Abstract
Background. The transfer of digital radiographic images is widely practiced. Digital image processing can influence the perception of image quality. The question arises as to how exposure, internal image adjusting algorithms and image file transfer affect the optical density of digital radiographs.
Objectives. To evaluate the influence of exposure time, optimization and file transfer on digital radiographs.
Material and methods. Calibration patterns were formed and a series of digital radiograms were recorded under standardized conditions. The radiographs were exported and then imported into the same software. Three groups of radiographs were analyzed: A – images originally performed and recorded in the software; B – images imported after exporting an optimized image; and C – images imported after exporting an image without optimization but with measurements of the density of the marked regions of interest.
Results. An increase of the exposure time decreases optical density. The optimization algorithm increases contrast and decreases differences between exposure times. Long exposures affect the visibility of objects with low optical density. After importing the images in Group B, there was a risk of using the optimization algorithm twice. When optimization was not performed, there were no differences between Groups B and A. In Group C, there was no risk of doubling the optimization algorithm.
Conclusions. The transfer of digital radiographs can exert an influence on the optical density values. To avoid the risk of image distortion, files should be exported without image optimization.
Key words: image analysis, digital radiography, image transfer
Introduction
The traditional technology using X-ray films is being replaced by digital radiography and other digital technologies. Images recorded on radiographs are black and white and individual pixels possess a specific lightness ranging from 0 to 255 (256-grade 8-bit grayscale – the scale of optical density). The brighter the area appears on radiographs, the higher the optical density. The software (the internal algorithms of image processing) compensates for changes in exposure time and allows the images to have suitable brightness and contrast; therefore, “lighted” (dark) or “under-exposed” (bright) images are uncommon.1, 2 Digital processing of image parameters such as brightness, contrast, sharpening, smoothing, and zooming can correct the visibility of certain regions, making the image more accessible to the human eye. However, digital image processing can produce artefacts that may resemble pathologies.3, 4, 5 The software also makes it possible to measure the length, angle and optical density of selected areas of the image.6, 7 In the case of measuring the length of an object, the picture can be calibrated; however, in case of the optical density measurements (radiodensitometry and radioabsorption), this is not possible. The transfer of digital radiographs and the scanning of conventional radiographs to obtain a digital image is practiced widely, but digital processing of an image can have some impact on both the diagnostic value of the X-ray image and the subjective perception of the image quality.8
The advantage of digital images lies in the ease of storage and transferring. However, it should be also remembered that most dental software uses an internal, integrated optimization algorithm to compensate for the exposure conditions and sensor properties. Therefore, the question arises as to how the exposure conditions, internal image adjusting algorithms and image file transfer affect the optical density of digital radiographs. There is a lack of data in the available literature on this topic.
The purpose of the study was to evaluate the impact that file transfer, exposure time and the optimization algorithm have on the optical density of dental radiographs.
Material and methods
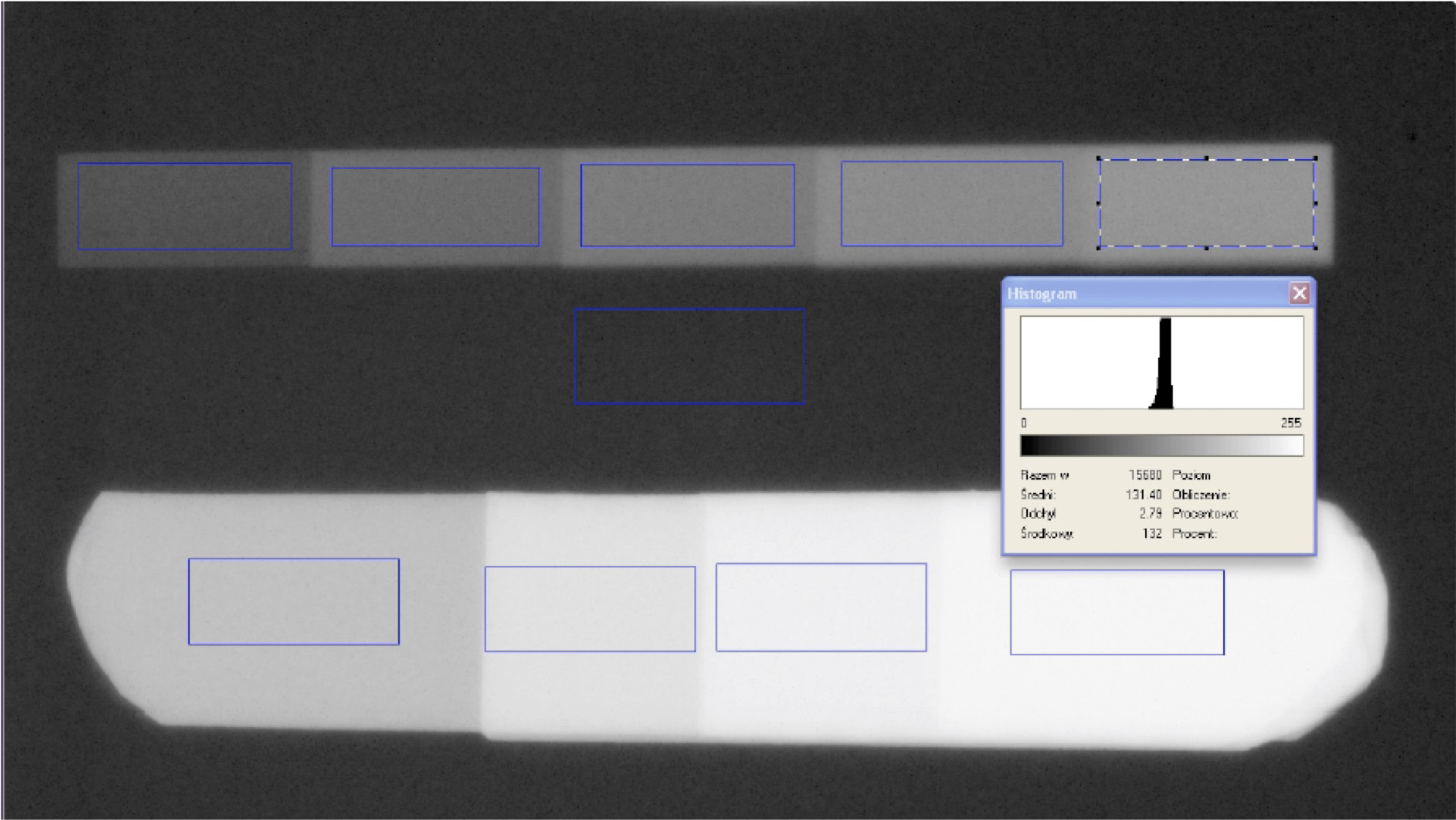
A pattern containing 2 separate stepped-wedge patterns for digital radiographs was produced. Pattern 1 was formed from aluminum and consisted of 5 steps: 0.7 mm, 1.3 mm, 1.9 mm, 2.5 mm, and 3.1 mm. Pattern 2, showing lower radiolucency, was made from lead foil that originated from radiographic film (Foton Dental DX-D 3–4 cm ANSI 1. ISO W2 Emulsion No. 00905.3; Foton, Warsaw, Poland,) and consisted of 4 steps formed by 1–4 foil layers (Figure 1). Radiographs were taken with a digital radiography Dixi 3-CCD sensor (Planmeca, Helsinki, Finland), Planmeca Intra X-ray apparatus (Planmeca) and Dimaxis Classic v. 4.2.0 (Planmeca). The Dimaxis Classic software was also used for image analysis export and import. The images were recorded after fastening the receptor and a holder to a 30-cm-long tube. The abovementioned patterns were located on the sensor surface (Figure 2).
