Abstract
Background. Psychosocial interventions encompass psychotherapy and psychological education that explicitly target psychosocial adaptation. These interventions have been shown to have a substantial positive effect on reducing anxiety and depression, as well as improving overall quality of life (QoL). Nevertheless, there is still no consensus concerning the therapeutic effectiveness of these interventions.
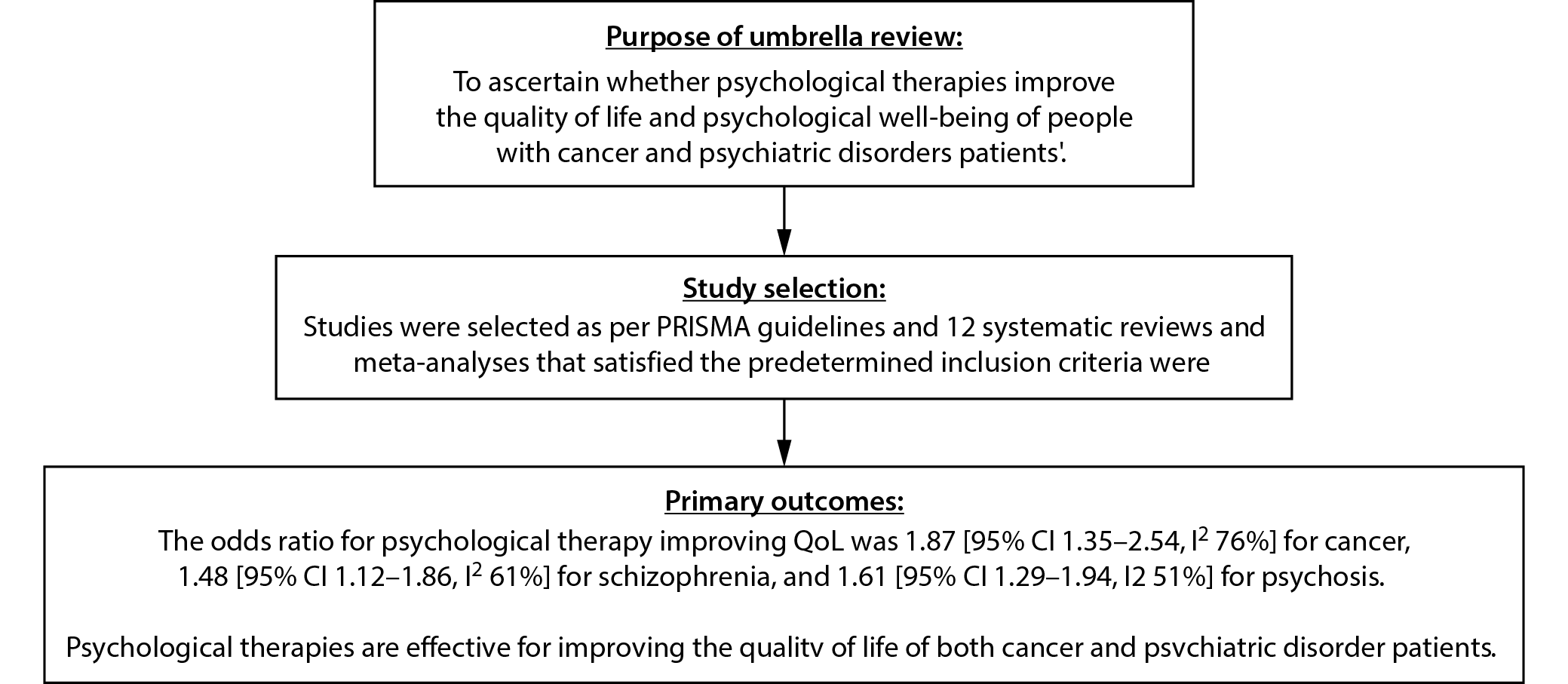
Objectives. An umbrella review of systematic reviews and meta-analyses was conducted to determine the efficacy of psychological interventions in improving the QoL and psychological wellbeing of patients with cancer and mental illness.
Materials and methods. A comprehensive literature search was conducted across multiple databases, namely PubMed, Embase, Scopus, and Cochrane Library. Assessing the Methodological Quality of Systematic Reviews 2 (AMSTAR-2) was used to evaluate research methodological rigor.
Results. The 12 papers analyzed in this umbrella review explored psychological therapy for cancer and psychiatric patients. The included reviews covered in total 8,198 studies. The AMSTAR-2 rated 8 of 12 studies as high-quality and 4 as intermediate. A total of 369 studies examined cancer, 166 schizophrenia and 165 psychoses. Psychological therapy improved the QoL for cancer, schizophrenia and psychosis by 1.87, 1.48 and 1.61, respectively. Psychiatric and cancer patients have anxiety, sleep issues and a lower QoL. This umbrella study showed that psychological interventions improved QoL in both groups of patients.
Conclusions. Psychological therapy appears to improve cancer and mental illness patients’ QoL and wellbeing. Most evidence is from high- and middle-income nations. Therefore, further high-quality research that covers a larger geographical area and rigorous systematic reviews with complete meta-analyses is needed to gain useful insights in this field.
