Abstract
Background. Disparities persist in access, quality and outcomes across different socioeconomic strata. Addressing these disparities requires a comprehensive understanding of the underlying factors contributing to healthcare inequities. Even though healthcare equity has been discussed in the literature, no comprehensive frameworks have been developed considering the given country’s distinctive demographic cultural and socioeconomic variables.
Objectives. This study proposed an equity-based financial framework to enhance the sustainability of the healthcare system in Saudi Arabia, the United Arab Emirates (UAE) and Qatar. Moreover, this research aimed to examine the key factors influencing equitable access to healthcare services.
Materials and methods. A cross-sectional study design was employed, utilizing national health accounts, demographic surveys and health outcomes data from 3 Arab countries: Saudi Arabia, UAE and Qatar. The study included participants from 15 medical organizations, 500 policymakers and 10,000 patients. A stratified random sampling technique was employed to ensure a diverse and representative sample. The economic equity measurements included the principal component analysis (PCA) and Theil index. Financial sustainability was evaluated using techniques such as the cost-effectiveness analysis (CEA) and systems dynamics modeling techniques.
Results. This study identified a positive convergence in healthcare systems among Qatar, Saudi Arabia and the UAE. The Theil index value of 0.35 suggested a balanced distribution of healthcare resources across the 3 countries. Policy A had an incremental cost-effectiveness ratio (ICER) of $15,000 per quality-adjusted life year (QALY), making it more cost-effective compared to Policy B with an ICER of $20,000 per QALY and Policy C with an ICER of $25,000 per QALY. The Delphi technique achieved a consensus level of 90%, while Policy C emerged as the most preferred option in the multi-criteria decision analysis (MCDA), scoring a total of 85 points. Moreover, the PCA accounted for 60% of the variations related to healthcare equity in the specified countries.
Conclusions. The findings of this study provide valuable insights for policymakers, offering a new roadmap for economic evaluation studies aimed at enhancing healthcare equity and sustainability in Arab countries.
Key words: multilevel analysis, principal component analysis, spatial analysis, healthcare equity, equity-based financial framework
Background
Sustainability refers to the ability to meet the needs of the present generation without compromising the ability of future generations to meet their own needs. The World Commission on Environment and Development famously characterized sustainability in a 1987 study as “growth which addresses the requirements of the present while maintaining the ability of future generations to meet their requirements”.1 This definition has since spread around the globe. The issue of healthcare system sustainability has become highly controversial due to the increasing demand for healthcare services and the corresponding high expenditures.2 Regardless of the debates, the study of healthcare system sustainability is moving forward rapidly. Its significance emerged from the desire to assess the sustainability of well-known healthcare organizations over the long term, considering their changing objectives. Financial sustainability, or keeping income equal to expenditures, is as essential in the healthcare industry as it is in every other sector of the economy.3, 4 Financial sustainability is a concept that has been used frequently in academic circles, the media and political discussions. However, there is no universal consensus on its definition or the best approach to its implementation.
Achieving financial sustainability, along with the political implications associated with this goal, are topics that the healthcare system seldom addresses.5 Healthcare system financing is central to the debate on healthcare system sustainability.6 According to the World Health Organization (WHO), healthcare system financing involves “collecting funds from numerous sources, pooling them and distributing them to healthcare providers.”7 A well-functioning health financing system, as defined by WHO, ensures financial protection and equitable access to healthcare services. Furthermore, the WHO emphasizes that “a good health financing system generates sufficient resources for health, enabling individuals to access the services they need without facing financial hardship or being pushed into poverty due to out-of-pocket payments.”7 In other words, securing sufficient financing should be the priority of any health system. Both providers and consumers are encouraged to be more efficient.8 As healthcare expenditures increasingly strain national and government budgets, the financial health of publicly supported healthcare systems in many countries is deteriorating. Resource scarcity, increasing health spending relative to their gross domestic product (GDP), and rising costs of health services caused by variables influencing demand and supply are reasons why healthcare systems are usually mentioned as requiring ever-increasing subsidies and showing that public funding is insufficient.5, 6 According to a 2013 study by the World Economic Forum (WEF), 9 the significant reasons for the increase in healthcare costs are an aging population, a shift toward chronic diseases caused by lifestyle choices, increasing public expectations, and a lack of value-care concepts among healthcare customers.
Access to high-quality healthcare should be a fundamental human right because of the substantial association between an individual’s productivity level and ability to flourish economically.10 Providing high-quality healthcare to all individuals is an essential objective of the United Nations’ Sustainable Development Goals (SDGs). According to SDG 3.8, it is emphasized that individuals should be protected from excessive healthcare expenditures, and access to adequate healthcare should be improved.11, 12 Universal health coverage (UHC) is an idealistic objective to improve healthcare accessibility, affordability and quality.13 Global support for UHC has developed since the 2010 World Health Report was released. To reduce healthcare disparities and promote equity, UHC must cover everyone, regardless of their income or where they live.14
An ongoing rise hinders worldwide efforts to achieve UHC in healthcare spending. In some nations, healthcare expenditures can exceed 10% of the GDP.15 A combination of factors, including an aging population, more individuals needing treatment, more people living with chronic diseases, and the increasing cost of new medical technologies, will have an impact on every society.16, 17, 18, 19 Sustainability, or the capacity of healthcare systems to keep running and be financially viable in the future, is a big concern in modern healthcare.11 Economic sustainability in healthcare means consistently providing high-quality services while covering operating costs.11, 20 Some people are concerned about the sustainability of possible financial solutions, such as cutting services, holding fundraisers or redistributing funds.13 Government action is required to assist nations in achieving their UHC objectives, which would need increased revenue or reductions in spending in other areas to fund the staggering healthcare expenses.15, 16
It is crucial to consider the policy choices of key stakeholders in health financing when determining health priorities to ensure that selected policy solutions are practical and that UHC is effectively implemented. Evaluating whether stakeholders have aligned or differing perspectives on healthcare funding is essential for assessing the effectiveness of policy developments. The literature on healthcare funding has just scraped across the surface of this problem and has recently been investigated extensively within the Arabian Gulf region. Understanding these preferences is of fundamental significance, given that healthcare represents a significant amount of the Saudi Arabia budget.
Numerous studies have examined the growing expense of healthcare; nonetheless, most of these studies have focused on the effects of out-of-pocket charges on individuals’ wellbeing and disparities in health.17 Findings from studies that explore different healthcare funding strategies are very few and far apart. The sustainability of healthcare financing methods over a long period is yet another field where knowledge is limited. Countries like the Saudi Arabia, United Arab Emirates (UAE) and Qatar, which depend excessively on revenue from natural resources, cannot pay for healthcare while providing it for free. This context cannot generalize results from comparable European studies.18 Additionally, the demographics of Arab countries are relatively unique due to their sizeable expatriate population, which necessitates different financing mechanisms to minimize government health expenditures.21 Therefore, conducting stakeholder surveys is essential to understand financing preferences and explore various policy alternatives, enabling the selection of the most effective approach. These results can be relevant to the whole Gulf region, not only Saudi Arabia, due to the similarities in culture and trust between all 3 nations.
Gulf countries currently face a high rate of lifestyle-related risk factors for non-communicable diseases (NCDs), including physical inactivity, obesity and a high-calorie diet, which are likely to worsen due to the sedentary lifestyles of the aging population. Non-communicable diseases are already the most significant burden on healthcare in these countries, but curtailing these risk factors will necessitate non-health sector involvement.21
Gulf countries currently face a shortage of skilled healthcare workers within the healthcare sector.22 Healthcare delivery systems are primarily dependent on the large expatriate population, which has resulted in clinician competency disparities and a high turnover rate.23 Other challenges that these countries are facing include timely referrals and follow-ups of patients and inadequate infrastructure for mental health.21
Objectives
The study aims to assess healthcare equity in the UAE, Saudi Arabia and Qatar while comparing the inequality in the distribution of access, quality and cost of healthcare services. The research shall further seek to establish specific causal factors behind these disparities by employing sophisticated quantitative instruments, including the principal component analysis (PCA) and the Theil index. These rigorous methods will ensure the accuracy and reliability of our findings. Further, the study aims to establish and advance an equity-based financial framework and policies that may be applied to promote healthcare equity in the region.
This research seeks to establish an equity-based financial model for improving healthcare systems. It aims to reduce inequalities in healthcare service delivery and the utilization of healthcare services by adopting different revenue models, equality in resource distribution and utilization, reasonable financial risk management, and collaboration between sectors. This research proposes a new financial model based on equity suitable for demography, culture and economy. The study provides a framework for narrowing healthcare disparities by integrating the health equity measurement framework (HEMF) with innovative financing methods, including social impact finance bonds and community bond plans. The framework focuses on a fair distribution of resources, people who need them the most, targeted protection of finances, and cross-sector working. This study aims to fill the gap by presenting a comprehensive approach, including a quantitative approach, culturally sensitive care interventions, constant assessment, and support. This gives equal opportunities for healthcare services to all the citizens of a country irrespective of their class or area of residence, hence making the healthcare systems more equitable and sustainable. The novelty of this study lies in its examination of multiple regions simultaneously, comparing their respective features and identifying actionable points of similarity between them that can impact the effectiveness of policies. Additionally, the framework developed here can be fitted to the specific needs of the countries in question, resulting in policies tailored to meet their populations’ demands.
Health equity measurement framework
The HEMF offers a broad theoretical framework for the study, representing a practical approach to identifying and eliminating healthcare inequities. The WHO developed the HEMF, which can be regarded as a comprehensive model that encompasses social determinants, health system issues and health outcomes.19 To begin with, the HEMF sheds light on the fact that the structural determinants are complex and synergistically affect healthcare access, utilization and outcomes. This set of factors is diverse and includes socioeconomic factors, such as income, education and employment, as well as geographical factors, including the urban–rural divide and distance to health services.19 It pinpoints health determinants that shape healthcare inequality relevant to this study, such as socioeconomic status and geographical features.
Additionally, the HEMF states that healthcare system characteristics such as provision, access and policy inequalities are crucial for achieving health equity. Such factors include funding systems, allocation strategies and service models that concern healthcare. The framework conceptualizes that every facet of equitable financing and efficacious resource distribution is a precondition for justice in healthcare delivery.20 Sustained by this notion, the study investigates the means of healthcare funding and their correlation to healthcare equality. The HEMF also reiterates the significance of inter-authority cooperation and policy interventions in eliminating health inequities. This concept underscores the notion that healthcare inequity transcends the confines of the healthcare system, necessitating collaborative efforts with other service sectors, such as social welfare, education and housing, to ensure equitable access to healthcare.20 This part of the framework is relevant to our work on policy interventions and their expected outcome on healthcare equity.
Furthermore, the HEMF highlights the importance of integrating and disaggregating data collection and analysis to identify and care for specific subgroups of populations, including their unique healthcare needs and barriers, such as age, gender and culture.24 This congruency aligns with the meaningful observation of demographic attributes as 1 health equity variable. Finally, HEMF supports the implementation of monitoring and evaluation systems to assess the effectiveness of health equity initiatives, ensuring they achieve their intended outcomes and allowing for data-driven adjustments as needed. This part of the systemic plan is congruent with the study’s objective of sustaining quality improvement. Consequently, it is based on applying evidence-based strategies to achieve the desired outcomes. This study relies on the HEMF as a robust theoretical foundation offering a comprehensive perspective from which the multifarious factors that promote healthcare equity in Saudi Arabia can be analyzed. In light of these considerations, the research has sought to examine the characteristics that determine the equity and affordability of health services, focusing on ensuring all citizens’ wellbeing. The findings of this research will contribute to the development of evidence-based health equity objectives.
The HEMF was chosen for this study because of its direct relevance to the goal. It provides a structure that includes the social determinants of health: income, education and geography, which are crucial for analyzing Arab healthcare disparities.20 The study’s objective of evaluating healthcare financing and access based on socioeconomic status is congruent with HEMF’s emphasis on policy inequalities.21 Furthermore, its consideration of both system factors and demographic needs of the related population makes it suitable for addressing the unique population and expatriate-oriented workforce nature of Arab countries.22 Lastly, HEMF is equipped with sound monitoring and evaluation approaches that ensure the continuous measurement of the performance of health equity undertakings, making it a valuable tool for sustainable and long-term health equity resulting from specially designed and implemented initiatives.
