Abstract
Background. Dacryolithiasis can occur anywhere in the lacrimal drainage system and is frequently associated with microbial infections. The presence of dacryolithiasis is difficult to determine based on its clinical manifestations, which complicates clinical treatment.
Objectives. To analyze the clinical diagnosis, treatment and characteristics of dacryolithiasis, as well as surgical methods used to treat it and treatment effects over the past 5 years.
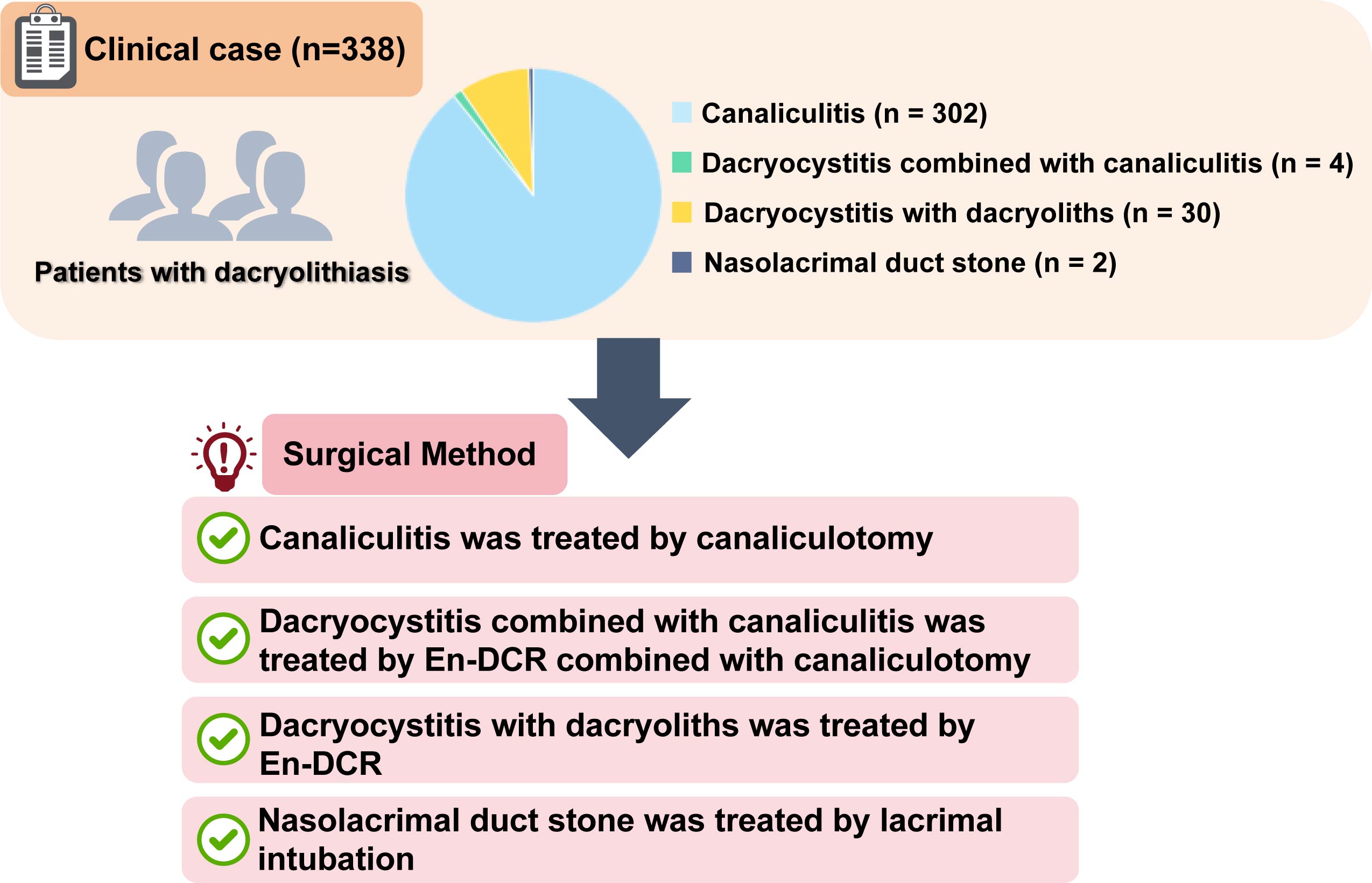
Materials and methods. A retrospective analysis was performed on the clinical data of 338 patients who were diagnosed with dacryolithiasis at our hospital from January 2017 to December 2021. Patients diagnosed with canaliculitis were treated with canaliculotomy. Dacryocystitis complicated by canaliculitis was treated with endoscopic dacryocystorhinostomy (En-DCR) combined with canaliculotomy. Dacryocystitis accompanied by dacryoliths was treated with En-DCR. Nasolacrimal duct stones were treated with lacrimal intubation. All patients were followed up for 6–12 months.
