skills and competencies, rather than adhering to a fixed curriculum or schedule. This method is especially important in nursing and midwifery, where the ability to apply theoretical knowledge in real-world scenarios is essential for delivering high-quality patient care.
Objectives
This study aims to examine the significance of CBE for nurses and midwives by systematically analyzing recent literature, with the goal of offering valuable insights to educational administrators for improving healthcare outcomes.
Materials and methods
An extensive literature review was conducted across various databases covering the past 15 years, using targeted keywords associated with CBE and clinical performance. Out of 1,751 identified records, 13 studies were chosen after applying stringent inclusion criteria.
Systematic preprocessing workflow
Data processing involved the following main steps: 1) initial search, 2) literature screening, 3) full-text evaluation, 4) initial data extraction, 5) quality assessment, and 6) data synthesis. The final step, data synthesis, involved incorporating summaries of findings from the selected literature and preparing them for interpretation.
Search strategy and initial preprocessing
The initial literature search included a primary screening of the literature in the database based on search queries and Boolean operators (AND, OR, and NOT). A comprehensive literature search was performed on original English-language research publications during the last 15 years from databases including PubMed, Embase, Cochrane Library, Web of Science (WoS), and Cumulative Index of Nursing and Allied Health Literature (CINAHL). Based on the predetermined aim of the study and the Preferred Reporting Items for Systematic Review (PRISMA) search strategy, literature searching was initiated using the relevant search queries and keywords as follows (alphabetically ordered): “basic clinical skills”, “clinical performance”, “clinical practice”, “clinical skills”, “clinical training”, “competency”, “competency enhancement”, “competency-based education”, “competency-based training”, “health professional competence”, “midwife competence”, “midwife education”, “nurse”, “nursing competence”, “nursing education”, “professional development”, “refresher course”, “self-efficacy”, and “skills”. Additionally, mentioned search terms were used in combination with Boolean operators such as “AND” and “OR”.
Screening and article selection
Screening was conducted independently by 2 trained authors in 2 steps. First, they assessed the titles and abstracts of the searched articles for relevance to the study’s aim. Second, they evaluated each article based on inclusion and exclusion criteria, quality and relevance to the review’s objectives. The abstract of each article was examined, and the full text was obtained for any article that could not be excluded based on the title or abstract. Duplicates were identified and excluded.
Inclusion and exclusion criteria
Published literature, including original research articles, quasi-experimental studies, case-control studies, and cohort studies, were included in the study selection. The focus was on evaluating the effectiveness of clinical skills refresher courses by measuring clinical performance and competency enhancement in nurses and midwives, regardless of factors such as age, weight, etc. Studies that assessed clinical skills and related parameters in evaluating nurse education with an emphasis on competency or the development of competence were also considered.
Articles that were not available in full text, including editorials, review articles and those included into nurses or midwives, or that did not evaluate refresher training in clinical skills, competency development or clinical performance in the targeted study population, were excluded from the analysis. Additionally, studies that were not published in full text were also excluded.
