Abstract
Background. Pulpal vitality is important for the tooth to maintain its physiological function and preserve its structure.
Objectives. The aim of this study was to evaluate the clinical and radiographic 6- and 12-month treatment success of calcium hydroxide (CH) and calcium silicate materials in indirect pulp treatment (IPT) and direct pulp capping (DPC) in teeth with deep dentin decay.
Materials and methods. The study included 143 teeth of patients aged 17–69 years with no systemic disease. The study is grouped under 3 main groups (Dycal, Biodentine, TheraCal PT). Direct pulp capping was applied to 65 teeth and IPT to 66 teeth. All teeth were restored with Universal adhesive system and Universal composite (G-Premio Bond; GC Corp., Tokyo, Japan).
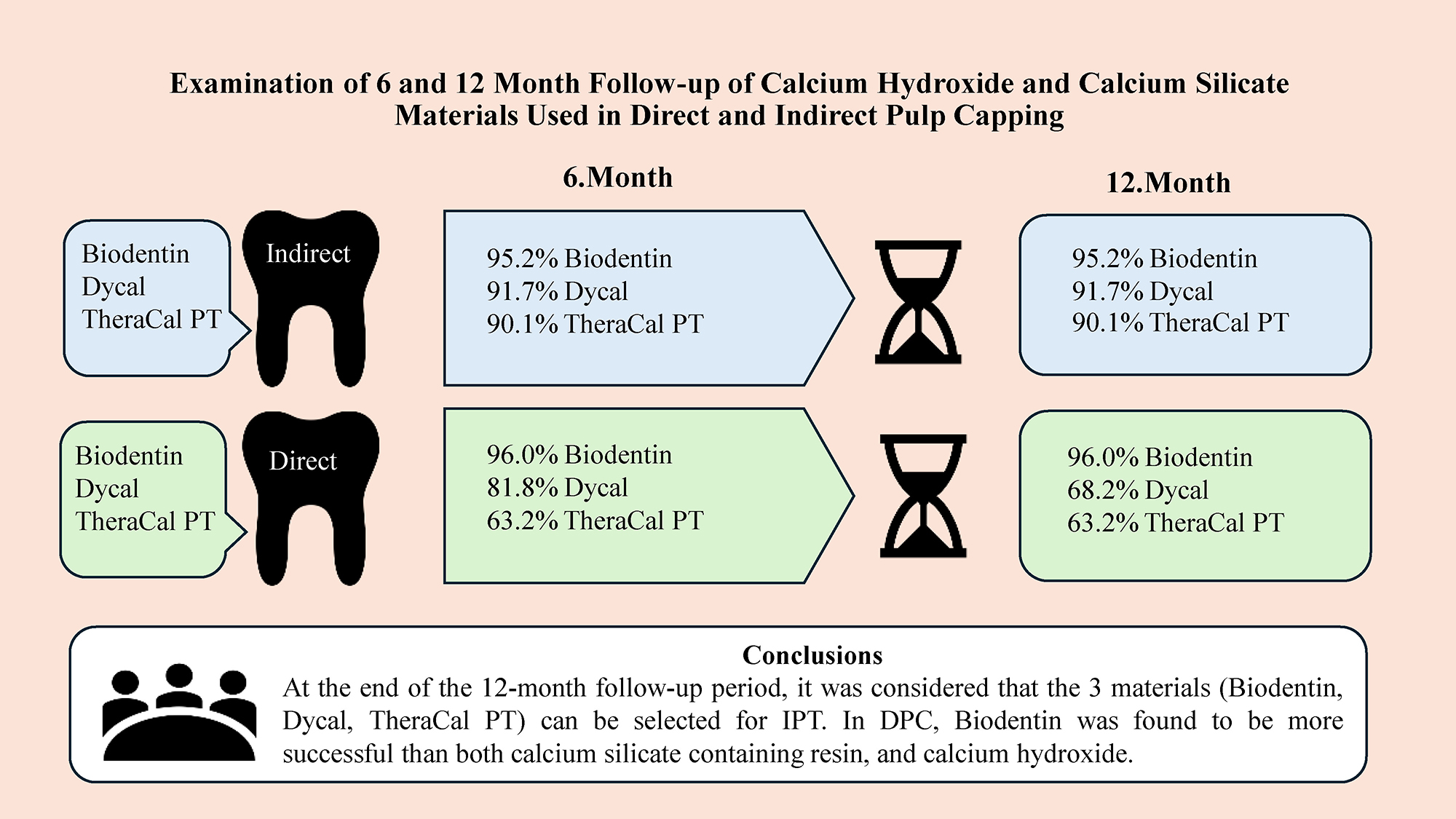
Results. In the statistical evaluations of the data obtained, 0.05 was accepted as the level of statistical significance. The general success rate in the IPT group was found to be 95.2% for Biodentine (Septodont, SaintMaur-des-Fossés, France), 91.7% for Dycal (Dentsply/Caulk, International Inc. Milford, USA) and 90.1% for TheraCal PT (Bisco Inc., Schaumburg, USA) at both 6 and 12 months. When the clinical and radiographic success was compared at 6 months and 12 months, no statistically significant difference was determined between the materials (p > 0.05). In the clinical and radiographic evaluations at the end of 6-month follow-up in the DPC group, the success rates were determined to be 96.0% for Biodentine, 81.8% for Dycal and 63.2% for TheraCal PT. At 12 months, these rates were 96.0% for Biodentine, 68.2% for Dycal and 63.2% for TheraCal PT. DPC Biodentine was found to be the most successful material (96.0%).
