Abstract
Background. Chronic obstructive pulmonary disease (COPD) contributes considerably to morbidity and mortality worldwide, necessitating innovative interventions to enhance patient outcomes.
Objectives. The present synthesis aimed to discern the impact of nursing interventions on physical, mental and social health outcomes among COPD patients, focusing on 6-minute walk distance (6MWD), self-efficacy, anxiety, depression, dyspnea, hospitalization, St. George’s Respiratory Questionnaire score, patient satisfaction, and all-cause mortality.
Materials and methods. This review was conducted to include randomized controlled trials exploring nursing interventions for COPD patients without demographic restriction and sourced from several databases (MEDLINE, Cochrane Central Register of Controlled Trials (CENTRAL), Scopus, CINAHL (Cumulative Index to Nursing and Allied Health Literature), and OpenGrey) until September 2023. Quality assessments were done using the Cochrane Risk of Bias 2 (RoB 2) tool, followed by meta-analysis using a random-effects model with continuous outcomes interpreted as standardized mean difference (SMD) and categorical outcomes as risk ratio (RR).
Results. Thirty-six studies were incorporated, revealing nursing interventions to notably enhance 6MWD (SMD: 0.628, p = 0.001) and self-efficacy (SMD: 0.800, p < 0.001), and significantly decrease anxiety (SMD: –0.952, p = 0.015) and depression levels (SMD: –0.952, p = 0.006). However, the effects of hospitalization, quality of life (QoL) and dyspnea did not reach statistical significance. Notably, high heterogeneity was observed in several outcomes.
Conclusions. Nursing interventions yielded significant improvements for 6MWD, self-efficacy, anxiety, and depression among COPD patients. However, their impact on hospitalization and QoL remains indeterminate, necessitating further nuanced research to optimize and tailor nursing care strategies for this demographic. Enhanced intervention standardization and larger, multicenter trials are warranted to confirm and expand these findings.
Key words: quality of life, nursing, meta-analysis, chronic obstructive pulmonary disease
Background
Chronic obstructive pulmonary disease (COPD) represents one of the most prevalent and impactful respiratory diseases globally. The World Health Organization (WHO) lists it as the 3rd leading cause of death, causing approx. 3.3 million deaths worldwide.1 The global burden of COPD continues to increase, particularly in low- and middle-income countries, with a significant economic impact on healthcare systems.2
Defined by persistent respiratory symptoms and airflow limitation due to airway and/or alveolar abnormalities, COPD is typically caused by significant exposure to noxious particles or gases.3 Tobacco smoke, occupational dust and chemicals, along with indoor and outdoor air pollution, have been identified as primary risk factors for the development of COPD.4
Clinical management of COPD poses numerous challenges. Patients with COPD often face recurrent exacerbations, which not only compromise their quality of life (QoL) but also lead to hospital admissions, contributing to the disease’s economic burden. Furthermore, the comorbidities associated with COPD, such as cardiovascular diseases, osteoporosis and anxiety or depression, compound the complexity of its management.5
Nursing care, as an integral component of COPD management, has evolved over the years. The shift towards a patient-centered care approach has highlighted the pivotal role of nursing interventions in improving the QoL of COPD patients, reducing hospitalizations and managing symptoms.6 These interventions encompass a broad spectrum, from health education and exercise training to behavioral therapy and self-management programs.
Health education is one of the cornerstones of nursing care interventions. Patients with COPD, when adequately educated about their disease, its progression and potential triggers, are more likely to adhere to treatment regimens and actively participate in their care. Such education also enables early recognition of exacerbations, thereby preventing hospital admissions.7
Exercise training, especially pulmonary rehabilitation, has proven to be highly beneficial for COPD patients. These programs, often managed by nurses, focus on strengthening respiratory muscles, improving exercise tolerance and enhancing overall wellbeing. Studies have consistently shown that patients undergoing pulmonary rehabilitation experience fewer hospital admissions, improved QoL and better exercise capacity.8, 9
Behavioral therapies, including cognitive-behavioral therapy, are also being integrated into nursing care interventions for COPD patients. Such therapies, aiming at addressing the psychological comorbidities of COPD, have demonstrated improved mental health outcomes and reduced hospital admissions.10
Self-management programs that empower patients to take an active role in their care have gained significant traction in recent years. These programs, often facilitated by nurses, provide COPD patients with tools and strategies to manage their symptoms, monitor medication and promptly respond to exacerbations.11 The importance of nurse-led management programs for COPD patients cannot be overstated. Nurses, with their detailed knowledge and regular patient interactions, are ideally positioned to lead these programs. They can provide continuous, comprehensive education on the disease process, inhaler techniques and lifestyle modifications. Moreover, nurse-led programs facilitate improved communication between patients and healthcare providers, enabling timely interventions and adjustments to treatment plans.
Given the diverse array of nursing interventions available for COPD management, it becomes imperative to ascertain their efficacy through rigorous research. While individual randomized controlled trials (RCTs) have provided insights into specific interventions, a comprehensive synthesis through a systematic review and meta-analysis can provide a clearer picture of the overall effectiveness of nursing care interventions in managing COPD.
The importance of synthesizing existing evidence lies in the fact that COPD, given its chronic nature, requires long-term, holistic care. While pharmacological interventions play an essential role, non-pharmacological strategies, especially those delivered by nursing professionals, can significantly impact patient outcomes, QoL and self-efficacy. With the increasing healthcare costs and the rising global burden of COPD, there is a pressing need to identify cost-effective and efficient strategies that can be integrated into daily clinical practice.
Objectives
This systematic review and meta-analysis aims to synthesize the evidence from RCTs on the effectiveness of various nursing care interventions in COPD management, providing clinicians, policymakers and researchers with valuable insights and directions for future research.
Methods
In alignment with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 guidelines,12 we systematically constructed and executed this meta-analysis to assess the effect of nursing interventions for COPD patients.
This review included studies involving patients diagnosed with chronic obstructive pulmonary disease (COPD), regardless of age, gender, ethnicity, or geographical location. Eligible interventions focused on nursing or nurse-led approaches provided in hospital or primary care settings, compared to conventional care or non-nurse-led interventions. The outcomes assessed encompassed physical parameters such as all-cause mortality, 6-minute walk distance (6MWD), dyspnea, and hospitalization rates. Mental health-related outcomes, including depression and anxiety, were also considered, alongside measures of QoL assessed through the St. George’s Respiratory Questionnaire (SGRQ), self-efficacy scores, and patient satisfaction.