Results. All patients underwent successful surgery. Of 302 cases (89.35%) with canaliculitis, 297 (98.34%) were cured with canaliculotomy; 5 cases (1.66%) recurred within 1 year after surgery and were cured with canaliculotomy again. Four cases (1.18%) of dacryocystitis complicated by canaliculitis were treated with En-DCR combined with canaliculotomy. In addition, 30 patients (8.88%) had dacryolithiasis; 28 (93.33%) of them were cured, and 2 (6.67%) with common canalicular atresia were cured after lacrimal intubation. Furthermore, 2 patients (0.59%) with nasolacrimal duct stones underwent lacrimal intubation. In addition, 62 cases (20.53%) with canaliculitis tested positive for bacteria, and the top 2 common bacteria were Staphylococcus epidermidis and Streptococcus mitis.
Conclusions. Secretions are the main clinical characteristic of patients with dacryolithiasis, and surgery is the primary treatment method. In addition, different surgical methods correspond to different locations of stones.
Key words: dacryolithiasis, canaliculitis, dacryocystitis with dacryoliths, endoscopic dacryocystorhinostomy
Background
Dacryolithiasis is a frequently occurring disorder of the lacrimal system, commonly linked with microbial infection and often underdiagnosed.1, 2 Dacryolithiasis is prone to occur in patients over 50 years old with a history of smoking, dacryocystitis, and facial and nasal trauma. Moreover, there is no significant difference in the incidence of dacryolithiasis between men and women.3 Dacryoliths, first described in 1670, are stones that form in the lacrimal duct system. They can be found throughout the lacrimal drainage system, mainly consisting of lacrimal duct stones and lacrimal sac stones, and also involving a small part of the lacrimal duct system, such as nasolacrimal duct stones.4 The lacrimal duct stones are mainly composed of lobulated and lamellar substances with amorphous nuclei. On the one hand, local necrotic tissue and calcification of mold or hypha can form stones. The formation of stones can be promoted by changes in tear rheology, mechanical stimulation, bacterial migration, and disruption of the balance between single mucin and trefoil factor peptides.5 Although the specific pathogenesis of dacryolithiasis is not yet clear, some proteins and peptides play vital roles in the pathogenesis of lacrimal duct stones.3 Moreover, Lew et al.6 claimed that the concentration of lysozyme in tears of patients with dacryolithiasis was related to the pathogenesis of the condition.
Canaliculitis, one of the more common inflammatory diseases of the lacrimal duct, is mainly induced by lacrimal duct stones.7 The presence of dacryolithiasis is difficult to determine based on its clinical manifestations, which complicates clinical treatment. Dacryolithiasis is mostly identified during dacryocystorhinostomy (DCR). Nasolacrimal duct stones are rare and lack typical manifestations, making them easily misdiagnosed as chronic conjunctivitis, chronic dacryocystitis or chalazion, which results in delays in effective treatment.8 Recent studies revealed the role of tear rheology, mechanical stimulation and bacterial influences in dacryolith formation; however, these findings have not yet been sufficiently integrated into a comprehensive pathogenetic model. Given this context, the present study aims to bridge this gap by conducting a detailed biochemical analysis of lacrimal stones and correlating these findings with the clinical profiles of dacryolithiasis patients. This approach is anticipated to shed light on the specific molecular interactions involved in the pathogenesis of dacryolithiasis, offering a foundation for novel therapeutic strategies.