Conclusions. At the end of the 12-month follow-up period, it was considered that the 3 materials (Biodentine, Dycal, TheraCal) can be selected for IPT. In DPC, Biodentine was found to be more successful than both calcium silicate containing resin and CH.
Key words: Biodentine, direct pulp capping, TheraCal PT, deep dentin decay, indirect pulp treatment
Introduction
In teeth with deep dentin decay which have formed cavitation, the aim is to maintain the vitality and function of the tooth in the mouth with appropriate decay management.1, 2, 3, 4 Irrespective of the method used to remove the decay, vital pulp treatment (VPT) is applied according to the status of the exposed pulp.1, 5, 6 Vital pulp treatment includes a series of conservative procedures based on the internal repair mechanisms of the pulp–dentin complex.7, 8, 9, 10, 11, 12 These have attracted more interest with the utility of new bioactive materials.1
Pulp capping biomaterials are placed as a protective layer on the pulp exposed following trauma to the teeth or after removal of decay lesions.13 These materials are found in live tissues and facilitate the survival and proliferation of stem cells which have the potential for repair.14 Calcium hydroxide (CH) is the oldest and most commonly used amputation agent in clinical dental practice and is considered the gold standard. It is a low-cost, easily applied material which supports reparative dentin formation, and can be applied rapidly to the exposed pulp area.15, 16, 17, 18
Calcium hydroxide is a basic salt (Ca(OH)2) with low solubility in water with a high alkalic pH, which breaks down into calcium (Ca+2) and hydroxyl (OH–) ions within the solution. When applied to pulp tissue, it produces a caustic effect, and coagulation converts the reserve mesenchymal cells below the necrosis first to fibroblasts and then to odontoblasts, which will form a matrix. It is also known to induce the expression of bioactive molecules such as growth factor- β1 (TBF-β1) and bone morphogenic protein-7 (BMP-7), which stimulate pulp repair.19, 20 Despite these positive properties, CH is resorbed over time because of weak mechanical properties which do not show adhesion to dentin, and cannot provide long-term biological impermeability against bacterial infection.21
In recent years, calcium silicate cements, which are derivatives of Portland cement, have been developed as an alternative to CH. Calcium-silicate cements are hydrophylic materials able to tolerate moisture (hydraulic materials) and to polymerize and harden (setting) also in the presence of biological fluids (blood, plasma, saliva, dentinal fluid).22 The hardening reaction alkalizes the environment by expressing calcium and hydroxyl ions to the tissues with which it is in contact, and creates the necessary alkaline environment for the formation of hydroxyapatite.22, 23 The hardeninng reaction of calcium silicate-based materials is hydration. When dicalcium silicate (C2S) and tricalcium silicate (C3S) enter into a reaction with water, OH–, Ca+2 and Si+4 (silicate) ions emerge as the side product. The OH– ion forms a thin necrotic layer by increasing the pH in the underlying vital tissue. The vital cells below this layer are protected from the alkaline pH of the material. By stimulating cells in the pulp, the Ca+2 ion contributes to mineralization. When the Si+4 ion remains free, it contributes to hard tissue formation by stimulating osteoblasts.24, 25, 26, 27, 28
