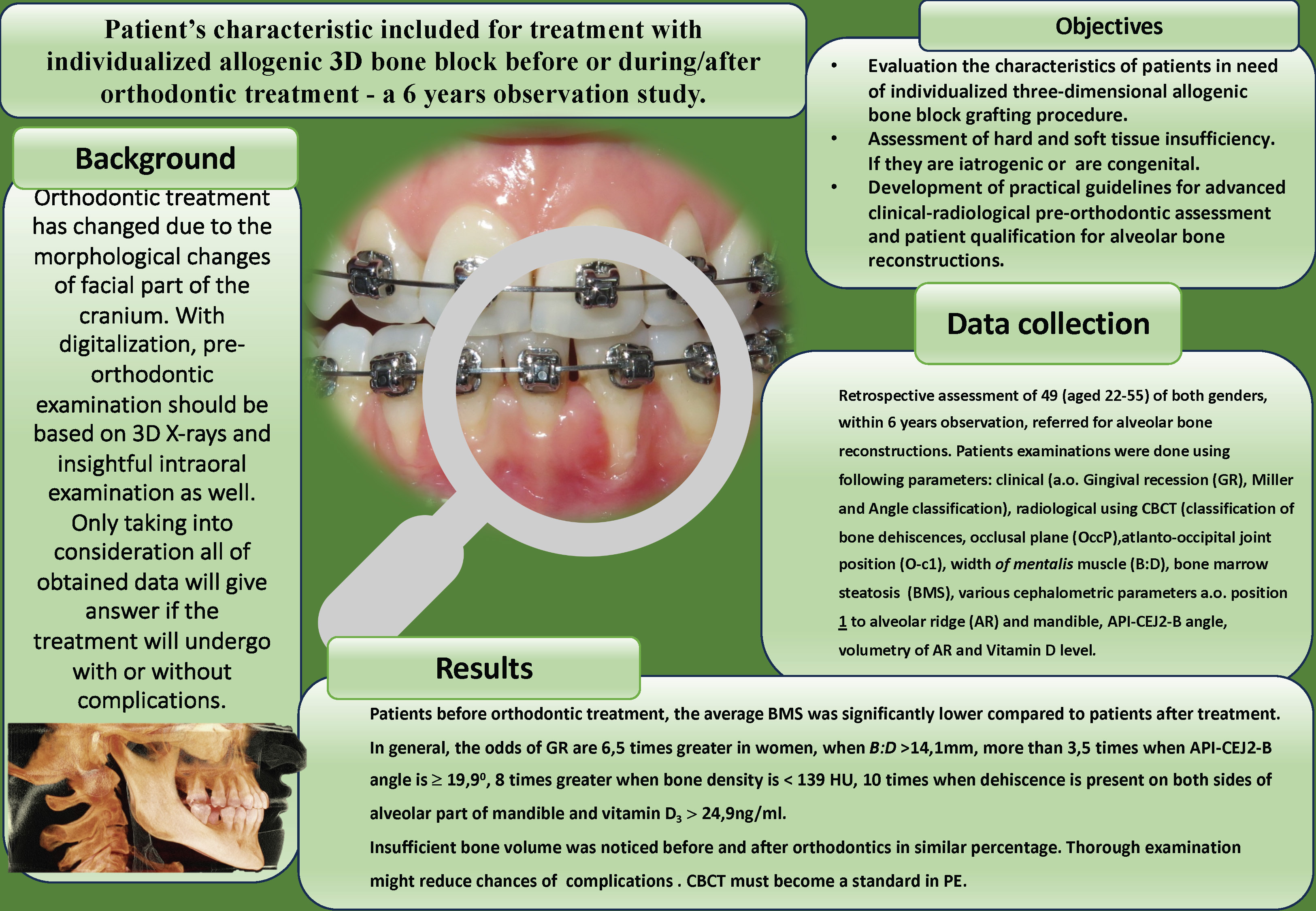
Abstract
Background. The most important part of orthodontic treatment (OT) is the pre-orthodontic examination (PE). Only a precise evaluation of clinical and radiological features can reduce the risk of complications.
Objectives. To develop practical guidelines for advanced clinical-radiological pre-orthodontic examinations and for qualifying patients for alveolar bone reconstructions.
Materials and methods. A retrospective assessment was performed on 49 out of 145 patients (aged 22–55) referred for alveolar bone reconstructions over a 6-year observation period, with 77.6% of the patients being women. Patient examinations were conducted using the following parameters: clinical (e.g., gingival recession (GR), Miller and Angle classifications), radiological (using cone beam computed tomography (CBCT) to evaluate bone dehiscence, occlusal plane (OccP), atlanto-occipital joint position (O-C1), width of mentalis muscle (B:D), bone marrow steatosis (BMS), and various cephalometric parameters such as the position of the alveolar ridge (AR) relative to the mandible, labial width angle, and volumetry of AR, as well as vitamin D level. Statistical analyses were performed using Student’s t-test, Shapiro–Wilk test and Pearson’s χ2 test.
Results. In the group of patients before orthodontic treatment (OT), the average bone marrow steatosis (BMS) was significantly lower compared to that in patients after treatment (–12 HU vs –137 Hounsfield units (HU)). In patients with class C dehiscence, the B:D measurement was significantly greater than in those with class A dehiscence (15.0 mm vs 12.5 mm). Additionally, a lateral shift of the atlanto-occipital joint (Oc-1) had a significant negative impact on the angles describing lower teeth inclination. Overall, the odds of gingival recession (GR) were 6.5 times higher in women (OR = 6.55); GR odds increased by more than 3.5 times when B:D exceeded 14.1 mm, by 4 times when the occlusal plane (OccP) was flat, and by 8 times when bone density was 24.9 ng/mL.
Conclusions. Insufficient bone volume was observed in a similar proportion both before and during/after orthodontic treatment. The described pre-orthodontic examination allows for an accurate assessment of soft tissue and bone condition, thereby reducing the risk of further complications. CBCT should become a standard component of the pre-orthodontic examination.
Key words: orthodontics, early diagnosis, recession, cone-cone-beam computed tomography, dehiscence
Background
Dentition and dental arch sizes have progressed significantly in the last 100 years; however, orthodontic guidelines have not. Diet has been shown to have a major impact on the dentition, the orthodontic area of interest also had to change.1, 2 As teeth and alveolar processes become smaller, consequently, a reduction in the width of the alveolar ridge is observed.
Therefore, during orthodontic treatment, a thorough pre-orthodontic examination must be performed, including evaluation of three-dimensional (3D) properties of the alveolar processes. For this purpose, cone beam computed tomography (CBCT) should be performed. Only this type of the X-ray examination allows to determine direction in which the orthodontic treatment should be carried out to avoid disturbing natural boundaries. Ignoring these principles is associated with a higher risk of complications such us gingival recessions, bone dehiscenses, teeth mobility, or even teeth loss.3, 4, 5
One of the most common complications are gingival recessions. They are described as a progressive loss of the gingiva and the underlying bone.6, 7 According to the above information, when the tooth is translated through the vestibular cortical bone, bone dehiscence will occur. Taking into account the biological width, or supracrestal apparatus, which is the biologically determined distance between the alveolar crest and the top of the keratinized gingiva (typically around 2.04 mm), apical migration of the gingiva can occur.8, 9 Considering that gingival recession is a common condition affecting much of the population, orthodontists face significant limitations in ridge expansion procedures to avoid violating the bony envelope and causing or exacerbating recession.10
Therefore, to avoid such complications, complete examination of the oral cavity should be carried out. Conditions which need to be taken into account are: the patient’s gingival phenotype, palpable roots through the soft tissue, pre-existing recessions, or patient’s pericervical restorations which may disturb biological width, and the depth of vestibule and frenula attachments. After (or even before) the intraoral examination, an extraoral examination should be done as well in which we should focus on the tension of the muscles surrounding the oral cavity, type of swallowing and breathing. Tension of the muscles around and inside the oral cavity is a crucial factor for the future success of the planned treatment. Imbalance between internal and external muscles might be a reason for teeth inclination. However, strong tension of muscles, such as the mentalis or mylohyoid muscle, may reduce the volume of the dental arches. Additionally, if the lingual frenulum is stiff and short, it is called ankyloglossia. It is responsible for several problems inside the oral cavity. It might be a reason for malocclusions, anterior and posterior crossbite, open bite, mouth breathing, and enlarged space between teeth called diastema. However, the organism should be considered as a whole and not as individual parts, so if one part is not working properly, it will affect the others. The influence of ankyloglossia can also be seen in a bad posture. This is caused by the anterior fascia which interconnects the whole body, from head to toe. A shorter and/or stiffer tongue frenulum will misalign the temporomandibular joints, which may also affect the occlusal plane and back problem of muscular origin.11, 12, 13
Leszczyszyn et al. reported a positive correlation between vitamin D3 deficiency and problematic skeletal growth.14 As this vitamin controls bone metabolism, its levels should be checked prior to orthodontic treatment, with adequate supplementation. In general, the endogenous vitamin D3 deficiency has been reported in the European population in several studies, so blood serum level should be assessed.15
However, vitamin D3 deficiency is not just a general problem in dentistry, since it can lead to poorer bone architecture and volume. Worse bone quality, increased fragility and susceptibility to microdamge are the results of many autoimmune diseases as well. For instance, in the case of the diabetes type I, it is caused by microangiopathy, insulin resistance, and lack of insulin-like growth factor 1 (IGF-1). In case of type II diabetes, the drugs lowering sugar concentration in the blood serum might influence in bone fragility too.16 Celiac disease might affect bones through malabsorption of minerals and vitamin D from intestines.17 Even bleeding disorders, such as hemophilia, can reduce bone density, not to mention bone diseases such as Paget’s disease.18 Another concerning issue is a growing problem of obesity and high-fat diet, common in a modern society. It weakens the bone by the T-lymphocytes which induce osteoclastogenesis through production of interleukin 6 (IL-6), osteoclastogenic cytokines such as RANKL, tumor necrosis factor alpha (TNF-α), IL-1β, and interferon gamma (IFN-γ).19
Patients facing these challenges often seek treatment through individualized 3D allogeneic bone block grafting. This surgical method, described and patented by Dominiak and Gedrange, has shown promising results in resolving complications, completing problematic orthodontic treatments, and even initiating treatment in complex cases. The entire method and surgical procedure are described in previous publications.3, 4, 5, 20
Objectives
The aim of this study was twofold: first, to evaluate the characteristics of patients who require individualized 3D allogenic bone block grafting – either prior to orthodontic treatment or following complications – and second, to develop practical guidelines for advanced clinical-radiological pre-orthodontic assessments and patient qualification for alveolar bone reconstructions.
