Abstract
Background. Dementia, a rapidly growing cognitive disorder, has a profound impact on the lives of individuals and their caregivers across the globe. Digital life storybooks have emerged as a promising non-pharmacological intervention to improve the wellbeing of people living with dementia (PLWD).
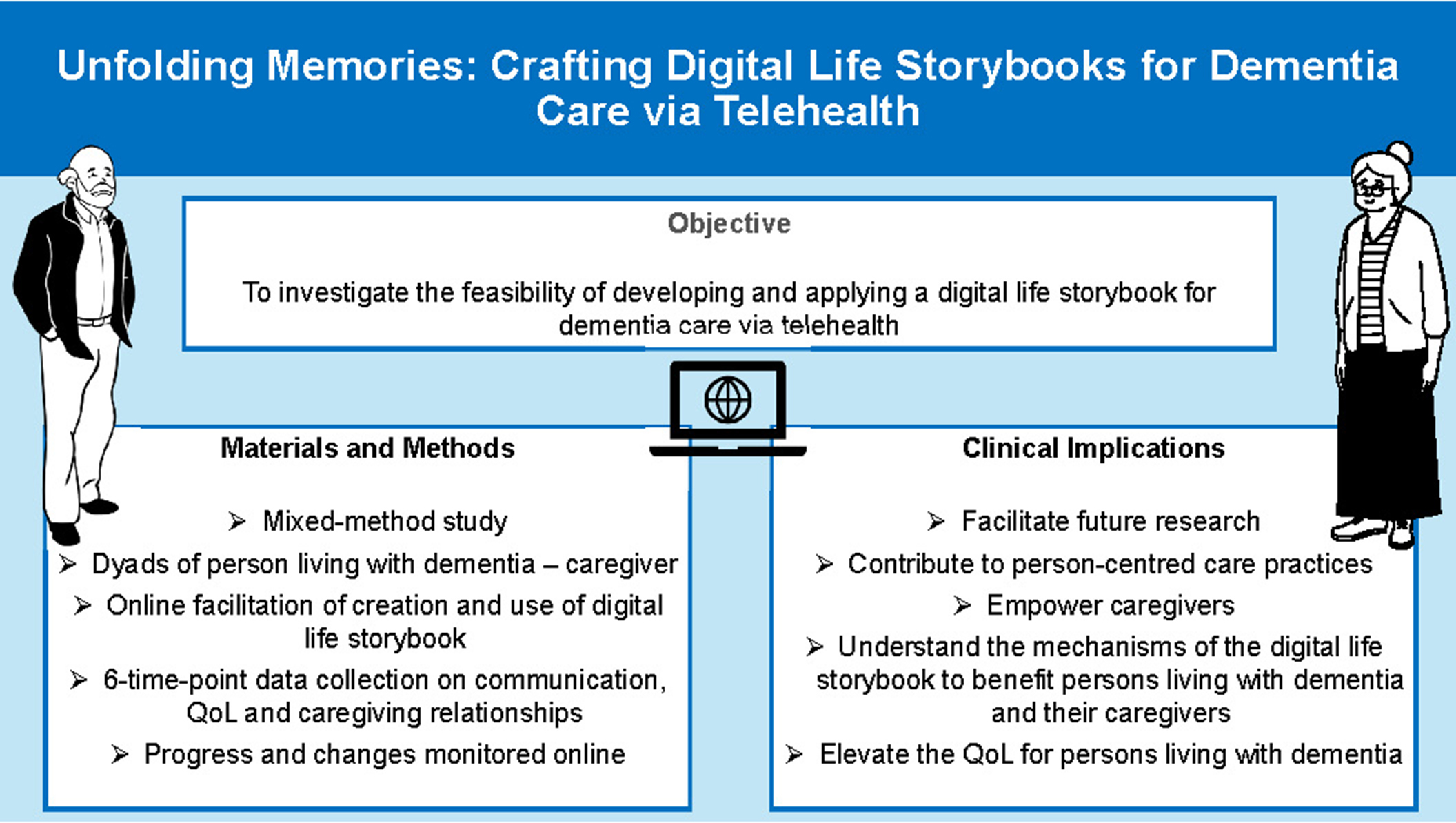
Objectives. This study aims to investigate the feasibility of developing and applying a digital life storybook for PLWD using telehealth, while evaluating its impact on communication skills, quality of life (QoL) and satisfaction levels.
