Abstract
Social prescribing (SP) has gained increasing attention as an approach to addressing non-medical determinants of health by linking individuals to community-based resources. While SP is frequently discussed in the context of health inequalities, its relevance to lesbian, gay, bisexual, transgender, and other sexual and gender minority (LGBT+) populations has not been systematically examined. LGBT+ populations experience multidimensional health challenges shaped by social, structural, and institutional factors, including unmet social needs and barriers within healthcare systems, which may render SP conceptually relevant but empirically uncertain. This narrative review synthesizes and critically examines the international literature on SP with a particular focus on its conceptualization, application, and limitations in the context of LGBT+ health. A structured narrative search of major biomedical databases was conducted, complemented by title-based screening and review of relevant policy and practice sources. Findings were synthesized thematically. The available evidence directly addressing SP in LGBT+ populations is sparse and limited. Existing studies are predominantly descriptive or qualitative, often embedding LGBT+ individuals within broader vulnerable groups without disaggregated analysis. While inclusive SP models and services exist in practice, particularly within the UK, their effectiveness has not been rigorously evaluated. Overall, the literature reveals a substantial gap between the theoretical relevance of SP for LGBT+ health and the availability of robust empirical evidence to inform its implementation.
Key words: social determinants of health, primary health care, sexual and gender minorities, health inequities, social prescribing
Introduction
Social prescribing (SP) has emerged internationally as an approach intended to address non-medical factors that influence health and wellbeing by linking individuals to community-based resources and services.1, 2 It is commonly described as a means of addressing social determinants of health, unmet psychosocial needs, and broader contextual factors that are not readily addressed through clinical interventions alone. From the perspective of primary care, psychosocial problems are widely perceived by general practitioners (GPs) as time-consuming and burdensome within routine consultations.
In this context, SP and other models integrating medical and non-medical services have been discussed by GPs as potentially meaningful approaches to addressing patients’ social needs, although concerns regarding their practical implementation remain.3, 4 Over the past 2 decades, SP has gained increasing attention within health systems in Europe, North America, and other regions, accompanied by a growing and diverse body of academic literature examining its delivery models, implementation, and outcomes.2, 5, 6, 7
Despite this growing interest, the field of SP remains heterogeneous and conceptually complex. Reviews of the literature consistently highlight wide variation in how SP is defined, delivered, and evaluated across settings and populations.5, 7 Outcomes studied range from mental well-being and social connectedness to healthcare utilization and patient experience, with substantial methodological diversity and limitations that complicate synthesis and interpretation.2, 5, 8
As a result, SP is best understood as a developing, system-level approach rather than a standardized intervention with clearly established effects. This implementation-oriented framing aligns with recent European primary care guidance, which emphasizes multidisciplinary delivery models and equity-sensitive approaches to translating prevention recommendations into routine practice.9
Social prescribing is most frequently discussed in relation to populations experiencing complex health and social needs, including individuals living with long-term conditions, mental health challenges, or social isolation.2, 10 These contexts have drawn attention to the role of structural and social conditions in shaping health outcomes and healthcare experiences. Within this broader landscape, there has been increasing recognition that specific populations may encounter patterns of need that render them particularly relevant for examining how SP is conceptualized and applied.
Existing evaluations of SP rarely examine differential effects across social positions such as socioeconomic status, ethnicity, gender identity, or rurality, with most evidence focusing on overall uptake and perceived benefits rather than subgroup-specific effectiveness.11 Similar equity gaps in implementation and reporting have also been highlighted in European prevention guidance for primary care, reinforcing the need for structured, equity-oriented delivery and evaluation frameworks.9
Lesbian, gay, bisexual, transgender, and other sexual and gender minority (LGBT+) populations represent one such context. A substantial body of international literature documents that lesbian, gay, bisexual, trans, and other sexual and gender minority individuals experience distinct health patterns and healthcare experiences shaped by social, structural, and institutional factors rather than biological differences alone.12, 13 These include a higher prevalence of mental health conditions, differential exposure to stressors related to stigma and discrimination, and less favorable experiences within healthcare systems.6, 12, 13 Quantitative and narrative reviews further demonstrate that structural stigma at the policy and societal levels is associated with adverse mental, behavioral, and physical health outcomes among LGBT+ populations.13
While SP has increasingly been framed as a response to non-medical determinants of health, its relevance and application in the context of LGBT+ health have not been systematically synthesized. The existing literature addressing SP and LGBT+ populations is limited, fragmented, and often embedded within broader discussions of health inequalities or community-based interventions. Consequently, there is a lack of consolidated analysis examining how SP has been conceptualized, applied, and critiqued in relation to LGBT+ health.
