Abstract
Background. Most patients with chest wall deformities have a negative body image, which affects their self-esteem and quality of life (QoL).
Objectives. The aim of this study was to evaluate changes in patients’ QoL after minimally invasive repair of pectus excavatum (MIRPE).
Materials and methods. A prospective, single-center study was conducted between 2019 and 2023. We included 20 pediatric patients at a median age of 15 years and 9 months who underwent MIRPE. Two QoL questionnaires were used: the KIDSCREEN-52 and the EQ-5D-Y. The data were statistically analyzed with the Wilcoxon and Mann–Whitney tests. All patients and their parents were asked to complete questionnaires preoperatively and 12 months after surgical treatment.
Results. All patients were followed up during the 12-month study period. The study group was comprised of 65% male patients. The median Haller index was 5.0 standard deviation (SD) = 1.58). The assessment of general health condition was higher among the boys (with postoperative improvement), though this finding was not statistically significant. Routine daily activities were easier for all patients after MIRPE (p = 0.048). The patients showed improved physical activity (p = 0.038) and psychological wellbeing (p = 0.013) after elevation of the anterior chest wall. There was no impact on relations with parents, free time or school environment, but we found better patient contact with peers in the postoperative period. A high correlation was confirmed between the parents’ and the patients’ responses in each questionnaire.
Conclusions. Chest wall deformities can have a strong impact on the patient’s wellbeing, which is a very important part of psychological development in adolescents. Our study showed that improved QoL should be always considered as an indication for surgical treatment of chest wall deformities in children.
Key words: quality of life, pectus excavatum, thoracic wall, adolescent health, health-related quality of life
Background
Pectus excavatum (PE) is a congenital chest wall anomaly characterized by an anterior depression of the sternum and ribs with an incidence of 1:1,000 in children.1 Pectus excavatum can present at an early age, but commonly occurs during the rapid physiological growth associated with puberty.2
A negative body image is found in most patients with chest wall deformities, which affects their self-esteem and quality of life (QoL).3 Many patients reduce their daily activities to avoid the embarrassment and fear of feeling abnormal compared to their peers. Cosmetic complaints are still the main indication for surgical treatment.4
The main goal of PE correction is to improve the patient’s self-esteem, body image and physical difficulties.5, 6 Currently, the “gold standard” surgical treatment for PE is the Nuss procedure. The aim of this surgery was to elevate the anterior chest wall and stabilize the sternum in a neutral position. This method uses the elasticity of the chest wall in adolescents, allowing for successful remodeling over time.7 Patient satisfaction and good long-term outcomes have been reported following minimally invasive repairs of PE (MIRPE) in children and adults.
Objectives
The aim of this study was to investigate whether MIRPE improves QoL and overall satisfaction in adolescents.
Material and methods
Study design
We conducted a prospective study between October 2019 and August 2023. All patients were children and underwent MIRPE with titanium bars and titanium stabilizers (ChM Sp. z o.o., Lewickie, Poland). All patients over the age of 16 years gave informed consent, as did their parents. In total, 20 patients were included in the study. The mean age was 15 years and 9 months (range: 13–17.8; SD = 1.48), with 65% of them being male. All patients underwent a Nuss procedure for PE.
The responses to the EQ-5D-Y questionnaire were compared between the male (n = 13) and female (n = 7) groups. Each patient and their parents completed the questionnaire before surgery and 12 months afterwards. Each dimension in the questionnaire was analyzed.
The study was approved by the Institutional Bioethics Board of Collegium Medicum UMK in Bydgoszcz, Poland (approval No. KB 710/2019). This study applied the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement.
Clinical information
The minimal age for inclusion was 12 years. Patients with coexisting chest wall anomalies, congenital heart disease, pulmonary disease, or a history of cardiac/thoracic surgery were excluded from the study.
All operations were performed by the same pediatric surgeon. The operative technique was similar in every patient. All MIRPE procedures were performed under general anesthesia. A bilateral oblique skin incision was made in an anterior axillary line on both sides of the chest wall after the points of deepest deformity were identified. Subcutaneous tunnels were created bilaterally. A 5-mm trocar was introduced into the right pleural cavity and the procedure was performed under thoracoscopic visualization. A dedicated dissector was inserted from the right side of the chest, going across the anterior mediastinum to the left side. A titanium bar was fixed to the tip of the dissector and inserted when the dissector was removed from the chest. Next, the bar was rotated 180 degrees and short stabilizers were implanted at each tip of each bar. Additional bars were placed in a similar approach as needed to ensure appropriate correction. The pneumothorax was evacuated with tube connected to the thoracoscopic port under a water seal. Lung expansion and bar position were always confirmed for about 6 h postoperatively. The bar removal was scheduled for 3 years after the Nuss procedure. Postoperative pain management was based on a local analgesia protocol. Each patient was discharged with a well-controlled oral pain medication.