Materials and methods
The study was conducted in accordance with the guidelines of the Declaration of Helsinki. Data were collected and analyzed with the approval of the Bioethics Committee of Wroclaw Medical University, Wrocław, Poland (approval No. KB-530/2021), and the study followed the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) checklist.21
Study group
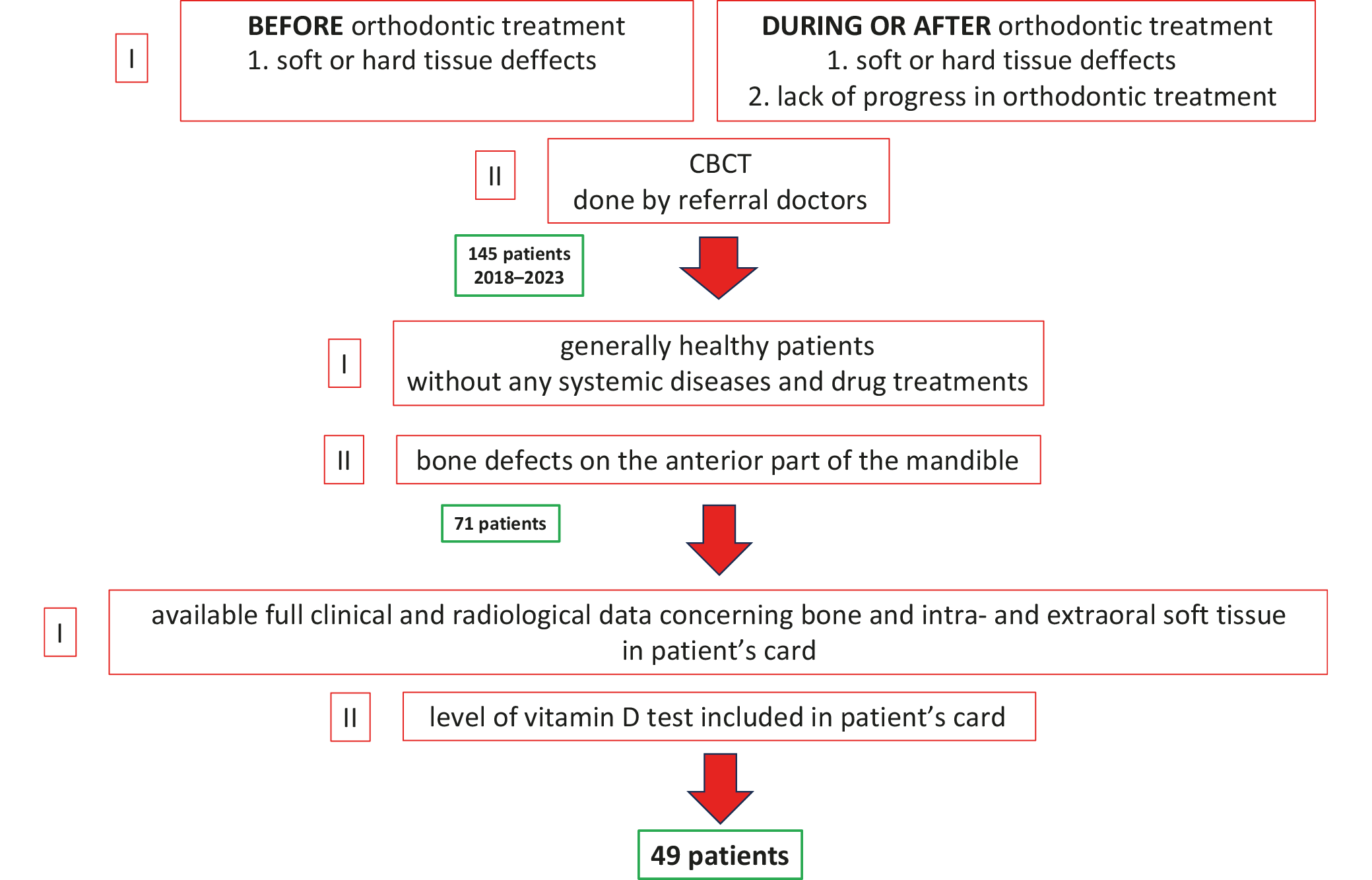
Between 2018 and 2023, 145 patients were referred to a private dental clinic in Wrocław, Poland, for consultation regarding soft or hard tissue prior to (group 1) and during or after (group 2) orthodontic treatment. Group 1 consisted of 16 patients, of whom 10 were women (62.5%), with a mean age of 35 years. Group 2 comprised 33 patients, with 28 women (84.8%) and a mean age of 39 years. As a result, a group of 49 patients was identified. The analysis included adult Caucasian patients of both genders who were referred as follows:
• Patients with pre-existing abnormalities of the dental arches prior to orthodontic treatment, such as visible recessions, loss of keratinized gingiva, palpable roots through the soft tissue, and periodontitis.
• Prolonged or complicated orthodontic treatment.
• Patients after partially successful orthodontic treatment, for whom procedures were postponed due to insufficient tooth movement or discontinued by the orthodontist because of emerging soft and/or hard tissue issues.
• Patients with full examination including CBCT scans prior to the start of a treatment with severe loss of teeth support.
Additional inclusion criteria for the study were generally healthy patients, with bone defect located in the anterior part of alveolar process and symphysis with remaining dentition.
All patients with any past systemic diseases and drug treatments that could affect bone tissue (e.g., Paget’s disease, osteoporosis, use of bisphosphonates, or denosumab), previous surgical or periodontal treatments in the anterior mandible, craniofacial anomalies, and previous trauma to the mandible were excluded from the study. All patients enrolled for study were qualified for the 3D allograft bone grafting procedure according to the method previously described.3, 4
Data collection
Data were gathered retrospectively from patients’ records, which included complete examination notes, clinical intra- and extraoral photographs and radiological CBCT scans. This subchapter is structured to reflect the methodology of data collection. The assessment of extra- and intraoral soft and hard tissues, the relationship between the dento-alveolar arches to teeth, and the relationship between the position of the upper maxilla with dentition as a part of craniofacial part of the skull with and O-C1 joint (atlanto-occipital joint) position were made by 2 different doctors independently independently and merged into 1 dataset. These parameters were chosen because of their possible mutual influence of musculo-fascial system on the condition of craniofacial part of the cranium. The visual representation of data collection is shown in Figure 1.
Radiological examination
The CBCT scans were acquired using the Pax Flex3D Vatech computed tomography radiography system (Vatech® Europe, Prague, Czech Republic). For the mandible center image, a field of view (FOV) of 80 mm in width and 50 mm in height was used, with a voxel size of 0.2 mm³. All images were analyzed using EzDent-i software (Vatech). Only CBCT scans that displayed the entire mandible and maxilla were included in the analysis.