Key words: mental health, cancer, quality of life, psychosis, psychological interventions
Introduction
The concept of quality of life (QoL) seeks to encompass the overall welfare of an individual or a population, taking into account both favorable and unfavorable aspects of their lives at a particular moment in time.1 Quality of life assessments must encompass a minimum of 5 discrete dimensions: physical health, mental health, participation in social and role activities on a daily basis, and overall perceptions of wellbeing.2, 3 The prevalence of cancer is increasing worldwide, and the individuals afflicted with cancer are susceptible to a multitude of psychological disorders, which significantly impair their overall QoL.4 A significant decline in the overall QoL was noted in both the physical and psychological aspects of cancer patients. They exhibit a diverse range of symptoms, and the insufficient control of symptoms can impede an individual’s ability to carry out their everyday tasks effectively. Increased symptom burden has been linked to elevated levels of mental distress and impaired physical and social functioning, as well as a reduced overall QoL. In addition to pain, sleep disturbances and fatigue, they endure substandard economic conditions.5, 6
Similarly, there has been an increase in the prevalence of mental health disorders, including anxiety, phobias, obsessive-compulsive disorder, and panic disorder, across the globe.7 Psychiatric disorder patients also experience a lowered QoL compared to the general population. This is due to the challenges posed by their mental illness, which hinders their ability to carry out daily activities, leading to a decreased level of independence. Primarily due to demographic shifts, the prevalence of mental health disorders has increased by 13%.8 Those suffering from severe mental illnesses tend to exhibit a reduction in their QoL compared to the general population. This is largely attributed to their impaired functional capacity, diminished autonomy, and the presence of low self-assurance and self-esteem.9
Psychological interventions include several approaches that positively impact the patient’s QoL by potentially alleviating the suffering arising from both the diagnosis and medical therapy.10 Psychosocial interventions include psychotherapy and psychological education aimed specifically at psychosocial adaptation. Psychosocial therapies, such as cognitive behavioral therapy (CBT) and acceptance and commitment therapy (ACT), are frequently provided by psychologists, social workers, mental health counselors, and community health professionals. These evidence-based therapies are delivered both individually and in groups.11, 12 Scientific evidence validated the efficacy of all of these treatments, demonstrating significant positive impacts in lowering anxiety and depression while also enhancing QoL. Furthermore, these benefits persisted in both short- and long-term follow-ups.13, 14 Despite the examination of this topic in several systematic reviews and meta-analyses,15, 16, 17, 18, 19 the most beneficial intervention for improving the QoL of cancer and mental illness patients remains unclear. Nonetheless, research on the efficacy of psychological therapies is characterized by a heterogeneity of strategies (e.g., individual or group therapy) and causes (e.g., improving personal skills or fostering emotional wellness).
Typically, individual studies and reviews have focused on a limited range of psychological outcomes. Collecting evidence on multiple outcomes is essential for assessing the effectiveness of an intervention on patient psychological wellbeing and for designing more effective treatments. Therefore, this study conducted an umbrella review of selected systematic reviews and meta-analyses20, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31 to determine the efficacy of psychological interventions in improving the QoL and psychological wellbeing of cancer and psychiatric patients.
Objectives
This study aimed to evaluate the effectiveness of various psychological interventions in enhancing the QoL and psychological wellbeing of cancer and psychiatric patients by conducting an umbrella review of selected systematic reviews and meta-analyses on the subject.
Materials and methods
An umbrella review was conducted in accordance with recently published guidelines.32 Regarding reporting, we followed the Preferred Reporting Items for Overviews of Reviews (PRIOR) protocol.33 Assessing the Methodological Quality of Systematic Reviews (AMSTAR) guidelines were applied to the evaluation of study quality.
Inclusion and exclusion criteria
For studies to be considered, they had to meet all of the subsequent criteria. The following criteria were used to evaluate the effectiveness of psychological interventions in improving the QoL of patients with cancer and mental illnesses: 1) systematic reviews that incorporated individual participant meta-analyses or meta-analyses of meta-analyses; 2) included individuals who had been diagnosed with any type of cancer or any mental illness; 3) reported efficiency of psychological interventions for improving the QoL of cancer and psychiatric patients: and 4) examined any of the outcomes listed below: a) change in QoL scores; b) improvement in psychological wellbeing; c) change in functioning capabilities; d) behavioral changes; and e) symptom reductions. Bibliographic references that were obsolete, anecdotal or solely relied on expert assessments were excluded from the assessment process. Furthermore, studies that were dependent on animal experiments or trials were excluded, along with those in which the authors lacked access to the primary data and critical information. Furthermore, non-research publications, qualitative studies, studies involving patients with human immunodeficiency virus (HIV) infection and other systemic diseases, and papers published in languages other than English were likewise omitted.
Literature search strategy
A literature search was performed using various databases, including PubMed, Embase, Scopus, Web of Science, and the Cochrane Library. The search covered the years 2000–2023 and utilized specific key words such as “psychological interventions”, “cancer”; “mental health”; “schizophrenia”; “psychosis”; “quality of life”; “QoL”; “positive psychology”; “wellbeing”; “positive psychiatry”; “depression”; “nursing”; “schizophrenia-spectrum disorders”; “cognitive behavioral therapy”; “psychoeducational therapy”; “supportive expressive therapy”; “anxiety”; “depression”; “mood”; “meta-analysis”; “systematic review and meta-analysis”; and “systematic review”. The key words were identified and verified for consistency in both the MEDLINE and Embase databases, in accordance with the PICOS framework.
Methodology for study selection
The aforementioned key words were entered into the Title (ti), Abstract (abs) and Keyword (key) fields in the Scopus search. Cochrane search terms included “psychological interventions” and “quality of life”. The PICO structure was applied to establish specific criteria for selection. “P” in this context represented patients diagnosed with either cancer or mental illnesses; “I” denoted the psychological intervention for improving the QoL, “C” represented a control, and “O” comprised the clinical outcomes, specifically the change in QoL scores and psychological wellbeing. The research design incorporated in this study was limited to the implementation of systematic reviews and meta-analyses. The inclusion criteria stipulated that only publications written in English would be considered. The identification of relevant studies was conducted through an unbiased and thorough examination of the related literature by 2 researchers: H.G. and Y.Y. Additional relevant papers were identified by carefully screening the references listed in the research selected for final analysis.
