Abstract
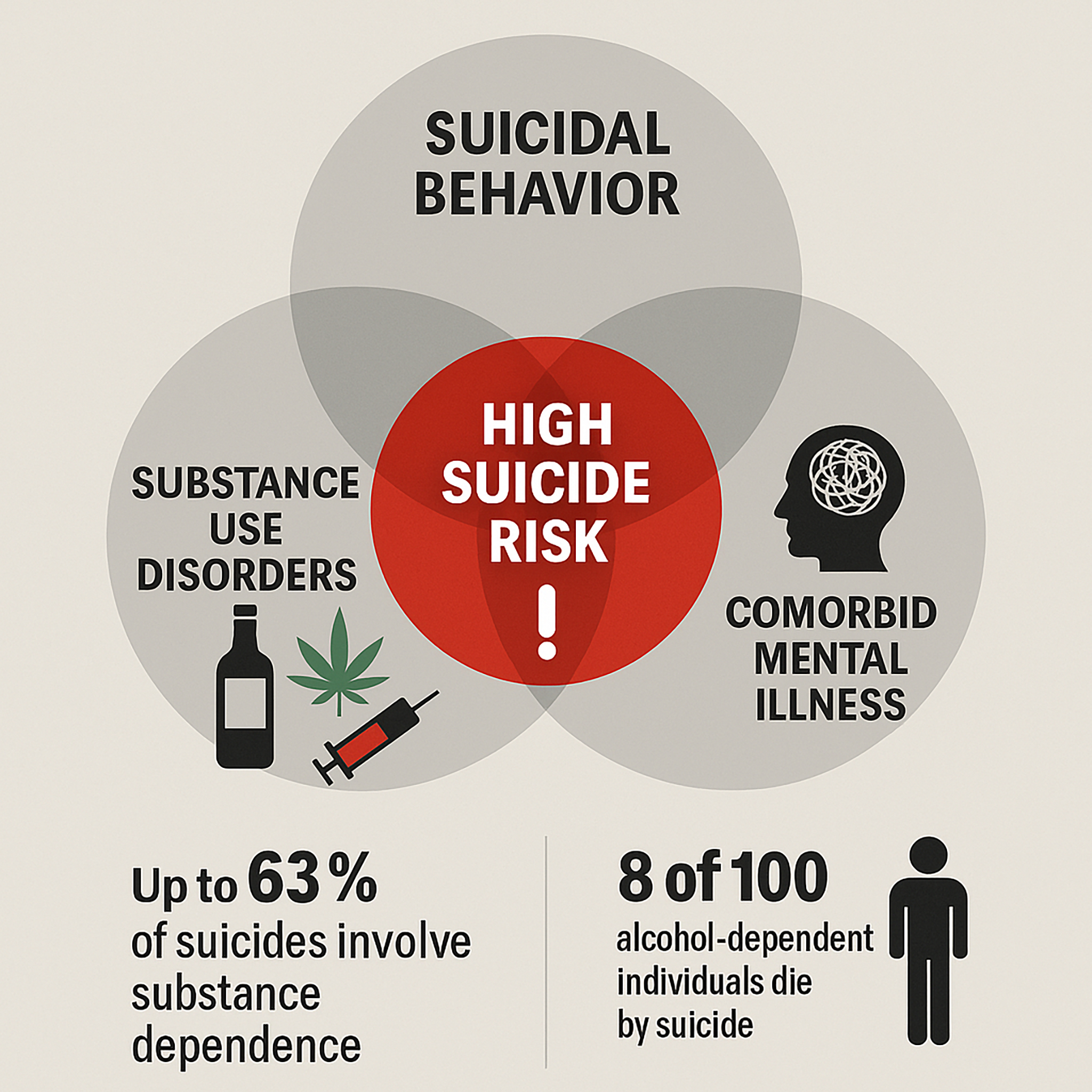
Suicidal behavior is a common psychiatric emergency and poses a significant challenge in mental health care. Substance use disorders are among the most frequently observed mental health conditions in individuals who die by suicide.
Key words: suicide, alcoholism, substance-related disorders
Introduction: Substance use disorder and suicide
Substance use disorders (SUDs) and suicidal behavior are both of great importance in medical and psychosocial care.1, 2 In Western countries, the majority of suicides are linked to mental disorders, with alcohol use disorders accounting for approx. 22% of all suicide cases.3, 4, 5, 6 Considering important association between suicide and SUDs, the following narrative review aims to provide a comprehensive overview of the current scientific knowledge covering the most important studies in this field. We conducted a literature search across multiple databases (PubMed, Embase, Web of Science, and PubPsych). Psychological autopsy studies indicate that nearly 1/3 of male suicides and approx. 15% of female suicides involved SUDs. Meta-analyses of cohort studies, primarily involving inpatient populations, and controlled studies using the psychological autopsy method have demonstrated that SUDs are associated with a substantially increased risk of suicide.7, 8, 9, 10 Substance dependence has been shown to elevate suicide risk by a factor of 3 to 17.9, 11
Among individuals with addiction who died by suicide, women were significantly more likely than men to have experienced sexual abuse, to be dependent on prescription drugs and to have a history of previous suicide attempts. Addicted women were also generally younger, more likely to be intoxicated at the time of death, and tended to use less violent methods compared to non-addicted women.12, 13
Different psychotropic drugs and suicide risk
The following list details the suicide risks associated with different psychotropic substances.
