Abstract
Background. The extent of pre-hospital medical care (PHMC) given to burned patients affects both the patient’s condition and the effectiveness of treatment.
Objectives. To improve the quality of PHMC of burns in children, based upon an analysis of the selected parts of pre-hospital medical records, with particular emphasis on analgesia.
Materials and methods. Medical records were used to analyze how PHMC was given to 117 burned children aged 0–18 years, treated at the Pediatric Surgery Ward between January 1, 2014 and December 31, 2017.
Results. In 41/85 cases, PHMC was delivered by Emergency Medical Teams (EMTs), in 42 in Emergency/Admission Rooms (ARs) and in 2 by Primary Health Care (PHC). Monotherapy was predominant. Medical records from ARs included the following information: the administration of analgesics with the name in 95% (21) of the cases, the route of drug administration in 45% (10), insertion of intravenous access and dressing in 33% (14), and fluid transfusion in 43% (6) cases. The way in which the EMTs provided assistance was described in 34% (14/41) of medical records, the administration of analgesics in 86% (12) cases, cooling and dressing in 43% (6), and the establishment of intravenous access with fluid transfusion in 36% (5) cases.
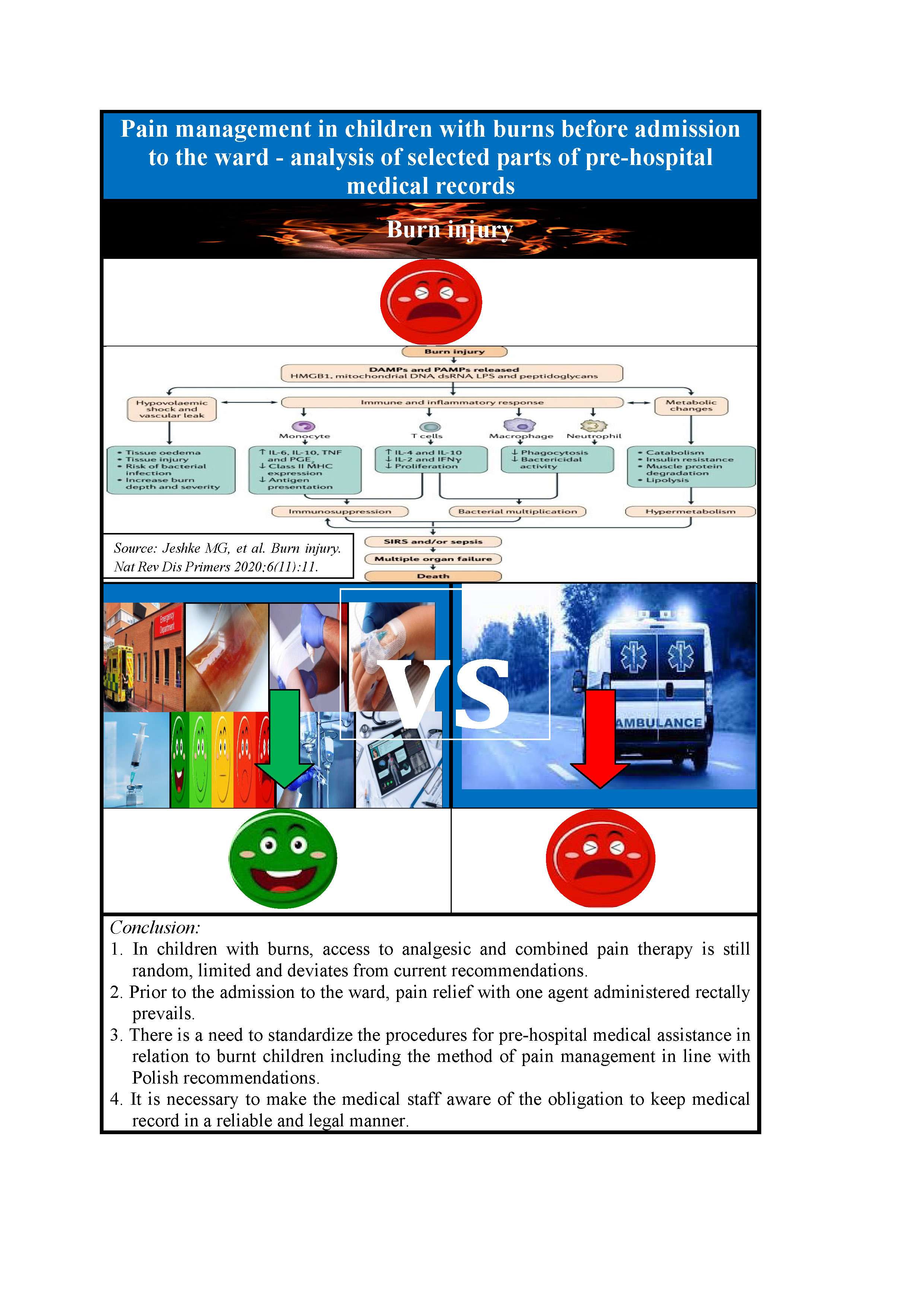
Conclusions. In burned children, access to analgesic and combined pain therapy is still random, limited and deviates from current recommendations. Prior to the admission to the ward, pain relief with 1 agent administered rectally prevails. There is a need to standardize the procedures for pre-hospital medical assistance provided to burned children, including the method of pain management in line with the Polish recommendations. It is necessary to make the medical staff aware of the obligation to keep medical records in a reliable and legal manner.
Key words: pain, burn, child, pre-hospital care
Background
Emergency Medical Teams, Admission Rooms (ARs) and Primary Health Care (PHC) staff provides medical assistance in pre-hospital conditions to people with burns. The scope of this assistance includes analgesia.1, 2 In burned children, analgesia is both a priority and an integral part of pre-hospital medical care (PHMC). The analgesia within this support is overlooked, limiting to non-pharmacological methods or a single analgesic agent, which negatively affects the child’s somatic and mental spheres.3, 4, 5, 6, 7, 8, 9, 10, 11, 12, 13 The consequence of small burns is a local defensive body’s reaction. Extensive