Screening and study selection
Following a preliminary screening of the titles and abstracts of the acquired articles, full texts of potentially eligible references were examined. Two evaluators conducted the screening process; in the event of any inconsistencies, the inclusion or exclusion of the material was resolved through deliberation.
Data extraction and critical appraisal of the included studies
Data extraction was conducted by one of the authors, and the information extracted was subsequently verified by 2 other authors. Any discrepancies were resolved by discussion. If an eligible publication had data on multiple disorders, we selectively collected information on QoL and psychological wellbeing outcomes that were relevant to our study. Initially, we gathered pertinent details from the eligible reviews, such as author information, publication year, journal of publication, study type, number of included studies, participants’ health conditions (cancer or mental illnesses), participants’ age, primary outcomes, statistical parameters analyzed, study conclusions, and methods of analysis and heterogeneity (if available). To encompass the full geographic range of evidence, we collected data regarding the specific locations of the individual studies that were included in the relevant reviews. This involved gathering information about the countries where the research was carried out. Regarding methodological rigor, we collected data on whether the authors utilized a pre-validated tool or an additional set of extracted questions to evaluate the methodological rigor of the studies included in each systematic review. If the answer was affirmative, we have documented the specific tool employed and the primary findings of the evaluation were classified into 3 broad groups: studies exhibiting weak methodological rigor, studies demonstrating a high level of methodological rigor, and studies displaying intermediate or mixed patterns from the 2 groups. The methodological rigor of the included systematic reviews was evaluated by 2 authors using the AMSTAR-2 program. Any differences were resolved with the assistance of a 3rd author. AMSTAR-2 utilizes a checklist consisting of 16 items or domains, of which 7 are deemed crucial for ensuring the overall validity of a review. The essential domains to be taken into account are as follows: 1) ensuring protocol registration prior to commencing the review; 2) conducting a thorough and comprehensive literature search; 3) providing a rationale for excluding specific studies; 4) assessing the risk of bias in the included studies; 5) employing suitable statistical techniques for conducting a meta-analysis; 6) considering the influence of bias when interpreting the findings; and 7) evaluating the existence and consequences of publication bias. Finally, utilizing abstracts and full-text analyses, we retrieved pertinent information regarding the primary conclusions drawn from each of the reviews included. Furthermore, if the review involved multiple disease areas, we only selected the primary outcomes from the individual studies concerning how the psychological interventions improved QoL.
Statistical analysis of primary outcomes of the included studies