Material and methods. A mixed-method study design will be employed, involving pairs of PLWD and their primary caregivers (dyads) recruited from a teaching hospital and a non-profit organization in Malaysia. The intervention involves the creation and use of a digital life storybook facilitated remotely via telehealth channels. Data will be collected at 6 points in time: prior to the commencement of development, prior to the submission of an application, on a biweekly basis, and at the conclusion of the assessment period. Quantitative measures will include the Holden Communication Scale, Quality of Life-Alzheimer’s Disease Scale (QoL-AD) and Quality of the Caregiving Relationship (QCPR) questionnaire. Qualitative data will be gathered through validated open-ended questions.
Results. Implications of the study include facilitating future research, contributing to person-centered care practices, and providing caregivers with tools to better understand and connect with PLWD. The findings will contribute to the understanding of the mechanisms through which digital life storybooks can benefit PLWD and their caregivers.
Conclusions. The successful implementation of this protocol could have significant implications for dementia care in both formal and informal settings, and could ultimately improve the lives of those affected by dementia.
Key words: dementia, training, caregiver, telehealth, digital life storybook
Introduction
Dementia has emerged as one of the most rapidly growing disorders, contributing to significant disability among the elderly population worldwide.1, 2, 3 Recent estimates suggest that around 55 million people globally are affected by dementia, with this number expected to double every 20 years.4, 5, 6 This progressive condition can impact various cognitive functions, including memory, language, judgment, visuospatial abilities, personality, and communication,3, 7, 8 ultimately leading to dependence on caregivers.9, 10
Treatment of dementia has focused primarily on slowing the progression of symptoms through medication and therapy, as a definitive cure for dementia remains elusive.11, 12, 13 Non-pharmacological interventions aim to maintain or improve cognitive ability,14, 15, 16 communication and social interaction, and reduce behavioral symptoms in people living with dementia (PLWD), which can ultimately enhance their overall quality of life (QoL).17, 18, 19, 20 Among these interventions, life storybooks have proven to be effective in the treatment of dementia, including improving mood, cognition, e.g., memory, maintaining identity, and overall wellbeing of PLWD.21, 22, 23, 24
A life storybook is a carefully crafted volume containing personalized photographs, familiar music and memorabilia, accompanied by concise text or captions that represent key events, important people and treasured memories from an individual’s life story.25, 26, 27, 28 Traditionally, the creation and development of life storybooks have relied on tangible prompts or memory cues to stimulate discussion and recollection of past activities and experiences, often taking the form of books, scrapbooks, photo albums, or memory books.28, 29 However, technological advancements have facilitated the development of digital life storybooks specifically designed for PLWD.30, 31, 32 These interventions have taken various forms, such as interactive multimedia storytelling devices,33 multimedia biographies,34 reminiscence work using platforms like YouTube and the internet,35 and the creation of personalized multimedia systems and digital life stories using life-logging entities.36, 37, 38 As emphasized by researchers,17 digital life storybooks offer the unique advantage of incorporating music, a powerful memory trigger, along with other auditory elements, such as narration.39, 40, 41 By combining video clips with photographs and presenting content in a cinematic format, digital life storybooks facilitate easy viewing for individuals with dementia, both independently and in the presence of others.42, 43
A recent systematic review compiled different studies addressing the effects of life storybooks on relatives and highlighted the crucial role of family members in curating the content of life storybooks for individuals with dementia.44, 45, 46 Involving family members in this process ensures the authenticity, accuracy and personal relevance of the life storybook, capturing the rich tapestry of the individual’s life experiences.47, 48 As primary caregivers and close acquaintances, family members possess unique insights into the individual’s life history, preferences and cherished memories, enabling them to create a narrative that deeply resonates with the PLWD.49, 50 Moreover, this collaborative effort promotes a sense of connection and continuity for the individual, reinforcing their sense of identity and self-worth.51, 52 The active engagement of family members in crafting life storybooks represents a meaningful therapeutic intervention that enhances QoL for individuals navigating the challenges of dementia.19, 53