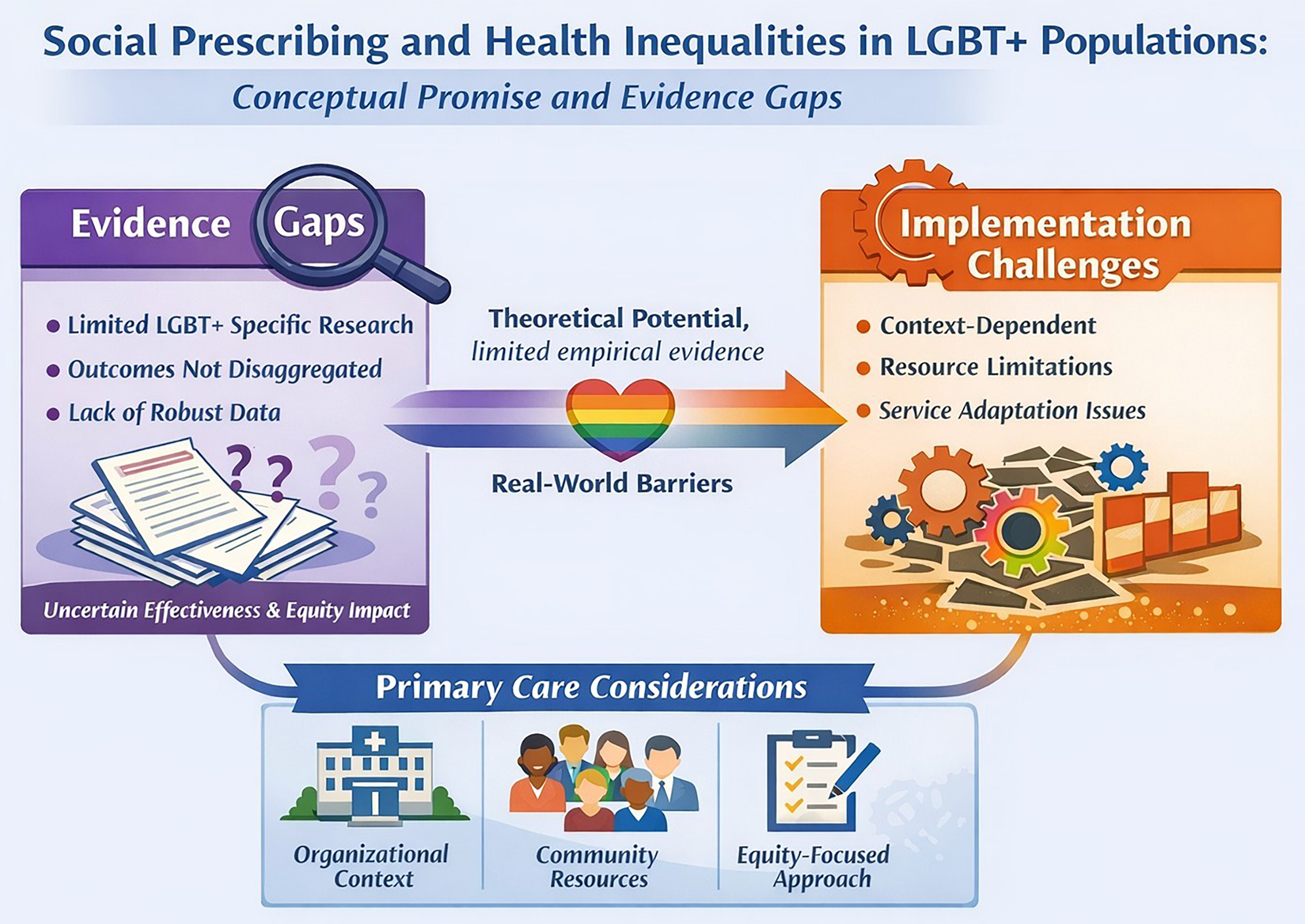
This narrative review aims to synthesize and critically analyze the international literature on SP, with a particular focus on its conceptualization, application, and limitations in the context of LGBT+ health. Figure 1 presents a conceptual framework that situates SP within the context of LGBT+ health determinants and illustrates the gap between its intended mechanisms and the current empirical evidence.