Due to high heterogeneity in the designs, study questions, outcomes, and metrics, a descriptive analysis was performed. Separate tables were created for the characteristic information, methodological assessment, and summary estimates, 95% confidence intervals (95% CIs) and heterogeneity estimates of each systematic review and meta-analysis. All of the included systematic reviews and meta-analyses suggested that psychological interventions were efficient in improving QoL. However, because the strategies used were so different, the overall odds ratios (ORs) of the studies included were also calculated to evaluate how strongly the psychological intervention was linked to QoL. The participant’s health conditions served as the basis for grouping the studies. An OR value higher than 1 was considered statistically significant and shows that psychological intervention is highly effective in improving the QoL of people with mental illnesses and cancer.
Results
Study selection
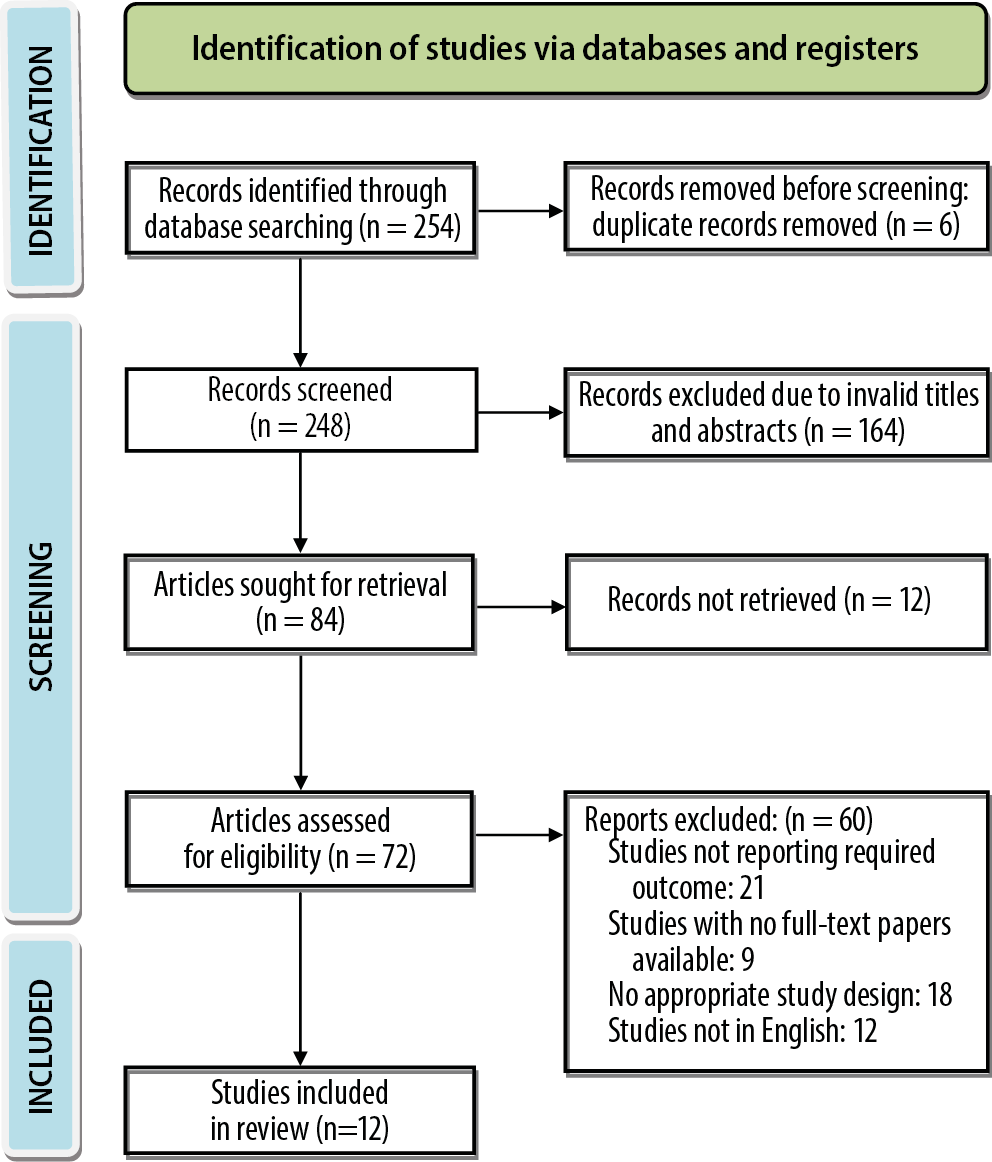
The process of selecting studies, in accordance with the Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) guidelines,34 is presented in Figure 1. An electronic scanning technique was employed to perform an exhaustive search across multiple databases, leading to the identification of 254 studies that satisfied the inclusion criteria specified in the PICOS framework.35 Prior to screening, 6 duplicate documents were eliminated, bringing the total number of papers screened to 248. A total of 164 papers were subsequently excluded for having invalid titles and abstracts, and 84 records were requested for retrieval. Twelve records were not retrieved in their entirety; the eligibility of the remaining 72 reports was evaluated. Upon implementation of the inclusion-exclusion criteria, 60 studies were determined to be ineligible and were subsequently excluded. The principal determinants that led to the exclusion of research studies were their failure to provide essential outcome measures, non-access to complete text papers, unsuitable study designs, and unavailability in the English language. In conclusion, 12 systematic reviews and meta-analyses that satisfied the predetermined inclusion criteria and spanned a time period from 2000 to 2023 were incorporated into this umbrella review.
Characteristics of included reviews
The included reviews were published between 2013 and 2023. Included articles were obtained from Scopus (n = 53), PubMed (n = 114), Embase (n = 29), and the Cochrane Library (n = 48). Out of the 12 included reviews, 6 reported the efficacy of psychological interventions for improving the QoL of cancer patients. On the other hand, 6 evaluations analyzed the effectiveness of psychological therapies in improving the QoL of patients with mental diseases. Four of these reviews focused on breast cancer patients.20, 21, 22, 23 The article by De La Torre-Luque et al.24 described an improvement in QoL among patients with multiple cancers, whereas the article by Son et al.25 described an improvement in QoL among patients with colorectal cancer. Three articles, Jagan et al.,27 Pina et al.28 and Valiente et al.,30 provided findings regarding QoL improvements in schizophrenia patients. Turner et al.29 and Wood et al.31 provided findings regarding QoL improvement in patients with psychosis. The article by McGlanaghy et al.26 describes the efficiency of psychological interventions in improving the QoL of both psychosis and schizophrenia patients. All included reviews were considered articles without any geographical restriction. The included evaluations comprised a variety of study counts, spanning from 8 to 198. Each of the 12 included reviews incorporated data pooling and meta-analyses in addition to qualitative analyses. Table 1 provides an overview of the characteristics of the reviews.