Objectives
This study was conducted to analyze the clinical diagnosis, treatment and characteristics of dacryolithiasis, as well as surgical methods used to treat it and treatment effects over the past 5 years, thereby providing a reference for the diagnosis and treatment of the disease.
Materials and methods
Study design and participants
This study was a retrospective analysis of cases. In total, 338 patients diagnosed with dacryolithiasis from 2017 to 2021 at Qingdao Eye Hospital of Shandong First Medical University (China) were enrolled. Among them, 71 were male and 267 were female, with an average age of 51.5 ±14.02 years. All patients were admitted to the hospital for a lacrimal duct irrigation examination, and dacryocystography was performed if the lacrimal duct was obstructed. The patients were divided into 4 groups based on the type of surgery. Specifically, 302 cases of dacryolithiasis diagnosed with canaliculitis underwent canaliculotomy; 4 cases of dacryocystitis complicated by canaliculitis were treated with endoscopic DCR (En-DCR) combined with canaliculotomy; 30 cases of dacryocystitis with dacryoliths were treated with En-DCR; and 2 cases of nasolacrimal duct stones were treated with lacrimal intubation. The definitive diagnosis was based on clinical manifestations and dacryocystography. This study was approved by the Ethics Committee of Qingdao Eye Hospital of Shandong First Medical University (approval No. 2022–48).
Types and surgical methods of dacryolithiasis
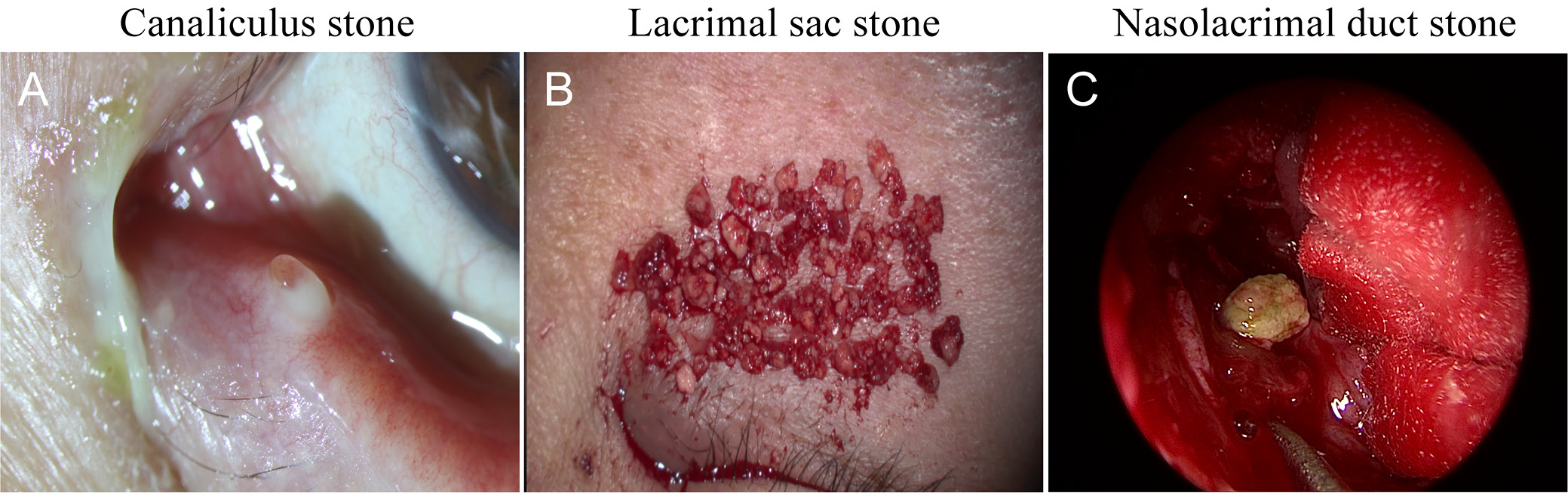
The clinical manifestations of canaliculitis (Figure 1A) were as follows: 1) hyperemia and redness at the lacrimal punctum; 2) swelling of the lacrimal canaliculus area; 3) purulent and granular secretion upon pressure; and 4) unobstructed lacrimal duct flushing with secretion overflow. The surgical method was canaliculotomy. Specifically, the lacrimal punctum was dilated first, followed by a vertical incision on the lacrimal canaliculus. Next, lacrimal canaliculus stones were removed via curettage. Afterward, the lacrimal passage was flushed until the fluid coming out was transparent. A silicone drainage tube was inserted if the duct was not clear.