Angle between the long axis of the tooth and the long axis of mandible
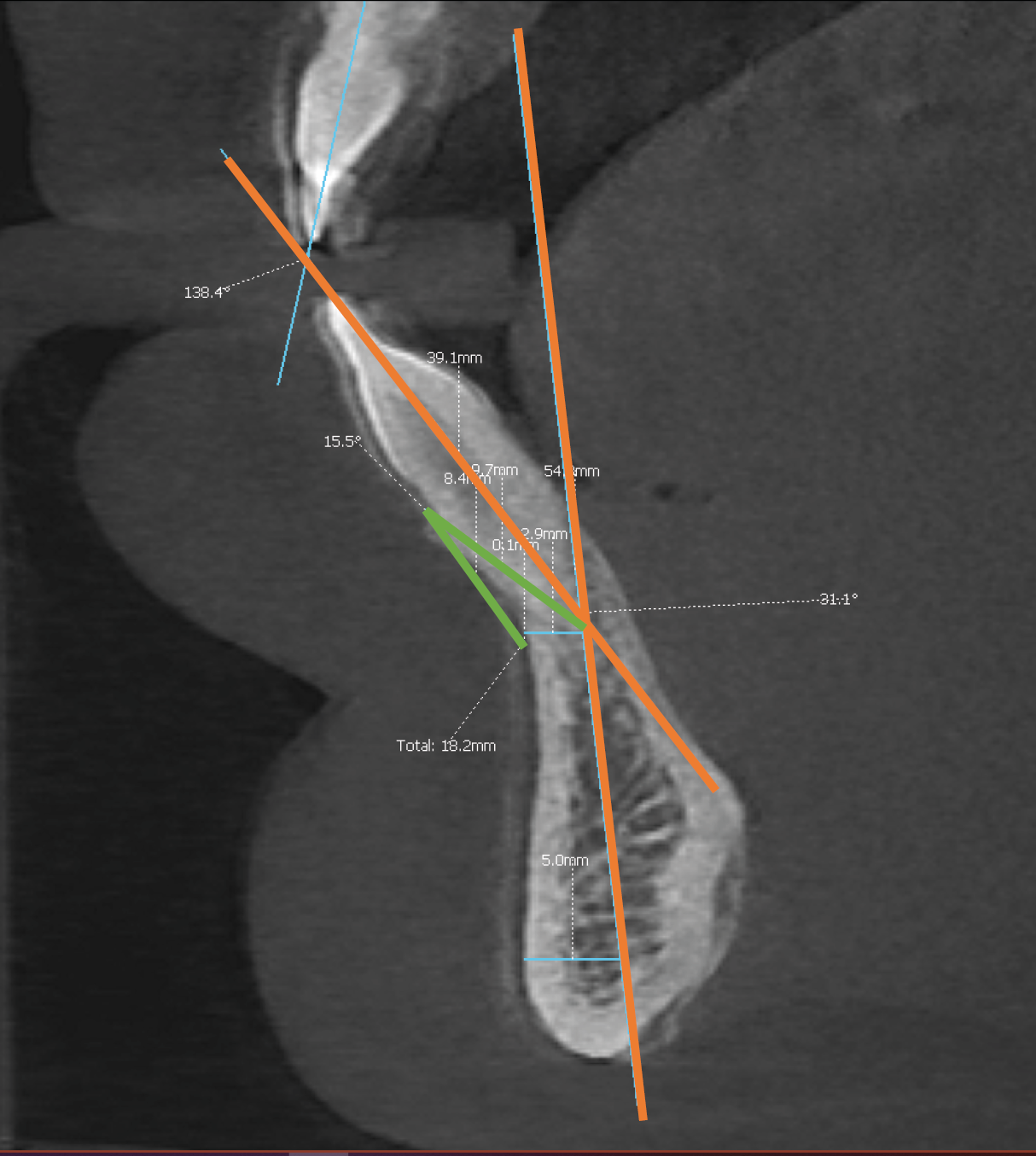
The angle between the long axis of the tooth and the long axis of the mandible (1:Ml) was measured to assess tooth inclination; a larger angle indicated a more protruded tooth. This angle was measured on the sagittal plane of the CBCT using software tools, with a mean value ranging between 10° and 15°.13 The long axis of the tooth was defined as the line connecting the tip of the crown to the apical point of the most anterior mandibular central incisor (Iia). The long axis of the mandible was determined by identifying 2 points on the mandible and drawing a line between them: the 1st point was located at half the width in the tooth’s apex region, and the 2nd was set 5 mm above the inferior border of the mandible (Gnathion (Gn)). The half-width point was also measured (Figure 2).
API-CEJ2-B angle
The API-CEJ2-B angle was measured to assess the remaining labial bone in front of the teeth. Long lines were drawn connecting the following points: the deepest point on the anterior concavity of the mandibular symphysis (point B), the apical point of the most anterior mandibular central incisor (Iia), and the point located 2 mm apical to the cementoenamel junction (CEJ) of the incisor (Figure 2), which reflects the sulcus depth.22
Classification of bone dehiscence
Examination of dehiscence was based on the sagittal plane of the CBCT, employing the classification system of Yang et al., as explained by Dominiak et al., to ensure accurate classification.5, 23 The highest labial and lingual points of the alveolar wall were determined to select the appropriate class and then compared to the positions of the CEJ and the tooth apex. The classification stages were modified to provide a more detailed description of Class II, highlighting various stages of dehiscence on both sides of the dental arch. Additionally, a new class (Class X) was introduced to describe dehiscence occurring simultaneously on both the labial and lingual sides.
Interincisal angle (1:1 angle)
The interincisal angle is defined as the angle between the long axes of the lower and upper incisors. Its mean value is approx. 122°, and it is used to assess the relationship between the lower and upper dental arches – particularly the protrusion of the incisors, which may indicate an insufficient bony base for the teeth. A decrease in this angle may suggest the need for tooth extraction as part of pre-orthodontic treatment.24
1:GoGn angle
The GoGn angle is defined as the angle between the line connecting Gnathion (Gn) and Gonion (Go) and the long axis of the lower incisor. Its average value is approx. 90°. This angle provides information about the inclination of the alveolar process and teeth relative to the GoGn line.25 It was measured on the sagittal plane of the entire area, which mimics a cephalometric X-ray. For optimal precision, the angle was measured using a protractor on a fixed screen image (Figure 3).26
OccP/GoGn angle
The angle between the occlusal plane (OccP) and the GoGn plane represents the inclination of the dental portion of the mandible relative to its base. Like the previous angle, it was measured using a protractor. For retrospective measurement on CBCT scans, a line was drawn from the tip of the lower incisor to the distal cusp of the lower first molar, and this line was compared to the GoGn line.
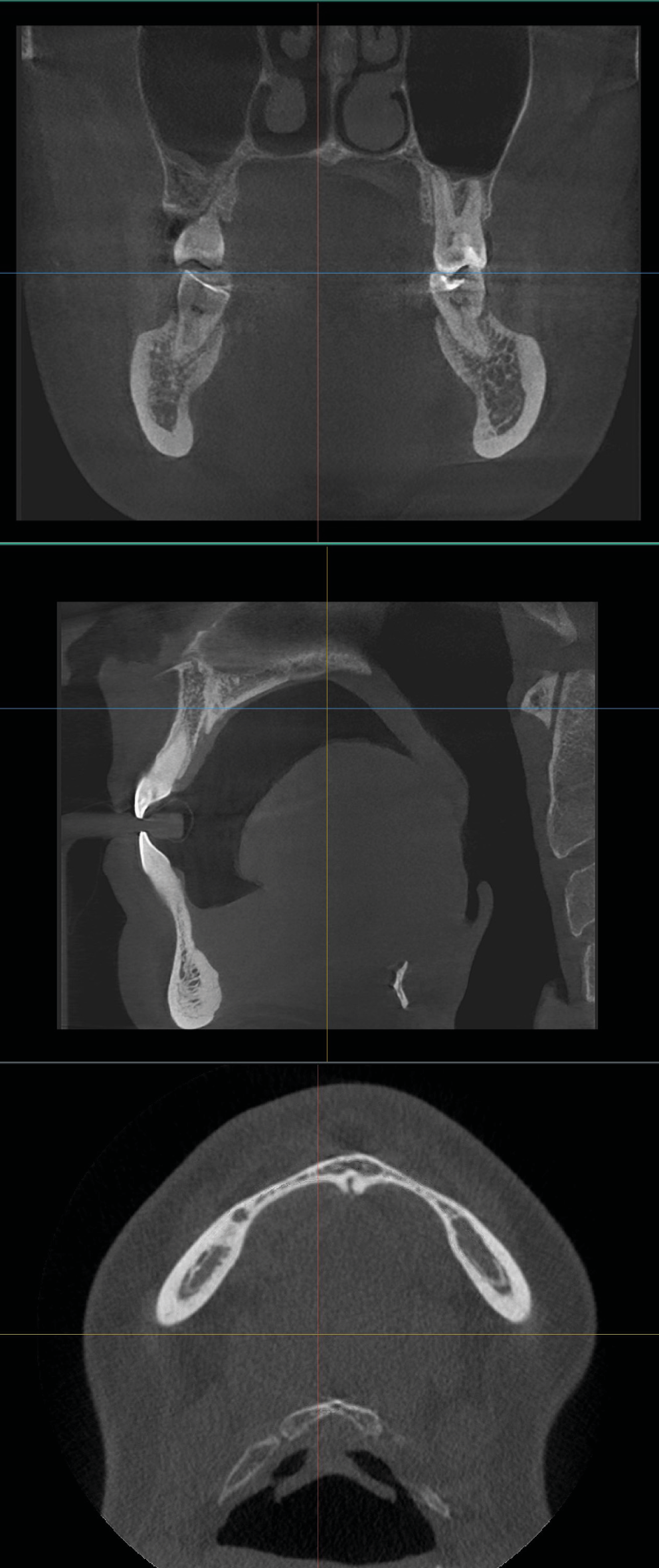
Anterior and lateral Stafne bone defects
The commonly known lateral or posterior Stafne bone defect is classified as a pseudocyst, with its origin attributed to either a salivary gland extension into the mandible or calcification of Meckel’s cartilage.27 In contrast, the anterior Stafne bone defect is less documented in the literature. It is located in the anterior region of the mandible, below the teeth and above the mylohyoid muscle.28 According to the 1993 classification, Stafne bone defects are divided into 4 types – the first 3 refer to posterior defects, while the 4th type represents the anterior Stafne bone defect (ASBD), which is explained as an insertion of the mylohyoid muscle.29 This deviation from normal bone structure should be considered during pre-orthodontic examinations, as it may indicate high muscle tension that could be problematic due to the tongue’s pushing pattern. Figure 4 illustrates both anterior and lateral Stafne bone defects.
Width of the mental muscle
The method for measuring the width of the mentalis muscle was proposed by Dominiak.22 Assessing this width helps estimate muscle tension and hyperactivity. In her method, a new landmark, point “D,” is defined on the soft tissue. To locate point D, a “GoGn” line is drawn between the Gnathion and Gonion points. Additionally, point “B” is identified as the deepest point on the mandibular concavity. Next, a line parallel to the GoGn line is drawn through point B, and its intersection with the soft tissue border marks point D. The width of the mentalis muscle on the sagittal plane is then defined as the distance between points B and D (B:D) (Figure 3).