A distance of 4 cm between the tube of the Planmeca Intra and the Dixi 3 sensor was kept constant. Likewise, the position of the patterns on the surface of the sensor was constant. The selected parameters of the exposure were 60 kV and 8 mA, whereas the exposure time was the only variable.
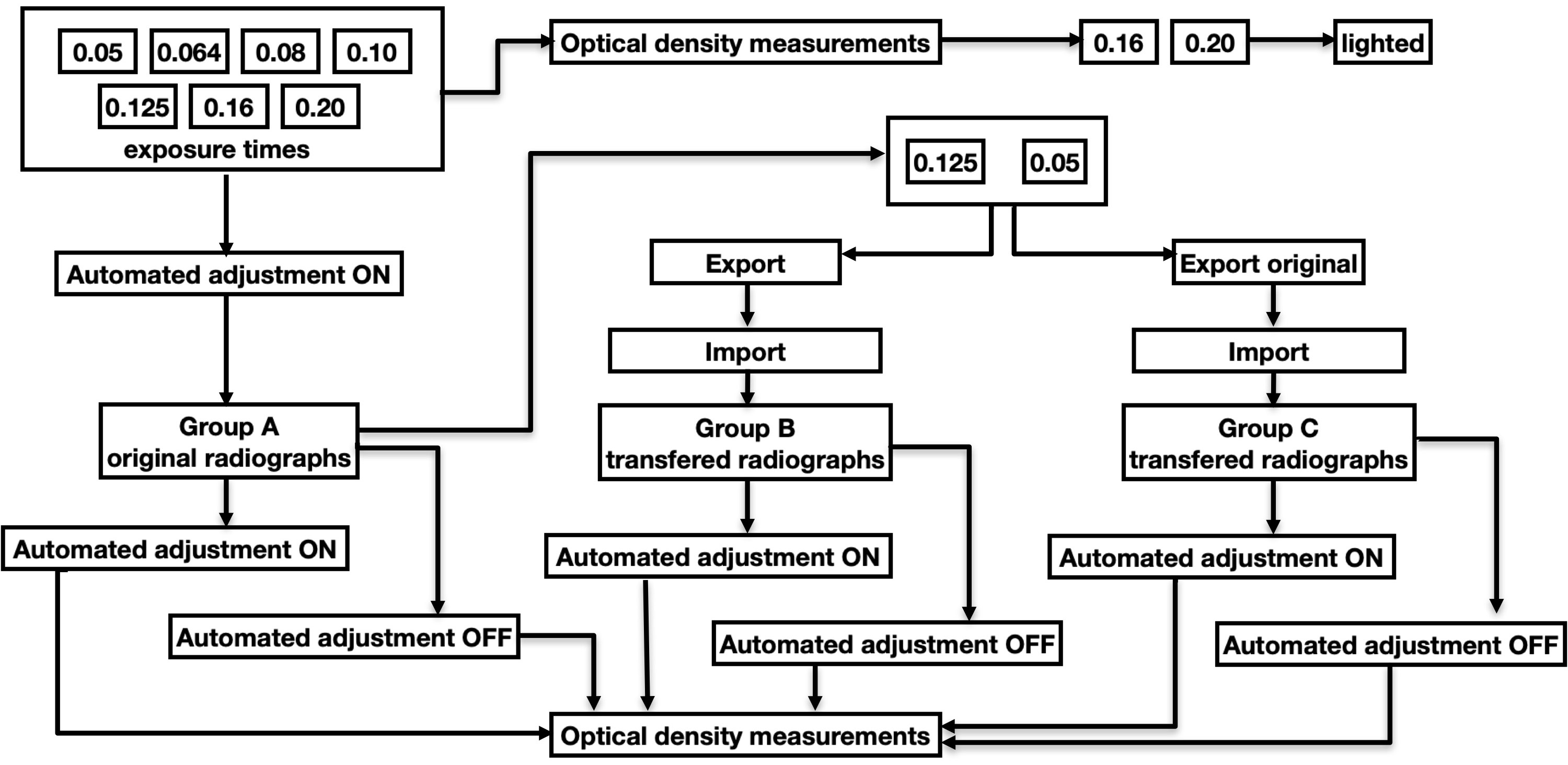
A series of 7 images were recorded (256-grade 8-bit grayscale) with exposure times of 0.05 s, 0.064 s, 0.08 s, 0.1 s, 0.125 s, 0.16 s, and 0.2 s, at the maximum resolution and equivalent software settings (Group A). Radiographs captured with exposure times of 0.05 s and 0.125 s, without any manual image correction, were exported from the software using 2 different file export options. The 1st one exported the image relying on default software settings with the automated picture adjustment algorithm turned on (the “export” function), whereas the 2nd one exported “the clear” image without an automated picture adjustment algorithm (the “original export” function). The exported files were saved in the lossless TIFF format. Then, the resulting radiograph files were imported into the Dimaxis software. In this way, 3 groups of radiographs were received. The 1st group of radiographs (Group A) included those which were originally made and recorded in the database of the Dimaxis software, whereas the 2nd one (Group B) comprised of radiographs imported after having been exported with optimization performed by the software (the “export” option); the 3rd one (Group C) comprised of radiographs imported after having been exported without optimization performed by the software, which is called “original export”. A diagram of the procedures of export, import and optical density measurements used in the study are presented in Figure 3.