The main symptoms of dacryocystitis combined with canaliculitis were similar to those of canaliculitis alone, primarily involving tear overflow and secretion. In addition, dacryocystitis + canaliculitis was characterized by obstructed lacrimal duct flushing and secretion overflow, along with swelling and redness around the tear ducts, with granular secretions released upon pressure. The surgical method used was En-DCR combined with canaliculotomy.
The symptoms of dacryocystitis complicated by dacryoliths (Figure 1B) were primarily lacrimation and secretion, with lacrimal sac stones observed during En-DCR. The surgical method involved removing calculi and granulation tissue from the lacrimal sac cavity via En-DCR.
Nasolacrimal duct stones (Figure 1C), while similar to dacryocystitis, were characterized by low obstruction in the nasolacrimal duct and a short disease course (less than 4 months). The surgical method was removal of the nasolacrimal duct stone through lacrimal duct probing with nasal endoscopy.
Postoperative medication and follow-up
The surgical eye was treated with antibiotic eye drops, 0.1% fluorometholone eye drops and antibiotic eye ointment. Patients undergoing En-DCR were given fluticasone propionate nasal spray twice a day and followed up at 1, 3, 6, and 12 months after surgery. Upon En-DCR, the patients underwent dressing changes and reexamination under a nasal endoscope. The secretion around the anastomosis was cleaned, and the lacrimal passage was washed. Subsequently, the epithelialization of the lacrimal sac, nasal cavity and anastomosis, as well as the recovery of lacrimal passage function, were observed.
Criteria for determining efficacy
Canaliculitis
The symptoms of lacrimation and secretion disappeared. The lacrimal punctum and lacrimal canaliculus had no redness and swelling. The lacrimal canaliculus had no secretion overflow after pressing the diseased lacrimal canaliculus, and the lacrimal passage was flushed unobstructedly and had no secretion.
Dacryocystitis combined with canaliculitis
The symptoms of lacrimation and secretion disappeared. The lacrimal punctum and lacrimal canaliculus did not exhibit redness and swelling. Upon pressing the diseased lacrimal canaliculus, there was no secretion overflow in the lacrimal canaliculus. In addition, the lacrimal passage was flushed unobstructedly and had no secretion. Nasal endoscopy showed that the mucosa of the anastomosis was epithelialized, the anastomosis was open and the lacrimal passage was flushed unobstructedly.
Dacryocystitis with dacryoliths
There were no symptoms of lacrimation and secretion. Nasal endoscopy displayed epithelialized anastomotic mucosa, with the anastomosis open and the lacrimal passage flushed unobstructedly.
Nasolacrimal duct stone
The symptoms of lacrimation and secretion disappeared. After pulling out the lacrimal drainage tube, the lacrimal duct was flushed unobstructedly and the secretion was absent.
Culture and identification of pathogenic bacteria
The secretions from the lacrimal punctum were extracted and sealed in sterile test tubes, and then bacterial culture and drug sensitivity tests were performed. In short, the collected specimens from the conjunctival sac and lacrimal duct were coated and scribed on a blood agar plate and cultured in a 35°C incubator for 24, 48 and 72 h to observe bacterial growth. If colony growth was observed, the bacteria were isolated and purified, followed by a drug sensitivity test.