Study design
Randomized clinical trials written in English from the inception of the database until September 2023 were included. Randomized clinical trials remain the gold standard for evaluating the efficacy of therapeutic interventions. By synthesizing data from various RCTs on nursing care interventions for COPD, we can draw more robust conclusions, validate findings and potentially identify areas for future research. It is especially crucial given the heterogeneity in nursing interventions, patient populations, healthcare settings, and outcomes measured across different studies.
Both peer-reviewed articles and grey literature were sought to circumvent publication bias.
Information sources and search strategy
A comprehensive search was initiated on databases such as MEDLINE, Cochrane Central Register of Controlled Trials (CENTRAL), Scopus, CINAHL (Cumulative Index to Nursing and Allied Health Literature), and OpenGrey. Reference lists of relevant articles and reviews were manually scrutinized. Correspondence with authors was established as required to obtain additional information or clarity. Search terms combined “nursing,” “chronic obstructive pulmonary disease” and each of the outcomes listed along with appropriate Boolean operators like “AND,” “OR” and “NOT.” Language (only publications in English) and time restrictions (up to September 2023) were applied. The full search strategy can be found in the Supplementary Appendix.
Selection process
Rayyan was utilized to manage and categorize identified studies. After discarding duplicates, the remaining articles were critically evaluated for inclusion. Two authors (Y.D. and L.Z.) independently assessed titles and abstracts of captured articles. They subsequently reviewed the full text of potential inclusions. Consensus was reached either via discussion or, if necessary, by involving a 3rd author (Y.W.).
Data collection process and data items
A standardized manual form was used by the same researchers (Y.D. and L.Z.) for independent data extraction. The information retrieved encompassed study attributes like author information; journal; study title; year of publication; participant demographics like age, gender distribution, and comorbidities; intervention details in terms of nursing type, frequency, duration, intensity, and follow-up; and all of the outcome measures mentioned above.
Study risk of bias assessment
The Cochrane Risk of Bias 2 (RoB 2) tool was employed to evaluate the risk of bias in included RCTs.13 Differences in assessments between authors (X.X. and B.W.) were resolved through dialogue or consultation with a 3rd authors (Y.W.).
This tool assesses the bias in 5 key domains. The 1st domain evaluates the bias arising from the randomization process. It considers the random sequence generation and allocation concealment mechanisms to determine if they introduce any systematic differences between intervention and comparison groups. The 2nd domain examines bias due to deviations from the intended interventions, which might result from blinding inadequacies or other reasons. The analysis is conducted for both participants and study personnel to understand if the outcome measurement is affected by knowledge of the received intervention. The 3rd domain addresses bias arising from incomplete outcome data. Studies are scrutinized for dropout rates, reasons for missing data, and whether appropriate methods were used to handle such missing data. The 4th domain focuses on bias introduced during outcome measurement. It checks for blinding of outcome assessors and determines if the outcomes were measured in the same way across intervention groups. Bias in the final domain arises when the reported outcome is selected from multiple outcome measurements or analysis methods. It checks for pre-specification and reporting consistency to ensure that selective reporting does not affect the results.
Each domain is rated as “low risk,” “some concerns” or “high risk” of bias. The overall risk for each study is then categorized based on the domain with the highest risk. For instance, if 1 domain is rated as “high risk,” the overall risk for the study is also deemed “high.”
Effect measures and synthesis methods
The collected data were systematically synthesized to draw consolidated findings. Meta-analysis was performed, and pooled effect sizes were computed using a random-effects model, given the expected variability in populations, interventions and outcome measurement.14 The primary measure of treatment effect for continuous outcomes was the mean difference (MD) or standardized mean difference (SMD) when different scales were used. For dichotomous outcomes, risk ratios (RR) with 95% confidence intervals (95% CIs) were computed. Each outcome was presented in individual forest plots, showing the effect size and CIs of individual studies and the pooled effect size. All the analyses were conducted utilizing STATA v. 14.2 (StataCorp LLC, College Station, USA).
The I2 statistic was employed to quantify the extent of variability in effect sizes that could not be explained by sampling error alone. An I2 value above 50% indicated substantial heterogeneity.14 To assess the robustness of our findings, sensitivity analyses were performed. This involved excluding studies with a high risk of bias, conducting analyses with different statistical models or removing studies with outlier results.
The symmetry of funnel plots was visually assessed to detect potential biases, with specific consideration for the distortions associated with using SMD as the effect size measure. To mitigate these distortions and ensure a more accurate assessment of publication bias and small-study effects, we employed an alternative precision estimate of 1/√n (i.e., n is the total sample size) in our funnel plot analyses. This adjustment, based on sample size, was chosen in response to documented concerns over SMD-related funnel plot asymmetry, providing a more reliable foundation for our statistical appraisal. Consequently, Egger’s regression test was applied using this revised precision estimate, offering a more statistically robust evaluation of funnel plot symmetry and the potential presence of publication bias.
