Abstract
Background. The number and diversity of published peer-reviewed studies in the discipline of laser dentistry have grown considerably during the past 10 years.
Objectives. Within primary research, the development of protocols to guide and formulate clinical practice demands precision and ease of reproducibility. Errors in data acquisition and management may become amplified as the applied randomized clinical trials (RCTs) forge new levels of clinical diversity and predictability in the use of laser photonic energy in both ablative (surgical) and sub-ablative (photobiomodulation (PBM) or photodynamic therapy (PDT)) applications.
Materials and methods. A comprehensive range of empirical and computational operating parameters must be included in published studies to facilitate the uniformity of power- and time-related values of laser irradiation.
Results. Choosing the correct “tissue irradiation parameters” is difficult and depends on the pathology and symptoms, the surface area to be treated, laser wavelength, the thermal relaxation time of each targeted tissue, and controlling penetration depth of the light into tissues. Therefore, to allow the reproducibility of the results, it is recommended that authors mention with the greatest care and clarity the irradiation parameters used in their study.
Conclusions. This paper outlines the concerns felt regarding the general shortfalls and proposes a minimum range of laser operating parameters that should be represented in future peer-reviewed publications.
Key words: dentistry, laser, operating parameter, photobiomodulation, surgery
Background
Laser use in the disciplines of clinical dentistry, oral surgery and oral medicine has developed over a period of more than 30 years. During this time, from a rudimentary base of non-awareness of the scientific processes involved and the scope of possible applications, the knowledge and understanding of lasers have grown and benefitted from structured research, postgraduate courses and qualifications. Both the sophistication and scope of using laser photonic energy have increased significantly, to the extent that lasers can be incorporated to benefit almost all areas of patient-centered clinical dentistry.
Research into laser-assisted therapies has reinforced the importance of “tissue irradiation parameters” to maximize the benefits of applied coherent, monochromatic light energy to a given procedure while minimizing the risk of conversion of excessive energy into heat and consequent collateral thermal damage.
However, broad scrutiny of peer-reviewed published studies and reviews has highlighted the range of disparity when examining the combination of applied laser techniques and the amount of photonic energy delivered. The latter may be viewed as either photon density delivered to complete the chosen clinical procedure or the energy applied over a chosen timeframe as part of the tissue healing phase. Collectively, this may be considered as the “light dose”, representing energy density (also known as fluence or radiant exposure) or power density (also known as irradiation).
Collectively, it may be argued that this disparity has contributed to confusion as to the effectiveness and benefits of adjunctive laser therapy. Additionally, the inconsistent nature of outcomes has resulted in the leading opinions of representative bodies as to the unsuitability of laser-assisted clinical therapy, which has been further compounded by the lack of clarity regarding the optimal dosage and frequency of laser therapy. It is notable that 2 periodontal and endodontic representative organizations have issued a series of position papers on the subject.1, 2
An example of the uncertainty as to the success of lasers in dentistry was published in the 1991 paper by Zakariasen and Dederich,3 who summarized in the article abstract as follows:
“Laser dentistry must be developed through extensive scientific inquiry – as all of our treatment modalities should be. We, as a profession, must insist that such laser development is done properly, not foisted upon us based on anecdotal reports and incomplete research.”
Central to the overall progress of evidence-based research should be clear and disciplined adherence to the principles of probity and reproducibility of the published studies. A common failing is amplified through the predominance of incomplete systematic reviews wherein so often, the concluding statement is “more studies are needed”.
The use of lasers in clinical dentistry represents a highly complex form of irradiation, with anisotropic hard and soft oral and dental structures in close proximity to non-target sites. The key to successful and efficient laser use, whether surgical or non-surgical, is to achieve optimal target absorption with an adequate “light dose” to support the treatment objective. Therefore, the fundamental issue in the safe delivery of laser photonics remains the adoption of the acronym MIMO – minimum input to achieve maximum outcome.
Objectives
Laser therapies are effective, and their benefits are based on the principle of inducing a biological response through energy transfer.4, 5 This applies to both surgical (ablative) therapy and sub-ablative photobiomodulation (PBM) or antimicrobial photodynamic therapy (aPDT).