Materials and methods
A narrative review was conducted to synthesize and critically examine the international literature on SP, with particular attention to its conceptualization, application, and limitations in the context of LGBT+ health. Relevant literature was identified through a structured search of MEDLINE (via PubMed), Scopus, and Web of Science. To ensure a broad and inclusive scope, searches were performed using combinations of Medical Subject Headings (MeSH), free-text keywords, and title-based screening. Search terms included variations of “social prescribing,” “community referral,” and “non-medical needs,” combined with terms related to sexual and gender minority health, such as “LGBT,” “LGBT+,” “sexual minority,” and “gender minority.” Title-based screening was used as a complementary strategy to standard database searching to capture conceptual and interdisciplinary contributions that might not be consistently indexed under standardized terminology; this approach was not intended to replace comprehensive database searching but to broaden conceptual coverage. The search covered literature published between January 2000 and December 2025, with the final search conducted in December 2025. Eligible sources included peer-reviewed narrative, systematic, and scoping reviews, conceptual papers, and empirical studies published in English-language international journals. Editorials, commentaries, and non-peer-reviewed materials were generally excluded from the analytic synthesis, although selected editorials were cited to provide contextual background. The included literature was analyzed narratively, with findings synthesized thematically rather than quantitatively. Given the narrative scope of the review and the heterogeneity of the included evidence, no formal appraisal of methodological quality was performed; instead, study limitations and design characteristics were considered in the thematic synthesis.
As this was a narrative review, the literature search was intentionally broad and iterative rather than restricted by predefined inclusion and exclusion criteria. The aim was to capture conceptual, empirical, and practice-oriented contributions relevant to SP and LGBT+ health, rather than to identify a comprehensive or exhaustive set of studies. Sources were selected based on their relevance to the review objectives and their contribution to the thematic synthesis.
Conceptual foundations of social prescribing
Social prescribing is commonly described as an approach that links individuals in contact with healthcare services to non-clinical, community-based resources in order to address non-medical factors influencing health and wellbeing.14, 15, 16 Although the term is widely used, there is no single, universally accepted definition, despite recent international efforts to establish consensus-based conceptual and operational definitions. Across the literature, SP is variably framed as a referral mechanism, a person-centered process, or a system-level strategy aimed at addressing social determinants of health.15, 17 Core elements recurring across definitions include the identification of non-medical needs, connection to community or voluntary sector services, and varying degrees of facilitation or follow-up support, often provided by link workers or care navigators.16, 18, 19
The emergence of SP is closely linked to broader shifts away from exclusively biomedical models of care toward biopsychosocial and preventive approaches.17 The concept gained particular prominence in the UK, where SP has been progressively embedded into primary care policy and practice, before spreading internationally under different terminologies and institutional arrangements.7, 16 While similar practices previously existed in multiple health systems, their consolidation under the label of SP has facilitated policy uptake and academic attention.
Several organizational models of SP have been described in the literature. These range from structured referral pathways involving dedicated link workers with an active community navigation role to less formal models focused primarily on signposting.15, 18 Models also differ with respect to implementation settings, target populations, and intensity of support, reflecting local healthcare structures and available community resources.7, 16 As a result, SP is best understood as a family of related practices rather than a standardized intervention.
Social prescribing has been applied across a broad range of healthcare contexts, most commonly in relation to mental health, long-term conditions, social isolation, and wellbeing.14, 20 However, systematic and narrative reviews consistently highlight substantial heterogeneity in study designs, outcome measures, and reported effects.5, 6, 20 The existing evidence base is therefore characterized by methodological limitations and contextual dependence, underscoring ongoing challenges in evaluating SP and drawing generalizable conclusions.