The study is structured as follows: the Background section presents the context and relevance of the study by discussing healthcare equity and sustainability issues. The Healthcare Equity Measurement and Financial Sustainability section covers aspects of healthcare equity measurement, the financial sustainability of healthcare and relevant case studies. The Study Design and Methodology section details the study settings, analysis instruments, techniques, and stakeholder communication approaches. The Healthcare Equity and Policy Comparisons section provides an overview of healthcare equity and financial sustainability while comparing policy scenarios. The Results and Policy Implications section reanalyzes the results, considers policy implications and recommendations, and outlines limitations and future research prospects. Finally, the Final Recommendations and Impact Assessment section provides the final recommendations and assesses the impact of the proposed framework.
Methodology
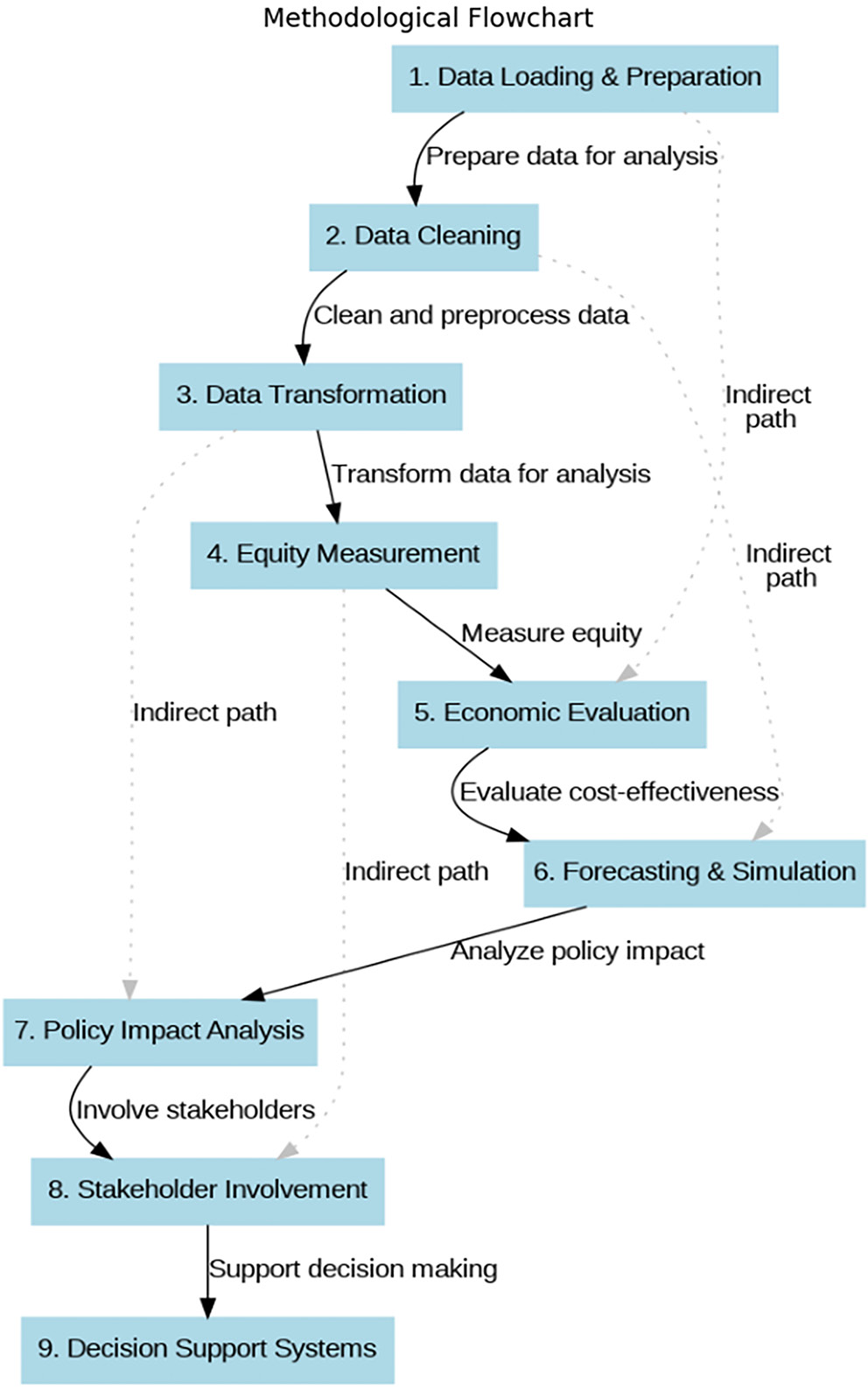
Multi-criteria decision analysis (MCDA) is a decision-support tool that helps evaluate multiple policy alternatives by considering several criteria. This study used MCDA to compare different healthcare policies based on factors such as equity, cost and efficiency. The analysis was conducted using Python 3.10 on Google Colab (Google LLC, Mountain View, USA), enabling a systematic ranking of policy options. The criteria for evaluating policies were identified based on their relevance to healthcare sustainability. Weights were assigned to each criterion through expert consultation, with equity (40%), cost (30%) and efficiency (30%) being prioritized. Each policy alternative was scored against these criteria, and the weighted sum model was used to compute the overall scores. The MCDA results showed that Policy C outperformed the others, with the highest score of 0.90, indicating it was the most effective in balancing cost, equity and efficiency. This structured decision-making process ensured that the chosen policy would maximize healthcare benefits while maintaining financial sustainability. The MCDA provided a clear framework for making well-informed, transparent policy decisions in the context of healthcare. Figure 1 shows the methodology adopted for this study. Initially, the data were loaded and prepared for analysis, cleaned, and preprocessed using various methods to ensure that missing data points did not adversely affect the applicability and accuracy of this research. Then, the data were transformed into a form that could be fed to the models involved in this study. The parsed data was analyzed to determine the extent of the equitability of healthcare distribution. The chosen method for this purpose was the Theil index and multilevel modeling. The economic sustainability of the various healthcare activities was analyzed by comparing their cost differentials against the differences in their effectiveness using the incremental cost-effectiveness ratio (ICER). Autoregressive integrated moving average (ARIMA) was then used to forecast future healthcare expenditures and needs. In contrast, systems dynamics modeling was used to evaluate the impact of policy changes on healthcare sustainability. Policy impact was analyzed deterministically and stochastically, while game theory was used to identify optimal decisions. The Delphi technique involved stakeholders, while MCDA was used to determine the ideal choices in ensuring healthcare sustainability. These details were further elaborated in the sections Study Design, Data Collection, Analytical Techniques, Stakeholder Engagement, and Policy Evaluation. This research used a cross-sectional design to build an equity-based financial model supporting sustainable healthcare delivery across Arab countries. It used national health accounts, demographic surveys and data on the health outcomes of multiple countries as components. Analytical tools employed when measuring equity and assessing the sustainability of costs included multilevel analysis and spatial analysis, among others. Cost considerations and system dynamics projections identified upcoming healthcare costs and resources required in the future. Delphi techniques and focus groups were prerequisites for assured stakeholder participation. The study sought to offer country-specific policy solutions to improve healthcare accessibility and financial stability within the Arab world. The study was conducted among healthcare systems in the Arab region and included primarily quantitative data. The target population would be national healthcare systems involving data from healthcare institutions, policymakers and patients. The stratified random sampling model included participants from different socioeconomic groups and diverse health facilities, including urban and rural settings. Individual data participants were divided into various strata based on their socioeconomic standings, after which participants were randomly selected until the requisite quotas were met. Data sources included National Health Accounts, demographic surveys, sentinel hospital records, and public health databases. The data were analyzed using multilevel, spatial and economic methods and other quantitative techniques, including multilevel modeling, spatial analysis and economic evaluations. This approach enabled a more integrated and comprehensive assessment of healthcare equity and sustainability in the Arab region.
In terms of data collection, this study utilized diverse sources and methods from across the Arab region. Both primary and secondary data were employed to analyze healthcare expenditures in the sampled countries. Data on healthcare expenditures were obtained from national health accounts, government budgets and insurance claims.
Cross-sectional data comprised demographic information sourced from population surveys and nationally representative census data obtained from the respective national statistics bureaus.
Information about health outcomes was collected from the hospital information system, national and regional databases and patient registers. Among other factors, income distribution, education and employment information were retrieved from various countries. The data collection techniques included structured questionnaires to provide accurate, uniform and comparable demographic and socioeconomic characteristics. Administrative data collection was standardized to ensure consistency despite differences in nations. Large datasets were collected from electronic health records (EHRs) and insurance claims; therefore, big data analytics were used for quantitative data analysis. This multifaceted approach utilizes multiple methodologies to provide a broader and more definitive approach to measure and assess the equity and sustainable characteristics of the healthcare systems in the Arab region.
Data preprocessing
We utilized techniques for managing missing data, including multiple imputations and the k-nearest neighbors (KNN) algorithm. Multiple imputations involved filling in missing data multiple times using statistical models and combining the results to account for the variation in the imputation process. The KNN algorithm replaced missing values by assigning them the value of the most similar observation within the dataset.
Outlier detection
The robust statistical methods used in identifying the outliers are as follows: z-score method, whereby an observation is considered an outlier with a z-score beyond the set limit, for instance, |z| > 3.
(1)
where X is the data point, μ is the mean or average of data, and σ is the standard deviation of the data points.
Data transformation
Normalization and standardization
Data normalization brings the data into a range of 0–1, while standardization centers the data at zero and gives a standard deviation (SD). This makes it easier to compare the information gathered from various countries.
Dimensionality reduction
After data collection and pre-processing, PCA was applied to analyze the dataset and reduce its dimensionality while preserving as much variance as possible. The PCA transformed the original variables into new orthogonal variables, known as principal components, which were ranked according to their contribution to the total variance in the dataset.
The PCA is a statistical technique that simplifies large datasets by reducing the number of variables while retaining the most significant information. It transforms the original variables into a smaller set of new components, each representing a combination of the original data. These components capture the essential patterns or variations within the dataset, allowing for a more manageable and insightful analysis.
In this study, PCA was employed to examine healthcare disparities by focusing on key factors such as healthcare expenditure, the availability of healthcare professionals and access to essential medical services. The 1st principal component accounted for 40% of the total variance, while the 2nd explained 25%.
Together, these components captured 65% of the variance in the dataset, providing a meaningful reduction in dimensionality. The number of components retained was determined using a scree plot and a cumulative variance threshold of 80%, ensuring the most significant patterns were captured.
The 1st principal component was associated with access to healthcare services, while the 2nd component reflected healthcare quality differences across regions. These insights are essential for identifying which healthcare elements contribute most to regional disparities. Understanding these key drivers of inequality is crucial for informing policies and strategies to improve healthcare access and quality. This approach ensures that resources can be more effectively allocated to areas where healthcare improvements are most needed.
In analyzing the patterns of healthcare equity in Arab countries, this study uses PCA methodology to examine the data. The reason for using PCA stems from the applicability of this technique for dimensionality reduction of large datasets and the necessity for the researchers to focus on the variables that impact the variance of healthcare outcomes most significantly. Another advantage of this method for analyzing initial variables is that by transforming them into principal components and conducting PCA, only the most significant factors are considered, which helps when interpreting the results. This method helps determine and compare the characteristics of healthcare systems in developing equity policies.
Equity measurement
Theil index
This study utilized the Theil index to assess economic disparity. The Theil index is particularly useful for decomposing inequality within and between groups, providing a comprehensive perspective on disparities in healthcare expenditures across regions. It effectively captures economic disparity and can be disaggregated into within-country and between-country components, allowing for a more nuanced analysis. The formula for the Theil index is as follows:
(2)
where:
T – Theil index;
N – total population size;
yi – income or expenditure of individual I;
yˉ – the average of the variable y across all units;
μ – mean income or expenditure across the population;
ln – the natural logarithm.