However, the onset of the COVID-19 pandemic necessitated a shift in healthcare delivery, prioritizing safety and minimizing physical contact.54, 55, 56, 57 In response to stringent pandemic restrictions, social distancing measures were widely adopted within healthcare settings.58, 59 This imperative accelerated the rapid integration of telehealth solutions, enabling the provision of essential medical services while reducing the risk of viral transmission.54, 60 By utilizing digital platforms and remote communication technologies, healthcare professionals were able to conduct consultations, monitor patient progress and provide timely medical advice, ensuring continuity of care in alignment with public health guidelines.61, 62, 63 This transformation in healthcare delivery not only highlights the adaptability of the medical field but also represents a significant advancement in leveraging technology to protect both patient and provider wellbeing during times of crisis.64, 65, 66, 67
The recent surge in interest in telehealth can be attributed to its multifaceted capabilities, which encompass a comprehensive range of clinical components. These include, but are not limited to, evaluation and assessment, ongoing monitoring, preventative measures, timely interventions, and expert consultations. In light of the increasing connectivity and digitalization of our world, telehealth has emerged as a comprehensive solution for the delivery of healthcare services.68, 69 It has demonstrated the potential to benefit the older adult population by overcoming geographical distances and providing easier access to healthcare, saving time and reducing travel costs.70, 71 Older adults receiving telehealth services have also reported high levels of satisfaction with the services provided, with minimal concerns.72, 73, 74 This adaptability underscores its potential to revolutionize healthcare delivery and improve accessibility, making it a crucial tool in modern healthcare systems.75, 76
A study by Laver et al.77 emphasized the advantages of using telehealth for dementia care, replacing face-to-face home visit services with digital health technologies. The study concluded that the use of telehealth technologies to deliver non-pharmacological interventions for individuals with dementia and their caregivers may reduce the costs of delivering the intervention, increase accessibility and facilitate research translation.78, 79 Findings from Cotelli et al.80 indicated that cognitive interventions delivered via telehealth to individuals with mild cognitive impairment are comparable to the same services delivered face-to-face.81, 82, 83 Furthermore, individuals with dementia and their caregivers have reported satisfaction with the use of telehealth for various outcomes, such as interaction with healthcare practitioners, addressing patient needs and its usefulness.70, 84, 85, 86
Telehealth used in dementia care services, especially for collaborative assessments, consultations and psychosocial interventions, has shown promising results in improving cognition, communication, overall QoL, reduced caregiver burden, and depression compared to those receiving the usual care.87, 88, 89 Despite numerous studies on various forms of digital life storybooks, research into the utilization of telehealth to train the development of material and use of digital life storybooks remains unpublished.31, 90 The feasibility of using digital life storybooks to enhance communication is also still scarce.91 The effectiveness of digital life storybooks on communication, social interaction, relationships, and QoL of individuals with dementia through the training of digital life storybooks is yet to be explored.92, 93
Adapting healthcare interventions in culturally congruent ways appears to increase the acceptability of these practices.94, 95 The benefits of using a life storybook for individuals with dementia, such as enhanced cognition, communication skills, reduced depression symptoms, and reduced caregiver burden, have been highlighted in previous studies.96, 97 Conventionally, reminiscence therapy using digital life storybooks has been conducted face-to-face.17, 28, 98 Previous studies have shown that telehealth has shielded individuals with dementia and cognitive decline from unnecessary exposure while also allowing providers to connect their patients to much-needed community services.72, 99, 100, 101 Thus, researchers need to study the outcomes of the benefits, acceptability and satisfaction,102 to report the feasibility of developing a digital life storybook using a telehealth modality among individuals with dementia.103, 104 More recently, in a single case study, Asano and Hird105 compared the outcomes of a digital life story intervention with online family participation to those of face-to-face sessions conducted without family participation. The online intervention was delivered under the same conditions as face-to-face (twice a week, 30 min per session, for 4 weeks) using the same life storybook. The results demonstrated that both online cognitive stimulations involving family participation and in-person intervention led to improvements in depression, apathy, caregiver distress, and cognitive function scores as measured by the Mini-Mental State Examination (MMSE). This indicates that family members’ remote participation could enhance the effectiveness of individualized cognitive stimulation, presenting a promising solution to accessibility challenges.