Results
Search results and study selection
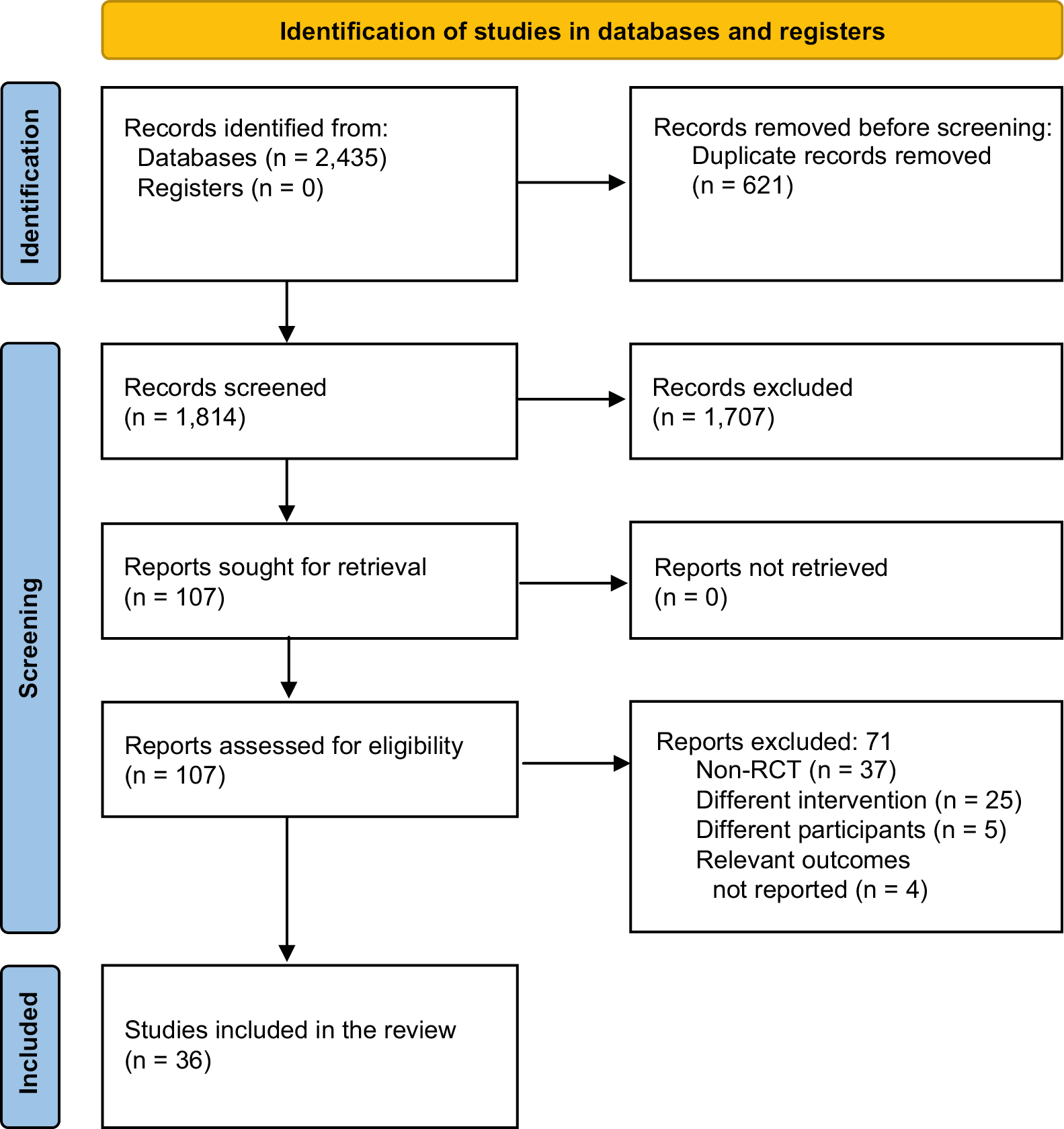
From an initial identification of 2,435 records in databases, 621 duplicates were removed. Of the 1,814 records screened, 1,707 were excluded, leading to 107 full-text articles assessed for eligibility. Finally, 34 studies met the inclusion criteria (Figure 1).15, 16, 17, 18, 19, 20, 21, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31, 32, 33, 34, 35, 36, 37, 38, 39, 40, 41, 42, 43, 44, 45, 46, 47, 48
Characteristics of the included studies
The included 34 studies investigating nurse-led interventions for patients with COPD originated from varied global locales, including the USA, Turkey, China, and the UK, between 2003 and 2022. Notably, the sample size within the intervention arm across studies fluctuates between 8 and 217 participants. While most studies focused on patients aged 40 years and above, interventions primarily revolved around telephonic support, home visits and various nurse-led programs, contrasting with control groups typically receiving usual or standard care. Risk of bias assessment showed varied integrity with 13 studies labeled “high risk,” 17 entailing “some concerns” and merely 6 assessed as “low risk.” The intervention duration predominantly ranged from 2 to 24 months, with 7 studies not reporting the exact study period (Table 1).
6MWD
A total of 7 studies encompassing 456 participants were meticulously analyzed to discern the effectiveness of nursing interventions against standard care, focusing on 6MWD. The pooled analysis unveiled an overall SMD of 0.628 (95% CI: 0.261 to 0.996; z = 3.348, p = 0.001), implying a statistically significant change in the 6MWD, attributable to the nursing interventions when compared with the standard care (Figure 2). Cochran’s Q statistic was 19.57 (p = 0.003), and the I² statistic was observed to be 69.3%, which further underscores the notable variability among the enlisted studies. Sensitivity analysis did not reveal any substantial variation in the estimates (Supplementary Fig. 1). The funnel plot was slightly asymmetrical, but Egger’s test indicated no potential publication bias or other small-study effects in the meta-analysis, evidenced by a nonsignificant bias coefficient (–3.18, p = 0.199) (Supplementary Fig. 2).
Anxiety
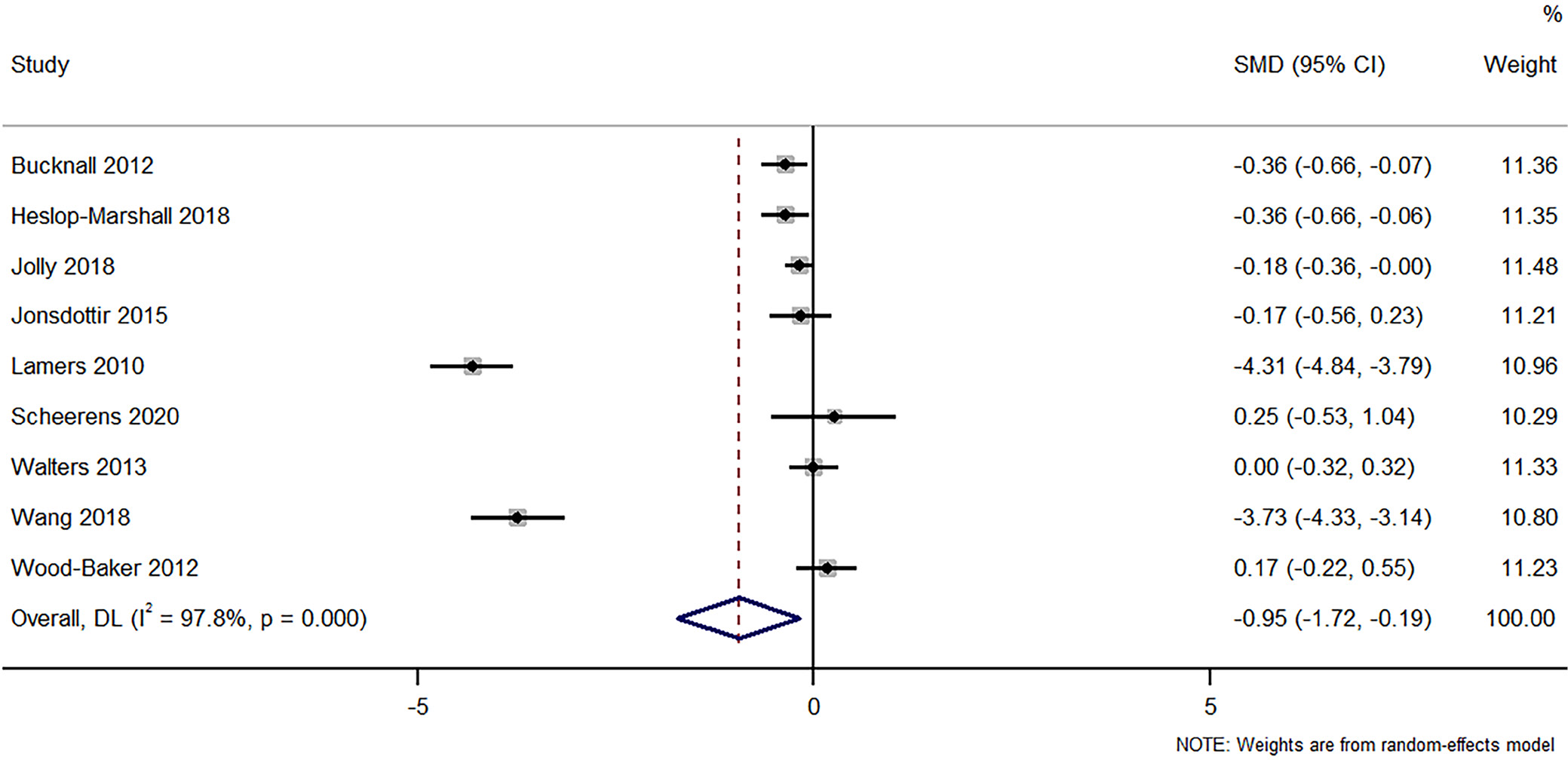
A total of 9 studies, enrolling 1,544 participants, were meticulously analyzed to discern the effectiveness of nursing interventions against standard care on anxiety scores amongst COPD patients. The pooled analysis revealed an overall SMD of –0.952 (95% CI: –1.719 to –0.186; z = –2.434, p = 0.015). This indicated a statistically significant reduction in anxiety, attributable to the nursing interventions, compared with standard care (Figure 3). Pertinently, Cochran’s Q statistic was reported as 357.35 (p < 0.001) and I² statistic at 97.8%, pointing towards a substantial level of heterogeneity among the included studies.