The Theil index is a powerful tool for measuring economic inequality. It allows researchers to analyze income distribution or resources within a population. It assesses overall inequality and can be decomposed to evaluate disparities within groups (e.g., regions or demographics) and between groups.
The index ranges from 0 to infinity, with 0 indicating perfect equality (everyone has the same income) and higher values representing increasing levels of inequality. The Theil index is handy because it can identify the contributions to overall inequality from different subgroups, providing insights into how various factors, such as regional disparities in healthcare spending, affect overall equity.
In the context of healthcare analysis, the Theil index can help quantify how healthcare expenditures are distributed among different regions or populations, highlighting areas where disparities may exist. This information is critical for policymakers aiming to address inequalities and ensure that healthcare resources are allocated more equitably.
In this study, the Theil index determined income distribution regarding health and health status access. The Theil index is particularly advantageous as it allows for the decomposition of inequality both between and within groups, providing a more comprehensive depiction of inequality dynamics.
This is useful in generating the productivity of health units and even in assessing the fairness of distributing healthcare within the sample population. The Theil index allowed the study to quantify the level of inequality and identify the contributing factors. Hence, the various mechanisms for change could identify which regions need attention to enhance a more equitable healthcare system.
Multilevel modeling
Multilevel modeling helps analyze datasets with nested data, where specific units group together within higher-order units (e.g., patients are nested within hospitals; hospitals are nested within countries). The basic form of a multilevel model is:
(3)
where:
Yij – outcome or dependent variable for individual i in group j;
β0 – intercept, or the average outcome across all groups, when the predictor Xij is 0;
β1 – fixed effect for the predictor Xij represents the relationship between Xij (the independent variable) and the outcome Yij;
Xij – predictor variable or independent variable for individual iii in group j;
μj – random effect for group j, which accounts for group-level differences. This term allows the model to account for variability between groups (such as hospitals, schools, countries, etc.);
eij – residual error or individual-level error term accounts for the variability not explained by the model for individual iii in group j.
Financial sustainability assessment
Cost-effectiveness analysis
A cost-effectiveness analysis (CEA) was conducted to compare the efficiency of various healthcare interventions in relation to their costs and overall impact.
The ICER was calculated as:
(4)
where:
ΔC represents the difference in cost, while ΔE denotes the difference in effectiveness between 2 interventions.
Forecasting and simulation
Time series analysis
Time series analysis predicts future healthcare expenditures and resource needs using models such as ARIMA:
(5)
where:
Yi – the value of healthcare expenditures and resource needs at time t;
c – a constant term that represents the baseline level of the time series;
θj – the autoregressive coefficient for lag j, indicating the influence of past values of the time series on the current value;
θj – the moving average coefficient for lag J, showing the influence of past error terms on the current value;
εj – the error term (or shock) at time ttt, accounting for the random variation not explained by the model.
Estimated parametric values for the ARIMA models
This research used the ARIMA model to analyze the time series data. The identification of the ARIMA model was determined by 3 sets of parameters known as p, d and q, where:
p depicts the number of autoregressive terms;
d depicts the order of differencing;
q depicts the count of moving average terms.
We have estimated the following parameters to model the selected commons: autoregressive (AR) coefficients: These coefficients measure the relationship between the current observation and a specified number of lagged observations. For example, using estimates from our model, the actual values were as follows: AR (1) = 0.65; AR (2) = −0.25. Moving average (MA) coefficients reflect the relationship between the current observation and a specified number of lagged forecast errors. Our model’s estimated MA parameter values were: MA (1) = 0.50; MA (2) = 0.10. C constant term: This term represents the mean of the series. The estimated constant term in our study was C = 1.5. Variance of the residuals: This parameter indicates the variance of the residual errors in the model. The estimated variance was σ2 = 0.75.
Model selection and diagnostic checking
The ARIMA model was selected based on the Akaike Information Criterion (AIC) and Bayesian Information Criterion (BIC). The model with the lowest values for these criteria was chosen, indicating the best fit.
To further ensure the model’s validity, a comprehensive residual diagnostics process was performed to check for autocorrelation and normality of the residuals. The results confirmed that the residuals were approximately white noise, indicating that the fitted ARIMA model was well-specified and reliable, providing a high confidence level in its adequacy.
The ARIMA is a widely used forecasting technique for time series data. This study applied ARIMA to model and predict future healthcare expenditures across regions. The ARIMA model was built following a systematic approach to parameter selection and model validation.
The selection of model parameters was based on examining the autocorrelation and partial autocorrelation (ACF/PACF) plots. Residual analysis was conducted to ensure model fit, and the Ljung–Box test confirmed that the residuals were not autocorrelated. The model was validated using cross-validation by comparing the forecasted healthcare expenditures with actual historical data to assess its predictive accuracy and reliability.
The ARIMA model provided reliable predictions, indicating no significant trends or seasonality in the healthcare expenditure data. This forecasting method is essential for anticipating future resource needs, enabling policymakers to allocate funds effectively for long-term healthcare sustainability.
System dynamics modeling explores how policy changes influence the sustainability of healthcare systems. Often, this involves differential equations that describe the temporal evolution of the system’s components.
Policy impact analysis
Deterministic scenarios
A deterministic approach involves evaluating the impact of a specific policy change within a defined context, where outcomes are precisely determined based on the given assumptions and environmental conditions.
Stochastic modeling
Stochastic modeling describes variability and uncertainty in policy impacts and predicts possible variations through probabilistic approaches.
Optimization techniques
Game theory
Game theory depicts how different players within a particular system are likely to behave. Nash equilibrium is a fundamental concept in this strategic framework. It represents a state where no player can improve their outcome by unilaterally changing their strategy, assuming all other players maintain their current strategies.
Stakeholder involvement
Delphi technique
The Delphi technique employs surveys to gather expert opinions and achieve a consensus on critical policy issues. It is particularly useful for reaching agreement among experts on various healthcare policy options. The utilization of the Delphi technique is based on the systematic process of soliciting and processing information from various experts through several questionnaires. This method also ensures that many opinions are considered and recommendations are well accepted and informed. The Delphi technique is used in this study to address gaps in equity-focused healthcare policies by involving all relevant stakeholders, enhancing the quality of policy recommendations and fostering consensus-driven decision-making.
Decision support systems
Multi-criteria decision analysis
The MCDA ranks policy alternatives concerning several goals or criteria, such as equality, cost and efficiency. A commonly used approach is the weighted sum model:
(6)
where:
Si represents the score of option i, wj reflects the weight of criterion j and xij denotes the performance of option i in criterion j.
It is essential to clarify how MCDA is applied in evaluating healthcare policy alternatives in the decision and criterion spaces that show the research problems (MCDA analysis). Policy options to improve healthcare equity include Policies A, B and C. The factors used to evaluate these policies, such as cost-effectiveness, equity, sustainability, and stakeholder acceptability, are all included in the criterion space.
In the current research, MCDA systematically compared these alternatives, scoring each policy against the criteria. Each criterion was weighted according to its importance to the overall objective of healthcare equity enhancement. This structured approach ensured that the policy chosen was well-rounded and covered multiple dimensions of the problem. Table 1 illustrates how each policy was scored across the selected criteria.
Results
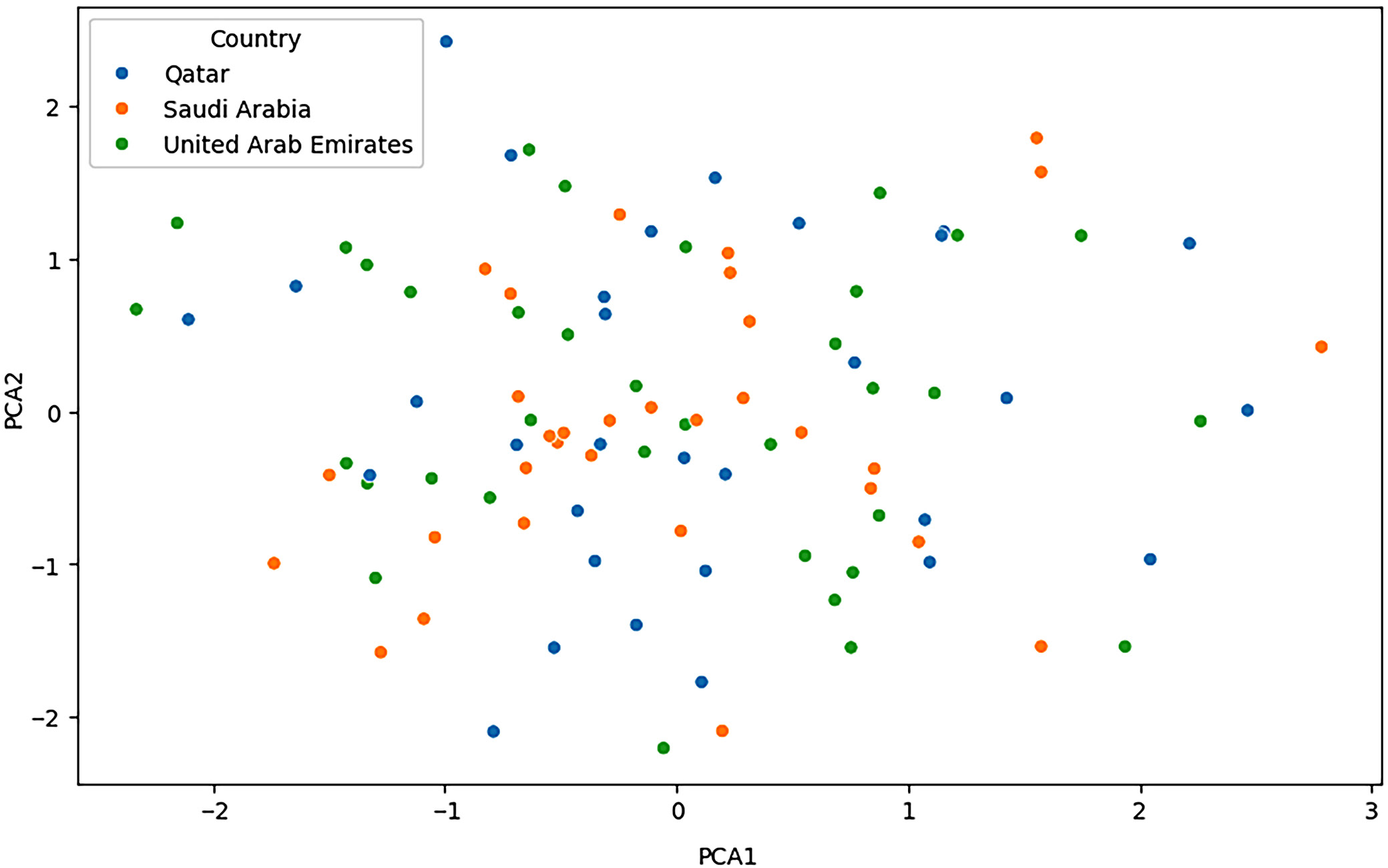
Figure 2 illustrates the application of PCA to healthcare data collected from Qatar, Saudi Arabia and the UAE. The PCA is an exploratory tool used in datasets to explore important features and patterns. It mainly aims to capture differences in the data through principal components. In this context, 1st principal component (PCA1) and 2nd principal component (PCA2) are the 2 leading principal components that explain the most significant number of variations in the healthcare data set. In the scatter plot, no distinct clustering of data points for the 3 countries was observed, suggesting that their healthcare data share similar characteristics concerning the identified principal components. Such overlapping means that perhaps there are minor variations in regional indicators, while the continuing fundamental healthcare statistics are similar across these countries. This suggests that the healthcare systems of the analyzed countries are structurally similar, facing comparable challenges and potentially benefiting from similar opportunities for advancement.
Within the framework of an equity-based approach to achieving financial sustainability in the healthcare system, this study emphasizes the importance of standardized measurement methods and coordinated efforts among the analyzed regions. Our findings hold important implications for policymakers as they can seek to foster cooperative solutions of shared concerns in the health system that support equity and sustainability. The PCA plot emphasized mutual goals that can improve healthcare outcomes in the analyzed region by developing a common framework.