Social prescribing and non-medical determinants of health
Non-medical needs, commonly framed within the concept of social determinants of health (SDOH), are increasingly recognized as key drivers of health outcomes and healthcare utilization. These needs include factors such as housing instability, food insecurity, social isolation, financial strain, and limited access to community resources, which are frequently encountered in routine clinical practice but are not adequately addressed through biomedical interventions alone.6, 14 Empirical studies conducted in primary care settings demonstrate that a substantial proportion of patients report unmet social needs. At the same time, clinicians often face structural, time-related, and informational barriers to identifying and responding to these issues.21, 22 Unaddressed non-medical needs have been associated with suboptimal treatment adherence, increased healthcare use, and compromised patient safety. Broader evidence also demonstrates that insufficient social relationships are associated with increased mortality, providing a central rationale for the development of system-level approaches such as SP.14, 23, 24
Social prescribing is hypothesized to operate through several interrelated mechanisms that extend beyond referral alone. Qualitative and realist studies consistently highlight the role of connection, whereby engagement with community-based activities reduces social isolation and fosters a sense of belonging.25, 26 Navigation represents a 2nd key mechanism, with link workers supporting individuals in identifying needs, accessing appropriate resources, and negotiating complex service landscapes.26, 27 A further mechanism involves relational support, including trust-building, validation, and sustained engagement, which may enhance motivation, self-efficacy, and capacity for self-management.27, 28 These mechanisms are highly context-dependent and shaped by organizational, relational, and structural conditions.
Social prescribing is most frequently discussed in relation to mental health, particularly psychological distress, anxiety, depression, and reduced wellbeing. Reviews and observational evaluations suggest that SP may be associated with improvements in wellbeing and social connectedness, especially among individuals with mild to moderate symptoms.29, 30 However, the evidence remains heterogeneous, context-dependent, and limited by methodological constraints, with ongoing debate regarding the appropriateness of SP as a response to complex or severe mental health needs.31
Social isolation and complex, multi-domain needs represent key contexts in which SP has been most frequently applied. Empirical studies indicate that individuals experiencing loneliness, multimorbidity, socioeconomic deprivation, or frequent healthcare use often present with intertwined social, psychological, and physical challenges that are poorly addressed within conventional clinical pathways.29, 32, 33
Realist and qualitative evaluations suggest that, for these populations, SP functions less as a brief referral and more as a sustained, relational process requiring tailored, long-term support and cross-sector collaboration.33 Evidence consistently highlights that standard SP models may be insufficient for individuals with complex needs unless adapted to account for structural vulnerability, fragmented services, and limited personal resources.32, 34
LGBT+ health as a contextual framework for social prescribing
Health disparities observed among LGBT+ populations are consistently described in the literature as multidimensional, spanning mental, physical, behavioral, and social domains across the life course.35, 36, 37 Elevated rates of depression, anxiety, loneliness, substance use, and suicidal ideation have been documented, alongside a higher prevalence of selected chronic conditions, including cardiometabolic disease, respiratory conditions, and multimorbidity, particularly among sexual minority adults and older populations.36, 38, 39, 40, 41, 42, 43 These patterns do not reflect a single dominant clinical condition but rather the accumulation and interaction of multiple health challenges.
Significantly, physical and mental health outcomes in LGBT+ populations are closely intertwined with health-related behaviors and social conditions. Studies indicate higher exposure to food insecurity, disordered eating, body dissatisfaction, and sleep disturbances, as well as disparities in health behaviors such as tobacco and alcohol use, which vary across sexual orientation, gender identity, age, and sex.37, 39, 44 Evidence also suggests that multimorbidity in sexual minority adults often co-occurs with mental illness and substance use, contributing to increased healthcare utilization and complex care needs.38, 40
Work-related stressors also constitute a key structural determinant of health among LGBT+ populations. Evidence indicates higher exposure to employment precarity, lower wages, and workplace discrimination, which are associated with poorer mental health outcomes, particularly among transgender individuals.45, 46, 47 Across these domains, social and structural factors emerge as central drivers of health outcomes. Conceptual and empirical work consistently points to the role of stigma, discrimination, minority stress, and socioeconomic disadvantage in shaping health risks, coping strategies, and access to care.13, 35, 37
As a result, health problems experienced by LGBT+ individuals frequently extend beyond isolated or purely biomedical conditions. Instead, they reflect dynamic interactions between psychosocial stressors, behavioral responses, and structural conditions, underscoring the limitations of narrowly focused clinical approaches and the relevance of broader, context-sensitive frameworks when examining potential health system responses.