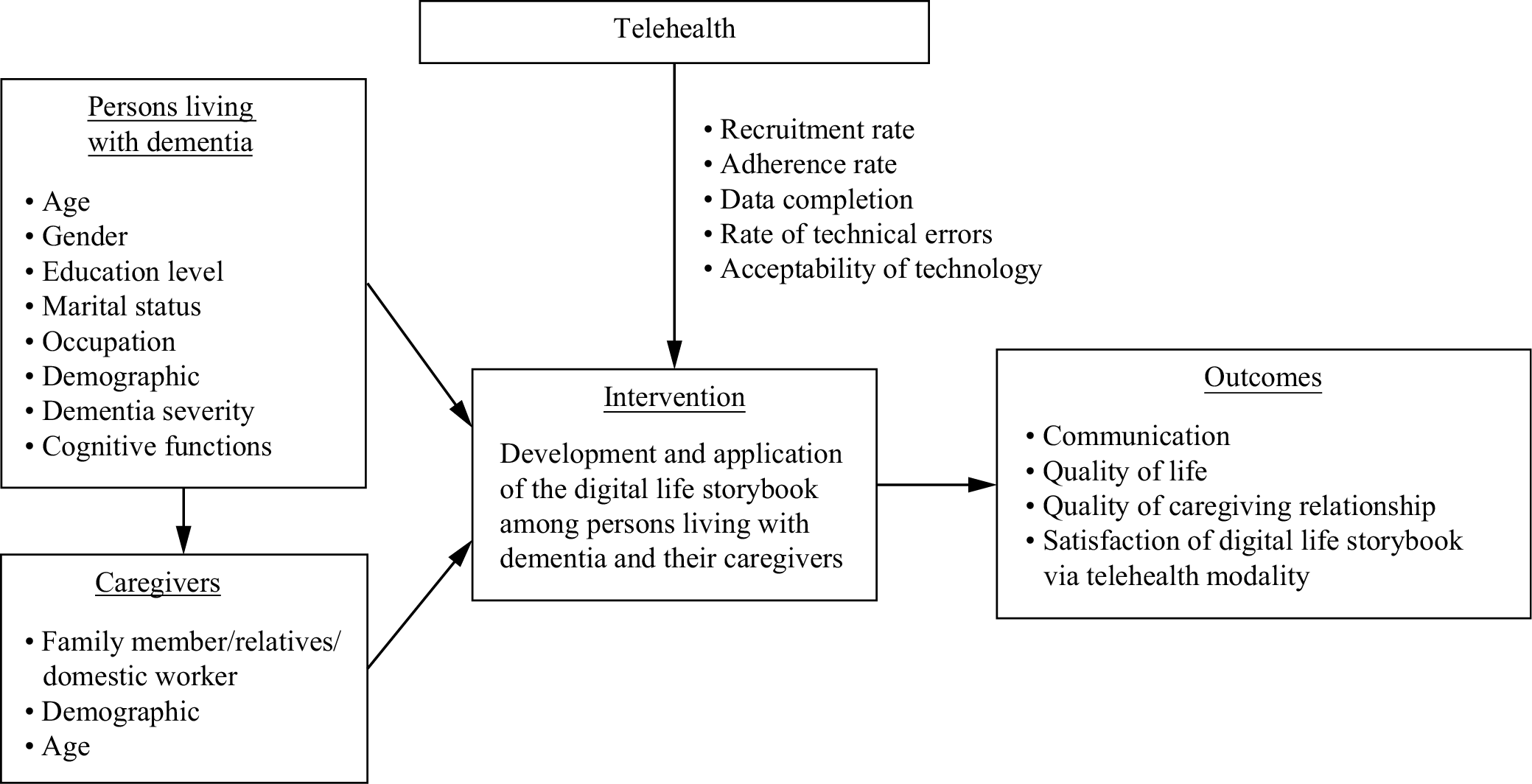
The current research, therefore, aimed to: 1) study the feasibility of developing a digital life storybook and its application for individuals with dementia via telehealth; 2) study the feasibility of applying a telehealth modality for the development of digital life storybooks for individuals with dementia; 3) compare the communication skills of individuals with dementia before and after using the digital life storybook via telehealth; 4) compare the QoL of individuals with dementia and their caregivers before and after using the digital life storybook via telehealth; and 5) evaluate the levels of satisfaction reported by individuals with dementia and their caregivers via telehealth. The conceptual framework of our research is presented in Figure 1.
Materials and methods
This mixed-method study is designed to investigate the feasibility of developing and applying a digital life storybook for PLWD using telehealth methods. The study design is based on previous research that has demonstrated the effectiveness of life storybooks in improving the wellbeing of PLWD22, 23, 24, 25 and the potential of telehealth in delivering non-pharmacological interventions for this population.72, 75, 85
Study design and setting
The study involves the entire process of creating and using the digital life storybook, facilitated remotely via telehealth channels. A secure and interactive platform, a subscribed version of Zoom (Zoom Communications, San Jose, USA), will serve as the primary medium for all sessions due to its security features and varied interactive functionalities.110 Preparatory training sessions focusing on Zoom navigation and its diverse features will precede the commencement of the digital life storybook’s creation and application for both the PLWD and their respective caregivers.