Methodological quality
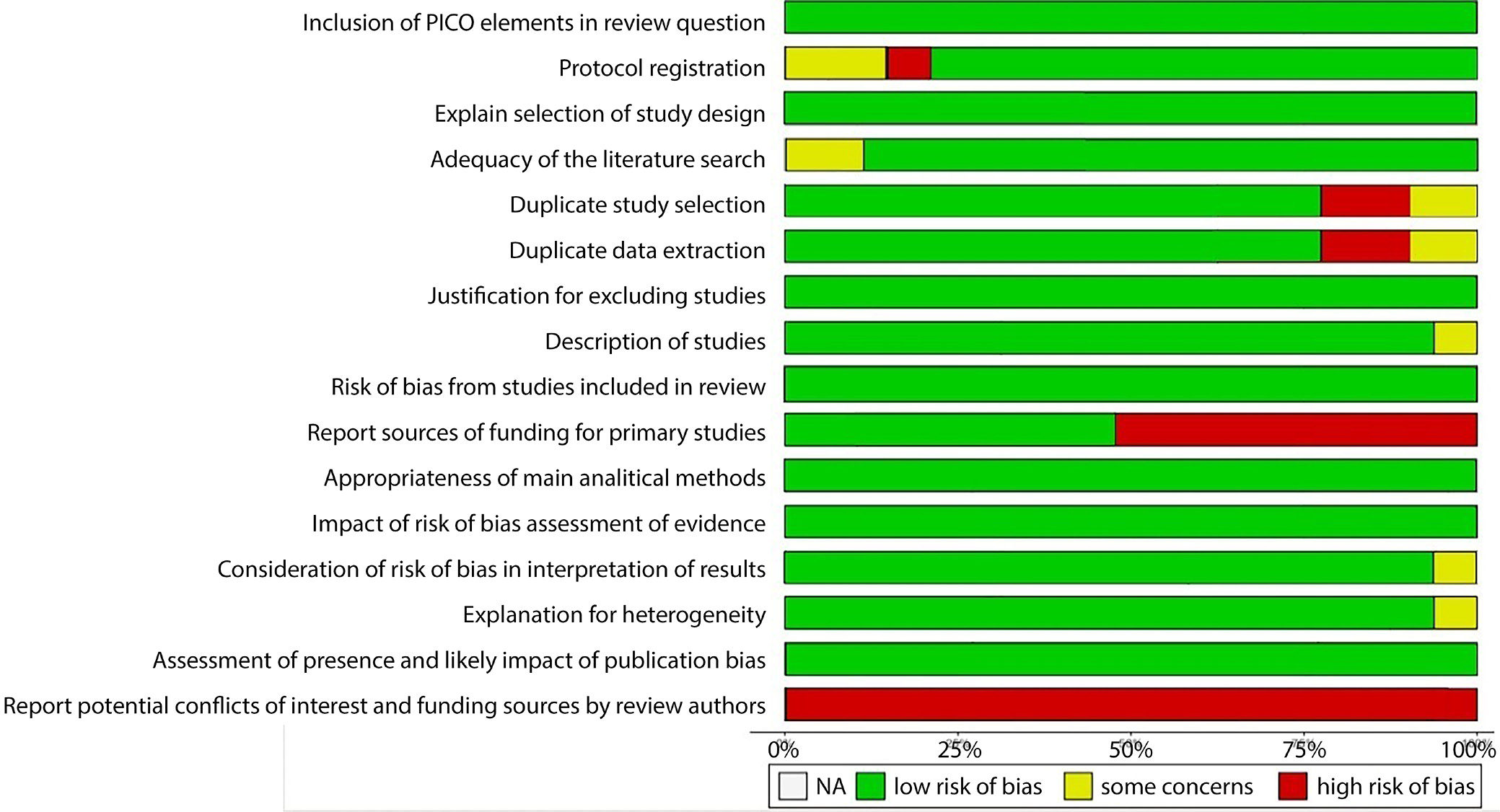
The frequency of each AMSTAR-2 rating for each domain across evaluations is summarized in Figure 2. In addition, the domain-specific methodological quality evaluations for each review are provided in Table 2. Twelve of the included studies20, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31 addressed the review questions using the PICO elements, provided an explanation of their study design selection, compiled a list of excluded studies, evaluated their conclusions, employed appropriate statistical methods, assessed the potential impact of bias risk in individual studies, and conducted quantitative synthesis. Eight reviews (Faller et al.,20 Li et al.,23 De La Torre-Luque et al.,24 Son et al.,25 McGlanaghy et al.,26 Jagan et al.,27 Pina et al.,28 Valiente et al.,30 and Wood et al.31) stated that the review methods were established prior to use and provided justification for substantial deviations from the protocol. While articles by Guarino et al.21 and Hwang et al.22 partially met this criterion, article by Turner et al.29 failed to do so. With the exception of article Li et al.,23 which could benefit from a more exhaustive search strategy, every article employed a comprehensive literature search. With the exception of the papers by Hwang et al.22 and Son et al.,25 all the other studies used double study selection; however, the methodology in the study by Turner et al.29 was ambiguous, so it received a partial yes. Likewise, apart from the studies by Faller et al.20 and Wood et al.,31 all remaining studies extracted data in duplicate; however, study by Son et al.25 was assessed as a partial affirmation. With the exception of the study by Valiente et al.,30 all remaining studies provide sufficient descriptions of the included studies. Except the studies by Faller et al.,20 Li et al.,23 De La Torre-Luque et al.,24 Pina et al.,28 and Turner et al.,29 all remaining studies disclosed the funding sources for the aforementioned studies. Excluding the study by Son et al.25, all other studies adequately investigated publication bias, and with the exception of study by Wood et al.,31 all other studies accounted for the risk of bias in the individual studies when interpreting or discussing the results. Furthermore, all 12 included studies did not disclose any potential sources in conflicts of interest. Based on the aforementioned evaluations, 8 of the 12 studies21, 22, 23, 24, 26, 27, 28, 30 received a high overall assessment, whereas the remaining 420, 25, 29, 31 were deemed to be of moderate quality.