thermal injuries cause systemic consequences leading to the development of burn disease and the systemic inflammatory response syndrome (SIRS). Thus, in the case of extensive burn lesions, it proceeds as a systemic inflammatory reaction resulting in, e.g., burn shock, sepsis and multiple organ dysfunction syndrome (MODS). Under the conditions of controlled inflammation, pro-inflammatory cytokines induce the formation of anti-inflammatory cytokines, cytokine inhibitors, and the symptoms of inflammation gradually subside – and compensatory anti-inflammatory response syndrome (CARS) is then diagnosed. However, if adaptive anti-inflammatory mechanisms are insufficient, the process becomes generalized inflammation. Thus, it is extremely important to implement analgesia in order to prevent the clinical complications.13
The medical services provided and the type of analgesia implemented should be carefully recorded in the medical records. Inaccurate completion of medical records and non-standards procedures are not uncommon, which hinders further management.14, 15
Objectives
The aim of study was to improve the quality of PHMC in burned children based on the analysis of selected parts of medical records, with particular emphasis on analgesia. Additionally, specific objectives were formulated:
– Is the pain in burned children relieved at the PHMC stage in accordance with the applicable recommendations?
– Is a single analgesic agent or a multiple therapy used for analgesia prior to admission to the burn unit?
– Using what route are painkillers given to burned children before admission to the ward?
– Did the PHMC staff properly complete the medical records before patients admission to the ward?
Materials and methods
The retrospective analysis comprised 117 medical histories of children, aged 0–18 years, admitted to the Department of Pediatric Surgery on the first day after sustaining a burn between January 1, 2014 and December 31, 2017. The analysis excluded 15 cases with burns occurring more than 24 h before admission. The medical records written by ARs doctors were subject to an analysis in terms of PHMC provided by the EMTs, in the ARs and in the PHC, with particular emphasis on analgesia. Medical procedures of ARs and EMTs affecting analgesia were compared. Percentage values of the studied variables were calculated and the descriptive method of statistical analysis of the studied parameters was used. The study was approved by the Bioethics Committee of the Medical University of Lodz, Poland (approval No. RNN/94/18/KE).