A growing body of evidence indicates that LGBT+ populations are disproportionately affected by social and structural determinants of health, beyond individual or biomedical factors alone. Population-based studies consistently demonstrate higher exposure to adverse social determinants of health, including housing instability, food insecurity, economic insecurity, social isolation, and medical mistrust, compared with cisgender heterosexual populations.48, 49, 50 These factors have been associated with poorer self-rated health, reduced quality of life, and delayed or forgone healthcare, even after adjustment for sociodemographic characteristics.13, 49
Conceptual and empirical literature further emphasizes the role of structural stigma, defined as societal-level policies, institutional practices, and cultural norms that restrict access to resources and opportunities.13, 51 Narrative and state-of-the-art reviews provide convergent evidence linking structural stigma to adverse mental, behavioral, and physical health outcomes among LGBT+ individuals across diverse sociopolitical contexts.13, 51, 52 Minority stress frameworks describe how these structural conditions interact with interpersonal discrimination and proximal stress processes, producing cumulative health effects over the life course.52, 53
Together, this evidence highlights that unmet social needs and structural barriers represent central drivers of health disparities in LGBT+ populations. These dynamics create a context in which approaches targeting non-medical determinants of health, such as SP, warrant critical examination.
A substantial body of international literature indicates that LGBT+ individuals experience persistent barriers within healthcare systems that extend beyond formal access and are rooted in interpersonal, organizational, and structural processes. Population-based studies from the USA and Europe consistently demonstrate higher rates of delayed care, unmet healthcare needs, and difficulties in identifying a usual source of care among sexual and gender minority populations compared with cisgender heterosexual individuals.54, 55 These disparities are particularly pronounced among bisexual individuals and transgender and nonbinary populations.54, 56
Qualitative and mixed-methods studies further document that negative healthcare experiences frequently involve enacted and anticipated stigma, including misgendering, heteronormative assumptions, dismissal of identity-relevant concerns, and a lack of provider knowledge regarding LGBT+-specific health needs.55, 56, 57, 58, 59, 60 Such encounters contribute to diminished trust in healthcare professionals and increased concealment of sexual orientation or gender identity in clinical settings.55, 61, 62 Fear of discrimination has been shown to influence healthcare-seeking behavior, with some individuals avoiding or postponing care even in the presence of significant health needs.55, 57
Evidence from both general and specialized care contexts suggests that these experiences are not isolated events but reflect broader institutional patterns. Studies highlight the role of insufficient professional training, the absence of inclusive policies, and the lack of visible affirming signals as key contributors to negative patient experiences across healthcare settings.58, 61 Importantly, studies focusing on seriously ill LGBT+ individuals indicate that discriminatory or dismissive care may be particularly consequential in contexts requiring long-term engagement, shared decision-making, and reliance on healthcare systems.57, 63
Collectively, this literature underscores how cumulative interactions among social stigma, professional preparedness, and institutional environments shape healthcare experiences among LGBT+ populations. These dynamics are directly relevant to the analysis of SP, which is increasingly proposed as an approach to addressing unmet needs that emerge at the interface between healthcare systems and patients’ social contexts. Across healthcare settings, LGBT+ populations consistently report unmet health and social needs that extend beyond the scope of conventional biomedical care. Population-based and cross-sectional studies demonstrate a higher prevalence of unmet medical and mental health needs, delayed care, and forgone services among sexual and gender minority individuals, particularly during periods of system strain such as the COVID-19 pandemic64, 65 Notably, emerging evidence suggests that while LGBT+ individuals may experience reduced contact with family members such as parents, siblings, or partners, levels of contact with friends appear comparable to those observed among cisgender heterosexual populations, highlighting important distinctions between structural and functional aspects of social relationships.42 These unmet needs are closely linked to socioeconomic insecurity, limited access to affirming services, and cumulative experiences of stigma. Medical mistrust represents a critical mechanism contributing to unmet needs, especially among individuals with intersecting marginalized identities. Empirical studies indicate that sexual orientation- and gender identity-related medical mistrust is associated with a higher likelihood of unmet care, with intersectional effects observed among LGBT+ people of color.66 Qualitative and mixed-methods research further highlights gaps in continuity of care, a lack of navigation support, and the limited availability of identity-affirming community resources.67, 68