Tongue position
Assessment of tongue position on CBCT scans was conducted on the midline sagittal plane. This approach allows for the visualization of the tongue, mylohyoid muscle, tongue frenulum, and the tongue’s resting position, which may provide insights into the patient’s breathing and swallowing patterns. Three classes have been established to categorize tongue positions: Class 0 – The tongue is positioned on the hard palate, with the entire dorsal surface in contact; Class 1 – The tongue is placed beneath the incisors; it may touch the palate, but not as extensively as in Class 0; Class 2 – The tongue rests at the bottom of the mouth.
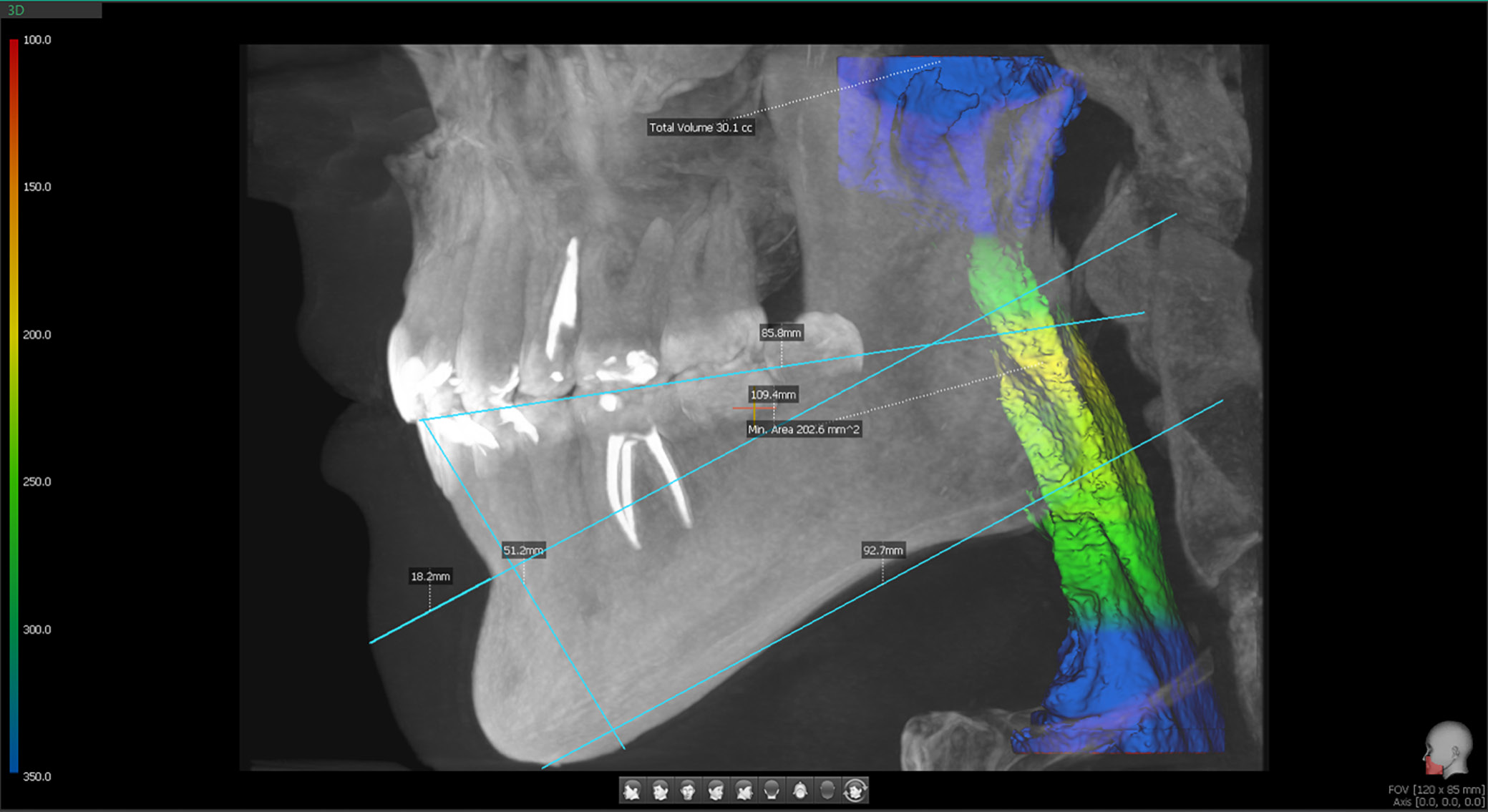
Volume of the airways
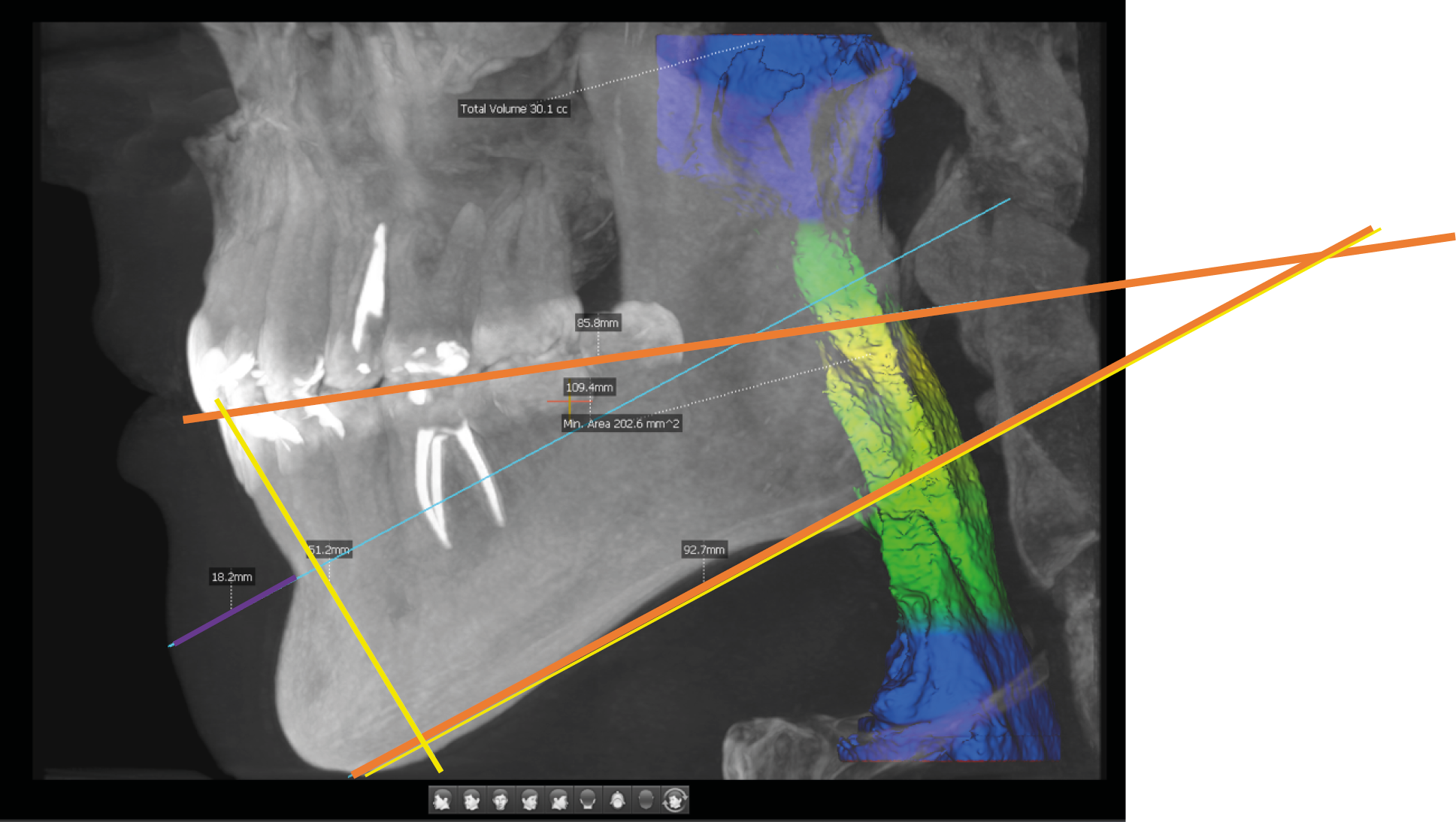
Airway measurement has become accessible to dentists through the increased use of CBCT. Thanks to built-in software, airway assessment is now one of the options available during routine X-ray examinations. It is reported – and as shown in Figure 5 below – that an airway capacity of approx. 200 mm² is considered satisfactory. To measure the airways, a CBCT scan with the full available field of view (80 mm in width and 50 mm in height) is required. Subsequently, the visible airway, extending from the nasopharynx to the sphincter, should be marked. It is known that airway narrowing is quite common in cases of malocclusion, especially in Class II malocclusion, where the retruded mandible reduces the space available for the tongue and decreases airway capacity.