Results
In the study group of 117 children, thermal burns were predominant (97.43%), as a result of dousing (87.18%), mild, I/II degree, including up to 10% of the total body surface area (84.61%) (Table 1). The most common burns involved the head and neck, upper limbs and chest. The provision of PHMC was noted in the medical records of 85 children – 42 in the ARs, 41 by the EMTs and 2 in the PHCs. In the ARs medical records, the following was noted: administration of analgesics in 22 children, including the name of the agent administered in 21. In 1 case, there was only an entry “analgesics administered” but without specifying the name, dose and route of administration. Pain was most commonly alleviated with a monotherapy – paracetamol in 17 out of 21 children. In isolated cases, morphine was administered in 2 children, Dolargan in 1 child and Fentanyl in another 1. The dose of analgesic administered was recorded only in 3 children out of 22. A combination intravenous (iv.) treatment was used in only 1 severely burned child. Paracetamol was administered to 16 children. The dose of the drug was recorded only in 2 cases and the route of administration in 8. Morphine was given in 1 case subcutaneously at an undetermined dose, and in the other case the dose was specified but the route of administration was not marked. Dolargan was given to 1 child intramuscularly, also at an unspecified dose. Administration of other drugs was recorded in 4 out of 42 children: Luminal without specifying the dose in 1 case and Relsed in 3 cases, specifying the dose in only 1 child; establishment of iv. access, entered into the medical histories of 14 out of 42 children; transfusion of intravenously fluids in 6 children; indicating the name and volume of fluids transfused in only 1 case; protection of the burn wound with a dressing in 14 children; a note: “dressing” in 10 children, sterile dressing in 3, Argosulfan in 1 child; electrocardiography (ECG) examination in 1 child with electrical burns. A referral letter with a request for further treatment in the ward was issued for all AR patients.
The EMTs transported 20 children to hospital. The remaining 22 children were transported by parents/guardians. The EMTs assisted 41 children at the scene and 20 during transport from the ARs to the ward. The EMTs provided assistance at the scene described in only 14 of the 41 children. No information about the way assistance had been provided was available in the medical records of the remaining 27 children and the 20 transported from the ARs to the ward. In the medical records of 14 patients, the EMTs recorded administration of analgesics in 12 out of 14 children. The name of the agent administered was indicated in 11 out of 12 cases: paracetamol in 3 children, ibuprofen in 3, morphine in 3, and dolargan in 2 children. In the records of 1 child, apart from the entry ‘analgesic’, the name, dose and route of administration were not found. The doses of analgesics administered were recorded in only 2 out of 12 children. Pain was alleviated with monotherapy in ¾ of cases. Combination treatment was reported in 1 child. The route of analgesics administration was determined in 2 cases; administration of other drugs without indicating their names, doses and routes of administration in 2 cases; establishment of iv. access and fluid transfusion in 5 of 14 children; the fluid name and volume in only 1 case, and the information on infusion in 4 cases; and cooling and care of the burn wound in 6 of 14 children (Table 2).
Medical assistance was provided to 2 children at the PHC facilities. In both cases, there was no note of the analgesics administration. The children were transported to the ward by their parents/guardians.
Discussion
Each burn causes tissue damage and pain and affects the psycho-physical sphere; hence, analgesia should be a priority at every stage of medical assistance.2, 4, 11, 12, 13 Pain causes systemic vegetative reactions in the somatic and mental spheres. No analgesia or ineffective analgesia provision (oligoanalgesia) causes early and late consequences. Patients who experience pain are more likely to also experience anxiety, depression, sleep disturbances, delirium, or persistently lowered pain threshold. In children suffering from pain, there is an increased risk of modifying their endogenous regulatory mechanisms. This may lead to enlargement of the somatosensory area of the cerebral cortex responsible for the perception of pain, which causes neurosensory changes, hypoalgesia to thermal stimulus, and hyperalgesia in areas affected by inflammation.11, 12, 16
Despite the progress in medical science, the importance of medical assistance including analgesia is not always understood by medical staff authorized to administer painkillers.17 An analysis of how medical assistance is provided to burned children in the PHMC period in terms of analgesia may better highlight this problem and further improve the quality of this assistance.
