Abstract
Physical activity (PA) significantly influences emotional wellbeing, from enhancing mood to counteracting emotional disorders such as depression and anxiety. This article offers an in-depth analysis of the neurobiological processes and theories underpinning the emotional benefits of PA which arise from exercise-induced physiological changes that simultaneously benefit brain function. We discuss the role of growth factors, neurotransmitters and biochemicals, as well as enhancements in mitochondrial biogenesis and antioxidant activity, and how they foster exercise performance and emotional health. Central to our discussion are theories related to depression: the “neurotrophic,” “neurogenesis,” “inflammation,” “oxidative stress,” and “monoamine” hypotheses. We also introduce the emergent “glutamate hypothesis” and discuss exercise-induced lactate release as a potential precursor for glutamate. Additionally, we explore the “endorphin” and “endocannabinoid” hypotheses, underscoring their implications in evoking feelings of euphoria, pain relief and diminished anxiety after exercise. In conclusion, PA exerts a diverse influence on brain health and emotional wellbeing. The dynamic interplay between PA and neurobiological processes signals a promising avenue for future research, with the potential to introduce innovative therapeutic strategies for emotional disorders.
Key words: neurotrophic hypothesis, neurogenesis hypothesis, glutamate hypothesis, monoamine hypothesis, endocannabinoid hypothesis
Introduction
Numerous studies have demonstrated the positive influence of physical activity (PA) on emotional wellbeing,1, 2, 3, 4 including enhancing mood, vigor5, 6, 7 and resilience,8, 9 and its therapeutic effects on depression10, 11, 12 and anxiety.13, 14 Despite the fact that neurobiological mechanisms underlying these benefits remain a dynamic area of research,9, 15, 16, 17, 18, 19 comprehensive reviews offering a synthesis of existing knowledge are notably absent. Here, we extend our recent work on the cognitive impact of PA20 to provide an exhaustive overview of the neurobiological mechanisms of the affective benefits of PA.
From exercise physiology to brain health
We have demonstrated that bodily adaptations that enhance exercise performance also benefit brain function.20 Specifically, PA triggers the release of biochemicals, including growth factors such as brain-derived neurotrophic factor (BDNF), insulin-like growth factor-1 (IGF-1), vascular endothelial-derived growth factor (VEGF), lactate, interleukin 6 (IL-6), and neurotransmitters such as dopamine and serotonin (5-HT). Additionally, PA facilitates mitochondrial biogenesis and bolsters antioxidant enzyme activity. These adaptations facilitate lipid and carbohydrate metabolism, and enhance tissue and blood vessel growth and repair, leading to optimized energy production. Both dopamine and 5-HT play vital roles in motor control, and together with growth factors, mitochondrial biogenesis and antioxidant enzyme activity, help mitigate central fatigue. Collectively, these adaptations bolster endurance and exercise performance.
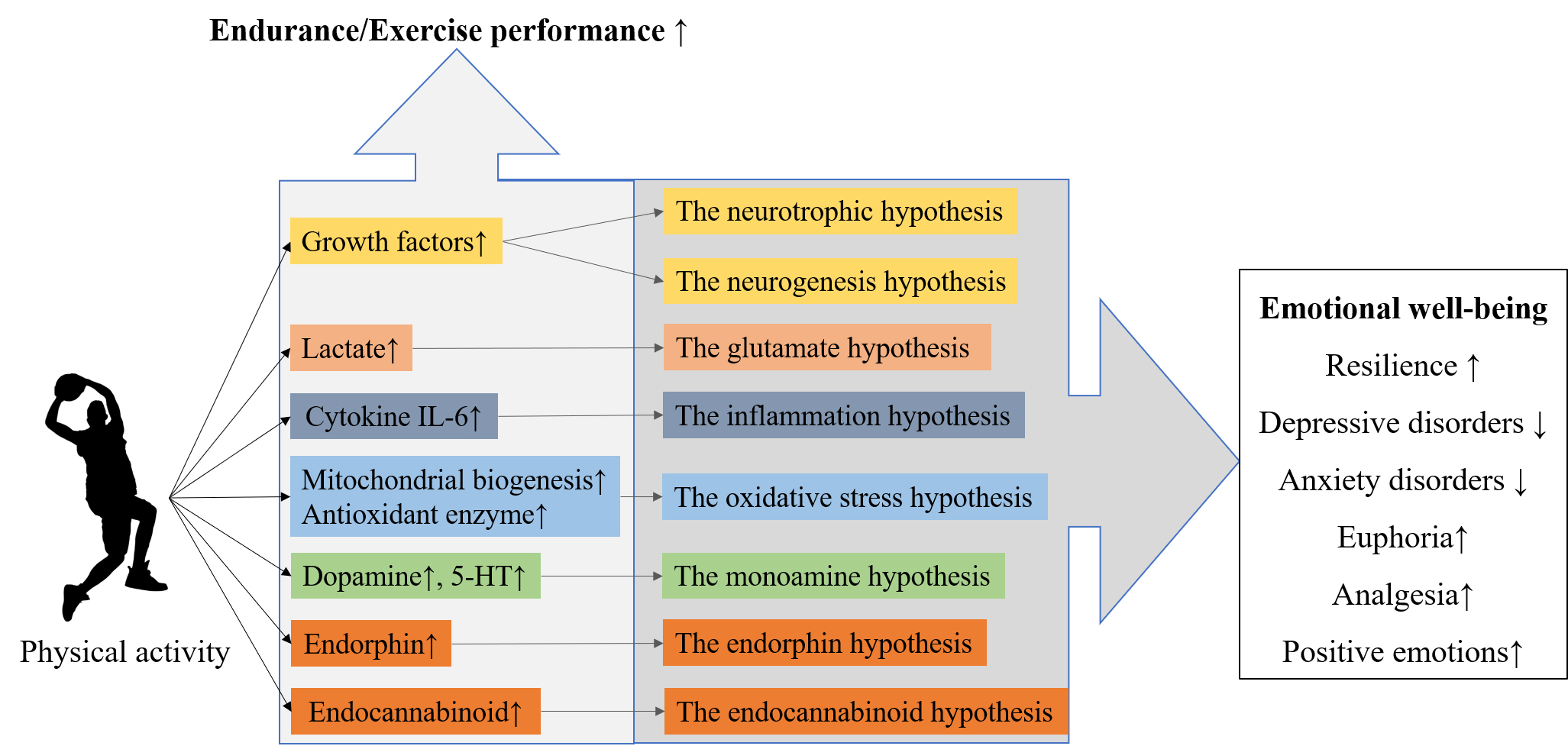