Quality of life assessment
The patients were examined with 2 standardized QoL protocols – preoperatively and 1 year postoperatively. The 1st instrument was the EQ-5D-Y questionnaire, which is a tool for measuring health-related QoL in the context of cost-effectiveness. It is designed to be completed by children and adolescents. The EQ-5D-Y descriptive system consists of 5 dimensions: “mobility”, “looking after myself”, “doing usual activities”, “having pain or discomfort”, and “feeling worried, sad or unhappy”. Each dimension has 3 levels: “no problem”, “some problems” and “a lot of problems”.8, 9
The 2nd QoL assessment tool was the KIDSCREEN-52 questionnaire. This instrument is intended to provide a multidimensional analysis of health-related QoL in children. It is divided into 10 main domains: “physical well-being”, “psychological well-being”, “mood and emotions”, “self-perception”, “autonomy”, “parental relations and home life”, “financial resources”, “peers and social support”, “school environment”, and “bullying”. We used 2 types of the KIDSCREEN-52 questionnaire designed for patients between 8 and 18 years old and for parents.10
Statistical analyses
Statistical analysis was carried out using SPSS for Windows v. 12.0 (SPSS Inc., Chicago, USA). The Wilcoxon test was used to assess the significance of differences between preoperative and postoperative results and between parents’ and patients’ responses. The Mann–Whitney test was used to compare preoperative and postoperative results