In our study, similar to other researchers, thermal burns resulting from a dousing were predominant, and almost all of the cases were superficial (99%), involving up to 10% of total body surface area (TBSA).4, 8 Pre-hospital medical care was received by 85 children. The remaining 32 children received aid from their caregivers. From the obtained medical records, it was evident that the PHMC in the ARs boiled down to the administration of analgesics – in only half of children, the placement of iv. access, burn wound care and dressing in ⅓ of cases, and issuing of a referral letter for further treatment in the ward in all 42 children. Intravenous access was provided in 14 children, iv. fluids were transfused in every 7 patients, and the name and dose of the fluid transfused was given in 1 case. The recorded PHMC consisted of administering analgesics in 12 cases, applying a dressing to the wound and cooling the burn in 6 cases, and setting up iv. access and fluid transfusion in 5 cases. The name of the analgesic administered was indicated in most cases – 11, the dose in 2 and the name of the fluid transfused in 1 case. In 1 case, the assistance provided in the PHC facilities was limited to referring patients to hospital and protecting the burn wound with a dressing.
Over half of the children in the ARs received analgesics. Preferred was mainly monotherapy with paracetamol, most often including patients with minor burns. Morphine was given only to 2 children with moderate-to-severe and minor burns. Dolargan was administered to 1 child with a minor burn. Multimodal analgesia was recorded in only 1 child with a moderate-to-severe burn. The administration of analgesics was not recorded in the medical histories of 18 children with minor burns, and of 2 moderately burned children.
We found some irregularities in the manner in which the EMTs staff handled the pain. Multimodal therapy was used in only 1 case (Table 2), which indicates that the choice of analgesics was discretionary and not always in line with current recommendations.18, 19, 20, 21, 22
It could be considered erroneous to administer dolargan or morphine to a child with a minor burn and to desist from giving any drug from the first step of the World Health Organization Analgesic Ladder (WHOAL). According to the WHOAL recommendations, it is optimal for the patient to be administered analgesics of increasing efficacy and in line with the intensity of the pain. For alleviating minor pains, non-opioid agents are recommended, e.g., paracetamol or ibuprofen. In moderate-to-severe burns, a combination therapy is suggested, e.g., paracetamol and a weak opioid drug, e.g., Tramal or Fentanyl administered iv., bucally or intraosseously. To treat severe pain, the combination of an opioid preparation, e.g., Morphine, Dolargan or Fentanyl, with a non-opioid such as ibuprofen, paracetamol or ketamine is recommended.2, 21, 23, 24 Currently, ketamine cannot be administered by basic EMT staff in Poland.19 An accepted practice in the treatment of acute pain is to choose the agent and route of administration, including the iv. route, depending on the origin and intensity of the pain experienced, its mechanism, the point of uptake, and the duration time of its action.2, 19, 21 It is unreasonable to administer analgesics subcutaneously and rectally, or opioids intramuscularly, especially in moderate-to-severe burns, due to the delayed absorption and peak concentration of rectally administered substances (in the youngest children in particular).19 The choice of the intramuscular route for Dolargan and the subcutaneous for morphine may have been due to the ease of administration, lack of experience and fear of adverse effects.3, 25 Paracetamol with Metamizol, non-steroidal anti-inflammatory drugs (NSAID) and weak opioids have been shown to reduce opioid doses and to increase analgesic effect and efficacy.23