Importantly, unmet needs frequently emerge at the interface between healthcare systems and everyday social contexts, including caregiving responsibilities, social isolation, and reliance on informal or community-based support networks.69, 70 Reviews focusing on older LGBT+ populations emphasize persistent gaps in accessible, inclusive community supports, despite evidence that such resources may mitigate loneliness and psychological distress.68 Together, this literature underscores system-level limitations in addressing non-medical needs, providing a rationale for examining SP as a potential, yet critically contested, response to these gaps.
Taken together, the literature indicates that health challenges experienced by LGBT+ populations are characterized by the co-occurrence of medical, psychological, and social needs that are strongly shaped by structural and contextual factors rather than isolated biomedical conditions. Persistent exposure to stigma, discrimination, unmet social needs, and barriers within healthcare systems creates complex care trajectories that extend beyond the remit of conventional clinical interventions. These characteristics align closely with the problem space that SP is intended to address, namely, the interface between healthcare delivery and the broader social contexts in which health is produced and maintained. Notably, the LGBT+ context highlights both the potential relevance and the inherent limitations of SP. The need for trust, continuity, navigation support, and access to affirming community resources underscores why SP is frequently proposed in this context, while simultaneously raising questions about its feasibility, reach, and equity in structurally constrained environments. As such, LGBT+ health provides an analytically informative setting in which to critically examine how SP is conceptualized, implemented, and bounded within contemporary health systems, rather than constituting a claim about its effectiveness for this population.
Evidence on SP in the context of LGBT+ health
Despite growing interest in SP within health and social care systems, empirical evidence explicitly examining SP in relation to LGBT+ health remains very limited. A systematic query of the peer-reviewed literature did not identify randomized controlled trials (RCTs), comparative effectiveness studies, or large-scale service evaluations explicitly designed for sexual and gender minority populations. What has been published consists predominantly of small exploratory studies, descriptive reports, and broader assessments of SP models that include, but do not disaggregate, outcomes for LGBT+ individuals as part of wider populations with complex needs. A small number of descriptive and qualitative investigations suggest potential areas of relevance where SP may intersect with the experiences of sexual and gender minority groups. For example, nature-based SP interventions with asylum seekers and refugees in the UK were reported to include participants identifying as LGBT+ and to focus on social connection and wellbeing. However, these evaluations did not explicitly assess outcomes stratified by sexual orientation or gender identity.71 Similarly, meta-syntheses of qualitative research on SP to address loneliness and social isolation include samples with LGBT+ representation but do not provide disaggregated analyses for this subgroup.72 Although informative about mechanisms such as connection and navigation, these studies are not designed to yield robust conclusions about the effectiveness or differential impact of SP for LGBT+ populations.
Existing SP evaluations frequently target broader categories of vulnerability (e.g., social isolation, multimorbidity, socioeconomic disadvantage), within which LGBT+ individuals may be implicitly included but are rarely analyzed as a distinct group. Descriptive accounts from primary care initiatives demonstrate that link worker models can engage people with complex social needs, including those related to stigma and discrimination. However, the available evidence does not allow assessment of how such models perform specifically for sexual and gender minority patients. Observational studies of general SP outcomes (e.g., self-reported wellbeing, healthcare utilization) do not typically report subgroup analyses by sexual orientation or gender identity, leaving a marked gap in understanding how LGBT+ status intersects with SP pathways.