Selecting the optimal “tissue irradiation parameters” is a challenging task. The choice is influenced by several factors, including the pathology and symptoms, the surface area to be treated, the laser wavelength, the thermal relaxation time of each targeted tissue, and the depth of light penetration into the tissues.6, 7
Additional factors related to irradiation parameters may be viewed as:
– “Single, instantaneous” dose;
– “Cumulative” dose – repetition of single dose events over time/gated – continuous wave (CW) or free-running pulsed (FRP) emission mode [Hz];
– 2-dimensional dose: fluence/energy density/radiant exposure [J/cm2];
– 2-dimensional dose: Power density – irradiance [W/cm2];
– 3-dimension (volume) dose: fluence/energy density/radiant exposure [J/cm3];
– 3-dimensional dose: power density – irradiation [W/cm3];
– Total energy delivered [J].
The consequence of such appreciation is to enable the chosen laser parameters to be employed, and to avoid the disadvantage of excessive and possibly deleterious thermal increases and resultant collateral tissue damage.
Whether the intended use of a laser is diagnostics, sub-ablative PBM/aPDT or supra-ablative target tissue manipulation, 3 essential elements require careful consideration:
(1) the correct or appropriate laser wavelength;
(2) the correct or appropriate light delivery parameters, and
(3) the appropriate thermal relaxation process management.
However, the parameters selected will represent the mainstay of competency on the part of clinicians.8 Failure to observe such parameters may result in unwanted and damaging collateral thermal rises, but also a change in the optical properties of the target tissue that may indeed alter the optimal desired laser–tissue interaction. A common characteristic of many studies to research further the phenomenon of laser-assisted uneventful healing has highlighted the lack of availability of full laser operating parameters. Additional errors amounting to significant power losses along optic delivery fibers may compromise study validity.9 This contributes to imprecise replication of the treatment modality and protocol, with an attendant risk of patient harm or limitation of the effectiveness of the applied treatment. Thus, the use of a power meter to calibrate the delivered laser beam seems essential for future research study publications.
Discussion
A further consideration is the delivery of PBM therapy to pathology located below the surface. Fortunately, within the confines of the oral and maxillofacial regions, the maximum depth from any surface – skin or intraoral mucosa – is in the region of 10 mm (1.0 cm). The applied surface dose must be computed to account for 2 basic variables, the applied wavelength and the optical properties of the overlying tissue. In addition, the nature of the therapy required (biostimulation/analgesia/bioinhibition) must be taken into account.5, 10 This is summarized in Table 1.
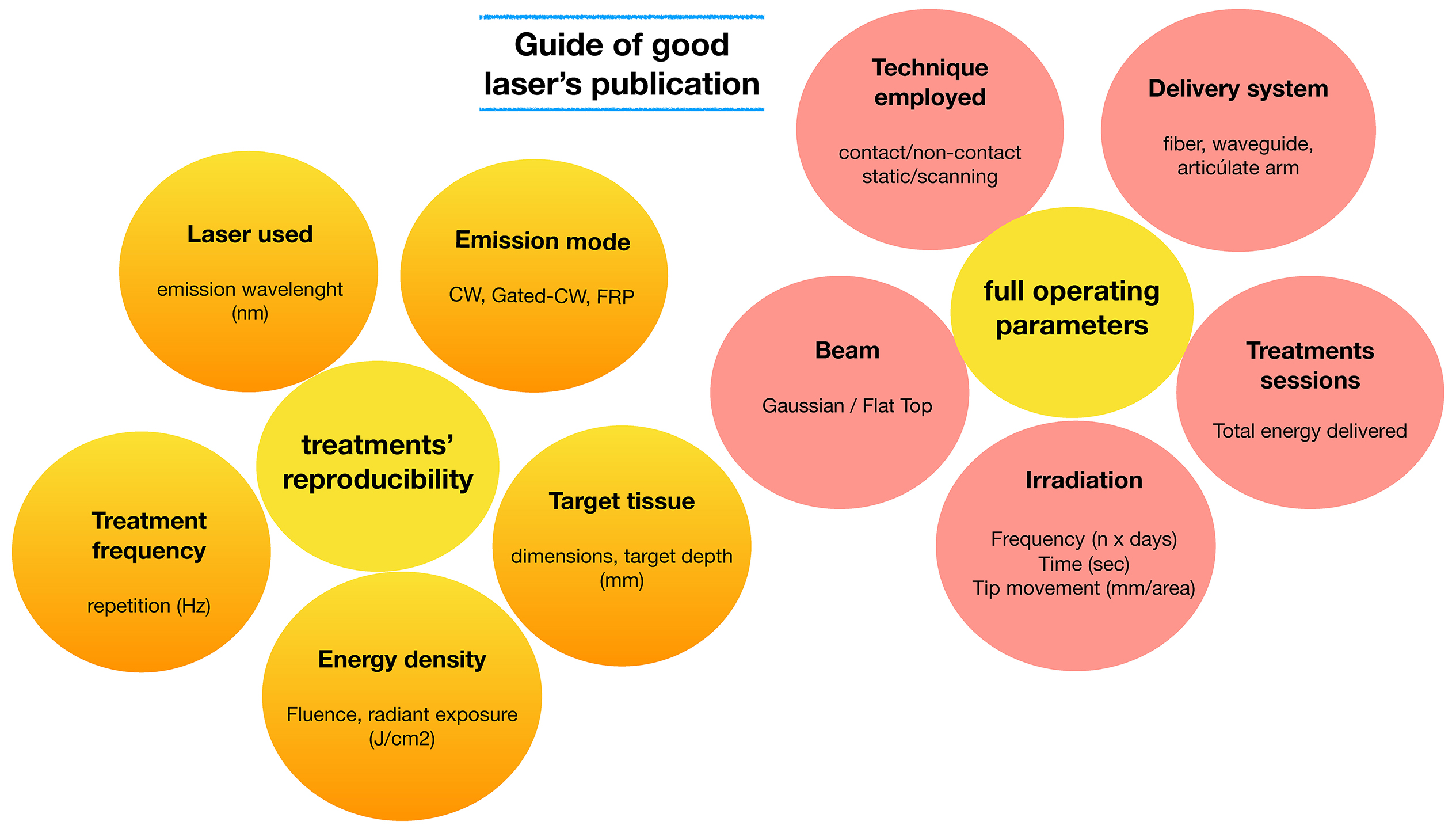