All radiographs were analyzed according to the same scheme, where the regions of interest (ROIs) were marked on the pattern-free background (marked as 0) and on particular steps of the 1st and 2nd patterns. The parts of the 1st pattern (the aluminum one) were marked in steps 1–5 and the parts of the 2nd pattern (the lead one) in steps 6–9. Higher figures refer to a higher degree of radioabsorption. The optical density for each of the ROIs was expressed by the software as an average value, together with standard deviation (SD) (Figure 4). The mean value and SD of each ROI (in a 256-grade scale of grayness from 0 to 255) were recorded. The blackened areas have low values, whereas the light ones have high values because they show high radioabsorption. The number of pixels in the ROIs ranged from 18,500 to 20,000 (the size differences between the ROIs did not exceed 1,500 ppx).
Additionally, to evaluate the effect that the changes in exposure time, the internal image adjusting algorithms, and the transfer of the image files had on the optical density of the bone structure, a series of dry human jaw bone radiographs were performed with the aluminum pattern as described above. The images were analyzed by 2 observers with general dental knowledge about X-ray image evaluation.
Results
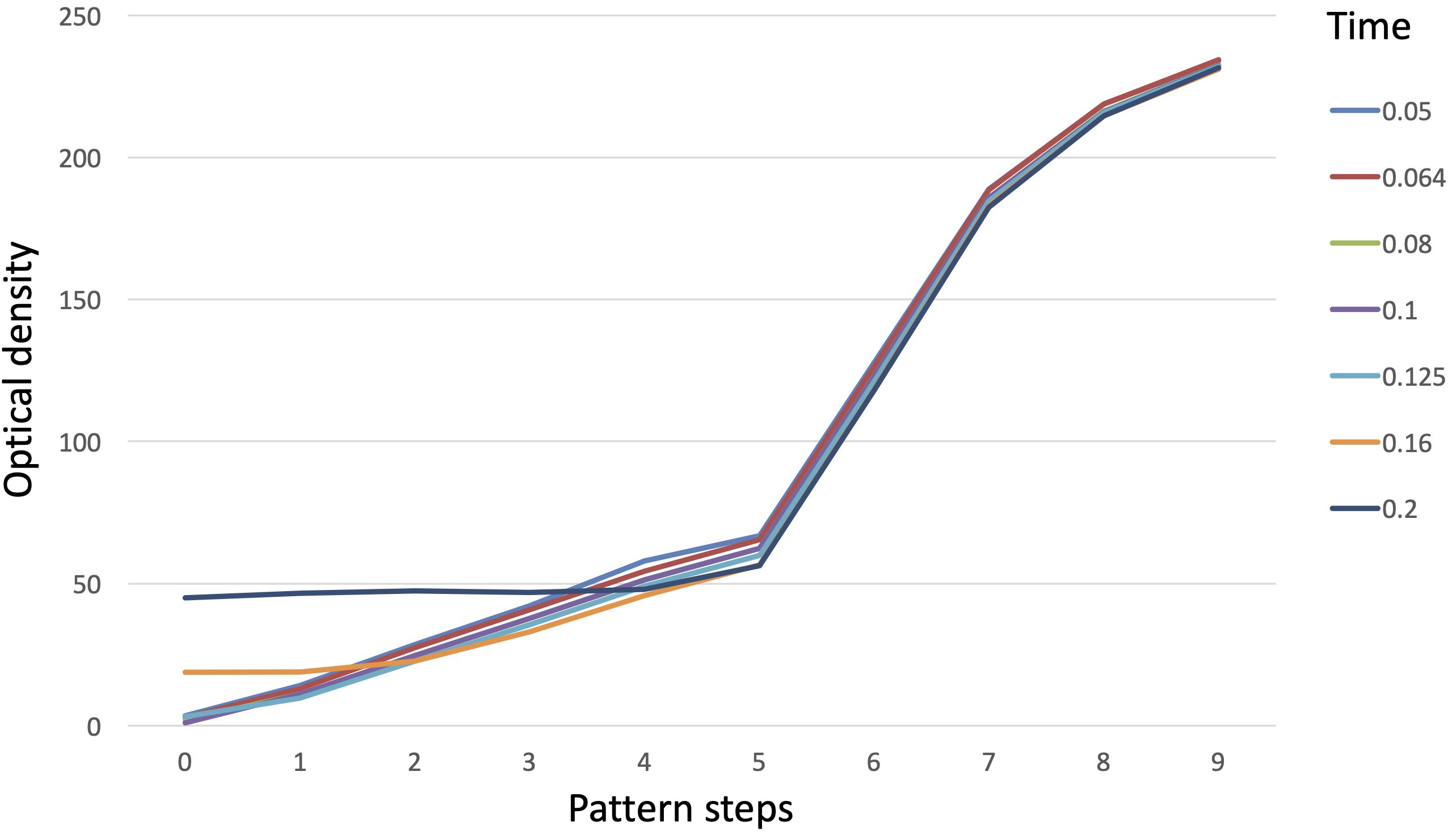
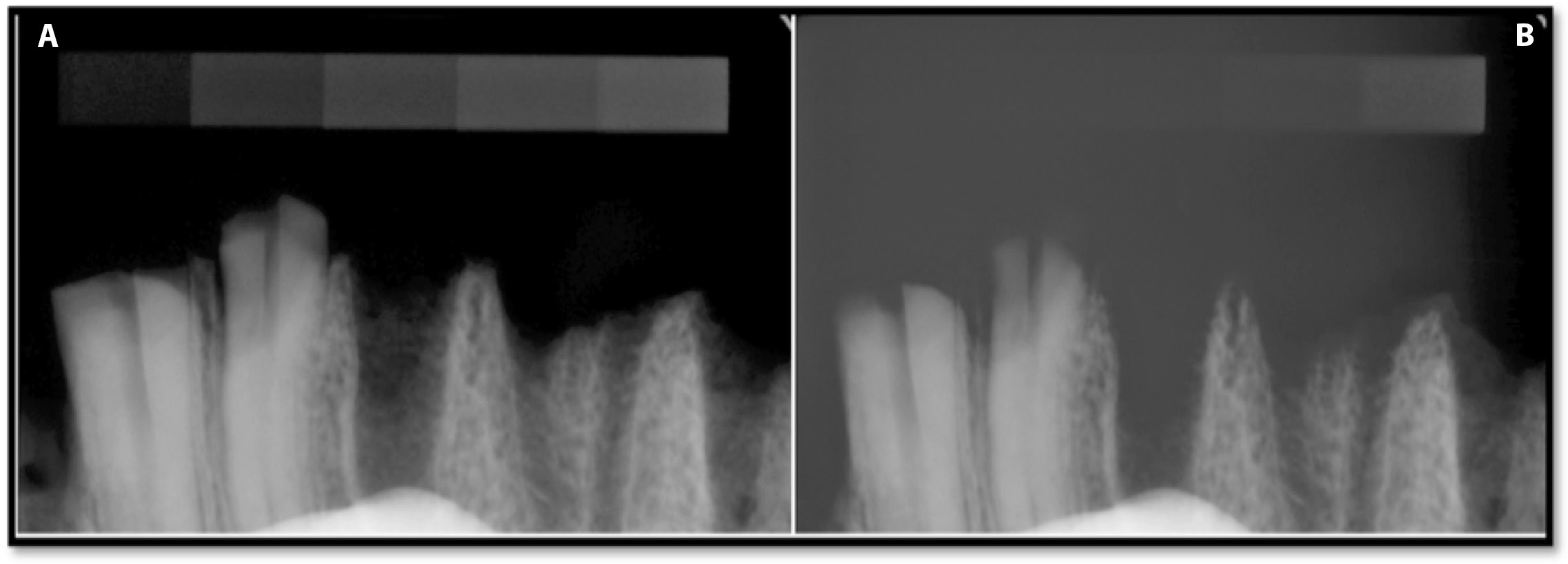
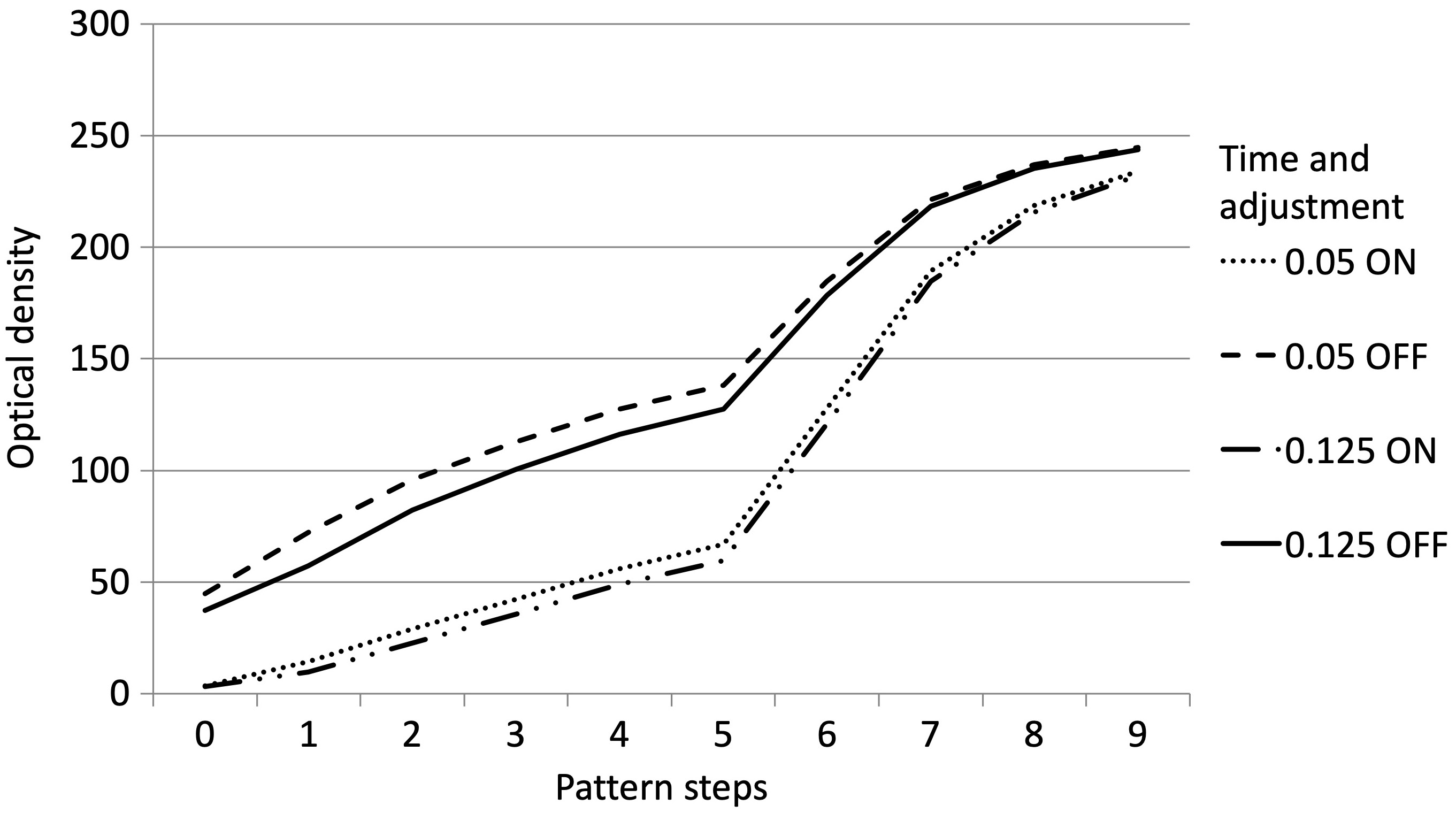
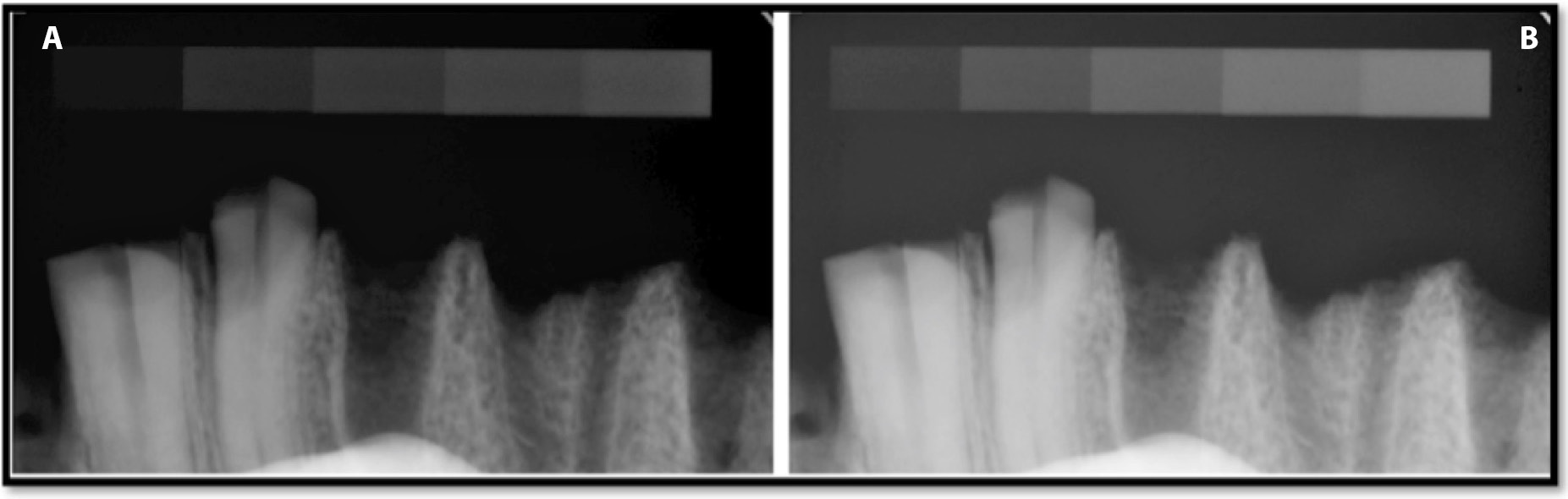
According to the study design, the 1st stage consisted in collecting values of optical density for all exposure times after image registration in the patients’ charts and without the image corrections being subjected to analysis on the PC connected to the Dixi3 sensor (Group A). The values of optical density in Group A are presented in Table 1 and Figure 5. The data (Group A) showed the influence of exposure time on optical density when the image optimization algorithm was active (default software setting). When the exposure times ranged from 0.05 s to 0.125 s, the optical density values measured along all phantom steps decreased with an increase in exposure time. The largest optical density decrease was observed for step 1 – 31.7% (14.2 ±2.2 at 0.05 compared to 9.7 ±1.4 at 0.125) – and the smallest was for step 9: 0.8% (234.0 ±1.9 at 0.05 compared to 232.1 ±1.2 at 0.125). At exposure times of 0.05–0.125 s and over the whole optical density range, the differences between the degrees of the pattern were sufficient, i.e., the images had sufficient contrast. The Group A radiographs of bone specimen captured with exposure times of 0.125 s and 0.2 s are presented in Figure 6. The excessive exposure time caused image disturbances of the objects with an optical density of less than 50. On the images captured with an exposure time of 0.16 s, the differences between the background and steps 1 and 2 of the pattern were blurred and no considerable differences between these ROIs were noticed. With an exposure time of 0.2 s, the differences were blurred not only between the background and steps 1 and 2, but also between the background and steps 3 and 4. Therefore, it can be stated that an object with low radioabsorption becomes imperceptible at exposure times of 0.16 s or 0.2 s. A comparison of the bone specimen radiographs that were captured with exposure times of 0.125 s and 0.2 s displayed a blurred difference between the background and the object at a longer exposure time (Figure 5).