Beyond the UK, SP models have also been implemented in other settings; e.g., in Ontario (Canada), SP has been delivered through community health centers explicitly oriented toward health equity and serving vulnerable populations, including LGBT+ communities. In contrast, Australian SP trials report the participation of LGBT+ clients within broader programs.73 In the absence of directly targeted evaluations, examples of real-world SP practice are helpful in contextualizing how services may be adapted or configured to address needs relevant to LGBT+ populations. In the UK, the UK National Health Service (NHS) personalized care policy promotes SP via link workers embedded in primary care networks to address non-medical determinants of health, including loneliness and social needs, among people with long-term conditions.74 Within this framework, local services have developed more tailored models. The Brighton & Hove LGBT Switchboard operates a dedicated SP service for LGBTQIA+ communities, including trans, non-binary, and intersex (TNBI) individuals, connecting participants with community support tailored to identity and lived experience (https://www.switchboard.org.uk). Similarly, the Central Liverpool Primary Care Network (PCN) offers an LGBT+ SP Service providing personalized link worker support and referrals to relevant community activities and resources for adults identifying as LGBT+ or questioning their identity.75 These examples illustrate that SP models can be configured to prioritize sexual and gender minority populations, even though their effects have not been formally evaluated in peer-reviewed research.
Other practice-oriented efforts demonstrate the potential breadth of inclusive SP implementation. Quality improvement programs such as Pride in Practice in the UK integrate community assets and workforce training to enhance affirming care pathways for LGBT+ patients, embedding aspects of community linkage and support that resonate with SP principles. However, they are not labeled or evaluated explicitly as SP interventions in the research literature.76 Similarly, youth-focused SP programs, such as Barnardo’s LINK service, work with community organizations, including LGBT+ groups, to address social isolation and access to safe spaces for young people, indicating avenues through which SP can intersect with identity-affirming community support.77 At the policy and research levels, gaps in evidence have been recognized and are beginning to be addressed.
Collectively, the literature and practice examples reviewed here indicate a substantive gap between the conceptual relevance of SP for LGBT+ health and the availability of robust evidence evaluating its implementation and outcomes. Current research is exploratory and descriptive, often subsuming LGBT+ individuals under broader vulnerability categories without explicit subgroup analysis. Service models demonstrating inclusive or targeted SP approaches exist in practice, but their effects remain untested in rigorous empirical studies. This gap represents a priority area for future research, including well-designed evaluations capable of distinguishing how SP may mitigate non-medical determinants of health for LGBT+ populations and under what conditions such interventions are most effective.
It should be noted that the predominance of UK-based examples in the literature reflects the more advanced institutionalization of SP within the UK healthcare system, rather than a deliberate geographic focus of this review. In other health systems, where SP is less formally embedded or operates under different organizational arrangements, similar principles may be relevant; however, their implementation, scope, and feasibility are likely to vary depending on primary care structures, funding mechanisms, and community capacity.
Limitations, challenges, and critical considerations
The findings of this narrative review should be interpreted in light of several significant limitations and challenges inherent to the existing evidence base. First, empirical research on SP in the context of LGBT+ health is sparse, heterogeneous, and predominantly exploratory. Available studies are primarily qualitative, descriptive, or feasibility-focused, with small sample sizes and limited methodological rigor, precluding causal inference or robust assessment of effectiveness. The absence of RCTs, comparative designs, and long-term follow-up substantially limits conclusions regarding the outcomes, sustainability, and scalability of SP for LGBT+ populations. Second, LGBT+ individuals are frequently subsumed within broader categories of vulnerability without explicit subgroup analysis, obscuring potential differences in needs, experiences, and responses to SP across sexual orientations, gender identities, and intersecting social positions. This lack of disaggregation hampers both interpretability and equity-oriented evaluation. Third, many SP models rely on assumptions of trust, service availability, and community capacity that may not hold in contexts marked by stigma, medical mistrust, or fragmented social infrastructures, raising concerns about uneven access and unintended exclusion. Finally, the implementation of SP is highly context-dependent, shaped by local policy environments, funding structures, and workforce competencies. Without clear standards for inclusive design and reporting, there is a risk that SP initiatives may reproduce existing inequities rather than mitigate them. These considerations underscore the need for cautious interpretation of the current evidence and for more rigorous, inclusive, and context-sensitive research moving forward. These limitations restrict the ability to draw causal conclusions about effectiveness and underscore the need for rigorously designed, equity-focused evaluations that explicitly report outcomes by sexual orientation and gender identity.