The choice of the appropriate analgesic and the route of its administration does not always correspond to the current recommendations and needs of a child. Medical staff often prefer oral route or non-pharmacological methods. Kiszka et al. noted the relief of burn pain with a hydrogel dressing alone in 15 out of 16 children described.9 Noskiewicz et al. reported the use of a hydrogel dressing in 96% of 310 children.8 Different observations were made by Baartmans et al., showing an increase in the administration of analgesics in a group of 622 patients from 68% to 79%, mainly of paracetamol and morphine, especially in burns above 10% of TBSA.26 The contradiction of the abovementioned observations may be due to doubts among medical staff about when and which analgesics should be used, depending on the type of burn, and when to relieve pain only locally and when in general. According to the literature, monotherapy of pain prevails in burned children during the pre-hospital period. Holak et al. showed monotherapy of pain by the EMT in 53% of 89 burned children, and combination therapy in only 20%.7 The current recommendation for pain scores of 1–3 on the numerical rating scale (NRS) is to administer non-opioid analgesics orally or per rectum. Instead, to relieve pain of 4–6 points, the NRS recommended the administration of a weak opioid and NSAIDs.21, 22, 23, 24, 27 To relieve severe pain of 7–10 points, a combination therapy is recommended, e.g., morphine/fentanyl with paracetamol or iv. metamizole. This strategy has an advantage of reducing the risk of side effects and increasing the extent of the analgesic effect.21, 22, 23, 24, 27 In 2019, the Polish Ministry of Health released recommendations for the treatment of pain in children for basic EMTs, which indicate that post-traumatic pain should be relieved regardless of intensity, with iv. or intraosseous opioids and non-pharmacological methods.19 In terms of the choice of analgesics, these recommendations are inconsistent with the WHOAL recommendations.21
Among healthcare professionals, the problem of oligoanalgesia may result from insufficient understanding of the need for pain management and commitment to pain relief, insufficient education, lack of regular assessment of pain intensity, and misconceptions.3, 7, 28, 29 Other researchers point to emotional, social, organizational, and environmental causes of pre-hospital oligoanalgesia in children.11 Giving up or avoiding iv. opioids may be due to the child’s age, difficulties in assessing pain intensity or providing iv. access, lack of experience, or the so-called opioidophobia.5, 6, 8, 14, 25 Those concerns were confirmed by Hartshorn et al., who reported more frequent analgesia in children provided with with non-opioid drugs (98%, 3802/3888), oral drugs (48%, 1880), paracetamol (29%, 1118), and ibuprofen (19%, 734).30
If iv. access is difficult to provide, fentanyl can be used safely by the sublingual or buccal routes.21, 24 Oligoanalgesia in children can be counteracted by periodic training of the medical staff, by reminding them of their obligation to treat pain, and through stronger enforcement of existing recommendations in clinical pracitce.12, 16, 17 Pain management among children and access to analgesics can be improved by a greater emphasis on teaching pain management in training standards.10
A series of deficiencies in the way medical records were kept also made it difficult to assess the extent of assistance provided. The ascertained deficiencies included the way in which emergency medical services were provided by the EMTs in all children transported from the ARs to the ward, the administration of any analgesic in almost half of the children, the way in which assistance was provided, the name of the drug administered, the dose, route of administration, as well as the establishment of iv. access, fluid transfusion and the burn wound care. These are problems frequently observed in medical facilities in other regions.4, 31 Holak et al. proved that information on pain management was missing in the medical records in 99% of 2,452 EMT patients.7
Pain management in burned children still leaves much to be desired. It requires a coordinated action and systemic interventions at the legislative, organizational and educational levels. The obtained results are the basis for further analyzes and improvement of clinical practice for comprehensive care for children with burns.
Conclusions
1. In burned children, access to analgesic and combined pain therapy is still random, limited, and deviates from current recommendations.
2. Prior to the admission to the ward, pain relief with 1 agent administered rectally prevails.
3. There is a need to standardize the procedures for pre-hospital medical assistance in relation to burned children, including the method of pain management in line with the Polish recommendations.
4. It is necessary to make the medical staff aware of the obligation to keep medical record in a reliable and legal manner.