Biodentine is a calcium silicate material that was first introduced to the market in 2010. The material comes in the form of a capsule with powder and a separate liquid. The powder is formed of tricalcium silicate (Ca3SiO5), dicalcium silicate (Ca2SiO4), calcium carbonate (CaCO3), calcium oxide (CaO), iron oxide (Fe2O3), and zirconium oxide (ZrO2). The liquid contains calcium chloride (CaCl2), water and modified polycarboxylate. Biodentine hardens with the hydration reaction starting with the mixing of the liquid and powder and the hardening process takes 9–12 min. As in other calcium silicate materials, there is a calcium-silicate-hydrate (C-S-H) gel phase and CH is formed while hardening. Upon contact with phosphate-containing solutions, the CH formation and hardening reaction give rise to the generation of antigen-presenting cell (APC) precursors. This represents the initial phase in the development of hydroxyapatite.29, 30 Biodentine has many clinical uses such as dentin liner below composite, direct pulp capping (DPC), pulpotomy treatment, apexification, root filling material, and perforation repair.31, 32 It has provided significant clinical advantages over other pulp capping materials, such as being very successful in dentin bridge formation, dentin substitution, good sealing properties, and sufficient pressure resistance. It shares its indications with CH, but its main disadvantages include setting time and material cost.33, 34
Light-curable resin-based calcium silicate cements have several advantages, including instant setting through light transmission and ease of use. However, these cements contain resin monomers, and incomplete polymerization during light curing is associated with the risk of pulp cell toxicity.35
TheraCal PT (Bisco Inc., Schaumburg, USA) is a calcium silicate-based material modified with dual-cured resin, designed for the use of VPT. According to the manufacturer’s instructions for the material, which is in the form of a double pat ready for use, it is applied in 1-mm layers polymerized with light for 20 s. Although calcium silicate cements with resin content show high physicaal properties, low solubility and ease of clinical use, such material can be separated from dentin tissue due to polymerization shrinkage during the hardening with light. The bonding strength between calcium silicate cements and adhesive systems directly affects the success of VPT.23, 36
Although CH is not accepted as the best possible material option today, CH is still widely used in direct and indirect pulp treatment (IPT) in many healthcare institutions due to the high cost of calcium silicate materials. Despite the superior properties of calcium silicate materials, can CH still be used in VPT?
Objectives
The null hypothesis of this study was that calcium silicate materials would show similar success rates when compared among themselves, and would present better clinical and radiographic results than CH material.
Materials and methods
To fulfil the research objectives, the authors planned a randomized, double-blind clinical trial, which was conducted in the Restorative Dental Treatment Department of the Dentistry Faculty of Harran University, Şanlıurfa, Turkey. The study was conducted in accordance with the Declaration of Helsinki, and the protocol was approved by the Ethics Committee of Harran University (decision No. HRU/21.15.31 dated September 6, 2021) . The risks and benefits related to the procedure were fully explained to all the patients included in the study, and written informed consent was provided by all the partcipants.
A total of 186 participants in the 17–69 age group were included in this study. Twenty-seven participants refused to take part in the study. Sixteen participants were excluded from the study according to exclusion criteria. As a result of clinical and radiographic examinations, the teeth included in the study were those with deep dentin decay where there was thought to be a possibility of pulp perforation resulting from the complete removal of the caries. Vital teeth were selected which had no history of spontaneous or long-lasting pain against thermal or chemical stimuli, no percussion sensitivity, pathological mobility, edema, fistula, or color change. In the radiological examination, premolar and molar teeth, in which the presence of deep decay approaching the pulp ICDAS 5, 6 (International Caries Detection and Assessment System) was observed, were selected when the lamina dura and periodontal gap were healthy, there was no loss of bone surrounding the root, no internal or external root resorption, and no calcified masses observed within the pulp.