between the male and female groups. The distribution of the data was assessed using the Shapiro–Wilk test. Due to the non-normal distribution, the analysis was performed using nonparametric tests. A p-value <0.05 was considered a significant result.
Results
The patients’ general characteristics are presented in Table 1.
Preoperative and postoperative evaluation using EQ-5D-Y was completed by parents and patients, divided into a male and a female group. The results of this analysis are presented in Table 2.
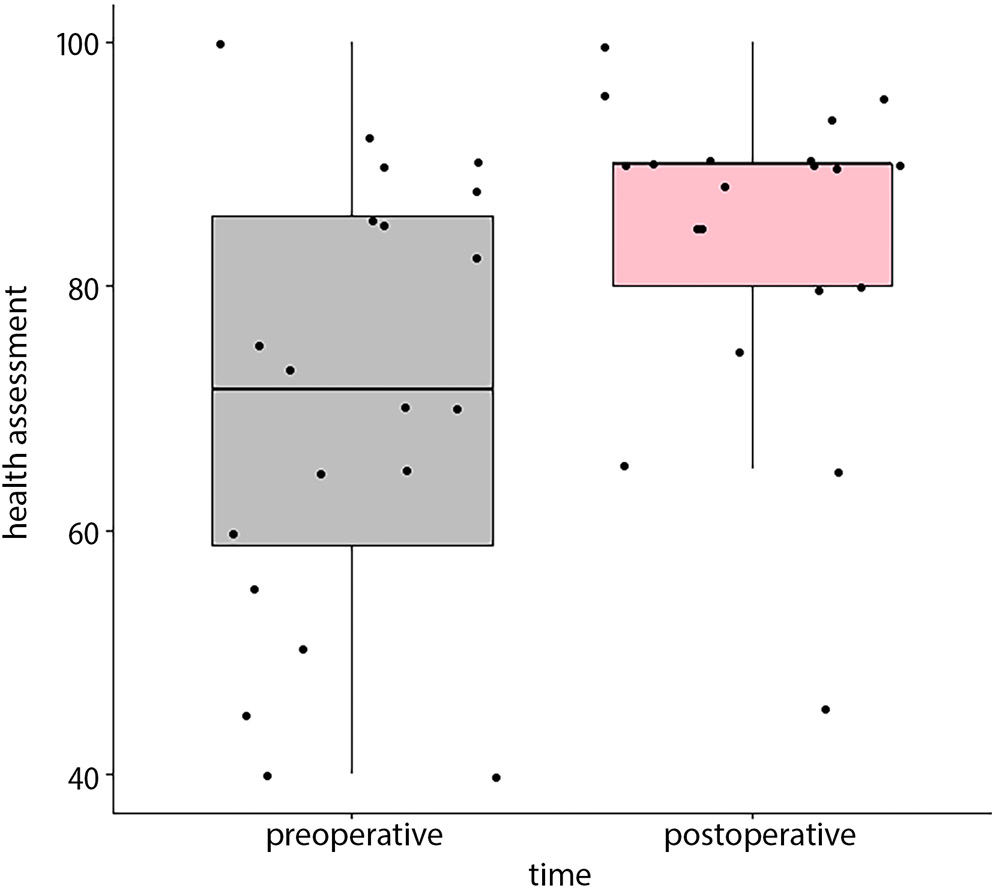
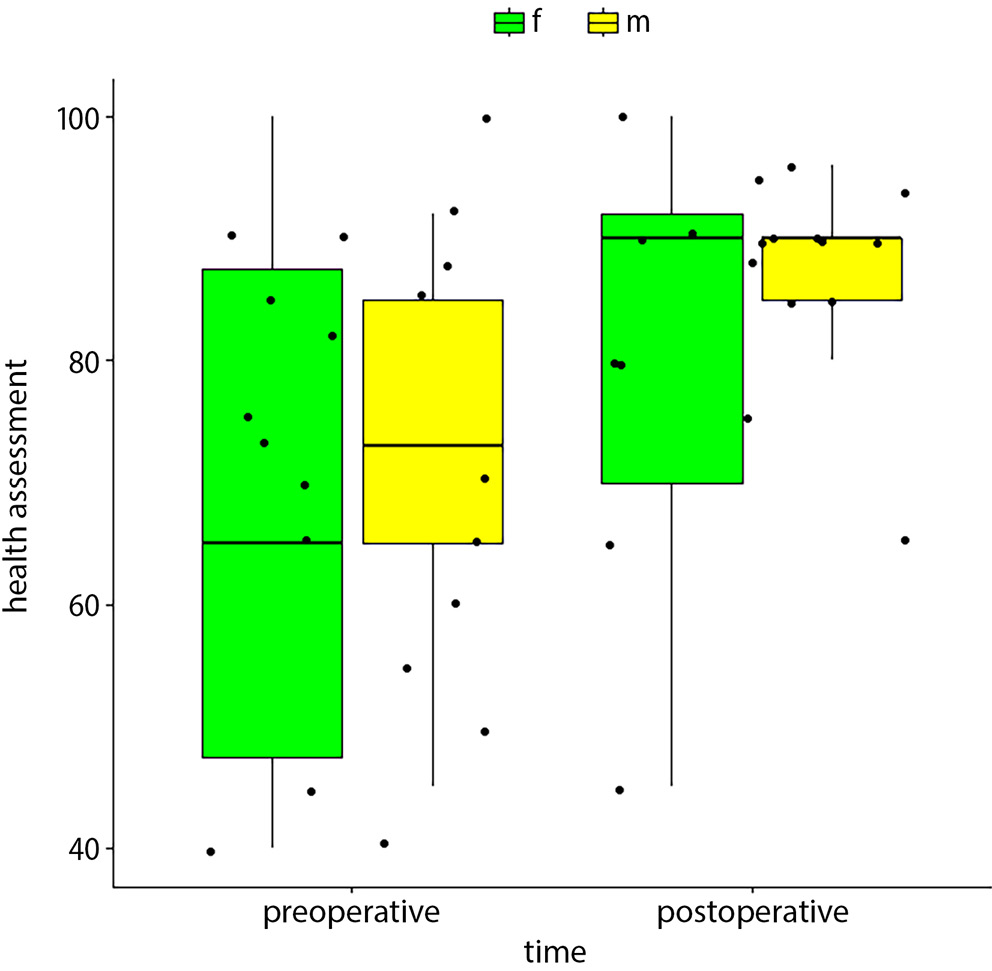
No male patients declared problems with mobility in either the preoperative or postoperative evaluation. Preoperative problems with mobility were more pronounced in girls than boys (p = 0.048), with no differences after surgical treatment. Daily routine activities were easier for patients postoperatively, mainly among the boys (mean = 1.0 vs 1.29; p = 0.048). There were no differences in the dimension of anxiety and “feeling sad” among the girls, but this indicator was higher in the postoperative period than in the group of “boys” (mean = 1.71 vs 1.15; p = 0.048). We did not reveal any important differences in postoperative mobility, perioperative “looking after myself” or “feeling pain and discomfort”, and daily activities. The boys’ assessments of their general health condition were higher (with postoperative improvement), though this finding was not statistically significant (Figure 1, Figure 2).