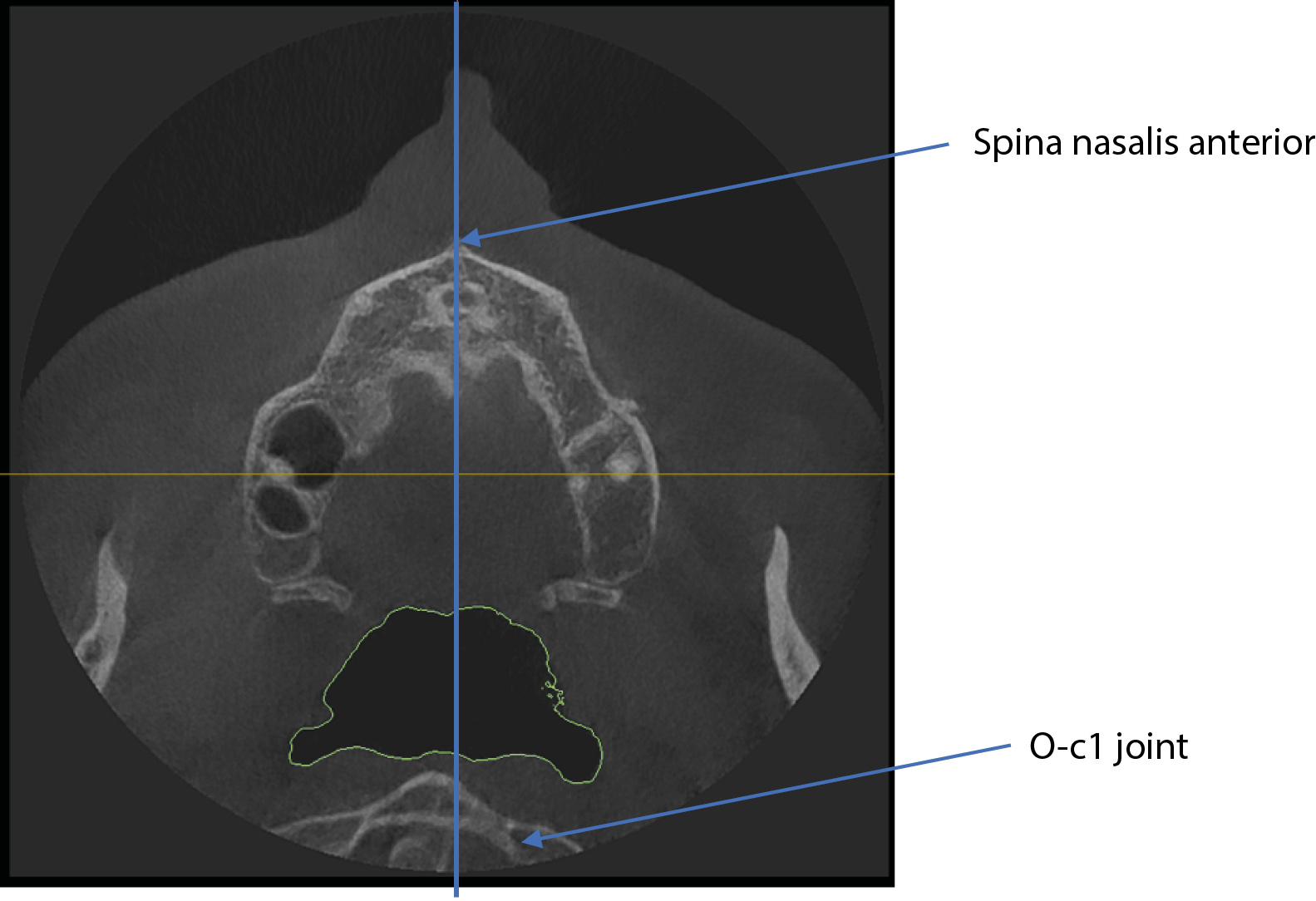
Abnormality in the position of the O-C1 joint
In addition to airway volume, the study investigated the correlation between lower airway capacity, dental abnormalities, and postural problems at a vertebral level. The deviation of the O-C1 (atlanto-occipital) joint was measured by automatically drawing a sagittal midline-using the spina nasalis and the sutura palatina media as reference points. Any displacement of the O-C1 spinous process relative to this midline was used to assess vertebral asymmetry. The methodology is illustrated in Figure 6.
Occlusal plane
Abnormalities and changes in the occlusal plane are among the most common issues in dentistry. The occlusal plane (OccP) can be altered over time due to wear, excessive biting force, bruxism, iatrogenic factors from dental procedures, or even congenital malocclusions. The occlusal plane is described in detail in point 6. If the cusps of the lower teeth align with the line following the curve of Spee, the occlusal plane is considered normal. If the curve of Spee is not maintained, the occlusal plane is classified as flat. If the curve of Spee is more pronounced, the occlusal plane is considered deepened. Finally, if the cusps of the premolars reach or extend above the line, the occlusal plane is referred to as a reverse occlusal plane (Figure 3).
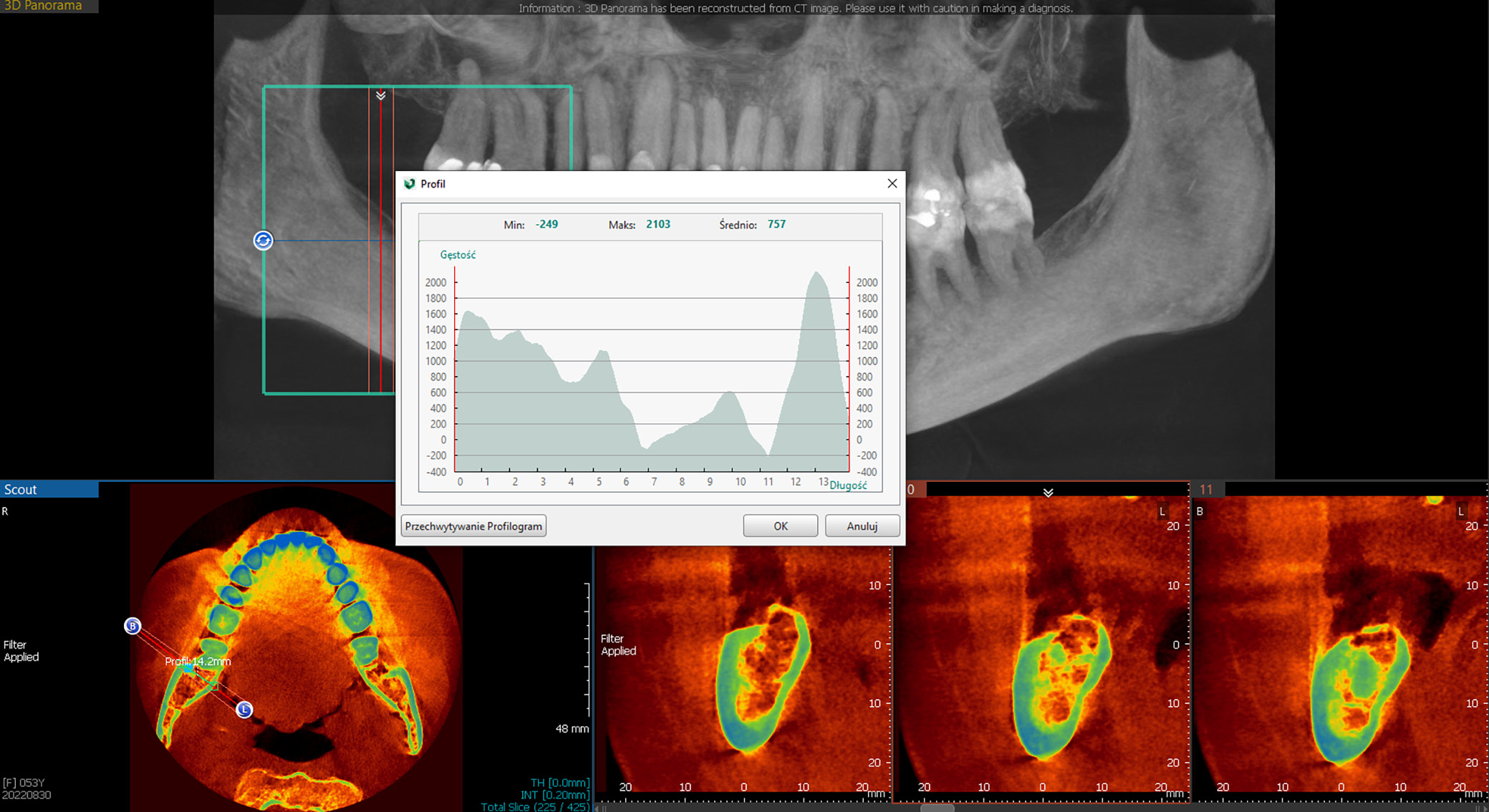
Bone marrow steatosis (BMS)
Measurement of this factor was enabled by the imaging software tools (Figure 7). It was quantified in Hounsfield units (HU), which are based on a calibrated grey-level scale of X-ray images. Originally, HU measurements were used to assess tissue density on CT scans; however, several authors have reported that CBCT images yield similar values.30, 31, 32 Nevertheless, it should be noted that these measurements are approximations that indicate the general direction in which tissue characteristics are changing, and they cannot yet be used with the same precision as CT scans. For example, compact bone typically measures between 662 and 1988 HU, spongy bone between 148 and 661 HU and fat between –205 and –51 HU. Measurements were consistently taken at the end of the retromolar triangle, at the level of the beginning of the ascending ramus of the mandible, using a specialized sub-option of the Vatech software.
Clinical intra- and extraoral photographs
Non-carious lesions
These lesions occur without bacterial interference and are classified as a loss of hard tissue around the CEJ with various morphologies.33 Their etiology is multifactorial; they can be caused by improper brushing techniques (particularly excessive force), erosive destruction or abfraction.34 In any case, understanding their origin is essential, as these lesions may affect orthodontic treatment.
Gingival recession
Gingival recession is characterized by the progressive loss of soft tissue, along with bone loss in the anterior region of the teeth. This condition was verified through clinical and radiological examinations in a retrospective study, which utilized clinical photographs and CBCT scans. Miller’s classification was employed to categorize the severity of the recession.6
Angle classification
To assess the presence of malocclusion, the classic Angle classification was used.35 When the Angle classification was not applicable, e.g., when a tooth was missing, the canine classification was used instead. The position of the teeth was examined using clinical photographs.