Three main groups were formed as follows: CH Group (Dycal, Dentsply/Caulk, International Inc. Milford, USA): In the Dycal group (n : 48), IPT was applied to 25 teeth and DPC to 23 teeth. Following clinical and radiographic examinations, pulp vitality tests were applied (Pulp Tester; Foshan Adelson Medical Devices Co., Ltd., Foshan, China). After a local anaesthesia injection, rubber-dam isolation was performed. In the IPT procedure, the decayed enamel tissue was removed with a cooled high-speed handpiece and a sterile diamond round burr (Diamant GmbH, Schürenbreder Weg 27, Germany). Infected dentin was removed with low-speed, tungsten carbide round burrs (Meisinger Hager & Meisinger GmbH, Neuss, Germany). In accordance with the manufacturer’s instructions for IPT, a thin layer of Ca(OH)2 (Dycal; Dentsply/Caulk) was applied to areas close (0.5 mm) to the pulp.
In the DPC procedure, a sterile cotton wad was applied with moderate pressure for 5 min to the bleeding pulp that was exposed after removal of the decay, and hemostasis was obtained. A thin layer of Ca(OH)2 was applied to the exposed pulp area and areas close (0.5 mm) to the pulp in accordance with the manufacturer’s instructions. Thus, DPC was performed.
Calcium silicate Group (Biodentine; Septodont, Saint-Maur-des-Fossés, France): In the Biodentine group (n = 48), IPT was applied to 22 teeth and DPC to 26 teeth. In the IPT procedure, the pulp capping material with tricalcium silicate content formed of powder and liquid components was mixed and then applied to areas close to the pulp (0.5 mm) in accordance with the manufacturer’s instructions. In the DPT procedure, a sterile cotton wad was applied with moderate pressure for 5 min to the bleeding pulp that was exposed after removal of the decay, and hemostasis was obtained. A thin layer of Biodentine was applied to the exposed pulp area and areas close (0.5 mm) to the pulp in accordance with the manufacturer’s instructions. A period of 12 min was waited for hardening of the material.
In the TheraCal PT group (n = 47), IPT was applied to 24 teeth and DPC to 23 teeth. In the IPT procedure, a thin layer of dual-cured resin-modified tricalcium silicate was applied at max. 1-mm thickness to areas close (0.5 mm) to the pulp in accordance with the manufacturer’s instructions, and was then polymerized with light for 20 s (Valo LED, Ultradent Products Inc., South Jordan, USA). In the DPC procedure, a sterile cotton wad was applied with moderate pressure for 5 min to the bleeding pulp that was exposed after removal of the decay, and hemostasis was obtained. A thin layer of TheraCal PT was applied at a maximum thickness of 1 mm to the exposed pulp area and areas close (0.5 mm) to the pulp in accordance with the manufacturer’s instructions; then, polymerization was applied with light for 20 s.
During the decay removal method, every effort was made not to expose the pulp tissue. After the pulp capping, the universal adhesive system G-Premio Bond (GC Corp., Tokyo, Japan), Filtek-Ultimate Flowable composite (3M ESPE, St Paul, USA) and 3M Filtek Universal composite (3M ESPE, St.Paul, USA) were placed over the pulp capping material in each of the 3 groups.
Before starting the study, power analysis was performed using G*Power v. 3.1 software. The sample size required was found to be 143 study participants at 0.05 error rate and in 0.80 confidence interval.
A total of 143 teeth with deep dentinal caries were numbered at random using Microsoft Excel 2013 (Microsoft Corp., Redmond, USA). It was planned to apply Dycal to the 1st tooth No. 1–48, Biodentine to tooth No. 49–96 and Therecal PT to tooth No. 97–143. Before the appointment, the randomization list was checked by the oral and dental technician, and the treating clinician was informed which application method should be used. Each group consisted of teeth randomly assigned by a blinded investigator according to the materials selected. All the clinical procedures in this study were performed by a single dentist (Y.Y.) The patients were instructed to call and inform the resarchers if they were in any pain or discomfort. All the patients were informed that if there were abnormal signs and symptoms, there could be a need for root canal treatment.
All clinical and radiographic follow-up evaluations were performed by the expert investigator (S.K.) who was blinded to the drugs used (not the operator). Patients were re-examined clinically and radiographically to evaluate pulp vitality 6 and 12 months after treatment. Among the clinical parameters used for evaluation, the presence of post-treatment pain, provoked pain, spontaneous pain, or night pain were used. In the clinical examination, the following aspects were investigated: percussion, palpation, mobility, edema, and the presence of a fistula. In radiographic evaluation, lamina dura continuity, periapical lesion, furcation lesion, and pathological root resorption were assessed. The presence of one or more of the clinical/radiographic findings was considered treatment failure.