The impact of the optimization algorithm on the Group A radiographs, which were captured at exposure times of 0.05 s and 0.125 s, are presented in Table 2 and Figure 7. The radiographs of the bone specimen captured with an exposure time of 0.125 s – with and without the automated adjustment option – are presented in Figure 8.
The results demonstrate that the algorithm causes a reduction in the difference between particular exposure times as well as a reduction in optical density. The lower the optical density, the larger the decrease in optical density was recorded (Figure 7). The decrease in optical density recorded for the exposure times of 0.05 s and 0.125 s at step 1 amounted to 80.5% and 83.1%, respectively, and at step 9 it was 4.3% and 4.8%, respectively. A detailed analysis of step 2 of the imaging phantom showed the difference between the optical density value for exposures of 0.05 s and 0.125 s to be 13.7 (96.0 ±3.9 compared to 82.3 ±3.2) with the automated adjustment function switched off, and only 5.9 (2.3 times lower) (28.7 ±2.8 compared to 22.8 ±2.0) when the function was on. These changes can be seen in the radiographs of bone specimen (Figure 7).
The use of automated adjustment resulted in the image becoming darker and more contrastive in areas with an optical density higher than 50 (phantom steps 5–9). The higher image contrast displaying the clearer structure of the object. However ROI’s with low optical density became blurred (decrease of contrasts between steps 1 and 2, 2 and 3, 4 and 5) in comparison with the radiographs without the automated adjustment option. The algorithm made the 1st degree of the pattern and a thin alveolar plate invisible to the observers (Figure 7).