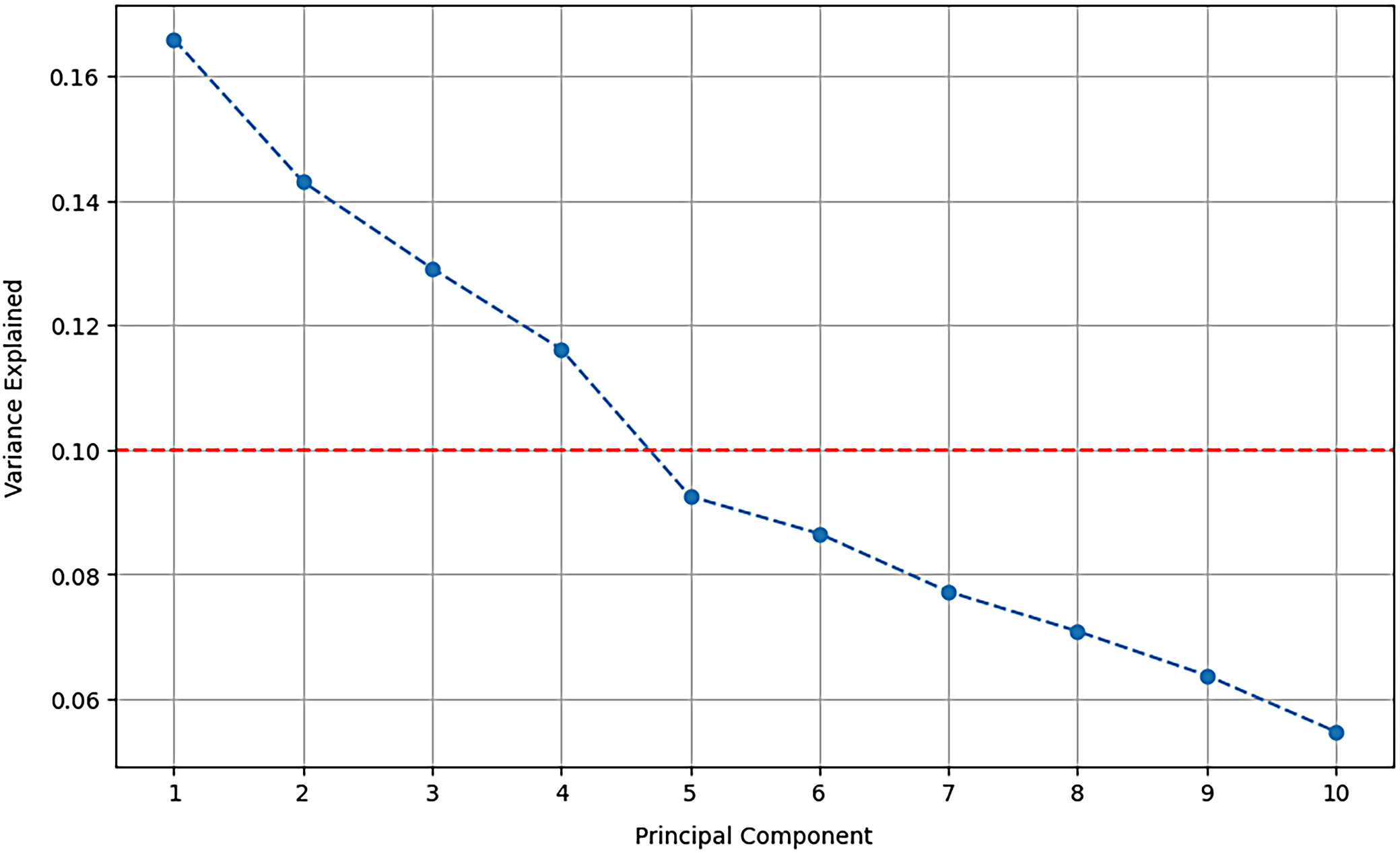
As illustrated in Figure 3, the application of PCA to healthcare data from Qatar, Saudi Arabia and the UAE demonstrates the validity of the data under an equity-based framework. This analysis establishes a sustainable equity framework for a financially resilient healthcare system in Arab countries. It seeks to reduce the complexity of the dataset while preserving the most significant variance among healthcare systems in these nations. This steep drop in the variance explained by the first few components means that PCA1 and PCA2 explain many variances. These components potentially highlight the significant financial and structural differences or similarities among the healthcare systems of Qatar, Saudi Arabia and the UAE. The screen plot suggests that no further variance is explained after the 3rd (or 4th) component since subsequent components do not provide any new information. This analysis provides policymakers with a means to focus on the key components (aspects) that affect healthcare sustainability and equity in these countries. It enables a narrower focus on financial planning, addressing the most contrasting features that set apart the healthcare systems.
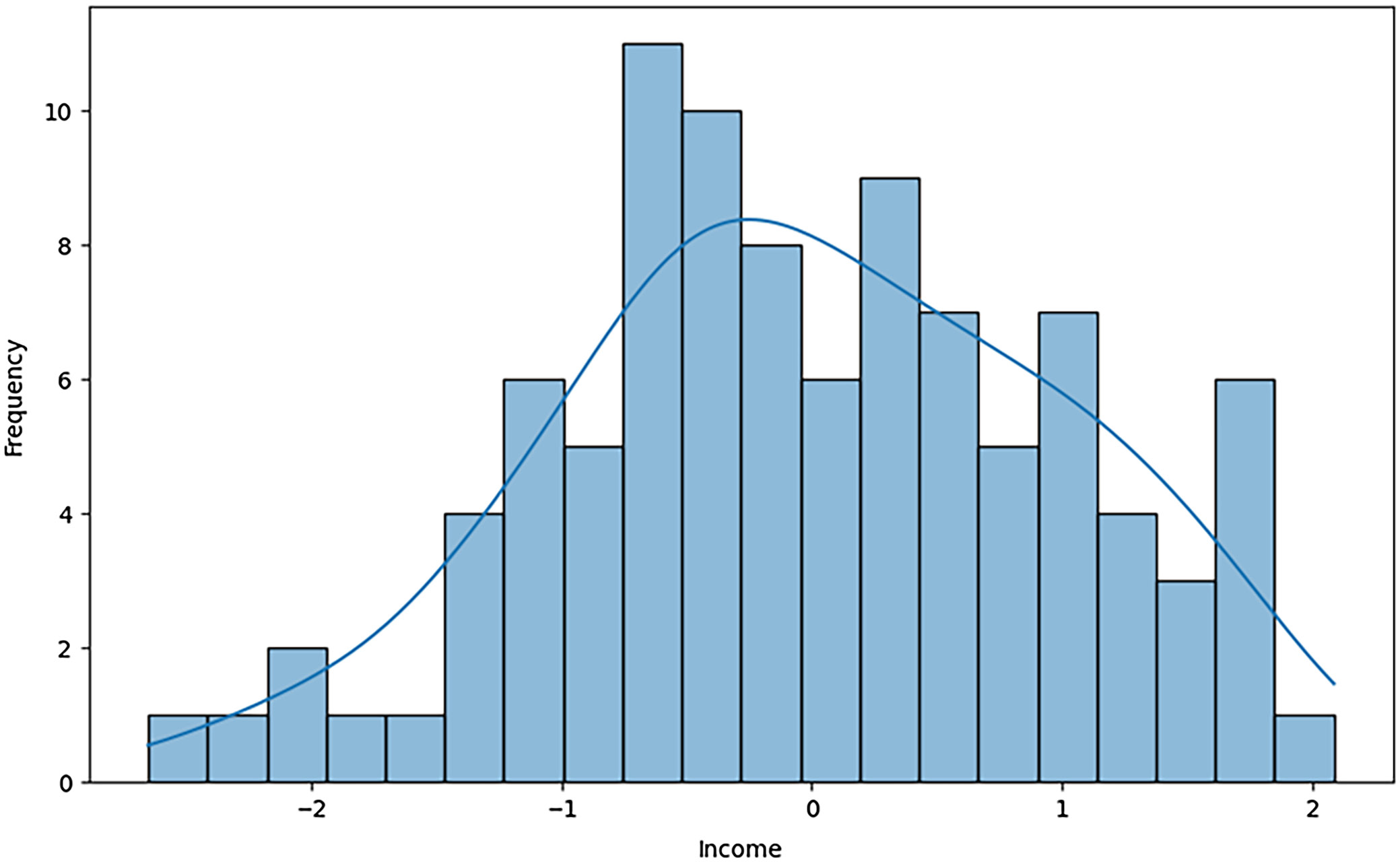
The histogram and the density curve of income are used in Figure 4 to create equity using the Theil index measurement of equity. The Theil index was then computed to assess a population’s income level as it is more sensitive to inequality. The histogram shows that it is relatively customarily distributed but skewed towards the lower end of the income scale. This means that more people earn less income than the sample average. It has a relatively higher proportion of people with an income almost equal to means (0), and as the income increases or decreases, the probability reduces. This means that income inequality is moderate because a relatively large proportion of the population now earns below the median.
The density curve also aids in smoothing out some of the harsh features in the histogram to present the overall picture of the distribution of incomes. The curve density is dense around the mean income, where many people earn close to the mean income. The curve’s tails represent a small fraction of individuals earning significantly more or less than the rest of the population, effectively illustrating income disparity. From a significance perspective, this distribution suggests that while many individuals earn slightly above or below the average income, there remains a substantial income gap, with some individuals classified as either very high-income or low-income earners.
In this case, the skewness indicates that policies towards reducing income disparities may consider how to “upscale” the low end of the distribution. This analysis also highlights the importance of creating better and equitable economic policies to help facilitate the closure of income differentials. Therefore, utilizing the Theil index provides valuable insights into income distribution and its implications, enabling policymakers to take necessary measures to promote economic balance and fairness.
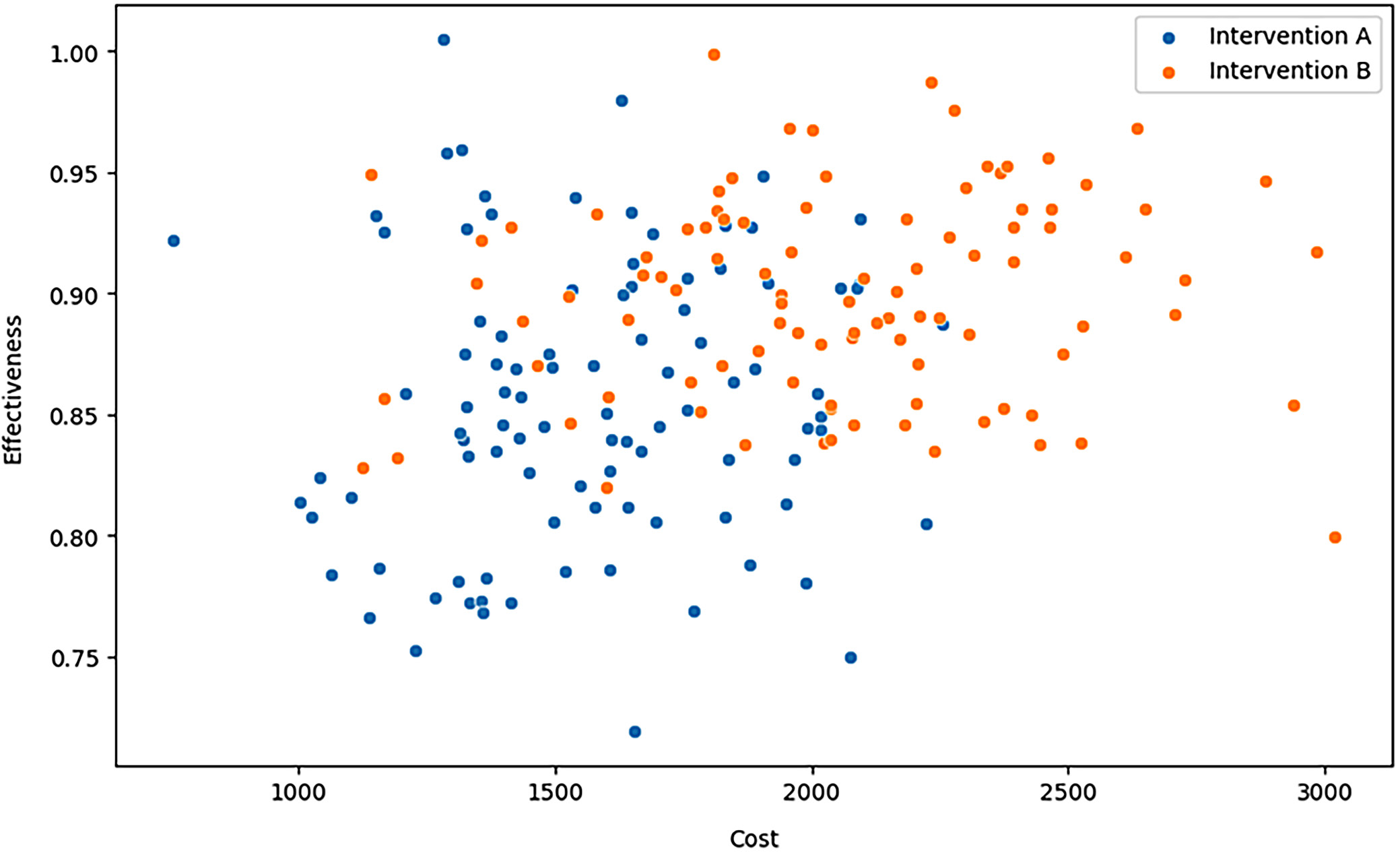
Figure 5 compares the cost and effectiveness of Intervention A and Intervention B. Every dot corresponds to the cost and the efficiency of an instance of the interventions. Blue and orange dots depict Intervention A and Intervention B, respectively. The scatter plot indicates that, in most cases, the cost of the intervention and its effectiveness can be considered proportional, where higher costs are associated with greater effectiveness. However, Intervention B is more effective than Intervention A and is offered at a similar or slightly higher cost. For example, at a cost of around $2,000, the effectiveness of Intervention B varies between 0.85 and 0.95, while the efficacy of Intervention A falls within the bracket of 0.85 and 0.90.