– Between 15% and 61% of all suicides were alcohol-related.7 The lifetime risk of suicide for alcohol-dependent people is around 8% and remains constant over lifetime.14, 15 Alcoholism has repeatedly been identified as a significant risk factor for all forms of suicidal behavior, despite differences in diagnostic systems, age groups and proportion of men.7, 8, 16 The risk of suicide in alcoholism is particularly high in middle age17, 18, 19; between the ages of 20 and 50, the risk rose sharply, especially in the presence of a depressive disorder.20 Worldwide, the prevalence of alcohol use disorders is higher among men than among women.21, 22 However, women with alcohol use disorders have a higher risk of suicide than men (up to 10 times higher in men and up to 16 times higher in women than in the general population).16
– The following risk factors for suicide in alcoholism have been identified7:
• heavy drinking (equivalent to at least 70 g alcohol/day);
• nicotine consumption of more than 20 cigarettes per day;
• suicide “threats”;
• living alone;
• little social support;
• relationship problems and breakups;
• little schooling, previous suicide attempts;
• comorbidity with affective disorders.
After adjustment for other mental disorders, the risk of suicide associated with alcohol dependence decreases.23 The risk of suicide attempts was 27 times higher in alcoholics than in the general population after 25 years.24
– Smoking is associated with an about twofold increased risk of suicide in both, men and women, even after adjustment (i.e., statistical correction) for mental illness and other, mostly sociodemographic factors.7, 25 The risk of suicide increased by an additional 24% for every 10 cigarettes smoked.26 In contrast to current smokers, former smokers do not have an increased risk of suicide.26 Nicotine dependence increased the risk of attempted suicide by almost a factor of 1, even after adjustment for sociodemographic characteristics and other mental and physical illnesses.27
– Young men with cannabis use disorder had a 2.56-fold higher risk of suicide compared to the general population.28 After 30 years of follow-up, risk of suicide was not increased after adjustment for confounding variables, including psychiatric diagnosis, social relationships, parental use of psychotropic medication, alcohol consumption, cigarette smoking, and use of other drugs.29 Chronic or heavy cannabis use can increase the risk of suicidal ideation (odds ratio (OR) = 2.5) and suicide attempts (OR = 3.2).28
– Opioid and opiate use were associated with a 14-fold increase in the risk of suicide compared to the general population.8 Heroin users in a methadone substitution program, although methadone reduces suicidal behavior (compared to heroin users who are not in a substitution program),30 had an 18.4 times higher risk of suicide than the general population.31 Particularly high risk was observed for female users (standardized mortality ratio (SMR) = 27.0).31 Female gender and psychopathology (depressed mood, inadequate behavior, suicidal intent, fear of psychological disintegration, insight into the psychopathology, high self-expectations) were associated with suicide among heroin users.32
– Among all acute illicit drug use, cocaine use is most frequently associated with suicide.33 Mixed drug use is associated with a 16- to 20-fold increase in suicide risk.8 The concurrent use of alcohol with illicit drugs further elevates this risk.34 Furthermore, the data indicates that among individuals who use drugs, 21.9% have attempted suicide, a figure that rises to 42.2% for those who use heroin.35
Comorbidity
Comorbidities of addictive disorders with other mental disorders and with physical illnesses are very common. It has been found that drug use increases the risk of suicide among people with schizophrenia.36 The comorbidity of psychotropic use disorders and affective disorders has been associated with a particularly high risk of suicide, even in adolescents.37, 38 Conner et al.39 found that the comorbidity of depressive disorders and alcohol dependence increased the risk of suicide by a factor of 4.5 in 20-year-olds and by a factor of 83 in those over 50.