Statistical analyses
The data obtained in the study were statistically analysed using IBM SPSS Statistics v. 23.0 (IBM Corp., Armonk, USA). Descriptive statistics were presented as mean ±standard deviation (mean ±SD) values for continuous variables and number (n) and percentage (%) for categorical variables. The suitability of the data for normal distribution was evaluated using the Shapiro–Wilk test. The χ2 ttest was used to analyze the relationships between categorical variables. Bonferroni method was used in the pairwise comparisons of success rates at 6th and 12th month according to the groups. In this paper, we focused on the results for each group separately. Therefore, the McNemar test was used, for each group separately, for measurements made at 2 different times. Kruskal–Wallis test was used because the mean age data were not normally distributed. The χ2 test was used to compare the distribution of genders between the groups. Comparisons in different groups are shown with letters in the tables. A p-value of less than 0.05 was deemed to be statistically significant.
Results
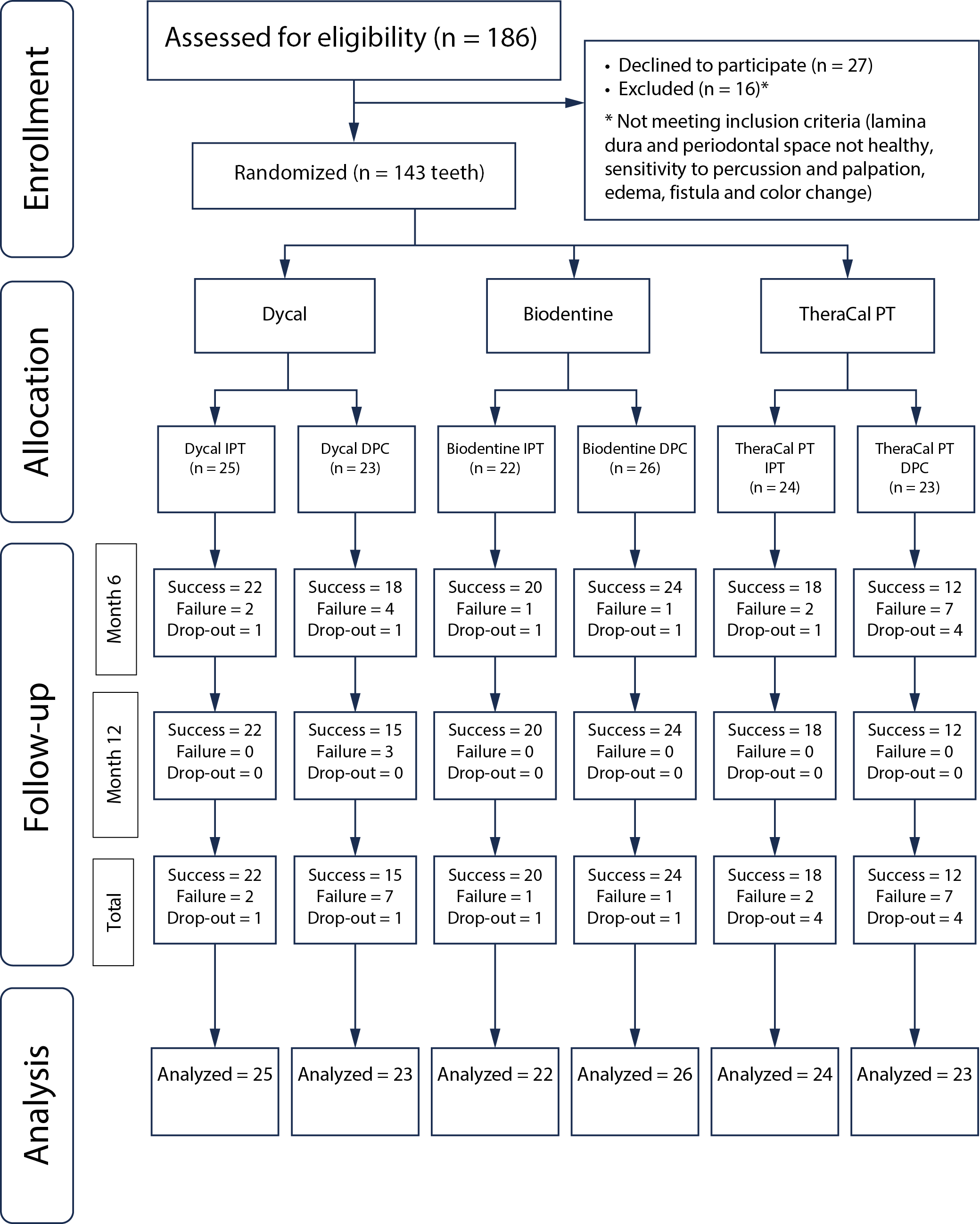
Figure 1 presents the flow diagram for patient recruitment and selection. The sample size of this study was 143. It was planned to apply Dycal to the first 48 teeth, Biodentine to the next 48 teeth and Therecal PT to the last 47 teeth. Twelve patients did not come to their appointments. Direct pulp capping was applied to 65 teeth and IPT to 66 teeth. Evaluation was made of 131 teeth of 50 men with a mean age of 34.26 ±12.86 years and 81 women with a mean age of 30.23 ±9.97 years (age range: 17–69 years). As a result of the statistical evaluations, age and gender distribution between the groups was not seen to be normal (Table 1) (p > 0.05). It was observed that there was no statistically significant difference between the mean ages of the individuals participating in the study in different groups groups (p = 0.139).