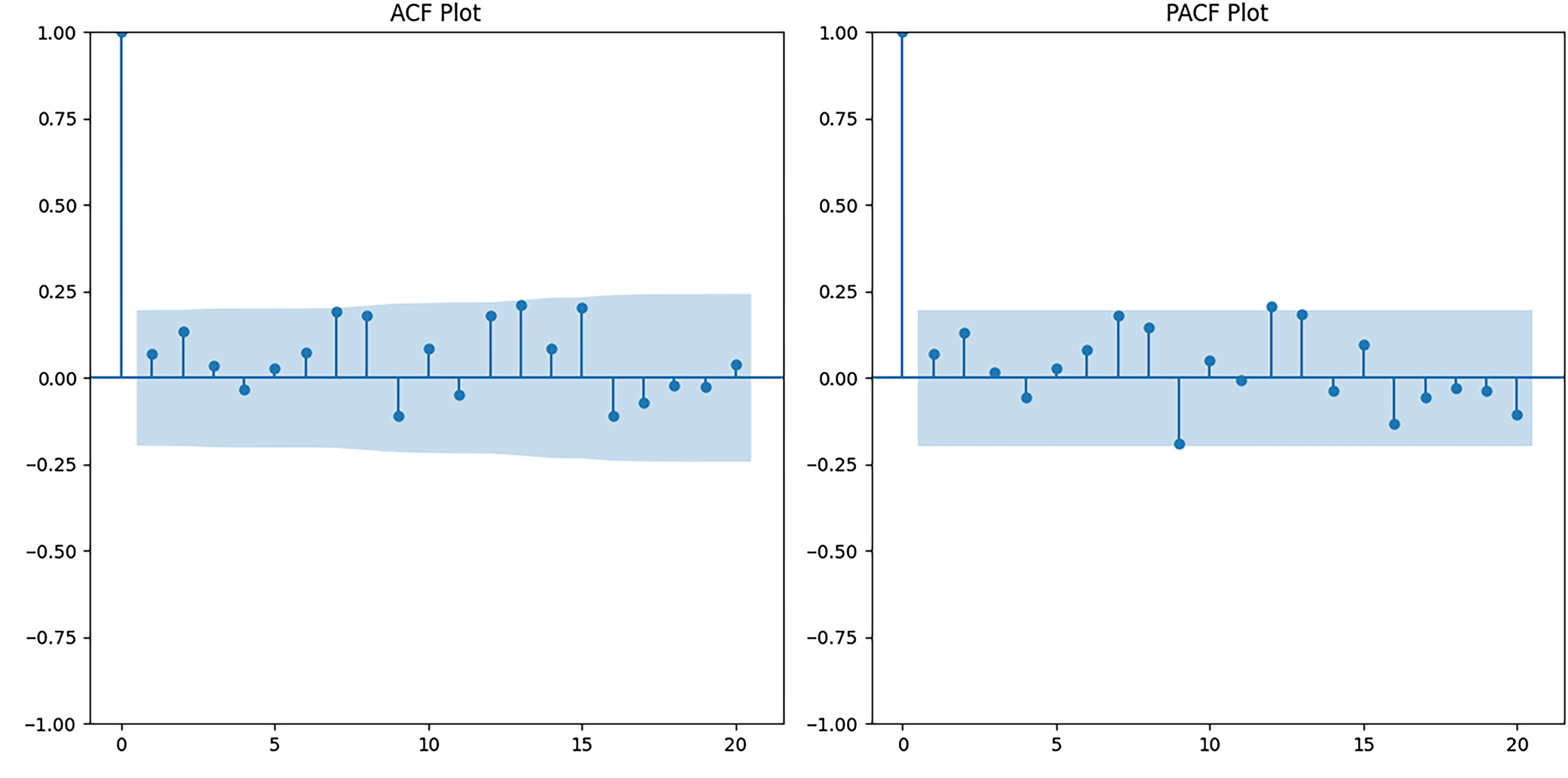
This analysis is essential as it provides a detailed presentation of the trade-off between cost and outcomes for various healthcare interventions. Plotting the data reveals that while both types of intervention are equally helpful, Intervention B may yield even slightly superior results at a somewhat higher expense, potentially making it more beneficial for achieving the most excellent utility from available healthcare resources. Decision-makers can then adopt this information to consider spending on the most effective interventions, improving the value of healthcare dollars. The ACF and PACF plots in Figure 6 help analyze time series data of healthcare spending, costs or outcomes over time in the context of the study: “An equity-based financial framework for a sustainable healthcare system in Arab countries”. The ACF plot reveals a strong correlation between the current period and previous periods, indicating that recent healthcare investments or policy changes have a significant impact on subsequent periods. For instance, an increase in funding or the implementation of a reform in one year may directly influence healthcare outcomes within the same year. The PACF plot suggests that past data have a diminishing influence beyond the 1st lag, indicating that the predictability of the healthcare system’s financial framework is primarily short-term rather than long-term. This implies that short-term interventions or changes in healthcare financing may yield more immediate effects than long-term reforms. These insights can assist policymakers in Arab countries in designing responsive financial frameworks that prioritize short-term outcomes while working toward building resilient and sustainable healthcare systems.
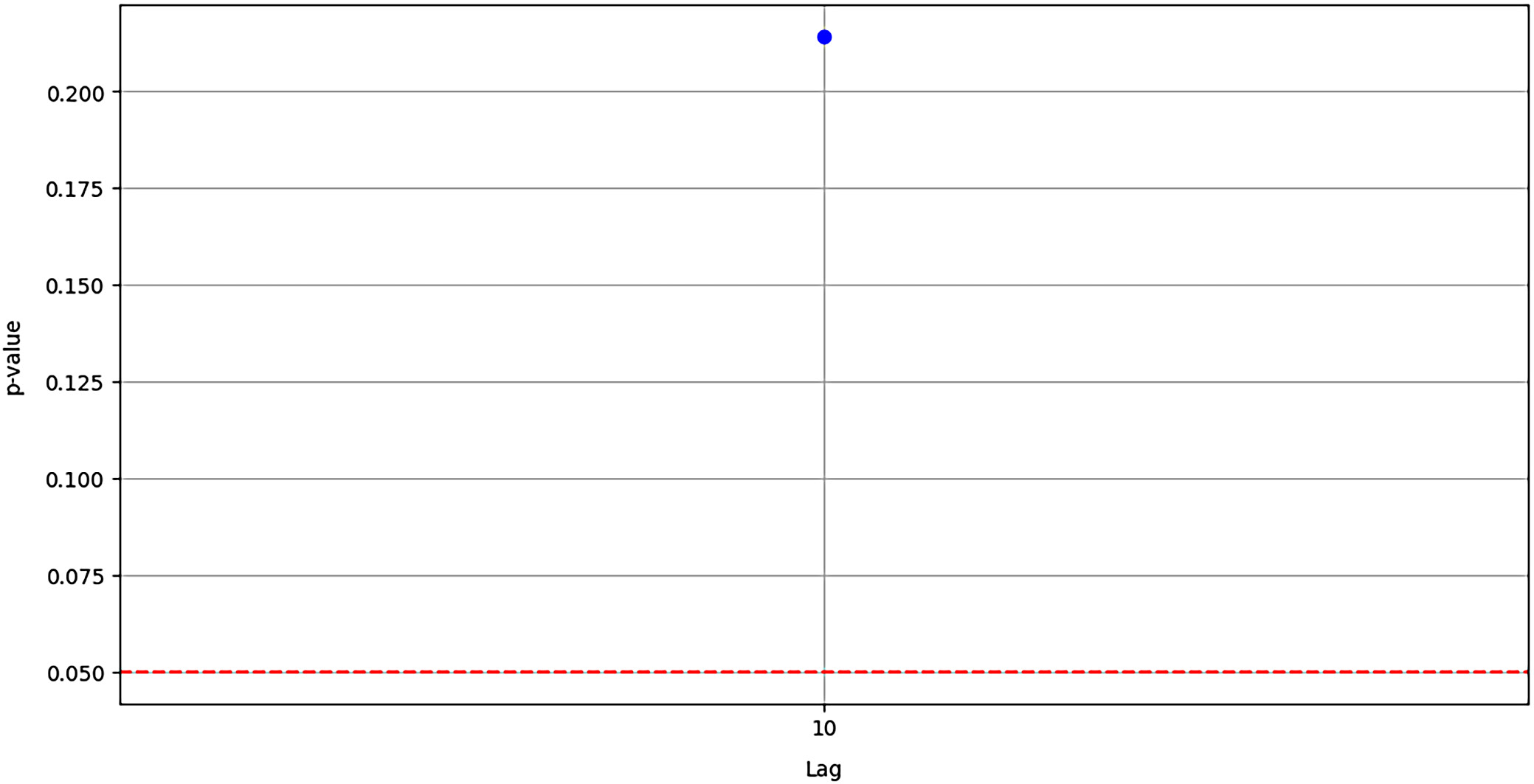
Figure 7 demonstrates the p-values from the Ljung–Box test against time series at different lags in the lower part of the graph. The Ljung–Box test is concerned with whether any of the autocorrelations of the residuals of a time series model are significantly different from 0. The horizontal bars of the graphs portray the lags, usually expressed as the number of periods measured backward in the time series. In contrast, the vertical bars indicate how statistically acceptable (or significant) a given value associated with the test is. The red dashed line here shows 0.05, which is considered the maximum for significant p-values depending on the number of lags. The plot shows that the p-values exceed 0.05 for all lags; therefore, there is no indication that the model’s residuals exhibit significant autocorrelation, even when lagged 10 times. The most positive p-value approximately at the blue dot is at lag 10, which is slightly more than 0.20, thus imposing no case for regression at this point. There is a lack of significant p-values from all lags, suggesting that the residuals look like white noise, which means that the model can adequately explain the data structure. This result enhances the credibility of this model when it is used to make predictions or make any other assumption. In summary, the model’s performance is robust and can be relied upon for accurate predictions.