Extraction results
The extracted populations of the ncluded randomized clinical trials (RCTs) were from different countries, with the majority of studies conducted in high-income or middle-income countries, including Germany, Italy, Spain, South Korea, the UK, Malaysia, Brazil, the Netherlands, Spain, and Ireland. The health conditions of the participants included in the studies were as follows: breast cancer for studies by Faller et al., Guarino et al., Hwang et al., and Li et al.,20, 21, 22, 23, colorectal cancer for the study by Son et al.,25, and lung, breast or prostate cancer for the paper by De La Torre-Luque et al.24 Patients with schizophrenia were the subject of research in articles by Jagan et al., Pina et al. and Valiente et al.,27, 28, 30 whereas patients with psychosis were the focus of studies by Turner et al. and Wood et al.29, 31 Patients with schizophrenia and psychosis were both covered in the paper by Mc Glanaghy et al.26 The effectiveness of psychological interventions in enhancing QoL was demonstrated across all the included studies through the assessment of the QL-index and QLQ-C30 (which were evaluated in studies by Faller et al.,20 Hwang et al.,22 Li et al.,23 De La Torre-Luque et al.,24 Son et al.,25 Valiente et al.,30 and Wood et al.31), World Health Organization-5 Well-Being Index (WHO-5; Guarino et al.23), Agitated Behavior Scale (ABS), Brief Symptom Inventory (BSI), Profile of Mood States (POMS), European Organization for the Research and Treatment of Cancer Quality of Life Questionnaire (EORTC QLQ-C30), Mental Component Summary (MCS-12), Cancer Rehabilitation Evaluation System-Short Form (CARES-SF), Short Form 36 Health Survey (SF-36), Functional Assessment of Cancer Therapy (FACT), Functional Living Index-Cancer (FLIC) (Guarino et al.23), Quality of Life (QoL) Scale (QLS) (Li et al.26), Positive and Negative Syndrome Scale (PANSS; Li et al.,23 Glanaghav et al.26 and Turner et al.29), Brief Psychiatric Rating Scale (BPRS; Glanaghav et al.,26 Turner et al.29 and Wood et al.31), patient and public involvement (PPI), positive psychotherapy (PPT) (Jagan et al.27 and Pina et al.28), and Psychological Wellbeing Scale (PWB; Jagan et al.,27 Pina et al.28 and Wood et al.31). Table 3 displays the summary estimates of these factors for the included reviews, searched using the specific key words shown in Table 4.
Faller et al.20 retrieved 198 studies reporting 218 treatment-control comparisons, encompassing 22,238 patients. The researchers found notable short- to medium-term effects of individual and group psychotherapy, as well as psychoeducation, that persisted in both the medium-term (≤6 months) and long-term (>6 months). It was noted that relaxation training exhibited noticeable short-term effects, whereas studies that preselected participants based on heightened distress observed substantial post-treatment effects. Guarino et al.21 utilized 45 studies with high methodological heterogeneity that satisfied all inclusion criteria. The researchers documented a moderate effect size for CBT and psychoeducational interventions as a whole. Notwithstanding certain constraints, these findings provide partial confirmation of the efficacy of psychoeducational and CBT in enhancing the wellbeing of women diagnosed with breast cancer. Eight investigations with 33 datasets were utilized in the meta-analysis by Hwang et al.22 Cognitive interventions, meditation and psychological education programs were anticipated to aid in the reduction of negative emotions and improvements in the QoL of breast cancer patients, according to an assessment using the Jadad scale.
In their meta-analysis, Li et al.23 incorporated a total of 12 articles for evaluation, employing the EORTC OLQ-C30. Significant statistical differences between the intervention and control groups (mean difference (MD) = 12.74, 95% CI: 6.34–19.14, p < 0.001) suggested that psychological nursing interventions can substantially enhance the QoL for patients diagnosed with breast cancer, despite the high heterogeneity among the studies (I2 = 92%). De La Torre-Luque et al.24 conducted a meta-analysis including 78 investigations. A moderate level of methodological quality was demonstrated by the majority of the studies (60.2% of the sample), as opposed to strong and weak levels (24%). This finding provides support for the notion that offering psychological treatments should be essential for the health of cancer patients. Son et al.26 conducted a meta-analysis comprising 8 studies, none of which yielded a statistically significant impact on QoL. However, the overall result of their analysis provided evidence for the positive effect of face-to-face psychosocial interventions on the QoL of colorectal cancer patients during the post-intervention period.
Ninety RCTs involving 8,440 randomized participants divided into 24 psychological intervention and control groups were utilized by McGlanaghy et al.26 They compared direct and indirect evidence for the effectiveness of each psychological intervention using network meta-analysis and a frequentist approach. They concluded that psychological interventions were more probable than control groups to reduce total symptoms, with 1 intervention, mindfulness-based psychoeducation, consistently ranked as the most likely to completely reduce symptoms. In their meta-analysis, Jagan et al.27 utilized extractable data from 18 studies. The results indicated a significant overall effect (Z = 3.00; p = 0.003; 95% CI: 0.69 (1.15–0.24); n = 1,633). However, there was substantial heterogeneity in the findings (Tau2 = 0.89; χ2 = 303.62, degrees of freedom (df) = 17; p < 0.001; I2 = 94%). The authors concluded that the majority of psychological interventions effectively reduced the levels of internalized stigma.
In their meta-analysis, Pina et al.28 utilized 9 studies and identified a significant effect (p = 0.042) for wellbeing enhancement (Z = 2.01). They documented psychological intrusions as a potentially beneficial resource for patients on the schizophrenia spectrum, with symptom reduction and improved wellbeing as potential outcomes. Turner et al.29 compared psychological interventions for psychosis with 3,295 participants across 48 outcome trials. It was noted that CBT exhibited a considerably higher efficacy in reducing positive symptoms (g = 0.16) compared to other interventions combined. Likewise, the effectiveness of social skills training in mitigating negative symptoms was found to be significantly higher (g = 0.27).
In their analysis, Valiente et al.30 incorporated a total of 36 articles and assessed the impact of psychological interventions on the QoL experienced by individuals with schizophrenia. The results of their study indicated a modest but noteworthy impact of the intervention on wellbeing outcomes, as well as a substantial moderating effect when wellbeing was the principal objective. Psychological interventions specifically aimed at enhancing wellbeing are suggested as a supplementary approach to the treatment and promotion of mental health. Seventeen trials employing interventions including cognitive behavioral intervention on positive symptoms (CBTp), ACT and metacognitive therapy (MCT) were analyzed by Wood et al.31 through 22 studies. It was determined that psychological interventions informed by cognitive behavioral principles yielded substantial positive outcomes. Specifically, cognitive behavioral interventions exhibited a noteworthy positive impact on negative symptoms following therapy, total symptoms during both therapy and follow-up, functioning during therapy and follow-up, and readmission during follow-up. It was proposed that psychological interventions may prove efficacious for individuals who are admitted to psychiatric inpatient care or experiencing an acute crisis.