A comparative analysis of preoperative and postoperative results in patients with PE using the KIDSCREEN-52 questionnaire was performed. We also analyzed the postoperative responses of children and parents. The results are presented in Table 3, Table 4.
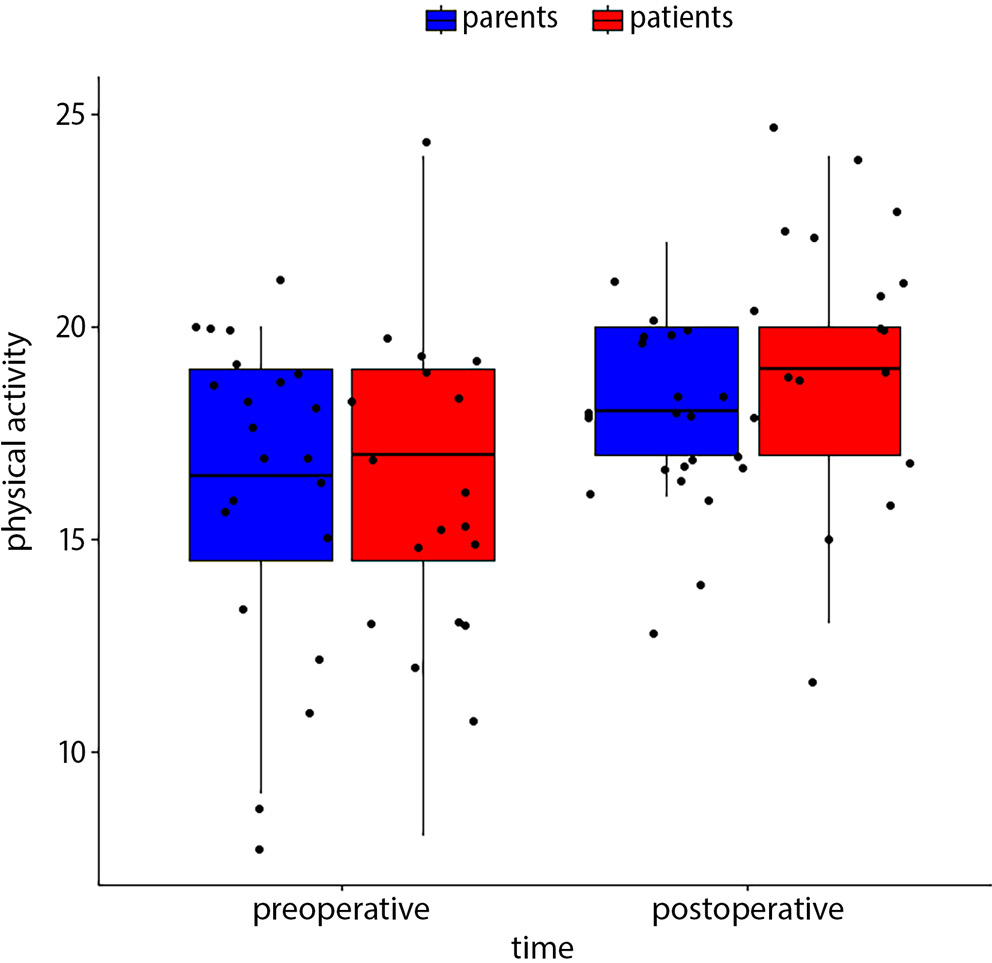
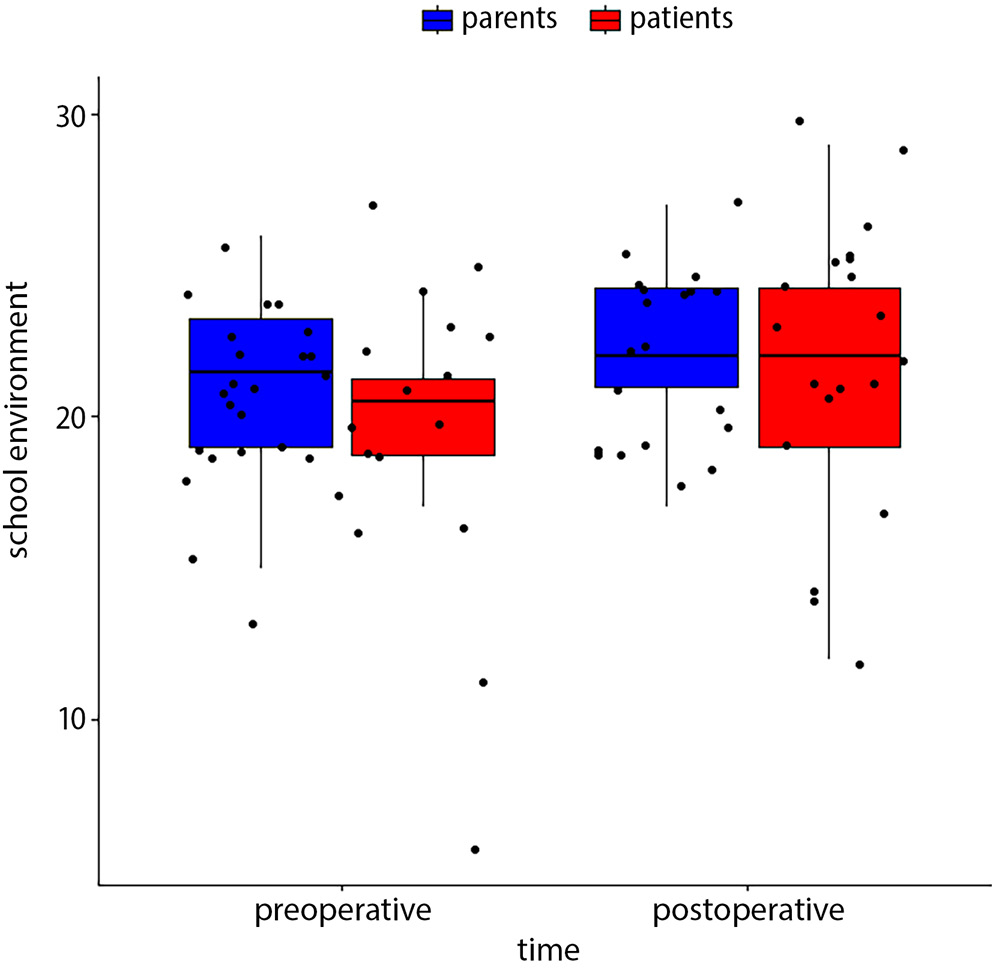
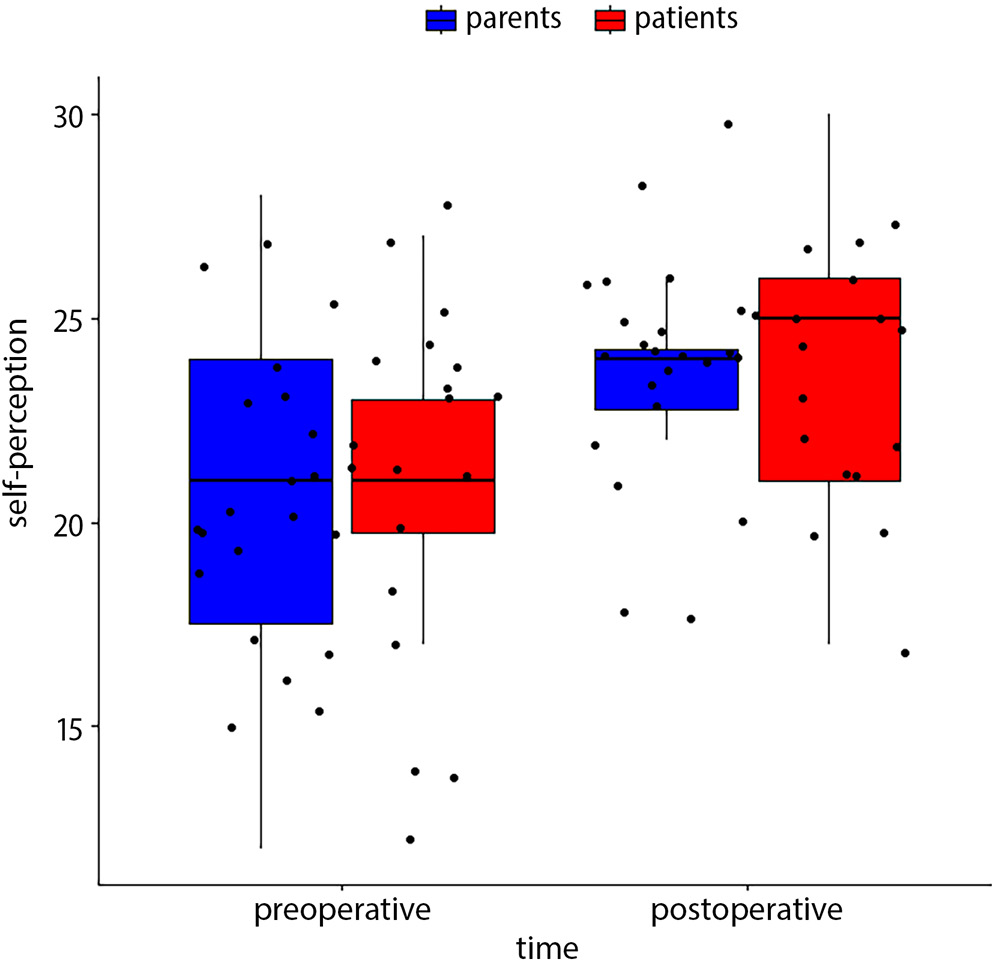
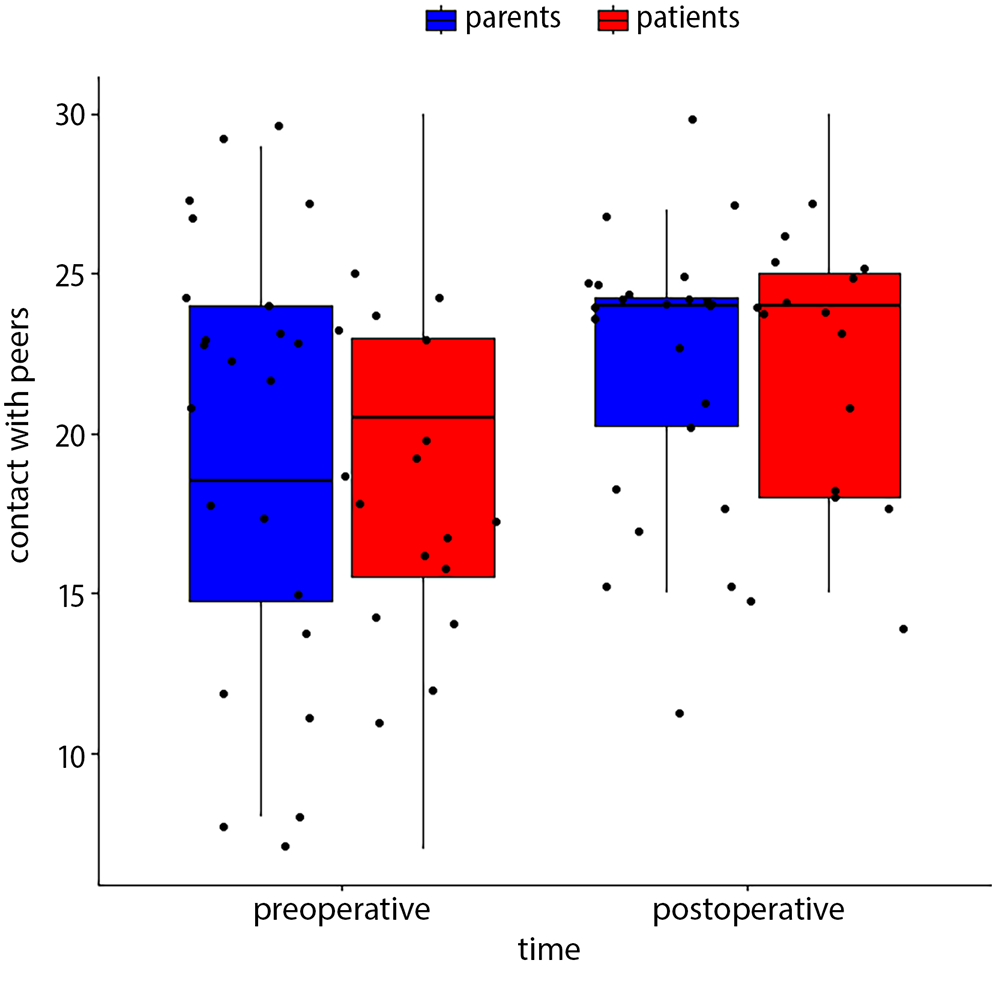
Following the MIRPE procedure, patients exhibited increased levels of physical activity (Figure 3) (18.65 vs 16.50; p = 0.038). Improvement in psychological wellbeing was also reported in the postoperative period (23.75 vs 21.05; p = 0.013). There were no differences in self-perception, free time, parental relations and home life, or financial problems. Also, there was no impact on school environment or bullying, but the patients reported better contact with peers after the operation (22.15 vs 19.20; p = 0.02) (Figure 4). Our study found worse general mood after correction of PE than before the operation (11.0 vs 13.65; p = 0.023). In the authors’ opinion, this was probably caused by typical mood variability in adolescents, especially since the improvement in general psychological wellbeing during the postoperative period was revealed to be statistically significant (p = 0.013).