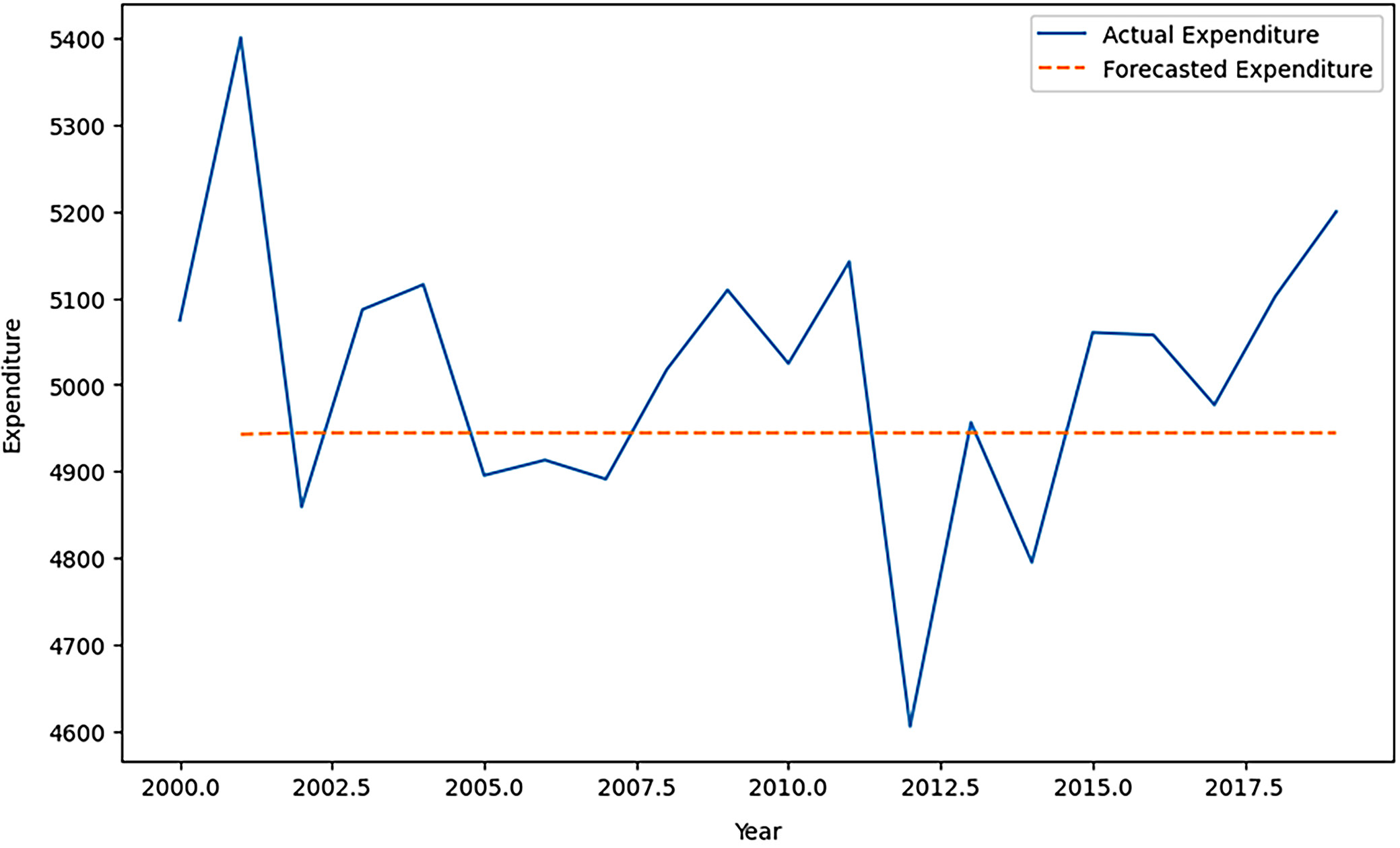
Figure 8 depicts the forecasted expenditures for healthcare, generated using ARIMA, alongside the fundamental values of healthcare expenditure for the same period. The x-axis represents the years from 2000 to 2020, while the y-axis denotes healthcare spending for each corresponding year. The ARIMA model forecasts a constant flat line for healthcare expenditure. This can indicate a lack of seasonality or trend in spending on healthcare, which is supported by the visualization of real values of healthcare expenditures. The real values do not exhibit any clear trends, and since annual data are used, there is minimal-to-no seasonality observed. Additionally, the real values do not exhibit cyclicality, as evidenced by the absence of such patterns in the graph. Consequently, the random walk model is likely the most accurate approach for forecasting.
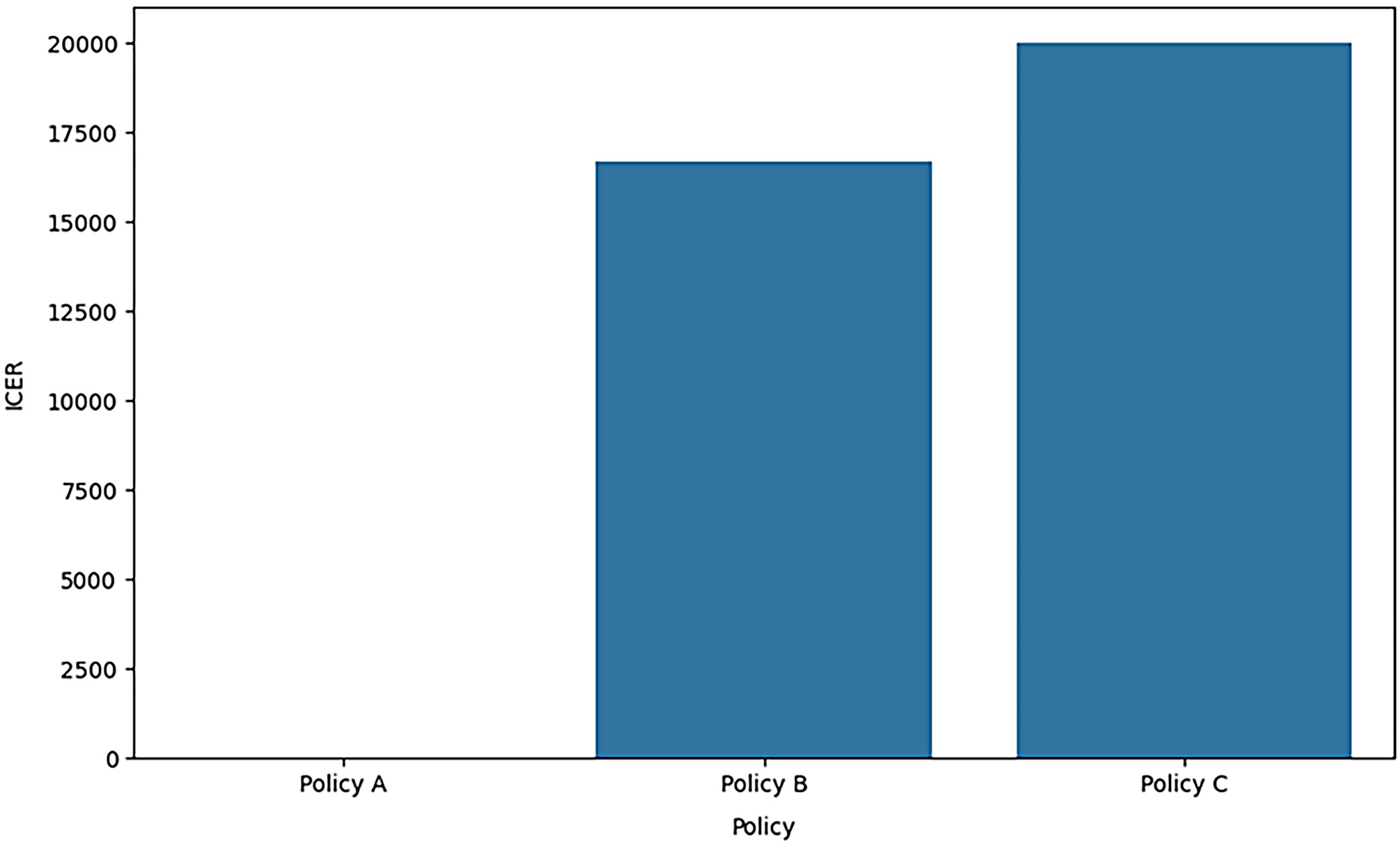
Figure 9 illustrates the ICER for different policies from the study “An Equity-Based Financial Framework for a Sustainable Healthcare System.” The figure compares the ICER of 3 existing health policies, Policy A, Policy B and Policy C, which serve as key measures in health economics for assessing the cost-effectiveness of various health interventions. It means the added cost of 1 more unit of health improvement, e.g., quality-adjusted life years of the new intervention over the current standard treatment.
In the same context concerning the figure, it is observed that Policy C has the highest ICER, followed by Policy B and then Policy A, meaning that Policy C may yield better health outcomes. Still, it is the most expensive in terms of those benefits. Policy A, which has the lowest ICER, is cost-effective compared to the other 2 quantities. The importance of this analysis comes from the fact that it can aid policy decision-makers in knowing which policies are worth the investment to get the maximum level of health in the population. Policy C had the highest ICER, suggesting it may need to be more cost-effective as it should provide more value for the cost incurred to implement such a policy. On the other hand, Policy A has a lower ICER than Policy B, which means there are optimal balance costs and benefits, making it a preferable model for sustainable health financing.
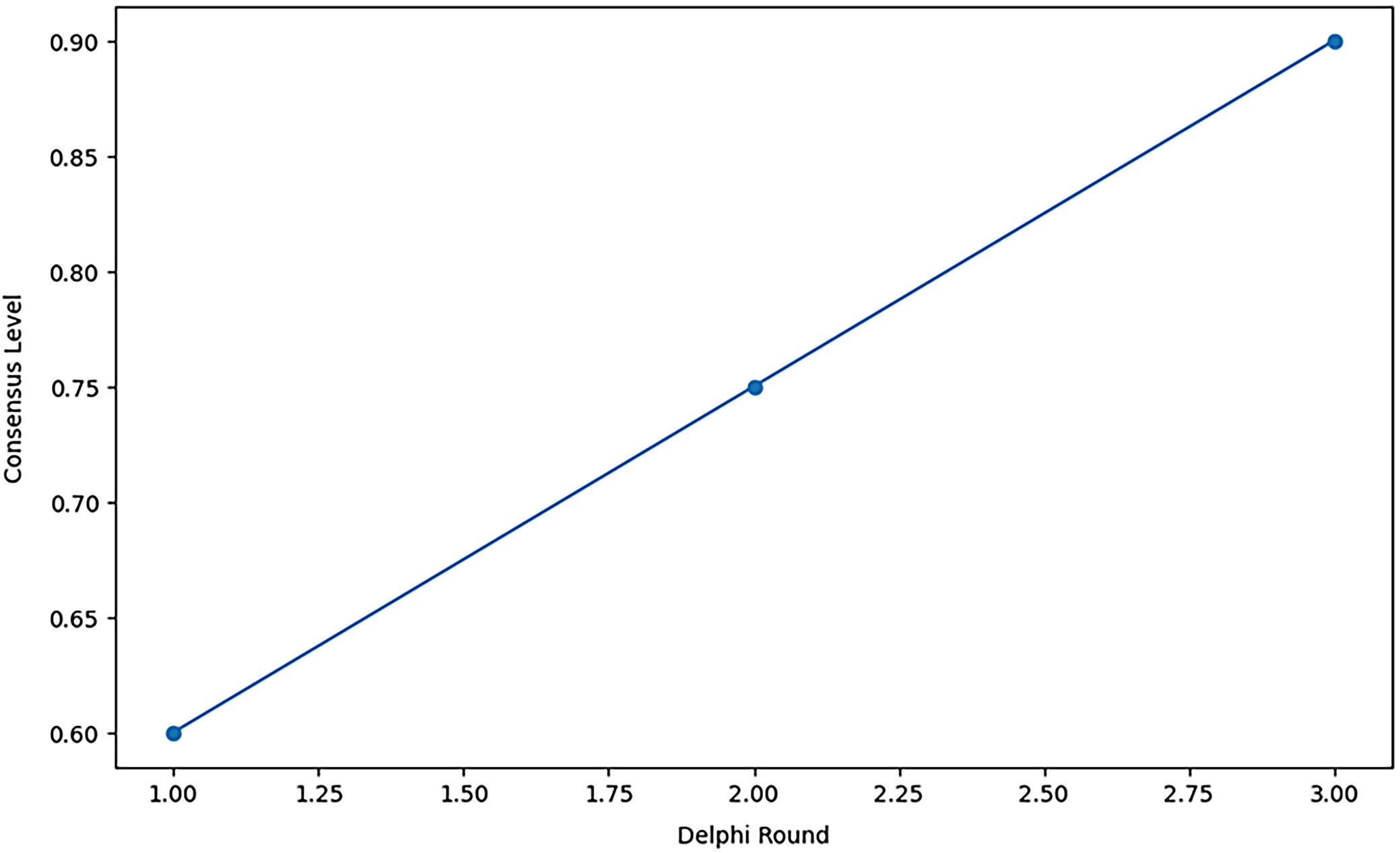
Figure 10 shows the “Delphi technique consensus over rounds,” which shows the consensus trend achieved by the expert panel across 3 survey rounds. The Delphi technique is an interactive method of reaching a consensus, which involves completing several sequential questionnaires. The figure thus depicts an upward trend, suggesting that the consensus level locally gets higher in the 3 rounds. It starts from a consensus level of 0.60 in the 1st round, increases to about 0.75 in the 2nd round and approximates to 0.90 in the 3rd round. This gradual trend demonstrates that the cyclical feedback mechanism inherent in the Delphi method strengthens and synchronizes offenders’ perspectives, which causes a high consensus over time.