Data presentation
For groups with less than 10 participants, the assumption of normal distribution was not checked; instead, data were reported using the median along with the minimum and maximum values. For larger groups exceeding 100 participants, the normality of distribution was not assessed; the central limit theorem was applied, and results were described using the mean and standard deviation (SD). For groups with sizes ranging from 10 to 100, the Shapiro–Wilk test was utilized to evaluate normality. If a statistically significant deviation from normal distribution was found, the median and interquartile range (IQR) were reported. If there was no significant deviation, the mean and SD were used to present the data. Categorical data were consistently summarized as frequencies and percentages (n (%)).
Results
Clinical data characteristics
In this study, the clinical data of 338 patients with dacryolithiasis were analyzed, and the results are shown in Table 1. The 338 patients consisted of 71 (21%) men and 267 (79%) women, with a men-to-women ratio of 1:3.8. Their age ranged from 17 to 90 years (mean 61.40 ±14.02 years), and the disease duration ranged from 20 days to 20 years (mean 1.62 ±3.03 years). In addition, there were 76 cases (22.5%) of smokers and 302 cases (89.35%) of canaliculitis. Furthermore, 297 cases were cured, giving a cure rate of 98.34%; 5 cases (1.66%) recurred within 1 year after the operation and were cured by canaliculotomy again. Dacryocystitis combined with canaliculitis was found in 4 cases (1.18%) during the operation and was treated with En-DCR combined with canaliculotomy. Of the 30 patients (8.88%) with dacryolithiasis, 28 cases (93.33%) were cured, and 2 cases (6.67%) exhibited closed lacrimal ducts and were cured after re-catheterization. Two patients (0.59%) with nasolacrimal duct stones underwent lacrimal intubation; 1 case of nasolacrimal duct opening was examined by nasal endoscopy during the operation, and nasolacrimal duct stones were discharged. One case of stone-like secretion was removed from the nasal cavity after the operation, and all cases were cured. No recurrence was found within 1 year after the operation.
The location of canaliculitis
Subsequently, the location of canaliculitis was analyzed. The results showed that the first 4 locations of canaliculitis were the left inferior lacrimal canaliculus, the right inferior lacrimal canaliculus, the left superior lacrimal canaliculus, and the right superior lacrimal canaliculus, accounting for 34.44%, 26.49%, 14.9%, and 14.24%, respectively. Canaliculitis usually appeared in the inferior canaliculus, and there was no difference between the left and right eyes (Table 2).
Etiology analysis
The samples from canaliculitis patients were sent for pathogen culture, and the distribution of pathogenic bacteria species in positive samples is shown in Table 3. Among the 302 cases with canaliculitis, 62 were positive for bacteria, with a culture positivity rate of 20.53%. In addition, a total of 17 bacterial strains were identified in these cultures, and the pathogenic bacteria were mostly Gram-positive cocci. Staphylococcus epidermidis was the most common pathogen, accounting for more than 51.61%.
The samples from dacryocystitis + dacryoliths patients were also subject to pathogen culture, and the distribution of pathogenic bacteria species in positive samples is presented in Table 4. Among the 30 cases with dacryocystitis + dacryoliths, 15 were positive for bacteria, with a culture positivity rate of 50%. Furthermore, a total of 6 bacterial strains were identified in these cultures, and the pathogenic bacteria were mostly Gram-positive cocci. Staphylococcus aureus and S. epidermidis were the most common pathogens, accounting for more than 66.67%.