The digital life storybook’s construction involves the use of video editing software such as Wondershare FilmoraX (Wondershare Technology Group, Shenzen, China) or Windows Movie Maker (Microsoft Corp., Redmond, USA), undertaken by the researchers. This process entails compiling soft copies of photographs, images or videos displaying personal memorabilia, pertinent information, beloved songs, or music obtained from caregivers or family members. However, the responsibility of selecting relevant material and uploading chosen images, videos and songs onto a digital photo frame with audio-video capabilities lies with the caregiver or family, thereby maintaining the privacy of personal materials as the researchers refrain from direct involvement in this step.34 Nonetheless, the researchers will guide the caregiver or family concerning image selection and crafting simple statements for each image. Tangible memorabilia will remain in the possession of PLWD or their families to complement the digital life storybook during subsequent reminiscence sessions.
A participatory design approach will be employed in the creation of the digital life storybook, emphasizing the active involvement of PLWD in the decision-making processes, design concepts, content creation, and direction of their life narratives.17 Collaboratively, researchers and caregivers will serve as co-editors, engaging in this process. However, it is essential to note that such involvement is voluntary rather than obligatory. The development of the digital life storybook will be done through 2 different approaches: first, full engagement with the PLWD, including a life review process, or alternatively, independent preparation by caregivers or family members and then presented to the PLWD as a “gift”. Before the study commences, a comprehensive plan and design inclusive of a realistic timeline will be established. The structured process for constructing the digital life storybook will draw upon Subramaniam et al.’s29 research. Collaboration among PLWD, their caregivers, relatives, and researchers will entail compiling supplementary elements, including selecting and sourcing favored music, songs, video clips, and/or footage if available. The chronological organization of the digital life storybook will span from childhood to the present, segmented into distinct phases such as childhood, teenage years, career, mid-life, etc., based on available visual materials. This content will be enriched by background music, participants’ preferred songs and a narrated storyline. Aligning with the individual’s preferences, the chosen songs and music will accompany appropriate images whenever feasible. Additionally, expressions articulated by PLWD throughout the development process may be incorporated as quotations where fitting.
Narration will be provided by either the PLWD themselves or by caregivers/relatives. The spoken word will be reinforced by the text appearing on the screen or scrolling across the screen, in a clear font, allowing the PLWD sufficient time to read the words if they wish to do so. The language used for the narration will be preferred by the PLWD and not restricted.
Weekly online meetings between the researchers and the participant pairs (dyads) will be held to develop the digital life storybook, with each week focusing on 1 segment of the digital life storybook (e.g.: week 1: personal information; week 2: childhood; week 3: school; etc.). Each segment will be reviewed by the dyads (where possible) before moving on to the next segment of the digital life storybook. The dyads are allowed to amend each segment of the digital life storybook if they are not satisfied. The final product of the digital life storybook will be saved and uploaded to a digital photo book and mailed to the PLWD. Based on past research, it is expected that the digital life storybook will take approx. 7–10 weeks to develop and finalize.29
Online training will be provided to the dyads on how to use the finalized digital life storybook. For purposes of this study, the dyads will be required to use the digital life storybook a minimum of 4 days a week, with each session lasting between 45 and 50 min, for 8 consecutive weeks.
Participants
Participants will be selected via purposive sampling techniques and recruited from the inpatient and outpatient caseloads of the geriatric medicine, family medicine and psychology clinics at a prominent teaching hospital in Malaysia and from a non-profit organization that supports people with Alzheimer’s disease and their caregivers in Malaysia. The potential participants will be contacted via the phone to get their oral and written consent to be involved in this study.
To be included in the study, dyads will comprise people living with mild-to-moderate dementia and their primary caregivers (family/relatives) who would consent to participate in the research. Caregivers involved will have to be adult family members or relatives (aged 18 years and above) or their domestic helpers who can ensure access to maximal personalized information for the digital life storybook. The caregivers of PLWD should also have functional cognitive abilities and be able to independently perform functions of daily life. The dyads must be able to speak, read and write in a common language and must be able to commit to a period of 4–6 months for this study.
The dyads should have access to personal photographs/videos and/or memorabilia of PLWD and a personal computer, laptop, iPad or tablet with stable internet connections. However, they are not required to have any knowledge or skills associated with computers and technology and will not be required to control the digital life storybook system before this study.
Any PLWD with high medical dependency, moderate-to-severe (or greater) levels of cognitive impairment as indicated within their medical history, significant auditory or visual impairments, and major psychiatric or other mental health issues will be excluded from participating.