In this study’s context, this increasing consensus further underlines the reliability of the Delphi technique for reaching a consensus among diverse experts on the financial framework for sustainable healthcare. This is essential because stakeholder engagement through a systematic approach can yield well-rounded and broadly supported policy solutions. The high consensus level in the last round means that the final framework was derived from various opinions. It is more likely to serve its purpose and be sustainable when implemented.
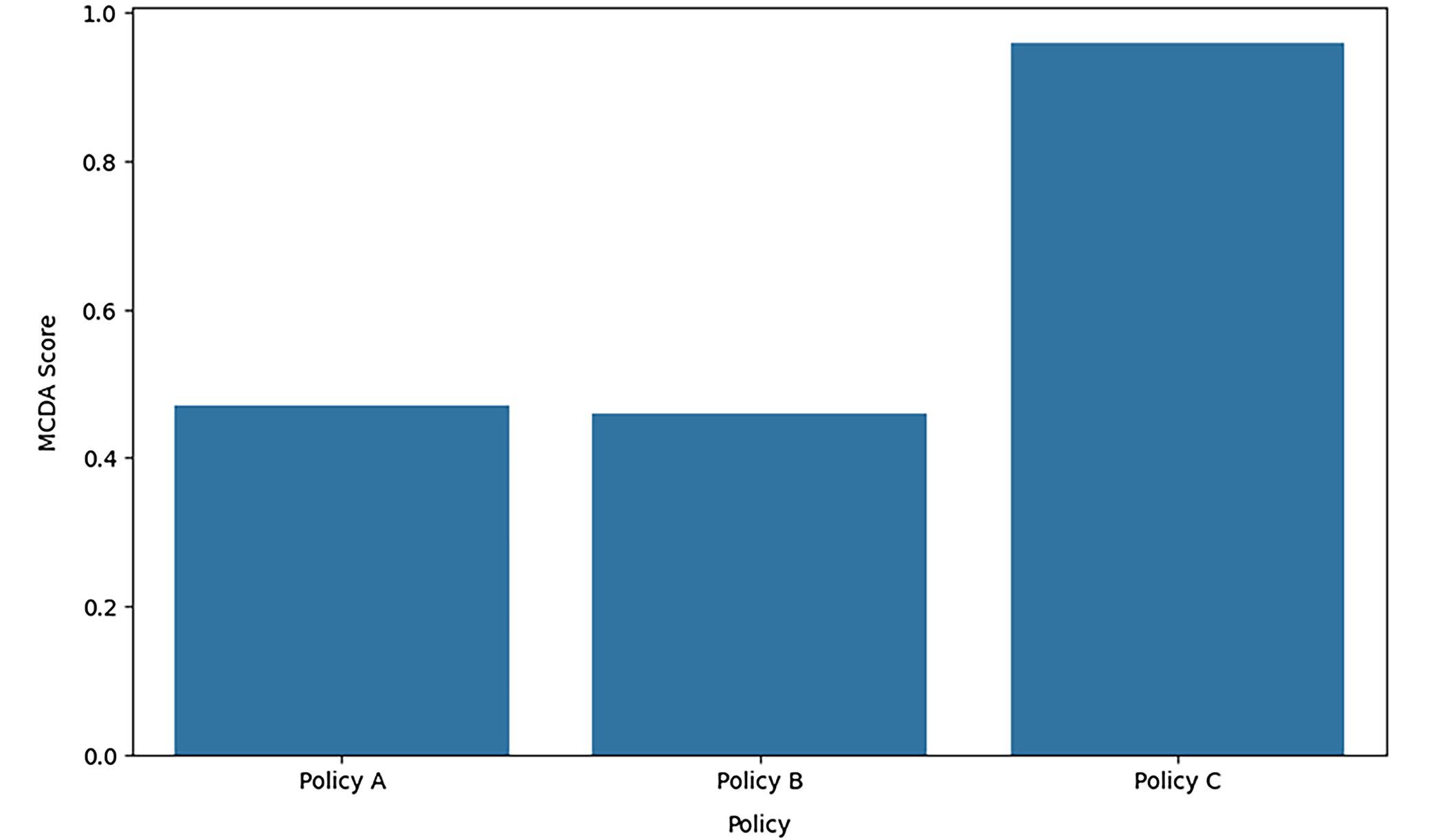
Figure 11 illustrates the MCDA scores for 3 different policies: A, B and C. Indeed, the chart “MCDA scores for different policies” provides an MCDA comparison of various policies about several criteria, which could be assumed to pertain to an equity-based financial framework for the sustainable healthcare system. Policy C is the best-performing policy according to the score closest to 1 and significantly outperforms Policies A and B. This implies that Policy C is the most preferred policy based on the adopted MCDA sets of criteria. Policies A and B have similar and lower values close to 0.5, suggesting a similar but lower level of performance. The importance of this figure is in ensuring that consumers can make an impartial comparison of the policies. Stakeholders can, therefore, quickly determine whether one policy is better than the other in achieving the goal of equity and a more sustainable healthcare system framework. The conclusion that can be made based on the figure is that Policy C is the best option as it holds the greatest likelihood of realizing the set objectives.
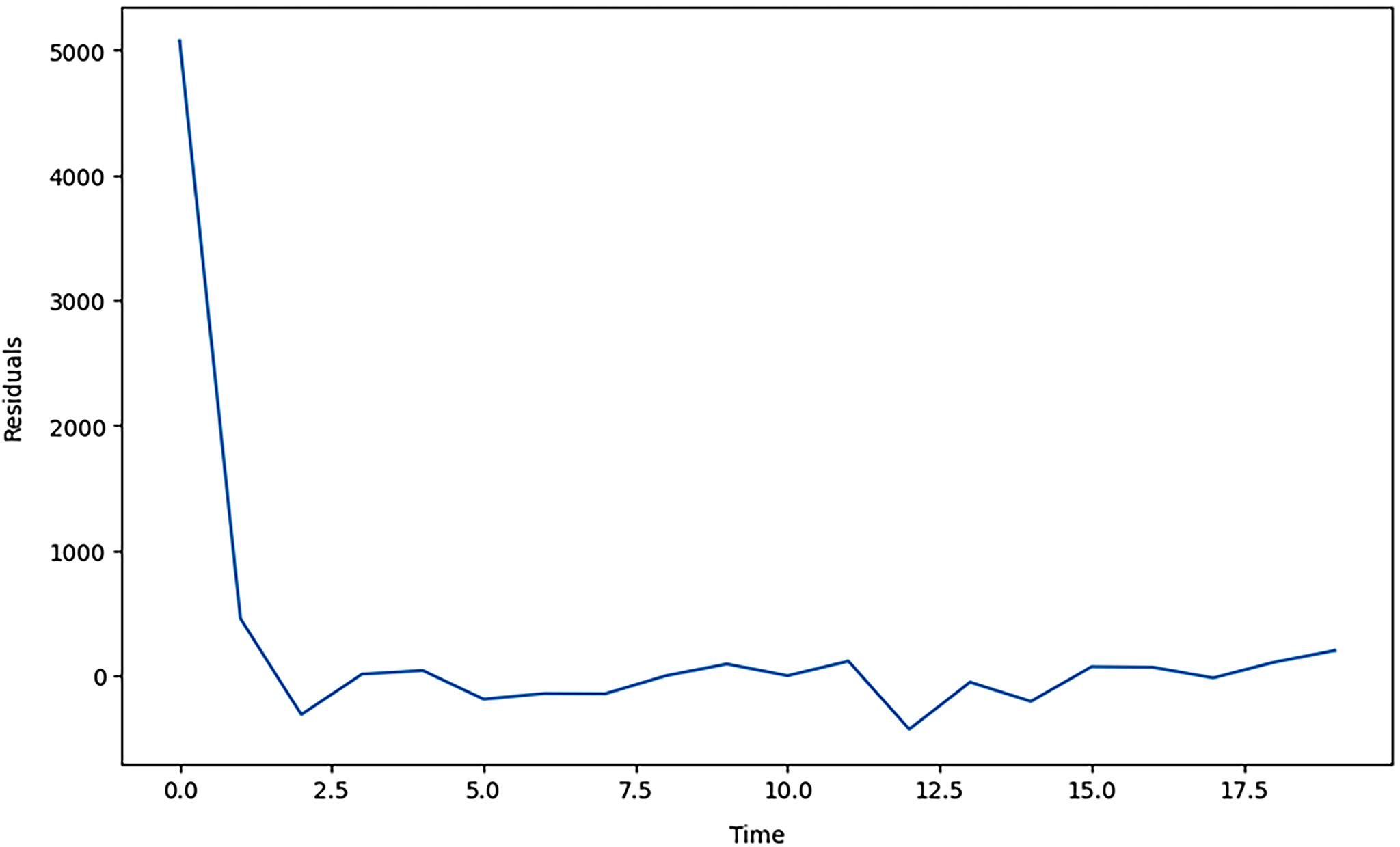
Figure 12 is the “Residuals of autoregressive integrated moving average (ARIMA) model.” The plotting factors show the residuals as a time series, where the residuals are calculated as the difference between the observed and the fitted values. First, the residuals are observed to be relatively large, with a maximum of over 5,000; however, they reduce sharply and oscillate around 0 periodically. This pattern suggests that after a certain period, the data-generating process is well captured by the ARIMA model. The high initial residuals imply that the model takes some time before stabilizing to fit the dataset. Over time, the residuals reach a pattern of randomness, thus suggesting that the model’s forecasts are improving and becoming more coherent. In essence, this figure is essential in verifying the reliability of the selected ARIMA model. The fluctuation of residuals around 0 indicates that the residual values are centered along the 0 line, suggesting that the model has accurately captured the data pattern and provides a good fit. The conclusion that can be derived from this analysis is that ARIMA is an effective forecasting model whose ability to predict accurately can be established from the residuals, which are low and constant after the initial adjustment period.
Discussion
The findings of this study on equity-based financial models for universal and sustainable healthcare systems in Arab countries can serve as applicable theoretical and practical guidelines for healthcare equity, financing and policymaking. The study reveals a multifaceted relationship between healthcare fairness and durability in the region.