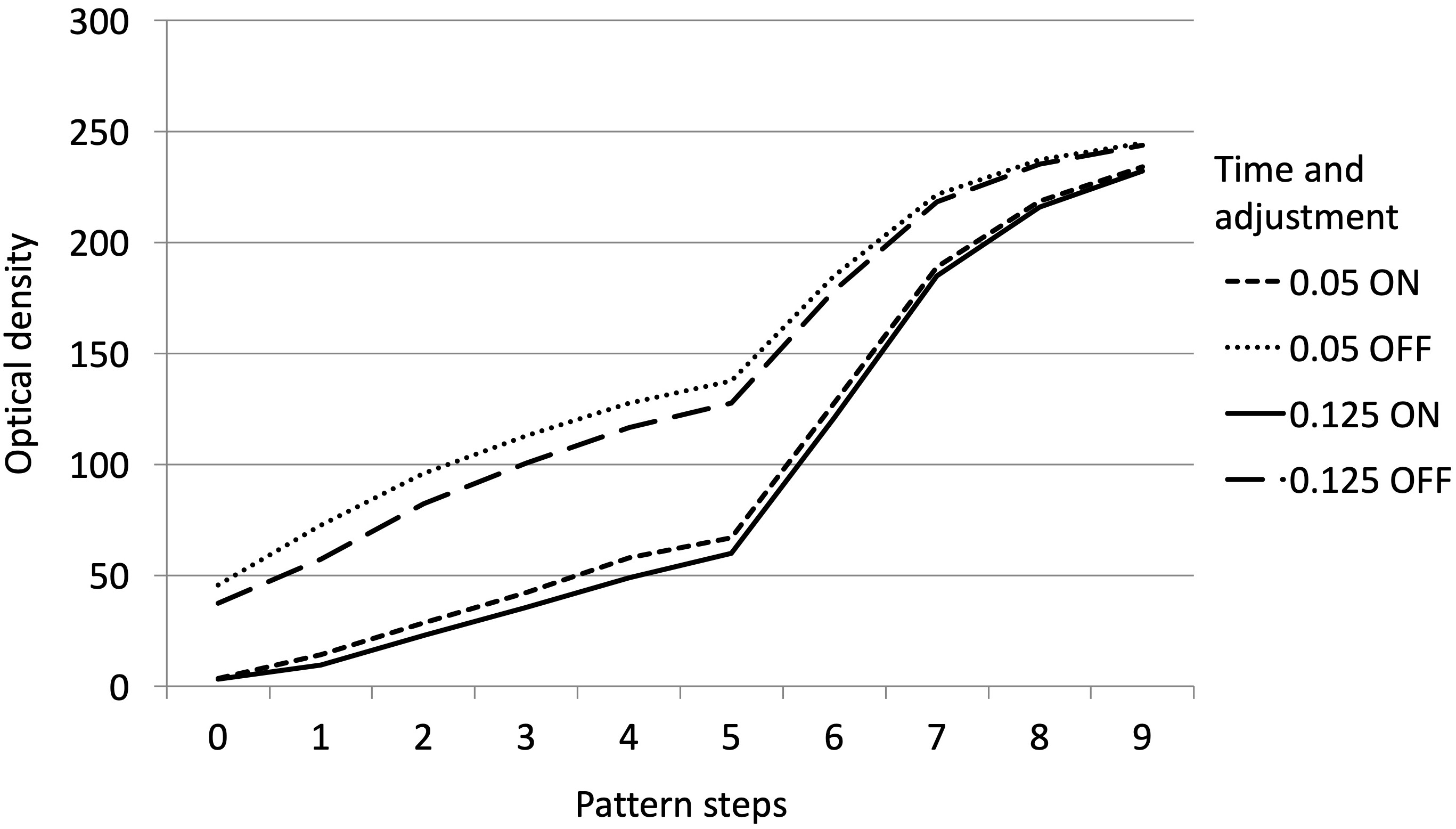
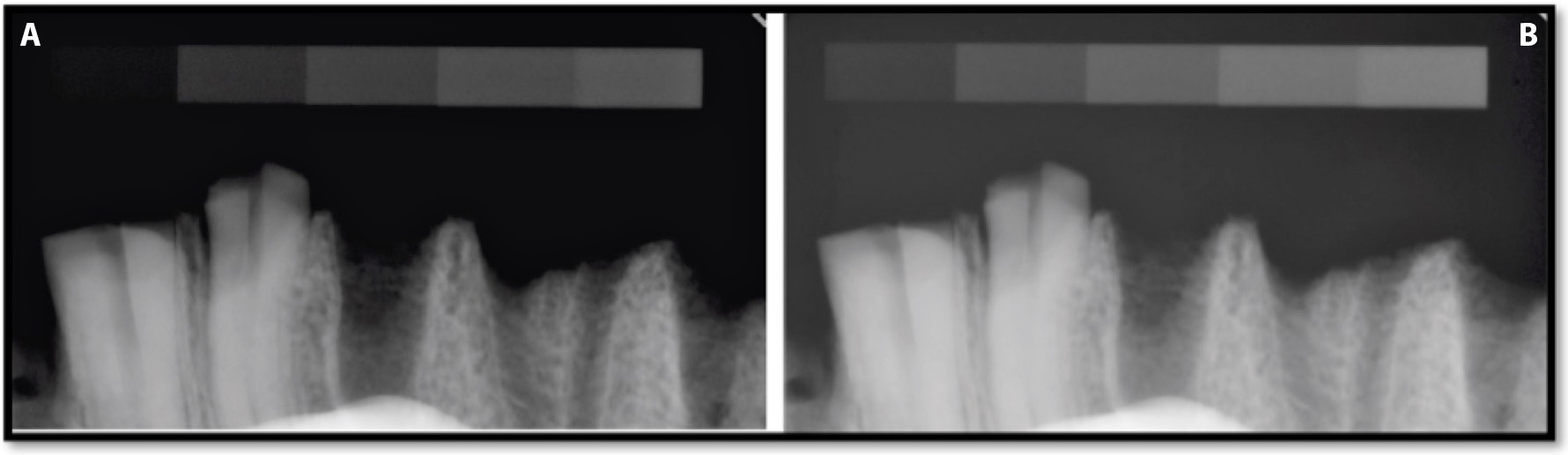
The optical density values of Group B and Group A images captured with exposure times of 0.05 s and 0.125 s are presented in Table 3 and Figure 9. Radiographs of Group B with a bone specimen recorded with an exposure time of 0.125 s are presented in Figure 10. The analysis of the Group B images transferred after exporting with the “export” option (after optimization) revealed that after importing, some structures of the spongy bone (density equivalent to steps 1, 2 and 3 of the phantom) may become undetectable. The use of automated adjustment, after file import, reduced the optical density values of the phantom radiographs from degree 1 to 8, at exposure times of both 0.05 s (from 95.9% to 2.2%) and 0.125 s (from 96.9% to 0.14%) – with the exception of degree 9. The observed ROIs were black and steps 1 and 2 of the phantom also became invisible at shorter (0.05 s) and longer (0.125 s) exposure times. The image background achieves the optical density equal 0 and is totally black. The structures with higher radioabsorption remained visible and the optical density was reduced for steps 6 and 7 of the phantom. It did not change in the case of step 8 and grew in the case of step 9 at both exposure times. The observed problems with the image were the result of using the optimization algorithm repeatedly. In this case, the algorithm should be turned off. Deactivating the optimization algorithm resulted in an optical density that was comparable (identical) with the original one at both exposure times and images that were less dark, displaying the object details more precisely (Figure 9).