Sample size calculation
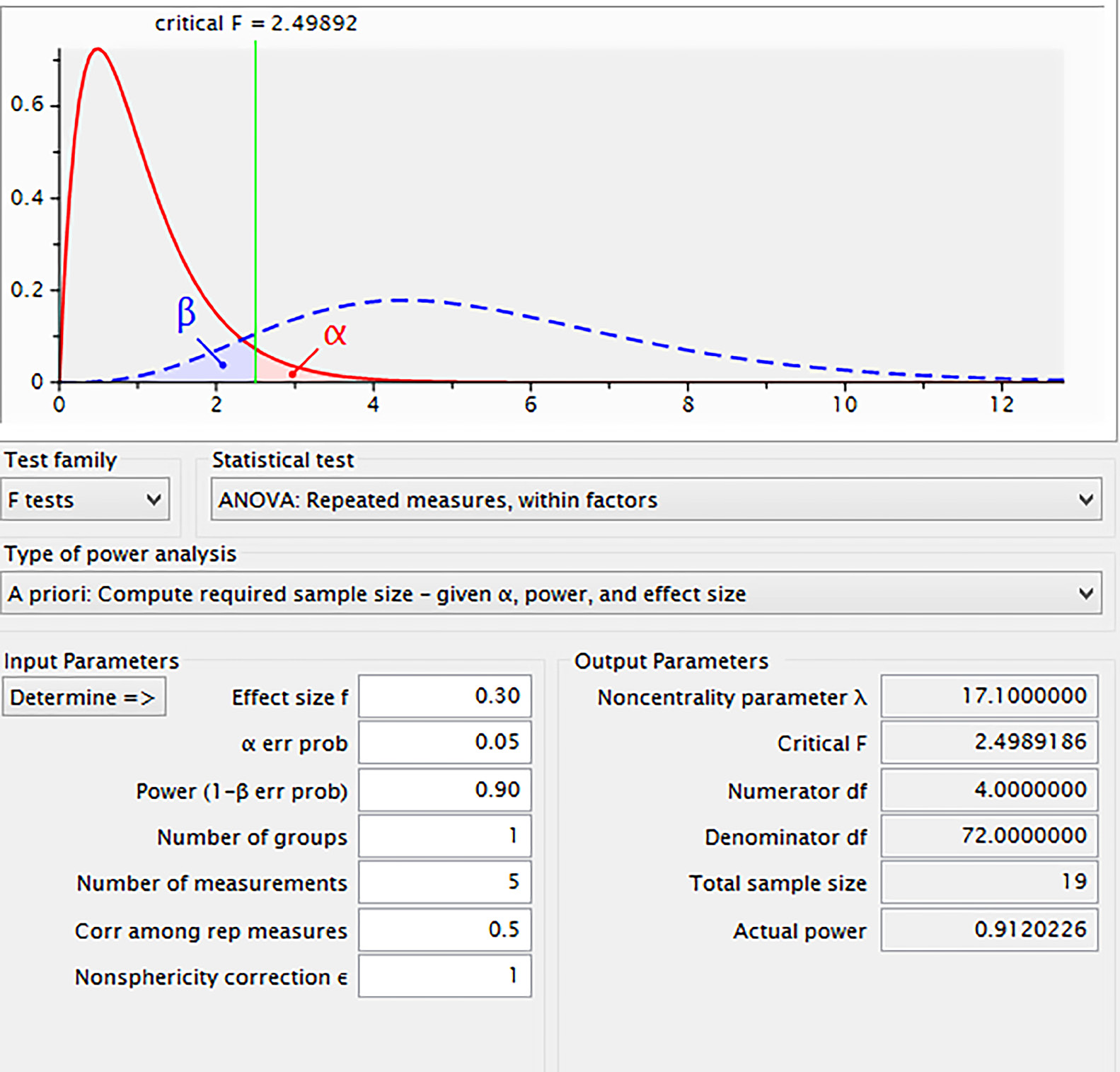
A priori power analysis was conducted using G*Power3,106 for repeated measures analysis of variance (ANOVA) with a single group, a medium effect size (d = 0.30), and an α of 0.05 as shown in Figure 2. A dropout rate of 15% is anticipated, with a minimum of 22 participants needed to achieve a power of 0.90. Hence, this research will involve 22 dyads of participants who meet the inclusion criteria.