Incomplete materials and methods and the specific lack of a record of using a power meter to confirm the delivered laser photonic dose (relative to the control panel values) are very important considerations. A series of recent systematic reviews have highlighted the absence of comprehensive operating parameters and laser-tissue interaction data. It is proposed that these deficiencies have contributed to a distorted evaluation of lasers as an evidence-based adjunctive instrument. Therefore, to allow the reproducibility of the results, it is recommended that the authors mention with the greatest care and clarity the irradiation parameters used in the study: effective output power delivered [W], energy [J], beam diameter at the target tissue [cm], energy density [J/cm2], pulse duration [s], repetitive rate of pulses per second [Hz], the total irradiation time [s], contact or non-contact mode, distance from the tip to the target, the angle of beam divergence when using a fiber [°], the beam diameter at the focal point in cases using beam focalization from an articulated delivery system, and the treated surface area [cm2]. In case of repetition of the same procedure, clear enumeration of the number of sessions per week and the total number of sessions is essential. This is summarized in Table 2. The recording of full operating parameters relative to the anatomical location will seek to readdress the challenge of study reproducibility and assist in the harmonization of the laser–tissue interaction.
Limitations
In summary of the above, there are 3 categories of laser parameters:
– “Fixed” parameters relate to the machine being used and are set by the laser manufacturer;
– “Adjustable” parameters relate to the capacity of the operator to adjust power output, frequency, time, etc.; and
– “Calculated” parameters relate to the product of 2 or more parameters, to confer specificity of the actual photonic “light” dose.
It is of little importance to report fixed parameters, other than laser make, wavelength and emission mode. Conversely, the recording of both adjustable and computed values, consistent with entries in Table 2, will develop a context for the evaluation of outcomes and the reproducibility of the study by later workers.
Conclusions
The impact and extent of incompletely recording laser operating parameters have been investigated. Recommendations have been made as to the adoption of full disclosure as part of submission guidelines for research presented through the World Federation of Laser Dentistry (WFLD). It is difficult to fully estimate the delay in the progress of laser dentistry due to the consequences of the (possibly inadvertent) lack of standardization in operational data and techniques. Equally, it is of relevance to acknowledge the contagion effect of poorly designed or incomplete data studies that are referenced in successive studies, often by the same group of researchers. There must be a responsibility on the part of peer-reviewed scientific journals to ensure full reproduction of the techniques and operating parameters. This may be achievable through the completion of a “tick box” declaration on the part of the authors. Additionally, it is worthy of consideration, when human in vivo studies are proposed, for full parameter disclosure to be included in the ethical approval application. Through a concerted effort to maintain the highest standards of representation of evidence-based laser dentistry, it is hoped that the extensive range of laser-adjunctive therapies may be confidently explored.
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Consent for publication
Not applicable.