Discussion
Canaliculitis is one of the most common complications in dacryolithiasis. Due to similar clinical manifestations to a variety of ophthalmic diseases, lacrimal canaliculitis is an ophthalmic disease with a high misdiagnosis rate in outpatient settings.9 Xiang et al.10 reported that the misdiagnosis rate of canaliculitis was 77.8%. Non-lacrimal specialists often misdiagnose lacrimal canaliculitis as common infectious diseases in ophthalmology, such as conjunctivitis, meibomian gland inflammation or dacryocystitis, and long-term repeated medication often yields unsatisfactory results.11 Some patients lose confidence and give up seeking medical treatment, which causes significant distress. When the patient exhibits conjunctival congestion and repeated drug treatments are ineffective, it should be differentiated from conjunctivitis. When the patient’s eyelid is red and swollen, this should be differentiated from meibomian gland inflammation. In addition, many patients with exudate spillage from the lacrimal punctum are misdiagnosed as having dacryocystitis and may even undergo DCR, but the symptoms are not relieved after the operation. Patients with dacryocystitis typically exhibit normal lacrimal canaliculus and lacrimal punctum, with the main manifestation being purulent secretion overflow from the lacrimal punctum when pressing the lacrimal sac area. In contrast, purulent or granular secretion overflow can be seen in lacrimal canaliculitis when pressing the lesion lacrimal punctum area. Most of the lacrimal duct is flushed smoothly and can be identified based on different characteristics. Although some patients have an insidious onset, as long as the disease is recognized, patients with long-term recurrent secretion from the lacrimal canaliculus should be carefully examined, and the lacrimal duct should be rinsed in parallel. Based on symptoms and signs, the diagnosis is not difficult.
The incidence of female patients is significantly higher than that of male ones,7 which our study also confirmed. The reason may be due to the decrease in estrogen levels in women during amenorrhea, leading to reduced tear secretion and decreased resistance to infection, making the lacrimal canaliculus more susceptible to microbial invasion. In addition, women’s daily lifestyle, such as the use of cosmetics and exposure to oil fumes, may contribute to the blockage of lacrimal canaliculi by microparticles, facilitating the growth of microorganisms within the lacrimal passage.
Regarding the location of canaliculitis lesions, canaliculitis usually affects the inferior canaliculus, predominantly occurring in 1 eye, with no significant difference between the left and right eyes. Due to gravity, tear drainage is mainly achieved by the inferior lacrimal canaliculus, and bacteria on the ocular surface tend to accumulate mainly in the lower part. The diameter of the inferior lacrimal canaliculus is larger than that of the superior lacrimal canaliculus. Pathogenic microorganisms from the lacrimal sac or nasolacrimal duct are more likely to spread to the inferior lacrimal canaliculus, making inferior lacrimal canaliculitis more common.12
Previous studies believed that actinomycetes were the main pathogenic bacteria of lacrimal canaliculitis. However, recent studies have identified that the pathogenic bacteria of lacrimal canaliculitis have changed.13 For instance, Alam et al.14 reported S. epidermidis as the most common pathogen of canaliculitis. Zhang et al.15 stated that the main pathogenic bacteria of lacrimal canaliculitis were Gram-positive bacteria, with common bacterial genera including Staphylococcus, Propionibacterium, Streptococcus, etc. In this study, the top 2 most frequently identified bacteria were S. epidermidis and Streptococcus mitis, consistent with the distribution of the most common bacterial flora in the normal conjunctival sac reported by Wang et al.16 A study17 on the distribution and drug resistance of ocular bacterial culture-positive strains also pointed out that S. epidermidis was the primary pathogenic bacteria and the most important multi-drug resistant bacteria in the eye. The removal of stones is the major treatment of lacrimal canaliculitis. If lacrimal duct stones continue to block the lumen, only squeezing and scraping the stones can relieve the symptoms.