Evaluation of the success rates of indirect pulp treatment
At the end of month 6, there were 2 failures and 1 patient who did not attend the follow-up appointment in the Dycal IPT group, 1 failure and 1 patient who did not attend the follow-up appointment in the Biodentine IPT group, and 2 failures and 4 patients who did not attend the follow-up appointment in the TheraCal PT IPT group.
At the end of month 12, no clinical or radiographic failure was observed in any of the 3 groups (Dycal, Biodentine, TheraCal PT) applied with IPT. The success rates of IPT in the clinical and radiographic evaluations at 6 months and 12 months were determined to be 91.7% in the Dycal group, 95.2% in the Biodentine group and 90.0% in the TheraCal PT group. There was no difference between groups with the same letter (Table 2).
In the Biodentine IPT group, it was found that there was no statistically significant difference between the filling procedures performed at 2 different times (p = 1.000). In the Dycal IPT group, there was no statistically significant difference between the filling procedures performed at 2 different times (p = 1.000). In the TheraCal PT IPT group, there was no statistically significant difference between the filling procedures performed at 2 different times (p = 1.000) (Table 3).
Evaluation of the success rates of direct pulp capping
At the end of month 6, there were 4 failures and 1 patient who did not attend the follow-up appointment in the Dycal DPC group, 1 failure and 1 patient who did not attend the follow-up appointment in the Biodentine DPC group, and 7 failures and 4 patients who did not attend the follow-up appointment in the TheraCal PT DPC group. In the clinical and radiographic evaluations at 6 months, the success rates of DPC were determined to be 81.8% in the Dycal group, 96.0% in the Biodentine group and 63.2% in the TheraCal PT group.
At the end of the 12-month follow-up period, there were 3 clinical and radiographic failures in the Dycal DPC group and none in the Biodentine DPC and TheraCal PT groups. In the clinical and radiographic evaluations at 12 months, the success rates of DPC were determined to be 96.0% in the Biodentine group, 68.2% in the Dycal group and 63.2% in the TheraCal PT DPC group (p = 0.020; p = 0.017) (Table 4). In the Biodentine DPC group, it was found that there was no statistically significant difference between the filling procedures performed at 2 different times (p = 1.000). In the Dycal DPC, there was no statistically significant difference between the filling procedures performed at 2 different times (p = 0.250). In the TheraCal PT DPC, there was no statistically significant difference between the filling procedures performed at 2 different times (p = 1.000) (Table 3).
Discussion
The aim of VPT in teeth with decay lesions is to protect the vitality and integrity of dental tissues.37
This randomized clinical trial was conducted to evaluate the clinical and radiographic behavior of Dycal, Biodentine and TheraCal PT in VPT (direct and indirect) during a 1-year follow-up. The focus was on the use of dental materials to preserve the vitality of the pulp in teeth with deep dentin caries. The main findings of this study were that failures in IPT were low in all 3 groups (Dycal, Biodentine and TheraCal PT). It was found that there was no statistically significant difference between the filling processes of 3 materials at 2 different times in IPT. It was also observed that most of the failures occurred in the 1st follow-up period and the rate did not change in the 12th month. In DPC, clinical and radiographic failures were observed to be less frequent in the group treated with Biodentine compared to the groups treated with Dycal and TheraCal PT. Although failure rate in the Dycal group increased over time in the DPC, it was not found to be statistically significant at 2 different times.