Data collection
The dyads will commence the study immediately upon consenting to participate. All questionnaires will be sent to the participants as editable PDF files or Google Forms (Google LLC, Mountain View, USA), to be completed online. Data will be collected at 6 points of time during the study period: pre-development, baseline (T0); pre-application (T1); follow-up assessment (T2, T3, T4) biweekly; and final assessment (T5) 2 weeks after T4. Progress will be monitored online using Zoom and all sessions will be video/audio recorded to allow for the monitoring of variations or changes in communication and didactic interactions. Records of the date, day and duration of digital life storybook usage will be charted in the record form provided to the participants. The main researcher will administer all the assessments during each point of time.
Information regarding the PLWD will be obtained from medical records and based on the formal diagnosis by the attending physician. Several screening tools will also be used to select the potential participants based on the inclusion and exclusion criteria of this study to determine the severity of dementia, cognitive level and depression level respectively by the main researcher before the commencement of this study:
1) Clinical Dementia Rating (CDR).107 The CDR is a clinician-rated dementia staging system with 5 levels – from no dementia to severe dementia. The CDR scores are healthy = 0; questionable dementia = 0.5; mild dementia = 1; moderate dementia = 2; severe dementia = 3.
2) MiniMental State Examination.108 The MMSE is a 30-point test used to measure the cognitive status in adults which includes orientation, attention, memory, language, and visual-spatial skills.
3) Geriatric Depression Scale (GDS).109 The GDS is a brief self-reported depression scale (yes/no) for older adults with a higher score indicating severe depression. In the GDS, a score of 0–9 is considered normal, 10–19 demonstrates mild depressive symptoms and 20–30 shows severe depression.
To evaluate the feasibility of the development and application of the digital life storybook via telehealth, recruitment rate, adherence and retention rate, data completion, rate of technical errors during videoconferencing, and acceptability of technology will be evaluated.110 The study will collect data to measure and compare the communication skills and QoL of people living with dementia, as well as the QoL of their caregivers throughout the study period.
The following measures will be used to monitor changes over time across the study duration:
1) Holden Communication Scale (HCS).111 The HCS consists of 12 items assessing the conversation, awareness, knowledge and communication in both aspects of verbal and non-verbal communication. Each item contains 5 response options, ranging from 0 to 4, where higher scores indicate more difficulties in communication. The Cronbach’s α of the HCS is 0.94 and test–retest reliability is r = 0.71. The Malay version of HCS will be translated and validated using content validity.
2) Quality of life-Alzheimer’s Disease Scale (QOL-AD).112 The QOL-AD is a 13-item questionnaire used to interview a PLWD to gather an indication of self-reported QoL via 4-point Likert scale items, with higher scores indicating higher QoL. Interrater reliability was excellent with all Cohen’s κ values >0.70. Internal consistency was excellent with a Cronbach’s α coefficient of 0.82.
3) Quality of Carer–Patient Relationship Scale (QCPR).113 The QCPR is a 14-item questionnaire with 2 subscales, will be used to measure the quality of caregiving relationship between the PLWD and their caregiver/relatives. The questionnaire consists of 14 5-point Likert scale items, where a higher overall score on this scale indicates a higher relationship quality.
Qualitative measurements
To gather more in-depth information regarding the satisfactory levels of the development and application of the digital life storybook via telehealth and the perceived value of the digital life storybook, a set of open-ended questions will be developed and validated. The caregiver and the PLWD will be asked the same questions separately in verbal interviews. The questions will cover feelings and thoughts about the content of the digital life storybook, the benefits of the digital life storybook, the repeat-watching experience, the ease of use of the telehealth modality, perceived strengths and challenges of the telehealth modality, and anything else they would like to share.
Data analysis
Quantitative data will be analyzed using the IBM SPSS software (IBM Corp., Armonk, USA). The demographic data of the dyads will be analyzed descriptively. The changes in communication skills of PLWD, QoL of PLWD and the quality of the caregiving relationship will be determined using a paired t-test at pre-development (baseline assessment) with post-development of the digital life storybook, and post-development with post application (final assessment) of the digital life storybook. A repeated-measures ANOVA will be employed to assess the changes from the post-development to the post-application of the digital life storybook. A value of p < 0.05 will be considered significant.
The qualitative data on the satisfaction levels of the development and application of the digital life storybook via telehealth and the perceived value of the digital life storybook will be analyzed thematically using the NVivo software (QSR International, Burlington, USA). The responses from the semi-structured interviews will be transcribed, and the coded data read and re-read and grouped according to emerging themes and reviewed. Each theme will be defined and named. The process will be counter-checked by members of the research team.