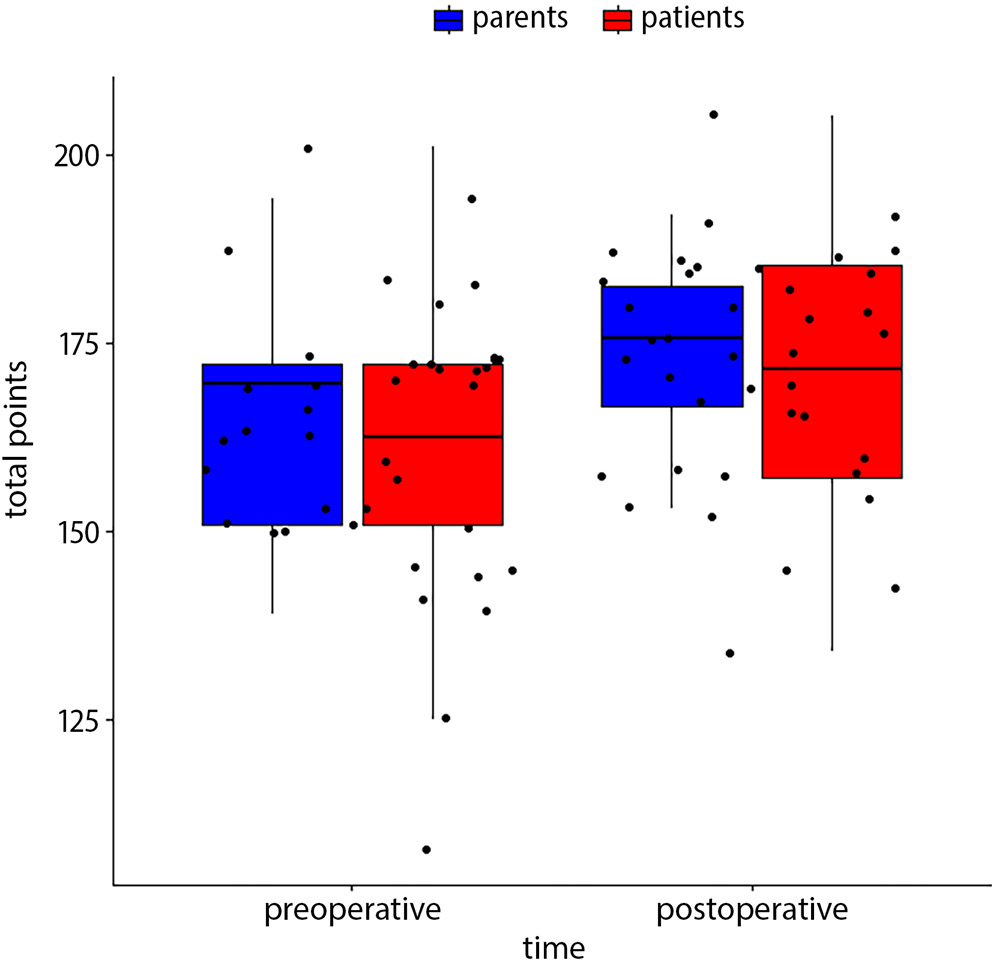
An increase in total points for the postoperative assessment was observed for physical activity, patient wellbeing, contact with peers, and school environment (box-whisker plots in Figure 3, Figure 4, Figure 5, Figure 6, Figure 7.
We found a high correlation between the patients’ and their parents’ responses in each dimension of the KIDSCREEN-52 questionnaire. No statistically significant differences were identified between these groups (Table 5, Table 6).