Faces’ profile type
To assess facial profile types, we distinguished between straight, oblique forward and oblique backward profiles. On clinical photographs, a vertical line was drawn from the Nasion, along with another line from the center of the iris, to create a biometric field. Two key points – Pogonion and Subnasale – were then evaluated in relation to this biometric field.
Examination notes
Orthodontic treatment
Patients were divided into 2 groups according to their treatment history: one group included patients before orthodontic treatment, and the other comprised those during or after orthodontic treatment.
Vitamin D3
Vitamin D3 levels and supplementation were assessed, as deficiency in vitamin D3 has been implicated in the development of malocclusion. The vitamin D3 level was determined using the VHC Vitamin-D-Test (Jungbrunnen–Fountain of Youth® GmbH, Rostock, Germany), a quantitative assay that employs immunochromatography to detect anti-25-OH-vitamin D monoclonal antibodies. Vitamin D3 levels were measured from capillary blood samples obtained via a finger prick collection.36
Statistical analyses
For quantitative variables, basic descriptive statistics were calculated, i.e., means (M), standard deviations (SD), minimum (Min), maximum (Max), medians (Me), and lower (Q1) and upper quartiles (Q3). In contingency tables, qualitative variables (nominal and ordinal) were presented as counts (n) and percentages (%). The Shapiro–Wilk test was used to confirm that the empirical distribution of quantitative variables fit the normal distribution. When quantitative data had a normal distribution, the t-test was used to check the statistical significance of differences in the mean values of quantitative variables between 2 independent groups, and when the data did not meet the assumptions of normality, the Mann–Whitney test was used. In the case of a larger number of groups, either analysis of variance and Tukey’s test were used as a post hoc test, or the Kruskal–Wallis (K–W) test and Dunn’s test were used as a post hoc test. The Pearson’s χ2 test with Yates’s correction or Fisher’s exact test were used to confirm the independence of 2 qualitative factors. Univariate and multivariate logistic regression analysis was used to estimate the probability of recession. Odds ratios (ORs) and their 95% confidence intervals (95% CIs) were estimated for statistically significant predictors of recession. For continuous variables, receiver operating characteristic (ROC) curve analysis and Youden index values were used to establish cutoff values. The strength and significance of correlations between 2 quantitative variables were assessed by calculating the Pearson’s r correlation coefficient or Spearman’s rho-rank correlation coefficient. All statistical analyses were performed at the significance level of 0.05 and presented in graphs as M and standard error (SE) or Me and interquartile range [Q1; Q3]. All statistical analyses were performed using STATISTICA v. 13.3 (TIBCO Software Inc., Palo Alto, USA).
In the comparisons of “volume of respiratory tract”, “API-CEJ2- B angle” and “B-D” 3 groups of patients differing in “position of the tongue in the resting position”, “vitamin D3 deficiency” and “classification of dehiscence” were used. In the first 2 cases, the distributions of residuals (deviations) in all 3 groups did not deviate from the normal distribution (Shapiro–Wilk test), and the variances were similar (as verified by the Levene’s test). In the 3rd case, the assumption of normality was not met, so the K–W test was used for comparisons, and the Dunn’s test was used as a post hoc test.
The variationally independent were not closely correlated with each other, which was checked using the variance inflation factor (VIF) index. No outliers were observed on the quantile–quantile (Q–Q) plots and residual histograms. Checking whether the assumption of linearity in the logit function was met involved analyzing residual plots, performing the Box–Tidwell test, and checking whether additional coefficients taking into account interactions between variables were statistically significant.
For the K–W test, post hoc multiple comparisons were performed using the Dunn’s test with Bonferroni correction. Univariate and multivariate logistic regression analysis was used to estimate the probability of recession (binary variable). Model parameters were estimated using the maximum likelihood method. The goodness-of-fit of the model to the observed data was verified using the Hosmer–Lemeshow test, and the statistical significance of individual independent variables was checked using the Wald test. Cutoff values for continuous variables were determined using ROC curve analysis and Youden index values. Odds ratios and their 95% CIs were calculated for statistically significant predictors.
Results of statistical analyses
Patients characteristic
This study included 49 patients who qualified for bone reconstruction using an individualized allogeneic bone graft. The participants’ ages ranged from 22 to 55 years, with a median age of 36 years, and the majority were women (77.6%). All variables are presented in Table 1.
Influence of orthodontic treatment
In the group of patients before orthodontic treatment, the average bone marrow steatosis was significantly lower compared to patients after treatment (–12 HU vs –137 HU, p = 0.010). A statistically significant relationship was observed between the position of the tongue in the resting position and the patient’s status due to orthodontic treatment (K–W test: p = 0.038). The tongue in the resting position between the incisors was significantly more common in the group of patients before orthodontic treatment (56.2% vs 21.2%, p = 0.014). The tongue stuck to the palate behind the upper incisors was more common among patients after orthodontic treatment, but this difference was borderline significant (36.4% vs 12.5%, p = 0.082). All interconnections are shown in Table 2.
Influence of vitamin D3 concentration
No statistically significant differences were observed among patients with varying vitamin D3 concentrations across the analyzed parameters (p > 0.05). All interconnections are detailed in Table 3.
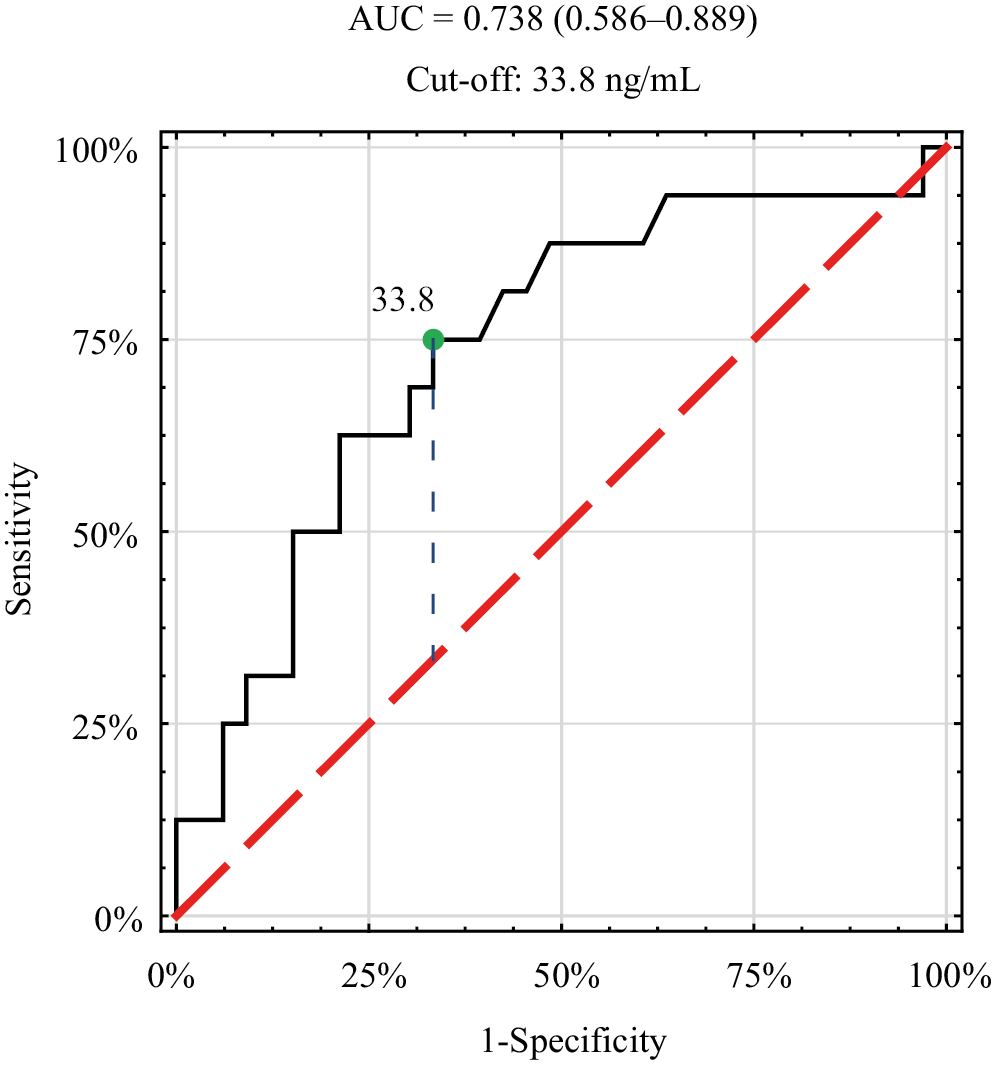
In this study, a significant dependence of vitamin D3 concentration on the position of the tongue in position 2 was observed. The ROC curve analysis (Figure 8) showed that the threshold value for the vitamin D3 concentration is 33.8 ng/mL, which means that when patients get this amount of the vitamin D3, they will put their tongues between the incisors.
Group A and group B patients were combined, and for this dichotomous division (A + B vs C), the optimal vitamin D₃ concentration threshold was determined using ROC curve analysis (Figure 8).
Table 4 contains calculations for the new division of patients according to vitamin D3 concentration. As a result, it turned out that there is a statistically significant relationship between the level of vitamin D3 concentration and gender, the width of the mentalis muscle and, of course, the position of the tongue in the resting position. Since there was a significant correlation between the width of the mentalis muscle and gender, a multivariate analysis was performed to determine independent predictors of the position of the tongue between the incisors (group C). It was found that the only independent factor differentiating patients according to the level of vitamin D3 concentration was the width of the mentalis muscle “B:D”.