Cho et al. reported that the material used in DPC was one of the most important factors affecting prognosis.38 Calcium hydroxide, which has been used for many years as a vital pulp capping material, is still accepted as it is low-cost and easy to apply.15, 16, 17, 18 However, pulp capping materials containing tricalcium silicate have been recently reported to be more successful than CH.7, 17, 39
In their research on the effectiveness of Kusuma, Biodentine, Ca(OH)2 and mineral trioxide aggregate (MTA) on the cellular response of pulp tissue; Biodentine showed activity with fewer neutrophils and macrophages and higher numbers of odontoblast-like cells and fibroblasts.40
In studies of pulpotomy, in which Biodentine and MTA were used, El Habashy et al. reported 100% clinical success of both materials.41
Hashem et al. compared the success of IPT using calcium silicate (Biodentine) and glass ionomer (Fuji IX™ GP; GC Corporation, Tokyo, Japan), and in a 2-year follow-up period, the clinical success rates were found to be 77.8% for Biodentine and 66.7% for Fuji IX.42
When clinicians are determining the biomaterial to be selected, the advantages of the material in clinical use should be evaluated. In hospitals providing oral and dental health services to the community, Dycal is the most frequently applied clinical material.43
In a study by Rahman et al., IPT was applied to young permanent teeth throughout 24 months, and the success rates were found to be 77.8% for CH, 94.4% for Biodentine, and 100% for TheraCal.44
In another study by Oğlakçıoğlu and Pamir, direct and indirect pulp capping was applied to teeth with deep dentin decay using CH (Dycal) as the coverage material. The 6-month follow-up results of the clinical examinations of the continued vitality of the teeth showed that vitality and functions were maintained in 92% of the teeth with no clinical or radiographic findings. The teeth in which failure was observed all had primary decay lesions and had been applied with Dycal and composite resin after preparation of the cavity.10 The results of the current study support these findings, with success rates of 95.2% for Biodentine, 91.7% for Dycal and 90.1% for TheraCal PT at both 6 and 12 months in IPT applied to teeth with deep dentin decay. No statistically significant difference was determined between these rates. The main reason why the 3 pulp capping materials exhibit similar success rates may be that the pulp is not directly exposed and there is little dentin barrier.
In a study with a 2-year follow-up period, Mente et al. applied DPC using MTA and CH, and reported success rates of 80.5% in the teeth treated with MTA and 59% for those treated with CH.45
Biodentine has been shown to stimulate odontoblast-like differentiation and secretion of TGF-β1, an important growth factor. It has been shown to induce odontoblastic differentiation and increase mineralization in human dental pulp stem cells.40, 46
In our study, the reason for the higher success rate in DPC of Biodentine compared to the other 2 materials (Dycal and TheraCal PT) may be that it increases repair dentin mineralization by inducing odontoblastic differentiation.
Light-hardened materials for VPT have been introduced by combining the superior use of resin with the desirable bioactive characteristics of calcium silicate cements. The fact that the hardening reaction occurs immediately and the restoration can be completed in a single session is seen as an advantage.36
Wassel et al. applied calcium silicate modified with dual-cured resin (TheraCal PT) and after a 12-month follow-up period of IPT, DPC, partial pulpotomy, and pulpotomy treatment, the success rates were found to be 93.87% in IPT, 80.4% in DPC, 96.15% in pulpotomy, and 57.4% in partial pulpotomy. The failure in partial pulpotomy was attributed to uncontrolled bleeding, the gap between TheraCal PT and the amputation region, and insufficient disinfection before amputation, associated with misdiagnosis of the pulp status.47
Peskersoy et al. investigated the in vivo efficacy of different calcium silicate-based materials (Dycal, LC Calcihyd, Theracal LC, Biodentine, BioMTA) in DPC related to the pulp exposure status (<0.5 mm and 0.5–1 mm) and reported that the success rates of Biodentine and MTA were high at the end of 1 year and 3 years. The lowest success rate was seen in LC Calcihyd, and no statistically significant difference was determined between TheraCal LC and Dycal.7
Covaci et al. performed IPT and DPC to teeth with deep dentin decay using different materials (Life Kerr AC, TheraCal LC, Calcimol LC), and reported the survival rates to be 100% for Life Kerr AC, 92% for TheraCal LC and 83.87% for Calcimol LC, with no significant difference determined between the materials. Although self-hardening CH material showed better results than both CH and calcium silicate materials hardened with light, the difference between them was not significant.3 Throughout a 9-year follow-up period of DPC applied with calcium silicate (MTA), Bogen et al. reported positive results in 97.96%. All the teeth in young patients with exposed apexes initially showed completed root formation (apexogenesis).5 In a study by Harms et al., DPC using calcium silicate (Biodentine) was clinically evaluated after mean 2.3 years, and it was reported that patient age and gender, tooth type, arch type, and spontaneous pain before treatment did not affect the treatment results.48 Therefore, the hypothesis that pulp capping should be avoided in elderly patients or in teeth with pain or discomfort was rejected.