Discussion
Quality of life was defined by the World Health Organization in 1994 as “an individual’s perception of their position in life in the context of the culture and value systems in which they live and in relation to their goals, expectations, standards, and concerns.”11 Adolescence is a period of life where many physical, social and emotional changes take place. During this time, physical appearance is an important subject because of changes in the body during puberty.12
Frieson and Frieson and de Castro et al. described this transitional period as a strong impact point on an adult patient’s life. One important area is self-esteem, a personal evaluation of oneself that influences one’s behavior. It is well known that people with positive self-esteem are more capable of coping with life.13, 14
The main factor for the importance of body appearance during adolescence was first reported by Elkind in 1967 as “adolescent egocentrism.” It is a result of a typical social cognitive development process. Adolescents are unable to discriminate between other people’s thought and their own mental preoccupations. They are apprehensive about other people’s opinions, especially about body image and actions.15, 16
Pectus excavatum is a deformity with a physiological and psychological impact on patients, decreasing their QoL. Patients with this condition can experience a disturbed body image and lower self-esteem. Chest wall congenital anomaly can cause embarrassment, which in turn may negatively affect social interactions.3, 17 In 2008, Kelly et al. reported that PE has a significant impact on patients’ and their parents’ wellbeing. The main goal of surgical treatment is to improve body image, self-esteem and QoL.18 The Nuss procedure (MIRPE) has become the gold standard surgical treatment of pectus excavatum in the pediatric population.
We compared QoL of our patients prior to the operation and 12 months afterwards. We found remarkable differences in the patients’ perception of specific dimensions of their life. These findings are similar to other reported results. Lawson et al. and Roberts et al. revealed that the Nuss procedure has a positive impact on physical and psychological wellbeing of children and their perception of QoL.19, 20
Chest deformation decreases children’s daily activities in over 70% of cases (reported generally for PE and carinatum). Usually, patients withdraw from social activities like swimming or sunbathing because of fear of being judged by their peers. A higher incidence of depression was reported in the PE patient group.1
Walsh et al. state that the perception of congenital chest wall deformity is individual; for many patients, a mild defect is tolerated, but for some, it is a source of severe psychological distress. It usually occurs during adolescence – the time of social development and interaction with peers.
We found better contact with peers after treatment in the study group. Patients who withdrew from social activities because of PE had reduced health-related QoL.21
In our study group, the patients’ assessment of their general health condition was better postoperatively. This confirms lower health-related QoL in the pediatric population with chest wall deformities.
Many authors have assessed QoL using health-related generic questionnaires. In 2016, Lomholt et al. studied a group of 107 patients evaluated with the Child Health Questionnaire and compared to 183 controls. The patients and their parents revealed improved self-esteem, emotional wellbeing and social activities when comparing preoperative and postoperative periods.22
An interesting fact of our study was that we did not find any important differences in the perioperative “looking after myself” dimension. This probably is an effect of the small sample size and their individual perception of their body image.
Kelly et al. reported a multicenter study on 264 children and 291 parents. They used the Pectus Excavatum Evaluation Questionnaire (PEEQ). The children noted a significant improvement in body image and physical difficulties after surgery. The parents also noted an improvement in their children’s emotions, self-consciousness and physical problems.18
The patients in our study had no problems with mobility before or after operative treatment. This is probably due to good compliance: each of them was obliged to perform a set of exercises in the preoperative and postoperative periods. We assume that preoperative problems with mobility and daily activities were higher in the group of girls because of their lower motivation to engage in physical activities during adolescence.
It was also demonstrated that disease severity and symptoms varied and were patient-specific. Every case should be individualized because there is no correlation between the degree of anterior chest wall depression and the patient’s problems.18 The PEEQ has been used as a disease-specific tool in many studies. The PEEQ is centered on aspects strongly including questions about typical patients’ problems with chest wall deformity. In our study, we evaluated children after MIRPE to detect changes in general areas of patient life, not only treatment-related changes.
Our results are similar to those of Lawson et al., who found that patients’ assessment of QoL after a Nuss procedure correlates to their parents’ assessment.19
Limitations
Our study has several limitations, such as the small study group and the lack of long-term follow-up (e.g., after removal of the titanium bar). The statistical analysis methods used in this research (Mann–Whitney and Wilcoxon tests) are only one-dimensional, so they give a simplified picture of the relationships between variables. More detailed statistical analyses, such as a multifactorial model, could be used in larger groups of patients. Multi-center studies including all children who underwent MIRPE could evaluate multifactorial aspects which have an impact on general QoL (differences between culture, environment, family, preschool problems, etc.). Such a survey would be significantly more valuable.
Conclusions
This study shows that PE correction with the Nuss procedure has a good effect on patients’ wellbeing. Future studies should include multi-center studies using standardized questionnaires designed for children with chest wall deformities.
In conclusion, the Nuss procedure for correcting PE in children has a positive impact on QoL. This fact should be always considered during the qualification process for operative treatment of congenital chest deformities.
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Consent for publication
Not applicable.