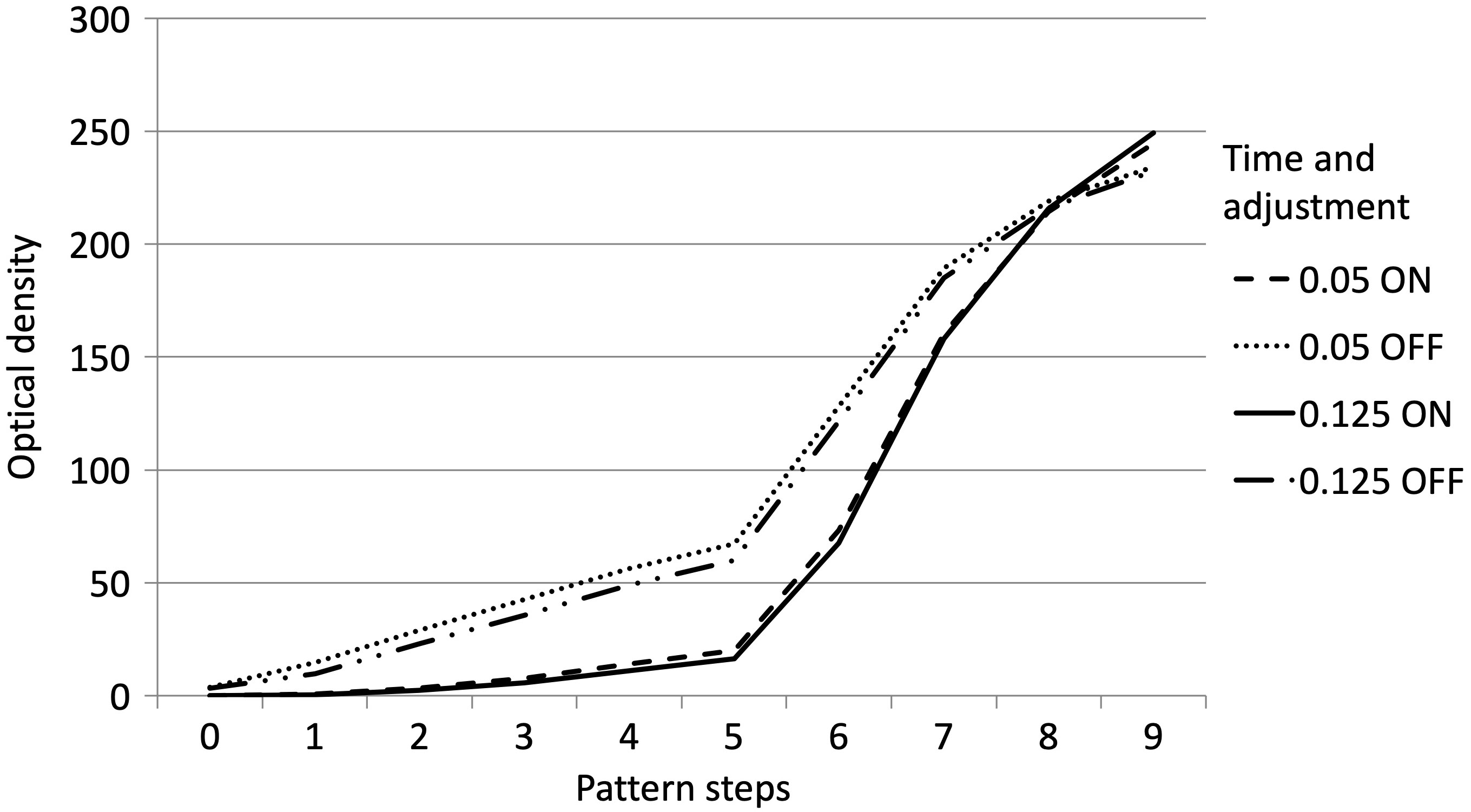
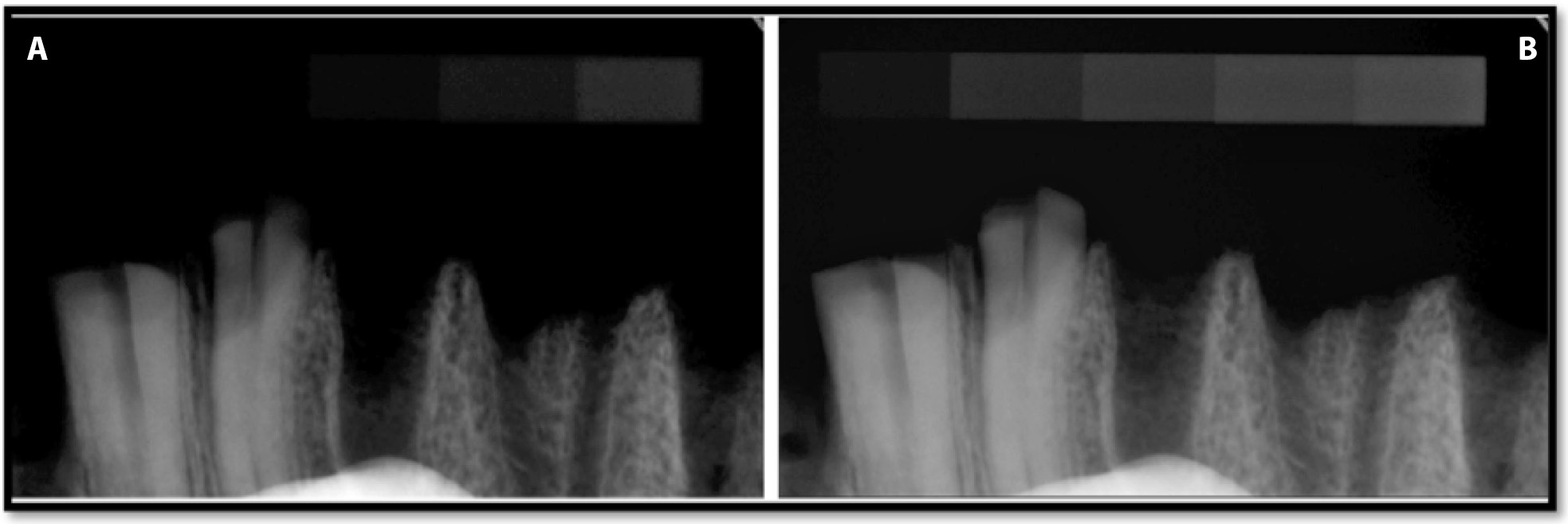
The recorded optical density values of the Group C radiograms captured at exposure times of 0.05 s and 0.125 s and the original images are presented in Table 4 and Figure 11. The Group C radiograph of bone specimen captured at an exposure time of 0.125 s is presented in Figure 12. The analysis of the Group C images (export without optimization) revealed that not applying the automated adjustment function after file import yielded an increase in the optical density values of the radiographs of all the phantom degrees over the original images (enhanced with the optimization algorithm). The increase was independent of exposure time (at 0.05 s the value changed from 80.2% to 4.4% and at 0.125 s from 82.9% to 4.7%). However, activating this function (after import) provided an optical density almost identical to the original radiographs of all phantom degrees at both exposure times. Similarly Group C radiographs of the bone samples appears identical to those of Group A. (Figure 7 and 11).