Potential mechanisms linking SUDs and suicidal behavior
Suicidal behavior is thought to be triggered by an interplay between genetic, psychological and environmental factors.40 All psychotropic substances affect the body’s neurotransmitter systems, and current evidence suggests that neurobiological factors are likely to lead to suicidal behavior, in particular, deficits in serotonin.41 There are only a few models that have been developed to explain the association between SUDs and suicidal behavior.1, 42, 43, 44 These models include predisposing and triggering factors, such as impulsiveness, hopelessness, lack of social support, aggressivity, low self-worth, interpersonal conflicts, and the experience of being offended. Sometimes, people use psychotropic substances when feeling helpless and aggressive. However, substance use can increase aggression and impair cognitive abilities, resulting in a lack of alternative coping strategies.42
Therapeutic interventions
Treatment of suicidal behavior must include the treatment of SUDs and that of comorbid mental disorders. Use of medications for maintaining abstinence in alcohol dependence and opioid dependence (naltrexone, acamprosate, buprenorphine, and methadone) should be offered. A significant reduction of suicidal behavior has only been found in the treatment with the opioid agonist methadone in opioid dependent patients compared to patients without opioid agonist treatment (hazard ratio (HR) = 0.60).30 Comorbidity of schizophrenia and affective disorders must also be treated: Clozapine was found to significantly reduce suicides and suicide attempts in patients with schizophrenia (OR = 0.23).45 Long-term lithium treatment, when compared to a placebo or other drugs, was associated with a reduction in death by suicide and suicide attempts, particularly in individuals with bipolar disorder.46, 47 There is currently no evidence that other psychotropic drugs, such as serotonin reuptake inhibitors and other antidepressants, reduce suicidal behavior.48 Preliminary evidence for the short-term efficacy of ketamine in suicidal behavior was noted by the majority of reviews; however, long-term effects remained unknown and also effects in addicted subjects must be reconsidered. Due to the low quality of many studies and the limitations of core studies, further research, in particular in SUDs, is required.49
Inpatient treatment, if necessary, under protected conditions, is indicated for acute suicidal behavior. Accepting suicidal behavior as a distress signal, understanding the meaning and subjective necessity of this signal, and dealing with failed coping attempts are the basic prerequisites for treatment in a suicidal crisis.50 The most important prerequisite for effective crisis intervention is the development of a trusting and sustainable relationship that allows patients to talk openly about their current complaints and the situation that triggers suicidal behavior.50 Particular attention must be paid to the increasing narrowing of personal options and the loss of interpersonal relationships in the case of suicidal behavior of substance abusers.
Special challenges in the treatment of suicidal substance users
Special challenges arise due to the affective symptoms that frequently occur during detoxification and withdrawal treatment: These are particularly depression, cognitive impairment, increased aggression, and impulsivity, which are often associated with suicidal behavior.42 A variety of difficulties can occur throughout the whole treatment of suicidal addicts.51 The quality of the relationship between patient and therapist significantly impacts the recognition of suicidality, but it is often difficult to establish a stable, trusting relationship. Overcoming a crisis takes time. However, addicts often “flee” back into substance use quickly and often use psychotropic substances as a form of self-medication, in particular in comorbid mental health conditions. Further medical treatment is frequently inseparable from psychiatric treatment, including treatment of suicidal behavior. Suicides of people with dependence disorders often occur outside the system of medical and psychosocial care. As a consequence of the circumstances of abuse (e.g., intoxication),52 unstable living conditions and a lack of social integration, suicidal addicts often cannot be reached (in time) by the suicide prevention support system. Further research on pharmacological and psychosocial interventions is necessary.53
Limitations
However, there are several limitations to epidemiological research into the relationship between SUDs and suicidal behavior. Although there is already extensive research on SUDs and suicide in general, recent and high-quality studies on this topic are lacking, especially in Europe. There is a lack of standardized measurement of suicidality across studies, as well as a potential publication bias in suicide research. Moreover, suicide risks for SUDs are estimated in various study designs, in different countries with different age structures and different socioeconomic conditions. The studies reported adjusted risk ratios (often adjusted for age and gender) and unadjusted risk ratios, especially in studies that only calculated SMRs. Furthermore, relying on self-reported data on substance use may result in consumption levels being underestimated. Despite all these limitations, there is a high level of evidence of risk factors associated with suicide risk in SUDs. However, research on potential protective factors for suicide, such as social support, access to mental health services and harm reduction programs in SUDs is lacking. Furthermore, the impact of different diagnostic systems or changes in patterns of psychotropic substance use, in particular of multiple substance use, on suicide risk estimates is still unclear.
Conclusions
Early recognition and, most importantly, effective treatment of addiction could significantly reduce suicide rates worldwide. In addition to targeted interventions for suicidal behavior and SUDs, general suicide prevention strategies – such as restricting access to common means of suicide (e.g., firearms) – play a crucial role in reducing suicidal behavior.
Numerous research questions remain open for future investigation, including how suicide risk varies across age groups in relation to specific psychotropic substances used, gender identities and socioeconomic backgrounds. Additionally, there is a need to examine how established theoretical models of suicidality – such as:
– Joiner’s Interpersonal Theory of Suicide54;
– the Cry of Pain Model55;
– O’Connor’s Integrated Motivational–Volitional Model56;
– the Fluid Vulnerability Theory of Suicide57;
– and the Cubic Model of Suicide,58
relate to the link between suicidal behavior and substance use. To date, these models have not adequately addressed the impact of psychotropic substances on suicidality. This gap highlights the need for new theoretical considerations and integrations.
Although there is a broad array of literature for suicide prevention measures,40, 59, 60, 61, 62 previous preventive measures should be supplemented by innovative approaches. Artificial intelligence (AI) could play a role in this regard. It promises new ways to reduce the effects of SUDs, refine treatment standards and minimize the risk of relapse through tailored treatment plans.63 Machine learning models show promise in suicide prevention. However, challenges like data limitations, bias and interpretability issues need addressing. Integrating AI in clinical workflows, particularly in risk assessment and early intervention, continued research and ethical scrutiny are crucial to fully realize AI’s potential in suicide prevention.64, 65
Use of AI and AI-assisted technologies
Not applicable.