Upon executing a leave-one-out sensitivity analysis, omitting each study in turn, the overall SMD in anxiety outcomes due to nursing interventions among COPD patients ranged from –0.5259 to –1.0948. These findings affirm that the observed reduction in anxiety, SMD = –0.952 (95% CI: –1.719 to –0.186), remained robust and statistically significant across the analyzed studies (Supplementary Fig. 3). The funnel plot was slightly asymmetrical, but Egger’s test indicated no potential publication bias or other small-study effects in the meta-analysis, evidenced by a nonsignificant bias coefficient (–8.15, p = 0.161) (Supplementary Fig. 4).
Depression
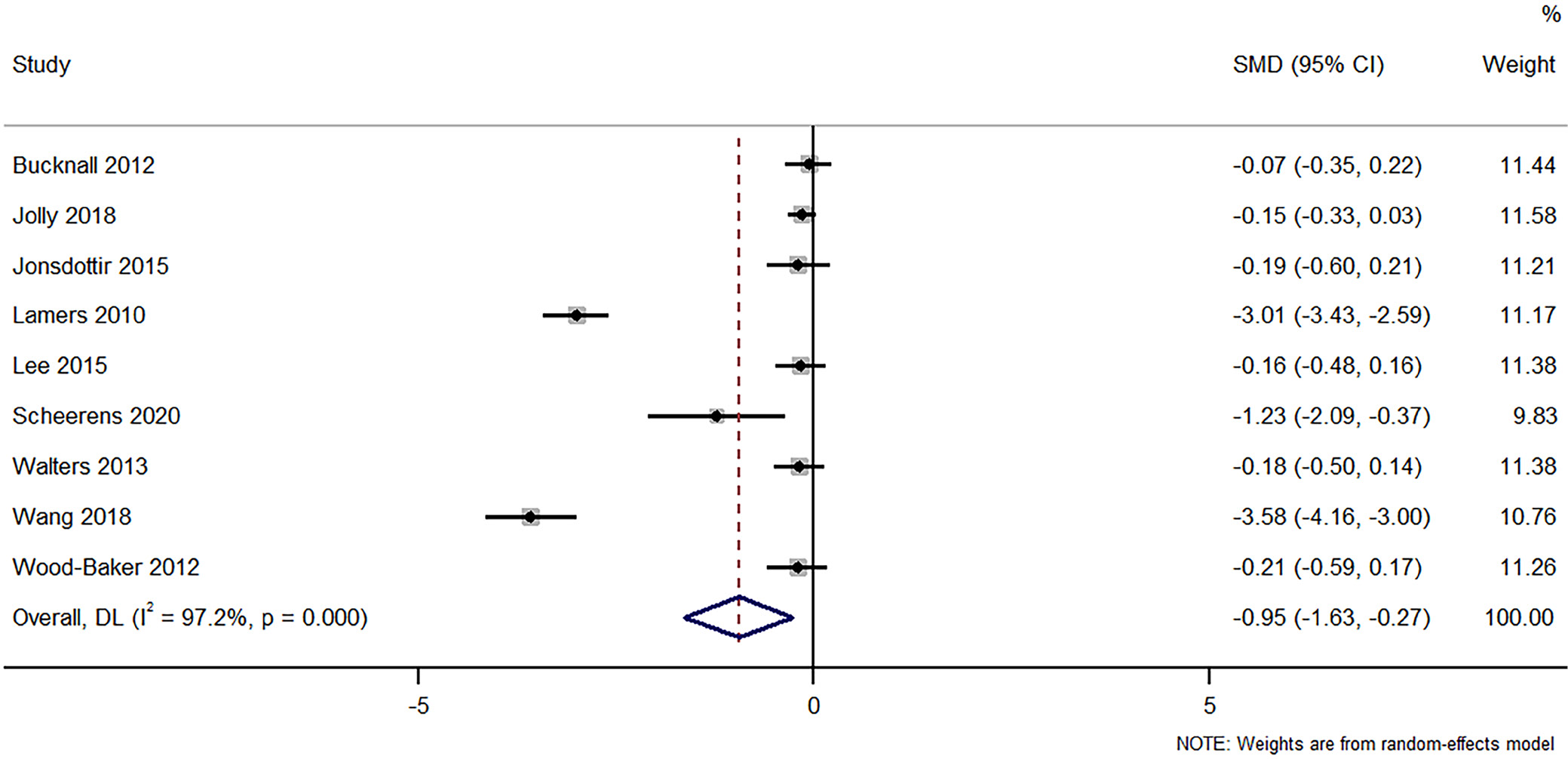
A systematic examination of 9 studies, incorporating 1,529 participants, was undertaken to discern the efficacy of nursing interventions relative to standard care in managing depression among COPD patients. The meta-analysis, employing a random-effects model, resulted in an overall SMD of –0.952, substantiating a statistically significant decrement in depression scores attributable to nursing interventions (95% CI: –1.631 to –0.272; z = –2.746, p = 0.006) (Figure 4). Substantial heterogeneity was manifested across studies (Cochran’s Q = 284.36, p < 0.001; I² = 97.2%).