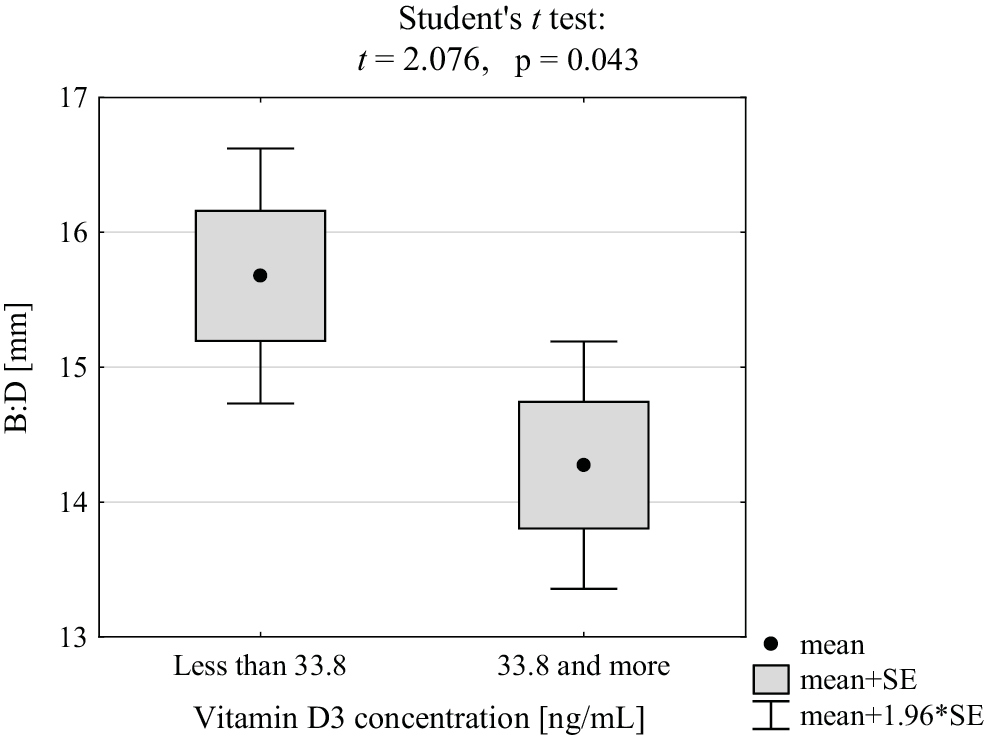
The average width of the mentalis muscle in women was smaller compared to men (14.6 mm vs 15.2 mm, p = 0.164), but the difference was borderline significant (Figure 9).
Correlation between width of mentalis muscle and dehiscence
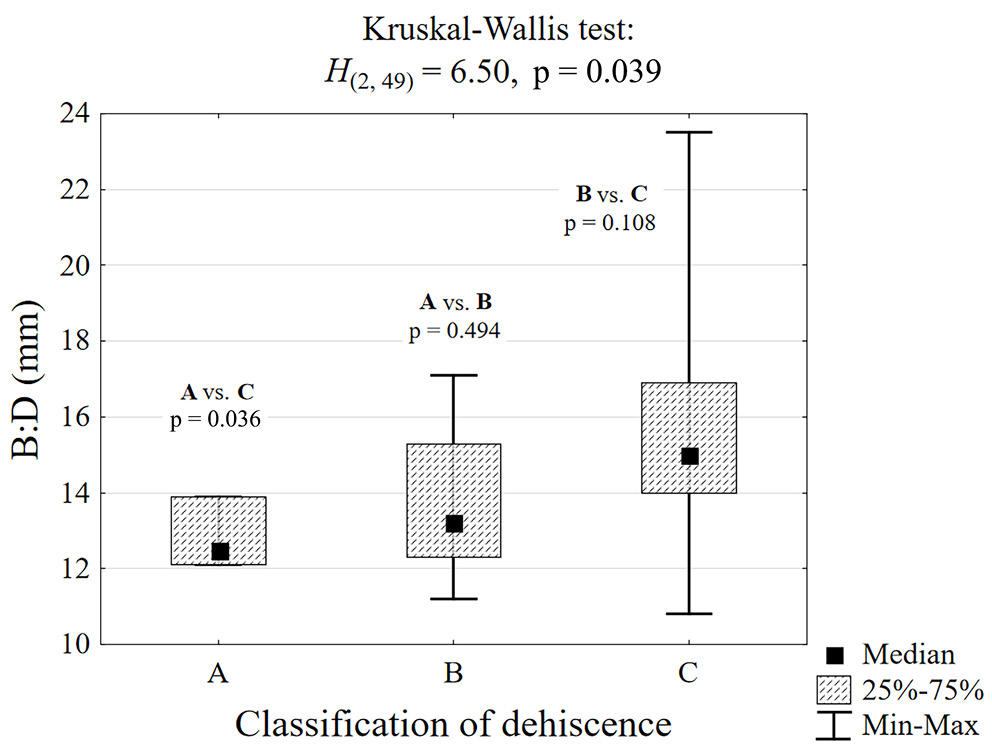
A statistically significant relationship (Figure 10) was observed between the width of the mentalis muscle and the dehiscence class. In patients with class C dehiscence, the mental width was significantly greater compared to class A patients (15.0 mm vs 12.5 mm, p = 0.036).
Correlation between tongue position and volume of respiratory tract
No statistically significant relationship was observed (p > 0.05). However, it was visible that around 2/3 of examined patients had some kind of an issue with muscular position of the tongue in the oral cavity (Table 5).
Correlation between OC-1 joint position to malocclusion, bone parameters, volume of respiratory tract, and recessions
A statistically significant negative correlation was observed between the O-c1 joint shift and the 1:Ml (rho = –0.330), API-CEJ2-B (rho = –0.319) and 1:GoGn (rho = –0.455) angles. An increase in the OccP:GoGn angle by 1° is accompanied by a decrease in the 1:GoGn angle by an average of 0.97°. The correlation between OccP:GoGn and volume of respiratory tract (mm2) was statistically insignificant (rho = 0.135, p = 0.262) (Table 6).
Correlation between the occlusal plane and malocclusion, mentalis muscle, angles and airway, tongue position, and Stafne defect
A statistically significant relationship was observed between the occlusal plane and the 1:Ml angle (p = 0.013; Table 7).
Determining critical values when a recession occurs
Among the 49 patients qualified for jawbone reconstruction, gingival recession was observed in 46 individuals (93.6%). Specifically, 19 patients (38.8%) exhibited recession only in the mandible, while 27 patients (55.1%) exhibited recession in both the mandible and the maxilla.
Patients were divided into 2 groups: group 1, consisting of patients with no mandibular gingival recession (Miller classes 0 and I), and group 2, consisting of patients with mandibular gingival recession (Miller classes II and higher). Both groups had similar sample sizes. The frequency of occurrence of the analyzed recession predictors in both groups was evaluated using Fisher’s exact test, and the results are presented in Table 8. Cutoff values for continuous quantitative variables were established based on ROC curve analysis.
In the univariate analysis, statistically significant predictors (stimulants) of recession were: female gender (90.0% vs 57.9%, p = 0.014), API-CEJ2-B angle ≤19.9° (76.7% vs 47.4%, p = 0.040), width of mental muscle ≥14.1 mm (76.7% vs 47.4%, p = 0.040), dehiscence on the lingual and vestibular side (93.3% vs 57.9%, p = 0.008), flat occlusal plane (50.0% vs 21.1%, p = 0.049), steatosis of mandibular bone marrow score less than or equal to 139 HU (60.0% vs 15.8%, p = 0.003), and vitamin D3 concentration ≥24.9 ng/mL (80.0% vs 52.6%, p = 0.048).
The odds of gingival recession are 6.5 greater in women (OR = 6.55), more than 3.5 times greater among patients with an API-CEJ2-B angle ≤19.9° (OR = 3.65), also more than 3.5 times greater among patients with the width of the mentalis muscle ≥14.1 mm (OR = 3.65), more than 10 times greater among patients with bone dehiscence on the lingual and vestibular sides (OR = 10.2), almost 4 times greater among patients with a flat occlusal plane (OR = 3.75), 8 times higher among patients with steatosis of mandibular bone marrow score less than or equal to –139 HU (OR = 8.00), and 3.5 times higher among patients with vitamin D3 concentration ≥24.9 ng/mL (OR = 3.60).
Due to the significant correlations between some recession risk factors (e.g., female gender and width of mentalis muscle), a multivariate logistic regression analysis was performed to determine independent predictors of recession.
In the logistic regression analysis, the recession variable was the dependent variable, where the value of 1 meant the occurrence of gingival recession at the level of at least Miller class II, and the value of 0 – no recession or class I recession. The remaining variables served as independent variables (predictors). The results are presented in Table 9, which highlights significant results at the p < 0.05 level.
Dichotomous independent variables were variables significant in univariate analysis at the p < 0.1 level.
In multivariate logistic regression analysis, independent predictors of gingival recession were: female gender, API-CEJ2-B angle ≤19.9°, dehiscence on both sides (DBS), flat occlusal plane, and steatosis of mandibular bone marrow score less than –139 HU.
The logistic regression equation used to predict the probability of gum recession takes the following logit form:
logit Pr{Recession = 1|X} = –6.96 + 2.62 × (Female) + 3.34 × (DBS) + 2.49 × (OPF) + 2.06 × (API-CEJ2-B ≤ 19.9°) + 2.00 × (SBM ≤ –139 HU)
For the cutoff value of the logistic model: Pr = 0.61, the sensitivity is Sens. = 0.933, specificity Spec. = 0.842, accuracy Acc. = 0.900, PPV = 0.90, NPV = 0.89 and LR(+) = 5.91.