Full-data extraction
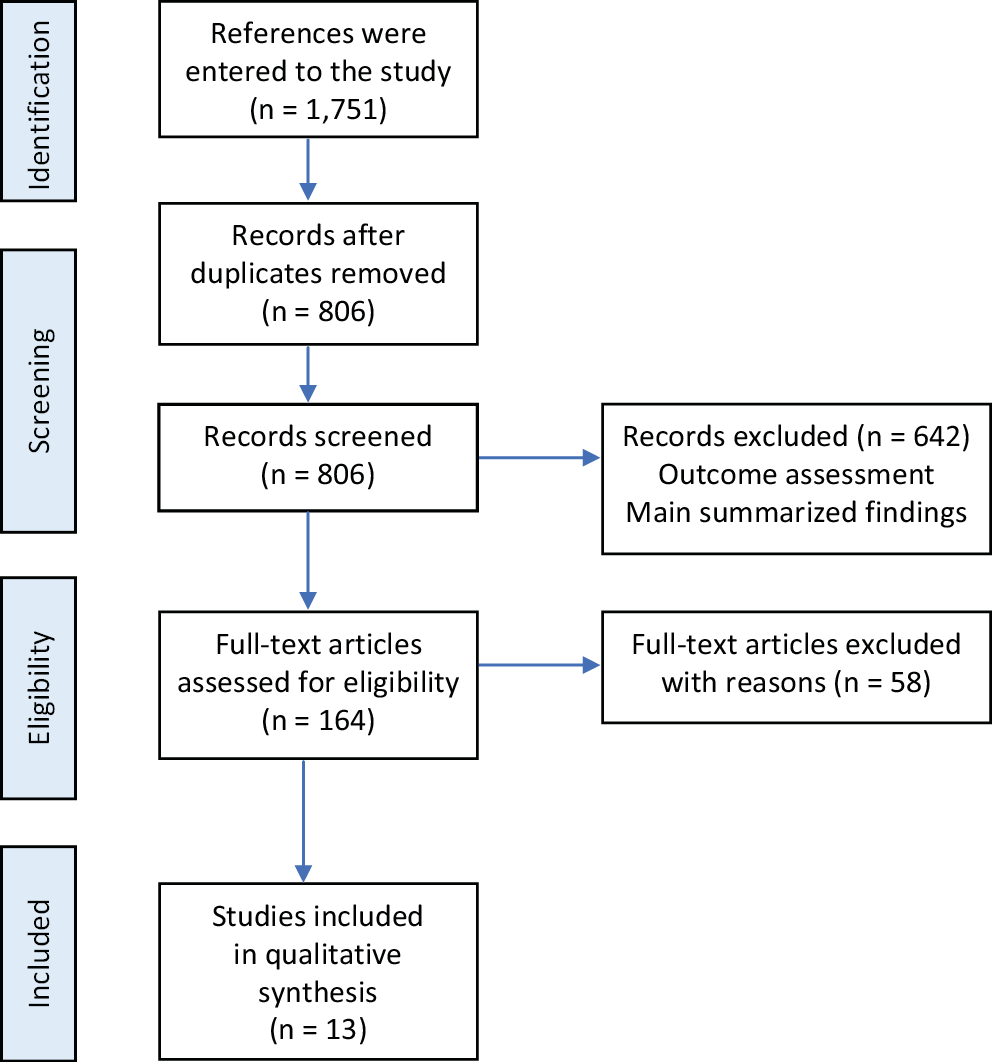
After screening, the full texts of the selected literature were downloaded, and the complete text and details of the reviewed results were obtained. Articles that met all inclusion criteria and were of sufficient quality were chosen for final evaluation. The goal of the study and data collection were determined using the PRISMA framework, which included the analysis technique and interpretation (Figure 1). Data extraction was performed by 2 trained reviewers, focusing on study design, sample size, participant ethnicity, outcome assessment, and key findings.
Checking articles quality
Two academics with backgrounds in systematic review research and nursing themes independently assessed the quality of the downloaded publications. The results were then addressed during meetings and in situations where there were disagreements, the conversation continued until 2 evaluators came to a final consensus. Quality assessment of resources was performed using the Cochrane Risk of Bias tool, which is an effective instrument for systematically evaluating the robustness of included publications. It considers key determinants of various biases, including selection, performance, detection, attrition, and reporting.20 In terms of selection bias, the researcher evaluated the adequacy of methodology in randomization to generate allocation sequence as well as sufficient description in methodology (random sequence generation (RSG)), and whether the allocation sequence was concealed from participants (allocation concealment). Performance and detection biases express the blindness of participants, assessors or both. In attrition bias, the author searches whether missing data were addressed well, and finally, in reporting bias, the researcher checks if all achieved data were reported in some of them removed selectively (selective outcome reporting). All 6 parameters were scored as “Low risk” and “High risk”. If it was not reported in the main resource, then we put “Unclear.” A lower summation of the risk of bias was favored for evaluation.