Upon excluding each study one by one to assess the robustness of the results in a leave-one-out sensitivity analysis, the consolidated effect size (SMD) varied from –0.627 to –1.069, consistently underscoring a statistically significant reduction in depression scores attributed to nursing interventions across various iterations (Supplementary Fig. 5). The funnel plot was slightly asymmetrical, but Egger’s test indicated no potential publication bias or other small-study effects in the meta-analysis, evidenced by a nonsignificant bias coefficient (–8.44, p = 0.101) (Supplementary Fig. 6).
Self-efficacy
The meta-analysis involving 12 studies and 1,695 participants indicated a statistically significant improvement in self-efficacy outcome, with an SMD of 0.800 (95% CI: 0.361 to 1.240; z = 3.567, p < 0.001; Figure 5) However, high heterogeneity was observed among the studies (Cochran’s Q = 192.12, degrees of freedom (df) = 11, p < 0.0001; I² = 94.3%). The sensitivity analysis, omitting one study at a time and recalculating the pooled SMD for self-efficacy outcomes, still revealed a consistent effect size, indicating that the overall SMD (0.800; 95% CI: 0.0361 to 1.240) was not highly dependent on any single study (Supplementary Fig. 7). The funnel plot was symmetrical, and Egger’s test indicated no potential publication bias or other small-study effects in the meta-analysis, evidenced by a nonsignificant bias coefficient (14.25, p = 0.124) (Supplementary Fig. 8).
Hospitalization
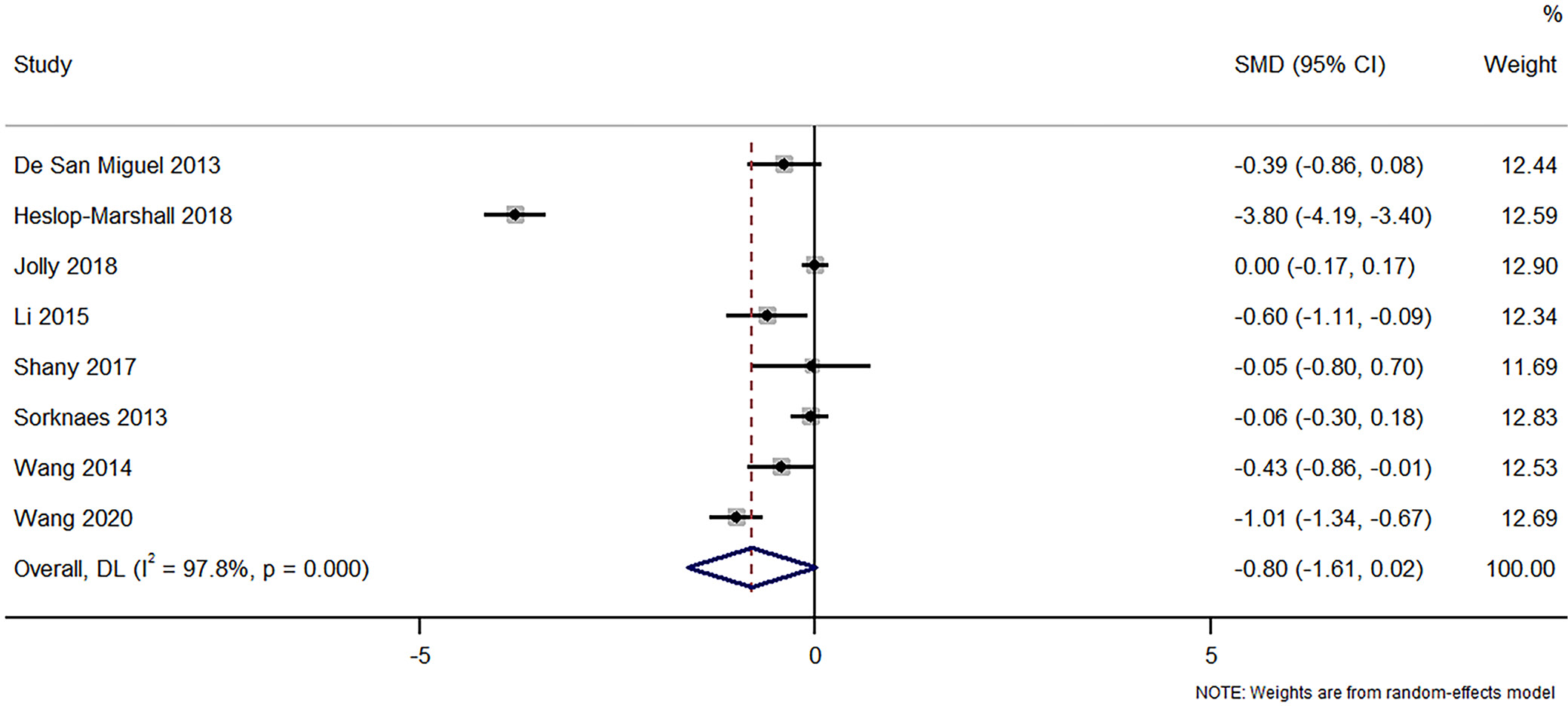
The pooled SMD from the meta-analysis, which included 8 studies and 1,464 participants, suggests a trend towards reduced hospitalization outcomes (SMD = –0.797, 95% CI: –1.611 to 0.018; p = 0.055), though it did not reach statistical significance (Figure 6). The high heterogeneity among studies (I² = 97.8%, p < 0.001) indicated substantial variability in effect sizes across the included studies. Leave-one-out sensitivity analysis suggests that the overall pooled estimate was relatively stable and not overly influenced by any single study (Supplementary Fig. 9). The funnel plot was symmetrical, and Egger’s test indicated no potential publication bias or other small-study effects in the meta-analysis, evidenced by a nonsignificant bias coefficient (–6.06, p = 0.133) (Supplementary Fig. 10).