The most recent data have shown the capacity of the pulp to respond by triggering dentin pulp regeneration with an inflammatory reaction. Materials containing resin, such as TheraCal, shift the response of the pulp towards an inflammatory reaction while changing the regeneration process.24 In contrast, materials not containing resin, such as Biodentine, have anti-inflammatory potential and induce the pulp regeneration capacity. This information contradicts the recent tendency for the development of resin-based calcium silicate hybrid materials for pulp capping.24 In the current study, the low success rate in DPC of TheraCal PT, which contains resin and has a dual-cure hardening reaction, could be attributed to the resin content and polymerization shrinkage. In contrast, materials not containing resin such as Biodentine have anti-inflammatory potential and induce the pulp regeneration capacity.46
Wang et al., in their study investigating the bioinductive effects of MTA and Biodentine on lipopolysaccharide-induced pulp cells with different severities of inflammation, showed that more Dentin sialophosphoprotein developed in both normal and lipopolysaccharide-induced pulp cells at 48 and 96 h. This may mean that Biodentine treatment is not affected by the duration of inflammation.49
Suhag et al. compared the pulp capping success rates and postoperative pain using CH and MTA in teeth with deep dentin decay and irreversible pulpitis. The results of thier study showed that treatment with DPC could be successful, and MTA was found to be better than CH in terms of success rates and pain severity.50
Ricucci et al. performed DPC on teeth clinically diagnosed with reversible pulpitis and exposed pulp due to advanced caries and reported long-term DPC success rates of 100% at 1 year, 95% at 5 and 10 years, 86% at 20 years, and 89% at 35 years. Especially in the first 10 years of follow-up of the treatment, a very high success rate was observed in DPC with CH. The main variable significantly affecting the treatment results in all the follow-up periods was found to be the quality of the coronal restoration.51
The follow-up period in the current study was 12 months, which seemed to be insufficient compared to the previous studies.39, 41, 44, 47 In parallel with other studies, the success rate was determined to be high in IPT when all the treated teeth were evaluated. In the clinical and radiographic evaluations of DPC at the end of 6-month follow-up, the success rates were seen to be 96.0% in the Biodentine group, 81.8% in the Dycal group and 63.2% in the TheraCal PT group, and after 12 months these rates were 96.0% for Biodentine, 68.2% for Dycal and 63.2% for TheraCal PT. However, the results at 2 different times were not statistically significant. The high success rate of Biodentine was believed to be due to the calcium silicate content, biocompatibility and the property of not showing microleakage of the material. The low success rate of Dycal with CH content at 6 months and the decrease over time was considered to be due to the absence of the property of excellent impermeability and that composite restoration was applied over the Dycal capping material in this study. The low success rate of TheraCal PT can be attributed to the fact that it does not show ideal impermeability because of the resin content and polymerization shrinkage.
Limitations
There are some limitations to this study. First, the post-treatment follow-up period was 12 months, which was insufficient for monitoring vital tooth functions. Second, the sample size was insufficient; therefore, larger sample sizes should be employed in future studies.
Conclusions
In IPT CH (Dycal), calcium silicate (Biodentine) and calcium silicate with resin content (TheraCal PT) showed high clinical and radiological success. Direct pulp capping, Biodentine containing calcium silicate was found to be more successful than CH (Dycal) and calcium silicate with resin content (TheraCal PT).
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Consent for publication
Not applicable.
Use of AI and AI-assisted technologies
Not applicable.