Results
In the initial search, 1,751 records were obtained by examining the article text, inclusion and exclusion criteria, and subject relevance. A total of 13 studies were selected for further examination (Figure 1). Regarding study type, 12 semi-experimental articles and 1 randomized clinical trial (RCT) were included, with all studies being case-control ones (Table 1).7, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31, 32 Six studies were conducted on Chinese nurses,21, 22, 23, 24, 25, 26 4 studies were conducted on Iranian nursing students,7, 27, 28, 29 2 studies were conducted on Taiwanese nurses,30, 31 and 1 study was conducted on South Korean nurses.32 In 5 studies, attention was paid to the effect of CBE on clinical skills.22, 24, 27, 30, 31 The outcomes of CBE were assessed using 2 main approaches: first, through formal assessments of nurses and midwives, enabling them to demonstrate their improvement and performance; and second, through assessment tools such as technical improvement evaluations, strategic examinations and self-report questionnaires. In 5 studies, clinical skills were examined alongside other variables.7, 23, 26, 28, 32 In 3 studies, other variables related to nursing skills were also examined.21, 25, 29 In 10 studies, the effect of CBE on improving clinical skills was reported.22, 28, 30, 32
Risk of bias in individual studies
The Cochrane Collaboration Risk of Bias scale was used to assess the quality of the 13 articles included in the systematic review. Table 2 presents the quality evaluation results of these articles.7, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31, 32 According to the Cochrane evaluation scale, 3 studies had a risk of bias in 3 areas, while 5 studies had a risk of bias in 1 area. The remaining studies did not show clear evidence of risk in the areas of selection, performance, reporting, or other forms of bias.
Discussion
This study suggests that clinical skills refresher courses can significantly improve clinical performance, reduce anxiety and better prepare nurses and midwives for their ongoing professional roles. Therefore, it is strongly recommended to implement integrated short-term refresher programs that focus on competency to enhance training outcomes more effectively. Nursing education includes both theoretical and clinical training, with the expectation that graduates will possess the necessary competencies for professional nursing practice. Additionally, participating in clinical skills enhancement courses can increase nurses’ self-confidence and improve their clinical proficiency.32 The results indicate that emphasizing supplementary training on nursing competence can significantly influence the development of clinical skills over time18; however, the scope of this matter remains highly significant.
In nursing and midwifery practice, CBE plays a crucial role in improving patient safety and healthcare quality. This approach ensures that healthcare professionals acquire essential skills, enhance their clinical decision-making abilities and adhere to standardized protocols. As a result, patients experience better outcomes, healthcare services become more efficient and overall satisfaction increases. Additionally, this educational model fosters professional growth and helps practitioners meet regulatory requirements.
This study highlights the importance of CBE and its effective implementation in real-world clinical training. Several key strategies can support the successful application of this educational model.33 First, it is essential to determine whether the training course is appropriate and built upon a well-structured curriculum. A curriculum should be designed around a set of competencies that encompass clinical skills, critical thinking and effective communication essential for nurses and midwives. Incorporating real-world experiences, maintaining continuous assessment and fostering collaboration with clinical institutes are also critical steps. Practical exposure in healthcare settings allows well-trained students to gain valuable experience. Instructors can use simulated competency-based training to engage students in unrealistic situations that reflect patient care expertise. Finally, evaluating the training program and collecting feedback through structured questionnaires can help educators refine and improve their training method.34
The present systematic study was conducted to investigate the effectiveness of competency-based clinical skills supplementary courses on nurses’ clinical performance. In the reviewed studies, the impact of CBE on improving clinical skills was confirmed. Shahsavari et al. demonstrated the positive effect of a clinical skills refresher course on clinical skills, although the focus of the course was not specifically on merit. They suggested that the undergraduate nursing curriculum could be strengthened with a supplementary course on basic clinical skills. This training course can bridge the gap between theoretical knowledge and practical application, providing a smoother transition from a student’s role to that of a nurse.7 Another study reported that students who received CBE had higher performance in theoretical and practical courses in medical-surgical nursing.31 They were better in terms of clinical performance.27 Additionally, based on another semi-experimental study, it was found that clinical and cognitive skills were higher in the group receiving CBE.28
This systematic review strongly emphasizes the importance of incorporating a competency-based approach into nursing education. Given the critical role that nurses and midwives play in patient care outcomes, such an approach is likely to enhance their professional performance and increase their self-confidence in clinical practice.