Quality of life
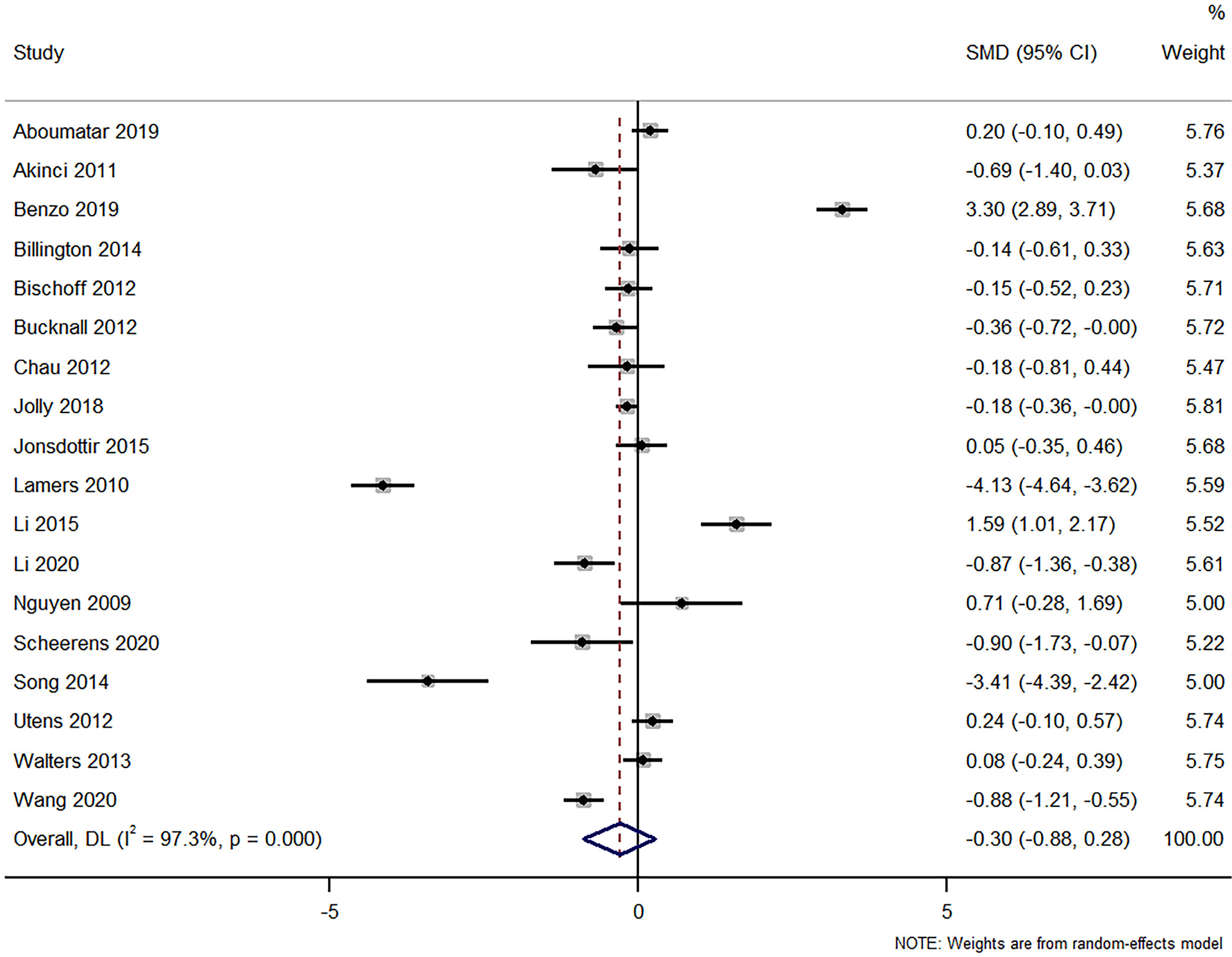
This analysis synthesizes the findings of 18 studies involving 2,179 participants, investigating the impact of nursing interventions on the QoL of COPD patients using the SGRQ as an outcome measure. The overall effect size (SMD) was –0.299, but was not statistically significant (p = 0.311), and there was substantial heterogeneity among study results (I² = 97.3%), suggesting that the interventions’ impacts on respiratory QoL varied widely across studies (Figure 7).
The sensitivity analysis reveals that the overall estimate of the impact on QoL marginally fluctuated when each study was omitted one at a time, with a combined estimate of –0.2989. The 95% CI ranged from approx. –0.877 to 0.279, crossing 0, which indicates a non-significant overall effect (Supplementary Fig. 11). This insensitivity to the omission of individual studies suggests that the meta-analysis was relatively robust. The funnel plot was symmetrical, and Egger’s test output showed that the intercept (bias) was –4.356, with a p-value of 0.727, which does not indicate a significant publication bias (Supplementary Fig. 12).
Dyspnea
Data from 6 studies, totaling 419 participants, were used to evaluate the effect of nursing interventions on dyspnea in managing COPD patients using a random-effects model. The overall SMD was –0.102 (95% CI: –0.529 to 0.326; p = 0.641), indicating no statistically significant effect of the nursing interventions on dyspnea compared to usual care across the included studies (Figure 8). Notably, there was significant heterogeneity among the studies (I² = 77.6%, p < 0.001). Sensitivity analysis revealed that the overall combined effect size, including all studies, was –0.102 (95% CI: –0.529 to 0.326). This CI crossed 0, indicating that the overall effect size was not statistically significant. However, the analysis revealed that the omission of the study by Akinci and Olgun48 changed the pooled effect size to a significant value, suggesting that this particular study might hold some weight or influence on the overall combined results (Supplementary Fig. 13). The funnel plot was symmetrical, and Egger’s test indicated no potential publication bias or other small-study effects in the meta-analysis, evidenced by a nonsignificant bias coefficient (4.83, p = 0.229) (Supplementary Fig. 14).