Discussion
The present study introduces an innovative online training protocol designed to empower caregivers in utilizing digital life storybooks for PLWD. This protocol adopts a participatory design approach in developing digital life storybooks via telehealth, aiming to explore their impact on communication skills and QoL for up to 2 months post-utilization. Additionally, it seeks to assess the satisfaction of both PLWD and their caregivers through qualitative interviews.
This approach builds upon the strengths of both telehealth and life storybooks, offering enhanced accessibility, flexibility and potential for personalized care. The protocol addresses key limitations of traditional training methods by enabling caregivers to access educational resources irrespective of geographical barriers and tailor their learning experience to their schedules.
Previous research has demonstrated that developing digital life storybooks via telehealth is as beneficial as face-to-face sessions for PLWD and their caregivers.20, 21 Similar findings were presented in the single case study by Asano and Hird105 with online family participation. Telehealth-based development offers several advantages, including broader geographical reach, cost-effectiveness and time efficiency. Researchers showed that remotely delivered interventions involving caregivers of PLWD were both useful and effective.114 A systematic review115 of the use of technology in creating individualized, meaningful activities for PLWD also summarized that the use of technology in creating individualized, meaningful activities seems to be promising in terms of improving behavior and promoting relationships with others and that future studies should aim to build a more concrete evidence base by improving the methodological quality of research in the area. However, a standardized protocol for developing digital life storybooks via telehealth has been lacking.
This study introduces an online training program for creating digital life storybooks, building upon previous work in the field17, 116 and aims to identify if online development/use of digital life storybooks through the proposed protocol will contribute to better use of technology for such services within PLWD and their caregivers. By providing a structured, accessible and user-friendly platform, this protocol has the potential to facilitate the effective implementation of digital life storybooks in various care settings.
Serving as a proof of concept, this study represents an initial step towards establishing the feasibility of developing life storybooks via telehealth. It lays the groundwork for gathering evidence to support this approach in future research and practice. The potential implications of this new protocol are far-reaching, providing a standardized framework for evaluating the impact of digital life storybooks on the wellbeing of PLWD and their caregivers. Moreover, widespread adoption of this protocol could contribute to a shift towards more person-centered care practices by equipping caregivers with tools to better understand and connect with the individuals they support.
From a theoretical perspective, this study contributes to our understanding of the mechanisms through which digital life storybooks can benefit individuals with dementia and their caregivers. It highlights the importance of capturing and honoring an individual’s unique life experiences and the role that technology can play in facilitating this process. Future research could explore the potential for integrating online training programs with other therapeutic approaches, such as reminiscence therapy29 or cognitive stimulation therapy.117
In terms of translational applications, the successful implementation of this protocol could have significant implications for dementia care delivery in both formal and informal care settings. The integration of these training programs into clinical practice may lead to more efficient and coordinated care delivery, fostering collaboration between formal and informal caregivers.
Limitations
It is important to acknowledge the limitations of this study, including technical challenges, access barriers, and the necessity for ongoing support and resources to ensure the successful integration of acquired knowledge into daily care routines. To address these limitations, the protocol incorporates user-friendly technology, simplified navigation and continuous reinforcement strategies.
Future studies should focus on addressing the identified limitations, such as technical barriers, personalization constraints and the practical application of acquired skills. Efforts should be made to develop user-friendly platforms, provide ongoing support and resources, and evaluate the efficacy of the intervention in diverse care settings. These endeavors will contribute to the refinement and broader applicability of digital life storybook interventions in dementia care.
Conclusions
This study introduces an innovative online training program for utilizing digital life storybooks in dementia care, offering a promising approach to enhance person-centered care and empower caregivers. The protocol demonstrates the potential for improving communication and relationship-building between caregivers and PLWD. Theoretically, this research advances our understanding of technology-mediated reminiscence by exploring how digital platforms can preserve and present autobiographical memories, contributing to the emerging field of digital gerontechnology. The implications are substantial, with the potential to revolutionize care delivery by enabling remote, personalized interventions. However, challenges remain, including the digital literacy of older caregivers and the technical infrastructure in nursing homes. Future research should address these limitations, perhaps by incorporating adaptive learning features to tailor the user interface to individual comfort levels with technology. Integration with complementary approaches, such as combining digital life storybooks with cognitive stimulation therapy, presents an exciting frontier for holistic dementia care. By refining this protocol through ongoing research and interdisciplinary collaboration, we can work towards a future where technology-enhanced, person-centered care becomes the standard, potentially reducing caregiver burden and improving QoL for PLWD. This study marks a significant step towards a future where technology-enhanced, person-centered care becomes the standard in dementia support and treatment.