There are serious gaps between theoretical learning and its clinical applications in healthcare educational systems.35 A well-identified approach to overcoming these faults can increase the integration and frequency of practical experiences, reinforce theoretical knowledge through training courses, enhance critical thinking, problem-solving and emergency management, and acknowledge CBE.36, 37 The results highlight the crucial role of supplementary clinical training in undergraduate nursing programs. Newly graduated nurses often experience significant stress due to a lack of confidence in their clinical abilities. Among the various challenges faced in nursing, anxiety is closely linked to perceived clinical incompetence, which emerges as a key concern affecting professional readiness.16, 38 Nursing educators and curriculum developers play a crucial role in easing students’ anxiety during training. Therefore, strategies aimed at reducing or managing this distressing experience should be thoughtfully implemented.7 Research by Valizadeh et al.29 indicates that CBE enhances both cognitive and behavioral skills in nursing students. Their findings showed that students in the experimental group demonstrated notable improvements in these areas. Moreover, these students exhibited higher levels of clinical competence compared to those taught through traditional methods. Their study concludes that outcome-focused educational approaches are more effective in building essential nursing competencies than conventional teaching strategies.29
It has been observed in various surveys that focusing on competence in the training courses can have a positive effect on nurses’ competence.30 In the meantime, patient safety competence is a critical issue, as nurses are responsible for patient care 24 h a day.39 On the other hand, the implementation of supplementary courses and education types in advanced countries has made the skills and self-confidence of nurses acceptable. A study in Italy reported the competence of nursing students in the patient safety field at a high level.40 In her review, Park considered the effectiveness of additional clinical skills courses on clinical practice to be important. She stated that learning clinical skills provides an opportunity for students to improve their clinical and communication skills by using a variety of teaching aids, models and mannequins. In fact, the clinical skills center creates a link between theoretical content and practical skills.32 In a study by Danting et al., it was found that competency training has a positive effect on nurses’ ability, innovation, performance and clinical performance.22
Harvey et al. conducted an in-depth study to design a foundational training program tailored for nurses, midwives and other healthcare professionals. The initiative included an 8-day course, with its effectiveness assessed through participant feedback, as well as evaluations of knowledge, skill development and confidence. The program featured clearly articulated learning goals and was designed to allow participants to implement what they had learned between sessions. Emphasizing a strengths-based approach, it built on participants’ existing capabilities and integrated both theoretical instruction and hands-on practice.41
Evidence suggests that simulation-based training and supplementary courses are among the most effective strategies for maintaining clinical skills. However, drawing firm conclusions about other types of interventions is challenging due to inconsistencies in research quality and design. The existing literature shows considerable variability, limiting the generalizability of the findings. Therefore, well-designed RCTs are urgently needed to identify the most effective methods for resuscitation training and long-term skill retention.42 A study in Iran showed that emergency nurses’ knowledge was at a relatively high level, whereas the skills, attitudes and overall patient safety competence of nurses working in emergencies were at a relatively favorable level. They reported that a basic understanding of competence and nurses’ working skills in the emergency room is important for improving nursing quality, and additional clinical skills courses designed in the field of nurses’ safety competence based on evaluations can enhance treatment quality.43 A study conducted in Iran highlighted that professional self-efficacy among nursing students falls within a moderate range, indicating a need to revise nursing graduate curricula. Emphasis should be placed on fostering clinical and professional competencies, and these elements should be actively incorporated into nursing assessments. Our systematic review supports the idea that competency-based refresher programs can significantly improve nurses’ practical abilities, knowledge and professional outlook. Overall, the evidence suggests that CBE plays a vital role in enhancing the clinical performance of healthcare practitioners.18