Patient satisfaction
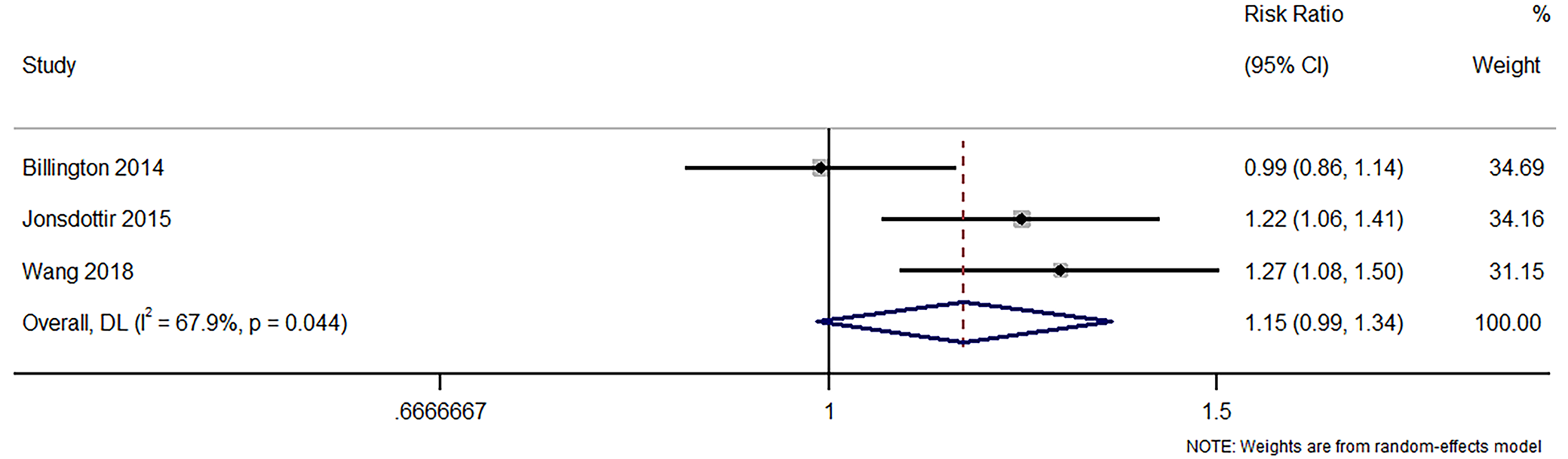
This meta-analysis incorporated findings from 3 studies, cumulatively analyzing data from 286 participants, to investigate patient satisfaction in COPD patients. The pooled RR across the included studies was 1.151 (95% CI: 0.987 to 1.343) (Figure 9). The test of the overall effect size was calculated with a z-value of 1.795 and an associated p-value of 0.073. Cochran’s Q was calculated to be 6.24, with an associated p-value of 0.044 and I² statistic of 67.9%, indicating a statistically significant level of heterogeneity. The sensitivity analysis revealed that the omission of the study by Billington et al.30 changed the pooled effect size to a significant value, suggesting that this particular study might hold some weight or influence on the overall combined results (Supplementary Fig. 15). The funnel plot was symmetrical, and Egger’s test indicates no potential publication bias or other small-study effects in the meta-analysis, evidenced by a nonsignificant bias coefficient (–0.20, p = 0.973) (Supplementary Fig. 16).
All-cause mortality
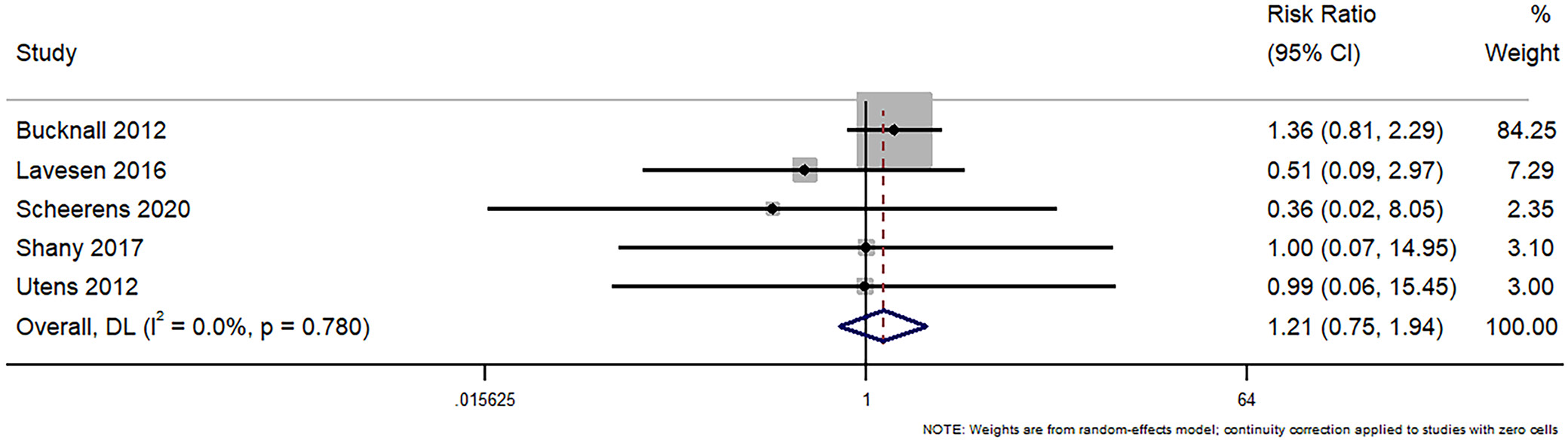
This analysis comprehensively synthesized the findings from a total of 5 studies involving 848 participants to investigate the impact of various interventions on all-cause mortality. The pooled RR across the analyzed studies was 1.206, with a 95% CI ranging from 0.749 to 1.943 (Figure 10). The overall effect was tested against the null hypothesis of RR = 1 and did not reach statistical significance (z = 0.771, p = 0.441). The Cochran’s Q value was 1.76 with df of 4, translating to a p-value of 0.780, suggesting that there was no statistically significant heterogeneity. Further, the I² statistic, which describes the percentage of variation across studies due to heterogeneity rather than chance, was 0%, indicating no observed heterogeneity (with its 95% CI ranging from 0.0% to 41.6%). The sensitivity analysis did not reveal any substantial variation in the estimates (Supplementary Fig. 17). The funnel plot was symmetrical, and Egger’s test indicates no potential publication bias or other small-study effects in the meta-analysis, evidenced by a nonsignificant bias coefficient (–0.76, p = 0.109) (Supplementary Fig. 18).
Discussion
In light of the critical role of nursing interventions in the management of COPD, this comprehensive review was conducted to illuminate the impact of these interventions on multiple clinical and psychosocial outcomes. The cumulative findings indicate a variable impact of nursing interventions on distinct domains of patient outcomes among individuals with COPD.
Regarding physical and functional capacity, there was a significant improvement in the 6MWD, with an SMD of 0.628. This underscores the potential benefit of nursing interventions in bolstering the exercise capacity of individuals with COPD, which is pivotal, considering the integral role of functional capacity in sustaining autonomy and QoL.
Anxiety and depression are paramount considerations in COPD management due to their prevalence and detrimental influence on adherence to treatment, health status and clinical outcomes. The evidence from this meta-analysis elucidates a statistically significant reduction in both anxiety and depression, aligning with some previous literature that has emphasized the efficacy of nursing care in enhancing psychological wellbeing through various strategies, such as patient education, behavioral interventions and self-management facilitation.49, 50
Contrastingly, although there was a trend toward reduced hospitalization (SMD = –0.797, p = 0.055) and improved QoL (SMD = –0.299, p = 0.311), these effects did not reach statistical significance.