Statistical analyses
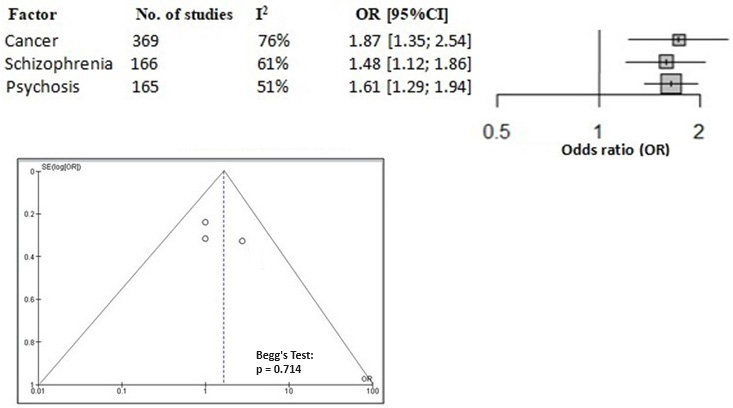
Using the results extracted on changes in QoL scores, the overall OR of the included studies was calculated to assess how strongly psychological interventions were associated with QoL. The studies were grouped based on the health conditions of the participants. A total of 369 studies were found concerning cancer, 166 to schizophrenia and 165 to psychosis. Figure 3 displays the OR forest plot. The OR for the likelihood of psychological therapies to increase QoL was 1.87 (95% CI: 1.35–2.54, I2 = 76%) for cancer, 1.48 (95% CI 1.12–1.86, I2 = 61%) for schizophrenia and 1.61 (95% CI: 1.29–1.94, I2 = 51%) for psychosis. Since all OR values were greater than 1, there is a strong correlation between the 2 parameters and a better chance that psychological intervention will improve the QoL of people with mental illnesses and cancer. Furthermore, the symmetrical funnel plot in Figure 3 and the statistically insignificant Begg’s test (p = 0.714), which is higher than the predetermined significance threshold of 0.05, demonstrates a lack of publication bias. This shows that psychological interventions are very successful in improving the QoL in cancer and psychiatric patients.
Discussion
As the medical paradigm has been revised, there has been a growing acknowledgment that disease management must encompass psychological therapy in addition to physiological interventions.36 Additionally, QoL should consider both mental and physical health. Psychological interventions primarily pertain to the utilization of psychological activities involving patients to facilitate their recovery from illness and promote positive physiological and biochemical changes.37, 38 Treatment procedures are often accompanied by persistent anxiety, depression, dread, and other adverse affective states among cancer and psychiatric patients.37, 38 These emotions not only have a detrimental effect on the patient’s personal wellbeing but also an emotional and happiness-reducing effect on their families.39, 40 Patients would be able to accurately and thoroughly comprehend the disease if the nursing staff could comprehend the psychological activities of postoperative patients and promptly implement individualized psychological treatments in accordance with the patient’s psychological capacities and differences. By doing so, individuals can confront the disease, relax their emotions and accept the physical changes that occur during and after treatment. As a result, their treatment adherence will be enhanced.41, 42, 43 Positive psychological nursing interventions can alleviate physical symptoms, stimulate the immune system, impede the progression of cancer, and enhance the patient’s prognoses while aiding in the diagnosis and treatment of mental illness and cancer, as well as improving a patient’s treatment compliance.44, 45
A multitude of investigations assessed the QoL in cancer patients who underwent long-term psychological interventions in nursing, including cognitive and pain management, health education and psychological counseling. Significant improvement in QoL was more prevalent in the study groups than in the control groups, according to these findings (p < 0.05).46, 47, 48 Several studies, however, have concluded that psychological nursing interventions do not significantly impact a cancer patient’s QoL.49, 50 Numerous studies have examined the QoL and mental health of cancer patients through the use of psychological nursing interventions in recent years.51, 52, 53, 54, 55 The incidence of cancer is significantly higher, and research indicates that patients exhibit disrupted emotional functioning as a result of lower survival rates compared to other types of cancer. Both direct and indirect psychological therapies are essential to enhance the result of cancer treatment. The combination of cognitive interventions with progressive muscle relaxation techniques has been found to be highly efficient in enhancing the QoL of patients, while also being cost-effective. Early psychological assistance during the cancer treatment process and before surgery shows the potential to enhance psychological wellbeing and results.56, 57, 58 However, a consensus regarding the therapeutic efficacy of these interventions has yet to be reached. Therefore, the primary objective of this umbrella review was to evaluate the clinical effectiveness of various psychological interventions, namely CBT, psychoeducational interventions and supportive-expressive therapy, in relation to distinct psychological outcomes encompassing mood, anxiety, depression, and QoL among patients diagnosed with cancer and mental illnesses.