The prevalence of dacryolithiasis gradually increases after the age of 50 years.18 Most of the pathogenic bacteria associated with dacryolithiasis are Gram-positive bacteria. However, dacryolithiasis is usually difficult to diagnose before operation. Given the inadequacies of imaging methods such as X-ray, dacryocystography and computed tomography (CT), dacryolithiasis often remains misdiagnosed or undetected. The overall incidence of dacryolithiasis is, therefore, difficult to assess. Dacryolithiasis is usually found when the lacrimal sac is opened during DCR, so intraoperative incision of the lacrimal sac is the only effective way to confirm the presence of dacryolithiasis. The DCR is often regarded as the gold standard for the treatment of dacryolithiasis.4 For repeated secretion, the presence of dacryolithiasis should be highly suspected if drug control is ineffective. Pressing the lacrimal sac can show purulent secretion overflow, and lacrimal duct irrigation can vary in terms of its smoothness. Studies have revealed that lacrimal duct stones were diagnosed in 6–18% of patients during DCR,2 and the proportion in this study was 6.68%, which is similar to literature reports.
Dacryocystitis complicated by canaliculitis is relatively easy to diagnose. Special attention should be paid to cases of canaliculitis combined with dacryolithiasis. In such patients, the lacrimal passage may sometimes be unobstructed, and secretion may spill, which is consistent with the symptoms of simple lacrimal canaliculus inflammation. If treatment of lacrimal canaliculitis alone does not resolve symptoms of secretion post-surgery and there is neither inflammation nor stone-like discharge upon compression of the lacrimal canaliculus, it is highly likely that the patient may have concurrent lacrimal sac stones. In such instances, DCR is required to incise the lacrimal sac for a definitive diagnosis. Two patients in our research were diagnosed with canaliculitis before the operation, but their symptoms were not relieved after the operation. Upon ineffective drug treatment, nasal En-DCR was performed. During the operation, large stones in the lacrimal sac cavity were found, granulation hyperplasia was present in the lacrimal sac cavity, and the inflammatory reaction was severe. If necessary, the treatments of such patients need to be combined with lacrimal intubation to prevent anastomotic adhesion and atresia.
Very few cases of dacryocystitis are not suitable for DCR as the first choice. Simple lacrimal duct probing combined with lacrimal intubation can dislodge intact lacrimal sac stones and sometimes nasolacrimal duct stones. This procedure is noninvasive, does not alter the natural anatomy and has a short operation time, making it a procedure that most patients are willing to undergo. This requires us to properly determine the surgical indications. For patients with a short duration of secretion symptoms and low-position of lacrimal duct obstruction as suggested by dacryocystography, which is generally located in the lower part of the nasolacrimal duct, we can attempt lacrimal duct probing combined with lacrimal duct intubation after communication with the patients and their families and obtaining their consent. Notably, if probing fails, En-DCR is performed.
Limitations
This study’s retrospective design inherently introduced selection and information biases, potentially leading to skewed data due to non-random patient selection and variable data accuracy. In addition, the relatively small sample size of 338 patients limited the statistical power and generalizability of the findings to the broader population with dacryolithiasis. The absence of a control group further restricted our ability to distinguish between effects directly attributable to dacryolithiasis and those resulting from extraneous variables. To overcome these limitations and enhance the validity of future research, it is advisable to employ a prospective study design and conduct randomized controlled trials (RCTs), which would allow for systematic comparisons and more controlled conditions. Increasing the sample size and including multiple research centers would also help achieve a more representative population sample, thereby improving the generalizability of the results. Finally, applying advanced statistical techniques, such as multivariate analysis, can help control for potential confounders, ensuring a more accurate isolation of the effects being studied.
Conclusions
This study offers a comprehensive clinical analysis of dacryolithiasis, highlighting the essential role of diagnostic tools such as slit-lamp examination, lacrimal irrigation and dacryocystography. These tools are crucial not only for accurately diagnosing dacryolithiasis but also for determining the precise location of lacrimal stones, which guides the selection of appropriate surgical interventions. Clinicians are encouraged to integrate these diagnostic procedures into routine assessments to enhance detection and management, thereby ensuring that surgeries are minimally invasive, reduce complications and improve success rates. Future research should focus on evaluating the long-term outcomes of surgical techniques, developing innovative diagnostic tools for more precise assessments, and exploring the pathophysiological underpinnings of dacryolithiasis to identify new therapeutic targets.
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Consent for publication
Not applicable.
Use of AI and AI-assisted technologies
Not applicable.