Discussion
Bone density is not only crucial in implantology, but it can be also a significant factor in oral surgery and orthodontics as well. Knowing patient’s bone density, proper methodology might be implemented, which reduces chances of complications. Nowadays, the most common classification of bone density is the one presented by Misch, which evaluated ratio between trabecular and spongious bone.37 More common usage of CT allows to assess density of tissues using HU. Patients with a history of an orthodontic treatment who were evaluated during our study usually presented some kind of complications, for example teeth excess mobility or gingival recessions and bone dehiscence. Most of orthodontic complications are somehow related to bone issues. In our study, the majority of the participants were women. In our opinion, it might be explained firstly with other studies’ findings that periodontal phenotype in women is generally thinner than in males, and consequently the buccal cortical plate is more exposed and predisposed to dehiscence in case of orthodontic treatment or malocclusion. Behavioral studies38 indicate that women are more likely to seek dental services, adhere to medical instructions and pay for dental visits, and they are also more inclined to undergo expensive surgical treatments.39 Comparing patients who visited the dental office before and after orthodontic treatment, the post-treatment group exhibited statistically lower bone density (measured in HU) than the pre-treatment group (–12 ±195 to –137 ±190). These results are similar to those obtained by other researchers.40, 41, 42 On the contrary, some studies have demonstrated that bone density may increase after orthodontic treatment due to the remodeling effects associated with tooth movement.43, 44 However, only a limited number of factors have been shown to affect bone density, particularly in the lateral part of the mandible. One such factor is bone steatosis. In the literature, early stages of steatosis are described as nonbacterial osteomyelitis of the mandible, which should be differentiated from conditions such as sarcoma, Ewing sarcoma and Langerhans cell histiocytosis. The etiology is considered an autoinflammatory disorder characterized by the hyperactivation of the immune system.45
Lower density is also visible in the course of hemorrhagic cyst and all types of dysplasia. Another factor is the level of vitamin D. More and more studies show or confirm correlation between its deficiency and tissue functioning. Vitamin D3 influences bone remodeling and muscles activity, has an anti-inflammatory effect and influences autoimmune diseases. As vitamin D3 receptors are present in muscle tissue, its higher amount will allow muscles to work with less contraction and more resilience. It is shown in our results as a better tongue position and slimer mentalis muscle in people with vitamin D3 concentration in serum over 33.8 ng/mL, which is similar level to the mean value – 30–100 ng/mL.46, 47, 48 However, we found the tendency to lowering of the API-CEJ2-B with lowering of vitamin D serum concentration (without statistically important significance). This may lead to the conclusion that with lower concentration of vitamin D, the lesser thickness of labial bone wil be present, as it is visible in the group C <20 ng/mL API-CEJ2-B reach only 17.5°. These findings are comparable to those of Leszczyszyn et al.14, who suggested that low concentrations of vitamin D3 are associated with a significantly increased risk of recession. They also found that low vitamin D levels correlate with crowding in the upper jaw, crossbite and narrowing of the upper arch. Furthermore, in another publication, the constructed model of multiple regression for parameters which influence significantly gingival recession (API-CEJ2-B, CEJ2-ID, age) allowed to explain their potential recession-causing influence in 72% chance of the recession occurence.49
Atypical tongue position may be a problem by itself or it can be connected with malocclusion (e.g., open bite). It is known that during orthodontic therapy, tongue position is crucial for the long-term results, so during or even before the treatment, patients are referred to the specialist or trained by the orthodontist. It is therefore not surprising that better tongue position is observed after orthodontic treatment.50, 51 There is no significant correlation between tongue position and the capacity of the airways. It is a similar result to the one obtained by the Chauhan et al.,52 who did not find such correlation as well.
Although the anterior Stafne defect may be attributed to hyperactivity of the mylohyoid muscle, our study did not find a statistically significant association between this defect and tongue position in the oral cavity. Therefore, it can be concluded that myofunctional disorders do not have a major impact on this poorly documented abnormality. However, the results of correlation between position shift of first cervical vertebrae and shape of the body of mandible with teeth inclination should be discussed in more detail. It is well known that increased tension of head and neck muscles might lead to orofacial pain and muscular rehabilitation may decrease patient’s pain.53 Therefore, it should be possible to interconnect the incorrect position of Oc-1 joint, which is caused most likely with abnormal head position, with increased tension of the muscle, larger teeth inclination and with larger posterioration of the mandible (which might lead to temporomandibular joints disorders). Important results were obtained by Olchowy et al.,54 who investigated masseter muscle stiffness and its rehabilitation by standard masticatory muscle therapy involving manual therapy and splint occlusal stabilization. The masseter stiffness has been measured by shear wave elastography. They stated that the above treatment has significant impact in pain reduction. Those promising result are similar to ours – that manual therapy might be a key factor in therapy of craniofacial area.
The etiological factors of gingival recession are well documented. Common factors include gender, toothbrushing techniques, improper tooth positioning, as well as systemic disorders and lifestyle habits. In contrast to other publications, in our study, women had gingival recession 6 times more often than men.55, 56, 57 Similar to the study by Cortellini and Bissada, tooth position and width of the buccal plate is important factor during genesis of the recession. API-CEJ2-B angle indicates remaining labial wall of alveolar part of mandible. With lower value of the angle, chances of the recession increase, and when the value is lower than 19.9°, chances of the recession are higher by 3.5 times.58 An even more important aspect is the appearance of the bone dehiscence on both sides of the tooth, which induce chances of the gingival recession up to 10 times; this factor is not discussed enough in the literature A high frenulum is one factor that increases the risk of gingival recession.59 Our study confirms this association: a wider mental muscle, which is linked to the frenulum attachment position due to its effect on vestibular depth, transmits greater forces to the gingiva, leading to pull syndrome. In another paper, it was stated as well that width of mentalis muscle significantly correlates with appearance of the dehiscences.22 Occlusal plane and occlusal trauma is another important factor of the gingival migration and flat occlusal plane indicates more pathological contacts between dentitions. Our results are similar to findings presented in other studies.60, 61
Systemic disorders are known to influence gingival recession, and their impact is increasingly being explored. It was presented by Jepsen et al. in the recent study.62 This association is also evident in our study. As steatosis of the bone marrow increases the chances for the recession by 8 times, it has to be seen as inflammatory process showing deeper problems with the system. In contrast to other researchers’ results, in our study, data indicate 3.5 times higher chances of ginigval recession as the concetration of the vitamin D is higher than 24.9 ng/mL63; however, it concerns a specific group of patients, because these patients are prepared to the regenerative surgery with allogenic bone graft and supplementation of the vitamin D3 is a part of preoperative pharmacology.
The numerous findings obtained from CBCT image assessments clearly demonstrate that a wealth of information – reflected in basic cephalometric measurements – should be analyzed before beginning orthodontic treatment. In today’s increasingly digital world, we should embrace the benefits that digitalization offers in dental examinations. Other researchers have reached a similar conclusion, noting that digitalization allows for the collection of more comprehensive treatment-related information – even in the early stages of potential disorders – than traditional standalone X-ray imaging.64
Limitations
One limitation of this study is that the retrospective selection process may have introduced selection bias. Additionally, no initial pre-orthodontic variables were analyzed; therefore, factors such as the amount, direction or speed of orthodontic tooth movement were not considered. Furthermore, assessing tongue position on a single CBCT scan may not accurately reflect its actual position. The study was conducted exclusively on a group of patients undergoing augmentation of the dentulous part of the mandible with an allogenic bone block, all of whom had a thin gingival biotype and existing recessions. There was no control group of “healthy patients,” and in some cases, patients without orthodontic treatment might have genetically or functionally determined changes that influence the reduction of the mandibular bone base. Consequently, the obtained values may differ from those in the general population. Comparing these results with data from individuals with a thick or normal biotype might provide a better assessment of the predisposition to these changes. Moreover, there is a limited number of studies on 3D bone allograft procedures performed in the mandible, and to the best of our knowledge, none have specifically focused on patient characteristics, which hampers meaningful comparisons with other findings.
Conclusions
The main purpose of this article was to shed some light on the rather serious consequences that may result from ignorant orthodontic treatment or not starting the treatment in a difficult situation without proper pre-orthodontic treatment based on surgical grafting of soft and hard tissues. Patients referred for the regenerative treatment with allogenic bone block usually had already undergone long treatment, which could be much shorter if orthodontists would make full examination, with CBCT visualization as well. More thorough results give the most important feedback, especially for the patients, who usually ask if their complications are less likely to have happened if they had not had the orthodontic treatment. The answer is complex, but statistical analysis gives a hint that there is no significant difference between pre- and post-treatment patients. Their problem might be congenital or caused by interconnection between many internal and external factors. Sometimes, it is impossible to avoid these factors. However if they are diagnosed early, it will be easier to solve these problems. The way of conducting pre-orthodontic examination presented in Materials and Methods section, added to classical cephalometric and dental arches models measurements, might be treated as guideline for avoiding complications. Orthodontic treatment should be considered as a complex one that often needs long preparation, and should include oral surgeon, restorative dentist, physiotherapist, and neuro-speech therapist.
Data Availability Statement
The datasets supporting the findings of the current study are openly available in Zenodo at https://doi.org/10.5281/zenodo.13869897.
Consent for publication
Not applicable.
Use of AI and AI-assisted technologies
Not applicable.