Clinical implications and directions for future research
From a clinical, service delivery, and organizational decision-making perspective, the current evidence does not support SP as a standalone solution for addressing health inequities experienced by LGBT+ populations. However, the documented burden of unmet social needs, barriers to care, and medical mistrust suggests that SP may have a complementary role when integrated into broader, affirming, and adequately resourced models of care. Clinicians and health systems considering SP should be attentive to issues of accessibility, trust-building, and the availability of identity-affirming community resources, as well as to the risk of shifting responsibility for structural problems onto community services.
Future research priorities include the development and evaluation of SP models explicitly designed with and for LGBT+ populations, using co-creation approaches and intersectional frameworks. Robust study designs, including comparative and longitudinal assessments, are needed to evaluate not only short-term wellbeing outcomes but also access to care, continuity, and equity-related impacts. Standardized reporting of sexual orientation and gender identity, along with transparent descriptions of implementation contexts, will be essential to advance evidence-informed and inclusive SP practices.78
The Horizon Europe-funded Social Prescribing-EU (SP-EU) project represents one of the first large-scale initiatives to adapt and evaluate the effectiveness of SP for multiple vulnerable populations, explicitly including LGBT+ persons as a target group alongside refugees, first-generation immigrants, and older adults living alone.79 SP-EU combines co-creation, pragmatic randomized trials, and qualitative research to assess the effectiveness of tailored SP models for these groups across multiple European countries. While results are not yet available and therefore are not part of the current empirical synthesis, the project underscores both the recognition of existing evidence gaps and the momentum toward generating robust, context-specific data on SP approaches for sexual and gender minority populations.
From an implementation perspective, the meaningful integration of SP in LGBT+ care contexts is likely to depend on several enabling conditions, including sustainable funding, appropriate professional training in sexual and gender diversity, and the availability of adequately resourced community organizations. Future evaluations would benefit from incorporating measurable implementation indicators, such as uptake and retention among LGBT+ service users, perceived trust and safety, referral completion, and continuity of engagement with community-based resources, alongside health and wellbeing outcomes. Without sustained policy commitment, adequate funding, and inclusive governance structures, there is a risk that SP initiatives may have limited impact on structural drivers of inequality or may unevenly benefit already well-resourced communities. Consistent with wider implementation debates in European primary care, SP should be viewed as a complementary pathway that requires workforce capacity, coordination, and equity-oriented governance to avoid reproducing existing gaps.80
Conclusions
Social prescribing is conceptually aligned with the complex, non-medical determinants of health that shape health inequalities experienced by LGBT+ populations. However, the current evidence base does not support conclusions regarding its effectiveness or equity impact in this context. Empirical studies directly addressing SP for LGBT+ populations are scarce, predominantly descriptive, and methodologically limited, with outcomes rarely disaggregated by sexual orientation or gender identity. Existing service models demonstrate that LGBT+-inclusive SP is feasible in practice, but their effects remain largely unevaluated. Overall, the findings indicate a substantial gap between the theoretical applicability of SP and the availability of robust evidence to inform its implementation for LGBT+ health equity. While practice-based examples suggest feasibility in specific settings, the broader implementation of SP for LGBT+ health equity remains highly context-dependent. The broader implementation of SP for LGBT+ health equity should therefore be approached with caution in the absence of robust evidence on effectiveness and equity impact. For primary care practice, these conclusions emphasize that any consideration of SP should account for organizational context and available community resources.
Use of AI and AI-assisted technologies
The authors declare that generative AI was used in the creation of this manuscript. It was used specifically to assist in translating the manuscript into English, utilizing OpenAI’s ChatGPT. The authors take full responsibility for this use.

















.jpg)