Another systematic review examining the impact of the CBE model in training newly graduated nurses found that emphasizing competency development in educational programs significantly enhances various professional abilities. These include improved clinical care performance, stronger critical thinking and innovation, better interpersonal communication, greater professional growth, increased knowledge, and more refined personal attributes. Furthermore, the benefits of competency-based training have also been observed among physicians, where such programs have been shown to enhance clinical skills and overall professional effectiveness.44, 45, 46, 47 Continuing professional development (CPD) should be implemented to enhance nursing competence. However, attention must also be given to the challenges encountered in clinical skills training. The findings identified 2 key obstacles in this area: the lack of effective clinical education facilitators and the presence of various barriers that hinder practical learning experiences.48, 49
Recent research has demonstrated the substantial impact of CBE in improving clinical performance among nursing students. Those who engaged in CBE exhibited improved clinical abilities and greater self-confidence compared to those trained through conventional methods. This study emphasizes the value of CBE in equipping nursing students to face real-world clinical scenarios effectively.50, 51 Similarly, refresher programs have proven successful in increasing nurses’ skills while also attenuating the anxiety levels linked with clinical responsibilities. These findings support the conclusions of our review and, further advocate for the integration of CBE in nursing curricula to better prepare students for real-world clinical challenges.52 Furthermore, existing literature suggests that ongoing professional development combined with CBE is essential for ensuring that nurses remain equipped to handle the evolving demands of modern healthcare. Through the implementation of these educational strategies, institutions can foster both clinical performance and confidence of current and upcoming nursing students, ultimately contributing to improved patient care.
Numerous studies have reported that nursing students and recent graduates often experience heightened anxiety, self-doubt and feelings of inadequacy as they transition into clinical practice and hospital internships.16 One widely recognized approach to alleviating this anxiety involves incorporating curriculum models that emphasize hands-on clinical skill development. Simulated clinical environments, in particular, have been shown to enhance practical skills while also reducing anxiety levels.7 Integrating such approaches within a CBE framework may further enhance the effectiveness of clinical skill acquisition. Learning is an ongoing and dynamic process through which individuals gain knowledge, refine skills and shift their attitudes and performance. A central goal of nursing education is to continuously enhance its programs by introducing innovative and practical strategies. By participating in supplementary courses that focus on competency development, nurses can improve their knowledge base, attitudes and professional performance, ultimately contributing to higher levels of clinical competence.
Limitations
Reanalyzing the data presented several challenges, primarily due to insufficient resources for constructing a robust CBE model. Additionally, the limited number of studies focused on a single competency framework, combined with various confounding factors such as differences in foundational clinical skills, cognitive abilities and procedural expertise, made the interpretation of the findings more complex. A key limitation of the current systematic review was the scarcity of research specifically targeting competence. Furthermore, we lacked detailed insight into the students’ training environments, which may have introduced variables that influenced the outcomes. However, the strength of our study lies in the critical evaluation of article quality and the quasi-experimental designs employed, which enhanced the credibility of the findings. Another limitation was the limited focus on the long-term retention and practical application of competencies acquired through follow-up programs.
Conclusions
This study provides a deeper understanding of the importance of training improvement in healthcare providers, especially nurses and midwives, owing to their crucial role in responding to patients by highlighting the beneficial outcomes of CBE as a good approach. Although the current research provides a systematic review of publications in this field, the heterogeneity in the study details of the selected articles made it impossible to perform a meta-analysis.
Performing comparative studies in future cohort studies with more detail and distinct categorization in participants is beneficial to confirm the results. This study highlights several innovative elements of the proposed CBE model for nurses and midwives. These include the integration of theoretical knowledge with hands-on experience, consideration of personalized learning styles to address specific skill gaps, the use of simulation-based interventions to enhance practical abilities, and emphasis on developing core competencies to improve patient care.
Our study strongly advocates for the adoption of structured competency-based training programs by nursing educators and healthcare professionals aimed at addressing the specific professional gaps commonly observed among nursing students. Competency-based education bridges the gap between academic learning and clinical applications, equipping students to effectively navigate the dynamic challenges of today’s healthcare landscape.
Use of AI and AI-assisted technologies
Not applicable.