Compared with prior research,49, 50 these results may reflect the inherent complexity and multifactorial nature of these outcomes, which can be influenced by numerous variables, including disease severity, comorbidities and social determinants of health, which are not solely contingent upon the quality or extent of nursing interventions.
In the context of self-efficacy, our findings illustrate a significant positive impact – an outcome that aligns with the theoretical underpinnings of self-management interventions, which often empower patients with skills and knowledge that foster a greater sense of control over their condition. Comparatively, the finding that nursing interventions did not exert a statistically significant impact on dyspnea diverges from some prior studies, which may be attributed to the variance in intervention types, delivery and the patient populations involved. This affirms the necessity for a nuanced understanding and application of nursing strategies, ensuring they are adeptly tailored to the multifaceted needs of COPD patients, potentially involving a multidisciplinary approach.
Given the importance of self-management in COPD care, it is imperative to highlight the interplay between self-management and the comorbidities often encountered by these patients. Effective self-management in COPD is not solely about managing the pulmonary symptoms but also entails a comprehensive approach that includes managing coexisting conditions such as cardiovascular disease, diabetes and anxiety/depression. This holistic approach is crucial, as these comorbidities can significantly impact patients’ overall health status, their ability to engage in self-management practices and their responses to nursing interventions.
Furthermore, the effectiveness of nurse-led interventions is intrinsically linked to their ability to enhance self-management capabilities in patients with COPD. Nursing interventions that focus on education, skill development and psychological support are designed to empower patients, enabling them to manage not only their respiratory symptoms but also the broader aspects of their health. This encompasses adherence to medication, recognition of exacerbation signs, lifestyle modifications, and coping strategies in dealing with the psychological burdens of the disease and its comorbidities.
The results from this meta-analysis necessitate a judicious interpretation. A critical assessment of the efficacy of nursing interventions underscores their potential role in enhancing physical, psychological and functional outcomes in COPD management, thereby advocating for their integration into routine clinical practice. These findings underscore the value of nursing professionals in the management of COPD, propelling the potential for targeted, patient-centered care, and also advocate for the integration of nursing interventions into conventional management protocols for COPD while emphasizing the indispensable role of nurses in enhancing patient-centered outcomes.
For nursing professionals and clinical practice, this study reaffirms the importance of targeted interventions for COPD patients and highlights domains such as psychological wellbeing and functional capacity as particularly responsive to such interventions. Furthermore, it reiterates the need for an individualized, patient-centered approach, considering the varied responses across different outcome domains.
This meta-analysis leverages robust methodological rigor and comprehensive data synthesis across numerous studies to provide a broad perspective on the impact of nursing interventions across various outcome domains. The sensitivity analysis also revealed that the findings of the study were credible and not sensitive to single study effects. This meta-analysis included only RCTs, the highest level of evidence to provide more reliable estimates, essential for making decisions regarding the implementation of the nursing interventions into the routine practice.
The relationship between nurse-led interventions and patient self-management in COPD is a critical area for exploration. The success of these interventions often hinges on their ability to foster an environment where patients feel capable and confident in managing their condition. This includes navigating the complexities introduced by comorbid conditions, which can complicate the management of COPD. By addressing these multifaceted needs, nurse-led programs can significantly contribute to the effectiveness of self-management practices among COPD patients. This, in turn, underscores the necessity for these interventions to be patient-centered and tailored to the individual’s specific health profile, including comorbidities.
While providing valuable insights, this study also paves the way for future research. A more in-depth exploration is needed to decipher the elements within nursing interventions that are most potent in driving positive outcomes in COPD management. Additionally, research investigating the longitudinal impacts of nursing interventions, the optimization of their implementation in varied healthcare contexts and the identification of patient subgroups who derive maximal benefit would be worthwhile. Future research with rigorous design, adequate power and meticulous reporting will further contribute to the evidence base, making it possible to delineate the role and optimization of nursing interventions in COPD management.
Limitations
Nevertheless, it is imperative to acknowledge the present study’s limitations. The evident heterogeneity among some of the included studies, particularly in areas such as anxiety and depression, is indicative of variability in study designs, populations and interventions, potentially influencing the collective findings. Furthermore, the risk of bias assessment unveiled varied integrity among the studies, with several marked as “high risk,” potentially affecting the credibility and generalizability of the findings.
Another limitation resides in the potential influence of unaccounted confounding variables such as varying healthcare systems, practitioner expertise, intensity of the management program, follow-up, method of conducting the patient, and patient adherence, which might have influenced the observed outcomes and heterogeneity. Furthermore, the varying duration of interventions across the studies presents a potential variable that could influence the results and is not systematically evaluated within this paper.
Conclusions
This review underlines the significant potential of nursing interventions in enhancing certain domains of outcomes for individuals with COPD, specifically in areas such as exercise capacity, anxiety, depression, and self-efficacy. Although variable impacts are observed across different outcome domains, these findings herald the value of nursing interventions as a crucial component of comprehensive COPD management. Harnessing these insights and refining and understanding these interventions will be pivotal in evolving the holistic, patient-centered management of COPD, thus optimizing patient outcomes and QoL in this prevalent and impactful condition.
Ethical approval and consent to participate
This study was approved by the Ethics Committee of The First Hospital of Hebei Medical University (approval No. 20230238).
Supplementary data
The supplementary materials are available at https://doi.org/10.5281/zenodo.11295652. The package includes the following files:
Supplementary Appendix. Search strategy.
Supplementary Fig. 1. Sensitivity analysis for 6MWD.
Supplementary Fig. 2. Funnel plot for 6MWD.
Supplementary Fig. 3. Sensitivity analysis for anxiety.
Supplementary Fig. 4. Funnel plot for anxiety.
Supplementary Fig. 5. Sensitivity analysis for depression.
Supplementary Fig. 6. Funnel plot for depression.
Supplementary Fig. 7. Sensitivity analysis for self-efficacy.
Supplementary Fig. 8. Funnel plot for self-efficacy outcome.
Supplementary Fig. 9. Sensitivity analysis for hospitalization.
Supplementary Fig. 10. Funnel plot for hospitalization.
Supplementary Fig. 11. Sensitivity analysis for QoL.
Supplementary Fig. 12. Funnel plot for QoL outcome.
Supplementary Fig. 13. Sensitivity analysis for dyspnea.
Supplementary Fig. 14. Funnel plot for dyspnea.
Supplementary Fig. 15. Sensitivity analysis for patient satisfaction.
Supplementary Fig. 16. Funnel plot for patient satisfaction.
Supplementary Fig. 17. Sensitivity analysis for all-cause mortality.
Supplementary Fig. 18. Funnel plot for all-cause mortality.
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Consent for publication
Not applicable.
Use of AI and AI-assisted technologies
Not applicable.