The PCA results indicate a high degree of similarity between Qatar, Saudi Arabia and the UAE, aligning with previous studies that suggest the healthcare systems in the Gulf Cooperation Council (GCC) countries share common challenges and opportunities.24 Such overlapping may serve as a foundation for regional cooperation in addressing healthcare trends, stating that the need for common strategies in enhancing healthcare in Arab countries should be coordinated.24, 25, 26
The findings of the Theil index depicting incomes of different groups for income distribution indicate relatively low levels of inequality but more concentration of income in the lower end of the bell curve.27 This finding aligns with previous research on income distribution in the Middle East and North Africa (MENA) region, where income inequality has persisted at high levels despite economic growth.28 This pattern of income distribution underscores the need for policy measures to address economic disparities, which are widely recognized as contributing to adverse health outcomes and disparities in healthcare access and utilization.29 The comparison of Interventions A and B in the context of cost analysis has proven that CEA plays a significant role in managing and delivering healthcare.30 This increased cost per patient is still associated with better effectiveness of Intervention B, which is consistent with the literature calling for more comparative effectiveness research in using available resources efficiently in the healthcare system.31 This result aligns with the general direction towards the increased utilization of research findings in formulating health policies.32
The ICER analysis of policies A, B and C shows that evaluating healthcare policies is not straightforward. The conclusion is that Policy A has the lowest ICER, indicating that it is the most cost-effective option for implementing the identified policy while aligning with the overall objectives of the study. Moreover, the ICER analysis highlights the importance of considering both costs and outcomes in health policymaking to ensure efficient resource allocation and improved healthcare effectiveness.33 This approach to policy evaluation is relevant within the constraints of scarce resources in healthcare system and the drive to attain UHC in many Arab states.34
The results obtained using the Delphi technique, illustrated by the increasing level of consensus in the responses from participants over 3 rounds, support the applicability and effectiveness of the structured approach to stakeholder involvement in the development of healthcare policy.35 This finding is consistent with the literature pointing to the need for community engagement to develop context-responsive and long-term health policy solutions.36 Therefore, the 3rd-round results show a high degree of consensus concerning the proposed framework, and it can be assumed that the final framework will be supported by various stakeholders who are significant to the success of the implementation.
In addition, the MCDA scores of various policies present an extensive assessment model encompassing numerous criteria. Policy C has demonstrated superior performance in this assessment, emphasizing the effectiveness of MCDA in multi-criteria decision-making within healthcare policymaking, as observed in earlier studies.37 This enables the consideration of policy impacts in a way that goes beyond mere cost-benefit and efficiency calculations and encompasses social and ethical concerns.
Regarding the evaluation of the framework’s performance under different economic conditions and policy shifts, a comparative analysis was carried out to identify the framework’s applicability and resilience. The impact of different financial conditions, such as economic growth, recession and inflation, on healthcare financing and resource mobilization was assessed using systems dynamics modeling.4 For example, in an economic downturn, lower revenues limit spending and require priorities such as public investment in basic infrastructure and social safety nets. Instead, economic growth can create conditions for service extension and investigation of various additional financing models, such as social impact bonds and government subsidizing for the permanent development of the service.10
Moreover, policy changes were evaluated using stochastic analysis to compare the variability of the impacts resulting from taxation alteration, healthcare subsidies and insurance premiums.5 The study illustrated that raising the tax revenue to finance healthcare enhanced equity and utilization but presented difficulties regarding the financial risk protection of the poorer sectors of society. On the other hand, extending healthcare subsidies led to improving UHC, but questions arose regarding financial feasibility issues, especially during the economic downturn.18 Based on these findings, it becomes clear that policy interventions should be adapted to changes in the economic environment to ensure that policies promoting equity do not compromise fiscal sustainability.
Therefore, this study’s findings help enrich knowledge about healthcare equity and sustainability issues in Arab countries. From economic evaluations to stakeholder engagement, the study offers a conceptual framework to develop a solution for the multifaceted problem of healthcare financing and equity. These findings validate the role of involving stakeholders to form evidence-based policies and reflect on the potential of regions to come up with united solutions to healthcare issues.
Proposed equity-based financial framework for the sustainable and equitable healthcare system
This research suggests the following equity-based financial framework, constructed around the fundamentals of the HEMF and visualized in Figure 13, for assisting Saudi Arabia in developing a sustainable and equitable healthcare system:
Diversified healthcare financing mechanisms
A diverse range of financing options should be utilized, incorporating government grants, business insurance and innovative methods such as social impact bonds and community bond plans. Moreover, healthcare financing needs to be structured to effectively tackle socioeconomic disparities and geographical variations in access to and consumption of healthcare services.
Resource allocation based on equity and need
The distribution of resources should be based on the population’s needs, considering factors such as population size, disease load and socioeconomic status. It is essential to prioritize resource allocation to underserved and rural areas to ensure that everyone has equitable access to healthcare. By doing so, we can address disparities in health outcomes and promote a more fair and just healthcare system for all individuals, regardless of their circumstances.
Targeted financial protection measures
Implementing UHC plans or subsidized healthcare services is essential for making healthcare accessible to low-income and marginalized groups. By doing so, we can ensure that essential healthcare services reach a broader segment of the population. Additionally, it is important to explore sliding-scale pricing and allowances, which can further enhance access to healthcare for those in need. These strategies work together to create a more equitable healthcare system that meets the needs of all individuals, regardless of their financial situation.
Intersectoral collaboration and policy integration
To create effective healthcare policies, it’s essential for healthcare officials, social welfare organizations, and other key stakeholders to collaborate closely. This collaboration will help in developing appropriate strategies that address the diverse needs of the community. Additionally, it is crucial to consider socioeconomic determinants of health, such as housing, education and employment, within the framework of broader healthcare financing plans. Addressing these factors is vital for ensuring holistic improvement in health outcomes and fostering a healthier society overall.
Population-specific interventions and culturally competent care
Gathering and analyzing de-identified data is essential for gaining a better understanding of the healthcare requirements and challenges faced by various demographic groups. By leveraging this information, specialized programs can be developed to address the educational, occupational and social needs of underserved communities. Additionally, it is vital for healthcare providers to receive training in patient-centered care techniques, cultural understanding and effective communication methods to enhance the overall quality of care and support these diverse populations.
Continuous monitoring, evaluation and quality improvement
The development of reliable data tracking and analysis tools is essential for measuring the success of healthcare financing strategies and equality measures. By utilizing these tools, organizations can regularly enhance healthcare equity results through informed modifications based on data-driven decision-making and evidence-based approaches. This continuous improvement ensures that healthcare systems can adapt and respond effectively to the evolving needs of the population, ultimately fostering greater equity and access to care.
Stakeholder engagement and community participation
Legislators, healthcare providers, patient advocates, and community leaders are all essential stakeholders in the planning and implementation of an equity-based financial aid system. Their involvement is crucial for the success of this initiative, which aims to address the diverse needs of the community. It is important to drive local participation and gauge the area’s sentiment to ensure that the plan effectively incorporates the community’s objectives and goals. By engaging these key stakeholders, the system can be designed to reflect the priorities and aspirations of those it intends to serve.
Equity-based financial framework for sustainable healthcare
This equity-based financial scheme, proposed to the authorities, aims to address the various factors contributing to healthcare disparities in the Arab region. It seeks to ensure equal access to healthcare for all citizens, regardless of socioeconomic status, geographic location or family history, ultimately improving health outcomes across the population. This framework outlines the implementation strategy that promotes sustainability goals, reduces health inequalities and creates a healthcare system that satisfies the various needs of Arabs.
Practical implications of the study
The study recommendations for policymakers include implementing evidence-based primary healthcare equity initiatives for each Arab country. This entails employing PCA to ascertain factors that need policy reforms to reduce healthcare disparities. Another measure that policymakers should use is the Theil index, which measures disparities concerning income with a view of directing resources towards the less privileged groups. Therefore, the study indicated that equity-based financial frameworks should be used to improve people’s health outcomes because they eliminate inequalities in the distribution of resources. Policymakers should seek active interaction with relevant stakeholders and use the Delphi technique to enhance and mutually define policies.
Second, it is vital to develop ways of updating and reviewing the healthcare equity data routinely to fit in the ever-shifting socioeconomic framework. These steps will ensure that the policies to be implemented are informed by research and are specific and appropriate for the long-term change desired in the region’s healthcare system.
The most pressing challenge to implementing the framework in healthcare within the analyzed regions is the lack of sufficiently skilled healthcare workers. Unfortunately, there is no clear-cut solution for resolving healthcare shortages.38
Healthcare labor can be increased in the short run by raising the wage rates. However, this temporary and unsustainable solution only incentivizes retired and foreign healthcare workers to enter the labor market. Longer-term healthcare labor markets face substantial time lags when reacting to labor shortages due to the long training period needed. Additionally, regulatory constraints and other barriers to entry restrict the number of licensed healthcare professionals. However, loosening regulations is not advisable, as they play a crucial role in maintaining the quality of healthcare services and ensuring standardized care across the system. Therefore, addressing the healthcare labor shortage requires more than just wage adjustments.39
While raising the retirement age for healthcare workers and incentivizing the migration of foreign healthcare professionals can help mitigate short-term labor shortages, bolstering the domestic healthcare workforce will be essential for ensuring the long-term sustainability of the healthcare sector.39
The proposed framework can provide a foundation for identifying the needs of heterogeneous regions. Governments should collaborate with regional stakeholders to comprehensively understand the financial and non-financial factors affecting the healthcare labor supply.
Expanding the number of seats in medical and nursing schools is a valuable policy initiative to consider. Additionally, integrating technological advancements, a trend already being adopted by many Gulf countries, can help alleviate the burden on healthcare workers and enhance efficiency in healthcare delivery.
Limitations
It should be noted that this study has several limitations. The emphasis placed on Arab countries may mandate caution when generalizing the conclusions to other areas of the world. The use of available data may have introduced biases or gaps within the datasets, potentially affecting the accuracy and completeness of the analysis. One of the key limitations of this research is its cross-sectional design, which does not capture temporal effects, making it impossible to establish trends or determine causality. Finally, the rapidly evolving healthcare systems and the changing socioeconomic dynamics of the studied area may impact the long-term relevance of the proposed framework. Future research should strive to use longitudinal designs to assess the effects of healthcare equity policies, with the potential to encourage significant changes in the field. By comparing countries or regions, we can reveal common trends and irregularities, exploding a sense of shared purpose in achieving equal access to healthcare services. To gain a deeper understanding of the mechanisms driving inequity, future studies should incorporate more detailed socioeconomic characteristics, offering a more comprehensive perspective on the issue. Moreover, future research should also analyze the outcomes of identified specific prevention and treatment measures developed through PCA and the Theil index methods, offering practical insights for policy implementation. These insights could transform the way we approach healthcare equity. Lastly, refining the Delphi technique could improve consensus-building efforts, fostering collaboration among healthcare stakeholders and facilitating decision-making in many different challenging environments.
Conclusions
The contributions of our research are summarized as follows: A survey of Arab countries and their healthcare sector was conducted, which revealed significant deficiencies. A novel framework was presented to address healthcare disparities by integrating equity with innovative financing methods. A comprehensive quantitative approach was presented, incorporating culturally sensitive care interventions, continuous assessment, and support.
This study designed an equity-based financial model to harness sustainable healthcare systems in Arab countries using different analytical tools to solve healthcare equity, financing and policy formulation. The PCA established a significant correlation in the healthcare data of Qatar, Saudi Arabia and the UAE, indicating the similarity of healthcare systems in geographical regions. The analysis of income distribution using the Theil index indicated moderate income inequality, with household incomes skewed toward lower levels. The ICER analysis indicated that Policy A was the most cost-effective among the 3 policies studied. The Delphi technique obtained a satisfactory consensus of 0.90 in the 3rd round with relatively high stakeholder consensus. Lastly, the MCDA analysis revealed that Policy C was the most efficient among the 3 options, achieving the highest score, closer to 1 than Policies A and B.
The study provides a comprehensive framework that integrates various analytical approaches, ranging from economic evaluations to stakeholder engagement strategies. This research is crucial for gaining a holistic understanding of the healthcare landscape in the region and identifying opportunities for enhanced collaboration and policy development. By utilizing diverse methods, the study can close the gap between theory and policy regarding healthcare financing and equity and strengthen the existing literature as the basis for future theoretical and policy work.
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Consent for publication
Not applicable.
Use of AI and AI-assisted technologies
Not applicable.