Discussion
Every image stored in the form of a file can be transferred, duplicated and changed digitally. Each adjustment which restores, improves, analyzes, or in some way changes a digital image is a form of image processing, e.g., image enhancement – brightness and contrast, sharpening and smoothening, or zooming in – or image analysis – measurement, segmentation, proportion finding, object classification, image synthesis, or compression.3, 5
This type of processing does not alter the content of the image but does improve (or change) the visual perception to enable a better diagnosis.9, 10 That is why understanding the individual of functions and their appropriate applications is extremely important in professional work, regardless of the X-ray detector type.11 On the other hand, the exporting of digital radiographs to a file format that is compatible with commercial graphic software can cause some changes in the original digital information.4 For the purpose of this study, a simple pattern consisting of aluminum and lead steps with graded thicknesses were prepared. The use of the pattern allows exposure differences to be compensated for (and/or detected), the optical density to be calibrated, and finally, for different exposure conditions to be compared objectively. The use of an imaging phantom to measure bone optical density provides accurate and reproducible results and allows the impact of file transfers on qualitative and quantitative image changes to be measured.12
A similar device with fixed degrees of absorbed X-ray radiation was successfully used as a phantom by Yang et al. to measure the density of the jaw bone.13 The repeatability of projection and exposure is an important factor when digital images are compared.14, 15 The use of a pattern simplifies the objective detection of and compensation for differences between objects with identical radioabsorption, as well as image calibration. On the other hand, the pattern covers a significant area of the small intraoral sensor or plate. Therefore, in clinical conditions, the use of a pattern is difficult or even impossible, especially when other structures overlap the image of the pattern. In most software used for dental radiography, instead of a phantom, some optimization algorithms are used to compensate for differences between the exposures. In clinical conditions, when it is difficult to maintain repeatability, the proper functioning of optimization algorithms is crucial.
The tools for measuring the optical density of bone radiographs and improving the image contrast are widely used during the evaluation of digital radiographs. Image manipulations, as well as the use of inappropriate monitors, affect perceptions; therefore, attention should be paid to the appropriate selection of exposure parameters and image correction tools.16 However, thoughtful and skillful application of these tools to detect root resorption can be applied according to the observer’s preferences without affecting the diagnostic accuracy.17 The use of appropriate filters in digital radiology allows for a more accurate assessment of radiographs when dealing with inflammatory conditions of periapical tissues.18 Some filters, like the reverse of the grayscale, allows the image to be evaluated from a different aspect. However, it does not always have significant influence, e.g., in assessing the length of root canal instruments radiographically.19 Optical density measurement with the use of cone-beam computed tomography (CBCT) was also used to compare bone density around the impacted canines, which allowed a higher optical density of the bone surrounding the impacted teeth to be shown.20 The use of appropriate software may also help in the detection of general diseases such as osteoporosis based on dental X-ray radiographs.21, 22 The correlation between the measurement of the bone density of alveolar bone and spinal bone indicates the importance of dentists being the first to pay attention to bone density disorders.23, 24
When analyzing and comparing images, it should not be forgotten that the software usually compensates for variations in exposure parameters with automated optimizing algorithms. The option (algorithm) of automated adjustment, which corrects a digital image, is also included in the Dimaxis software that was used in this study. The default application of an optimization algorithm significantly reduces the differences between exposure times if they are in the range of 0.05–0.125 s. The use of longer exposure times (0.16 s and 0.2 s) highlights the limitations of the software and the sensor used in this study, as it caused image disturbances of objects with an optical density of less than 50. Because an object with low radioabsorption becomes imperceptible at exposure times of 0.16 s or 0.2 s, those radiographs were recognized as “lighted.” A similar selection was made in the article by Morea et al. due to the ghost images which were produced by an exposure time beyond the latitude of the sensor.16 Overexposure of the 0.16-second and 0.2-second images can also be caused by the lack of a soft-tissue-equivalent absorbing part of the radiation between the X-ray beam and sensor. The soft tissue model was not included in the current study. This assumption is confirmed in Figure 7, Figure where the operation of the algorithm is visible and makes the first-degree pattern and a thin alveolar plate invisible.
Suryani et al. presented the importance of post-processing the digital panoramic radiographs for a more accurate visualization of anatomical structures in children.9 Image quality processing techniques affect the quality of the image in various ways depending on the diagnostic purpose (caries, periapical lesion or root canal treatment) and must be properly selected. Based on the optical density of the ROIs, the use of automated image adjustment should be considered unfavorable because some structures may become invisible.
Bone density measurement to assess bone tissue and the images after importing is used in various studies.25 Measuring and comparing the density of selected jaw fragments is important when the healing or inflammation processes are compared over time.26 The efficacy of this method of testing the optical density of rat bones after the administration of ketoprofen was found by Martins et al.27 Disturbances in the readout of X-ray image parameters during transfer, such as optical density measurements or contrast differences, may be important in diagnosis. This was confirmed in studies in which the contrast change significantly changed the possibilities of measuring the length of small root canal instruments.28 However, accurate measurement of the optical density of bones is also important and may be a complement to CT analysis before implantation in the mandible.26 The results of the current study suggest that the automated adjustment function can disturb the process of image transfer (exporting from the raw data and importing to another database), and that in some cases, it can cause considerable differences in the recorded values of optical density. The analysis of Group B images revealed problems associated with the repeated use of image optimization, when areas with low radioabsorption become completely invisible. Importing files that have not been subjected to the optimization algorithm (Group C) seems to be safer, as there is no risk of image darkening or blurring of structures. In the era of digital radiology, the clinician assessing an imported radiograph should be aware of the possibility of such interference. In this study, a specific sensor and software were used, so the resulting limitations should be considered when analyzing the results.
Conclusions
Within the limitations of this study, it can be concluded that 1) the transfer of digital radiographs can exert an influence on the recorded values of optical density, and thus on a comparative assessment, so the same (or a similar) algorithm of image processing should be used; 2) automated contrast enhancement and exposure compensation may blur the image of low-density structures; and 3) the radiogram files should be exported without image optimization. This way the risk of image distortion can be eliminated and the perception of low-density structures will not be distorted.