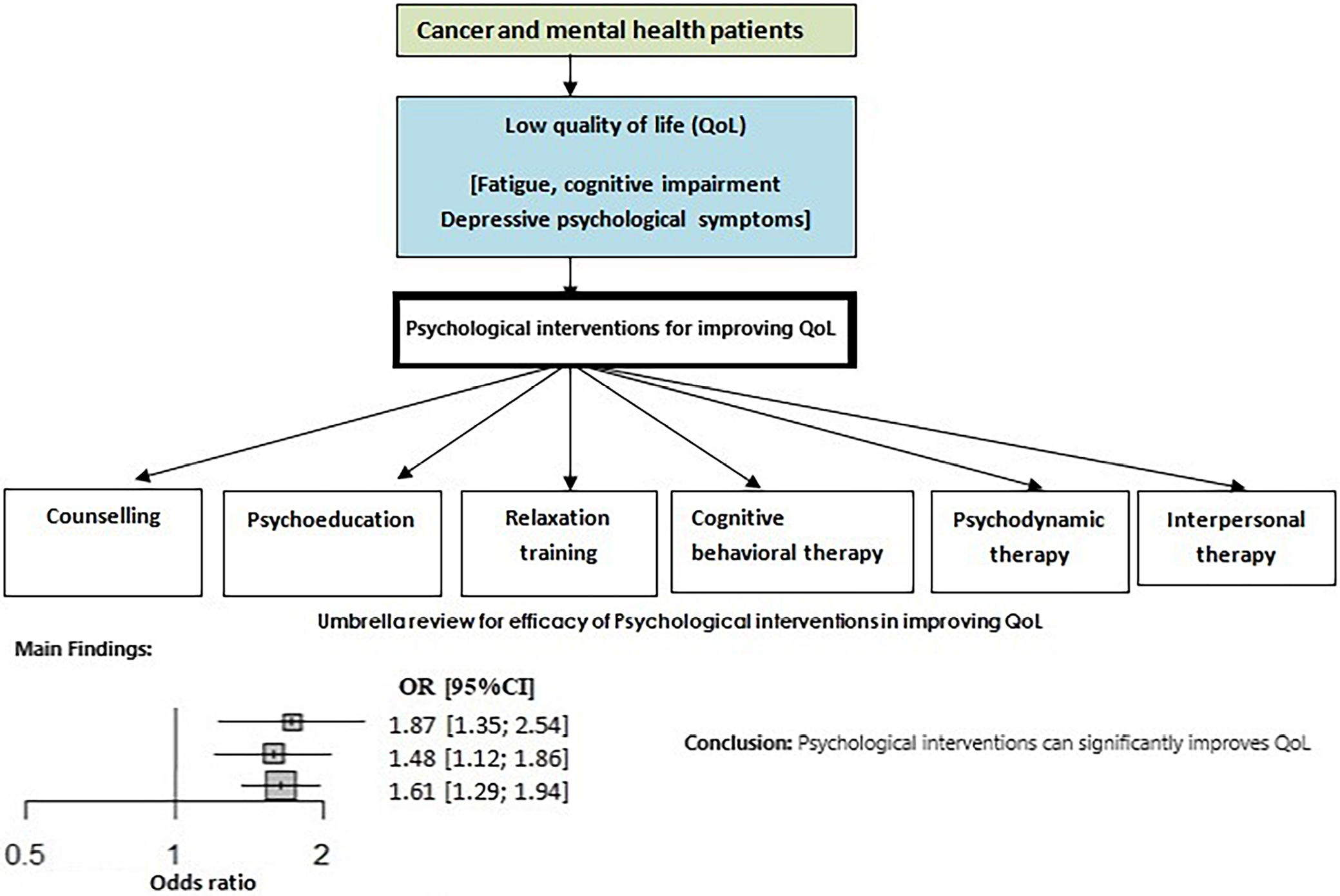
The present umbrella review demonstrates that psychological therapies have a broad and substantial impact on the QoL and physiological wellbeing of patients with cancer and mental diseases (Figure 4). A noticeable enhancement was noticed in their QoL score, psychological wellbeing, functional capacity, and behavior, coupled with a considerable reduction in symptoms. Figure 5 displays a flowchart elucidating the purpose, synthesis and main outcomes of this umbrella review.
However, the preponderance of information is derived from affluent and moderate-income nations, as well as low-quality research. Hence, it is crucial to undertake well-executed investigations that encompass a broader geographic scope and carry out meticulous systematic reviews with rigorous meta-analyses to get vital insights into this domain.
Limitations
There are certain limitations to this study. First, although we followed recent recommendations regarding the optimal databases to search for umbrella reviews while conducting the search, it is still possible that we overlooked additional pertinent systematic reviews. This umbrella review consists mainly of systematic reviews that utilized studies with a moderate-to-high risk of bias. Furthermore, the conclusions drawn from these reviews were primarily based on retrospective observational, cross-sectional and case-series research designs, which are prone to residual confounding and are insufficient for establishing temporal associations. Risk of bias assessments revealed substantial variation in the quality of the studies, with notable disparities in the quality observed among particular interventions. Selection biases can also affect likelihood estimates. Furthermore, it is imperative to recognize the possible presence of selection bias in our study, as a considerable number of papers were omitted. Lastly, the majority of the results were gathered in high-income nations, which consequently restricts their applicability to countries with lower and middle income. Therefore, this emphasizes the need for additional research to gain a more comprehensive understanding of the effectiveness of psychological interventions in enhancing QoL and their long-term effects.
Conclusions
Compelling data indicates that psychological therapies have a wide range and significant effect on the QoL and physiological wellbeing of individuals with cancer and mental illnesses. A significant improvement was observed in their QoL scores, psychological wellbeing, functional capacity, and conduct, accompanied by a significant decrease in symptoms. Nevertheless, the majority of evidence comes from high- and middle-income countries and low-quality studies. Therefore, it is important to conduct future high-quality studies that cover a larger geographical area and perform rigorous systematic reviews with careful meta-analyses to gain valuable insights into this field.
Supplementary data
The Supplementary materials are available at https://doi.org/10.5281/zenodo.12792916. The package includes the following files:
Supplementary Table 1. Quality of Life Questionnaire.