Interestingly, physiological adaptations also confer brain benefits (Figure 1). Growth factors cross the blood–brain barrier (BBB) and function as nutrients for neurons and blood vessels, facilitating enhanced angiogenesis and adult hippocampal neurogenesis, and increasing cerebral blood volume, dendritic spines, brain volume, and long-term potentiation (LTP). Lactate crosses the BBB and acts as an energy source for neurons and a precursor for the predominant excitatory neurotransmitter, glutamate, thereby augmenting LTP. Interleukin 6 activates IL-1 receptor antagonist and IL-10, which initiate anti-inflammatory actions, including reduced production of IL-1β, IL-8 and tumor necrosis factor alpha (TNF-α). Enhanced mitochondrial biogenesis and antioxidant enzyme activity decrease reactive oxygen species (ROS) production and oxidative stress. While chronic inflammation and oxidative stress impair the BBB, causing neuroinflammation, microglia activation and neuronal damage, PA protects against these effects (see Chen and Nakagawa20 for details).
The multifaceted role of physical activity in boosting resilience and alleviating depression
Remarkably, physiological adaptations to PA play a significant role in promoting emotional wellbeing. The so-called “neurotrophic hypothesis”21, 22 and “neurogenesis hypothesis”23, 24 have established the crucial role of growth factors and adult hippocampal neurogenesis in resilience and depression. Essentially, both neurogenesis and growth factors diminish under chronic stress and depression, yet are restored or rejuvenated by antidepressants and PA. Moreover, growth factors are essential for adult neurogenesis, which mediates pattern separation, thus contributing to cognitive flexibility and resilience.25, 26 Growth factors also enhance the growth of dendritic spines, the primary locations for synaptic inputs to neurons. As such, PA increases dendritic spine density in the hippocampus and the prefrontal cortex (PFC).27, 28 In tandem, the “inflammation hypothesis”29, 30, 31 and the “oxidative stress hypothesis”32, 33 have garnered considerable interest. Chronic stress triggers inflammation and oxidative stress that contribute to depressive and anxiety disorders. Antidepressant treatment and PA, however, reduce these effects. A potential mediator of PA-enhanced mitochondrial biogenesis is the peroxisome proliferator-activated receptor gamma coactivator 1-alpha (PGC-1α),34 which further regulates the kynurenine pathway, another mechanism through which PA reduces depression.35, 36, 37
Regarding neurotransmission, the “monoamine hypothesis,” which proposes that antidepressants act on serotonin, noradrenaline and dopamine, has been a dominant theory for over half a century.38 It posits that depression involves the depletion of these monoamines, and that agents increasing them alleviate depression. However, it does not explain the latency in depressive symptom relief,39 prompting the emergence of the “glutamate hypothesis.”40 The alterations in glutamate and its metabolites identified in various brain regions of depressed patients, along with the rapid antidepressant effects of ketamine (a glutamate N-methyl-D-aspartate (NMDA) receptor antagonist), provide compelling evidence for this hypothesis. Notably, ketamine induces transient activation of glutamate neurotransmission in the PFC via gamma-aminobutyric acid (GABA) interneuron disinhibition, followed by a sustained increase in PFC synaptic connectivity.41, 42
Physical activity not only boosts the release of dopamine and serotonin in the brain, but also increases the levels of lactate crossing the BBB, which serves as a glutamate precursor.20, 43 As per our previous work, voluntary wheel running increased prefrontal dopamine in rats,15 which aligns with the functional role of prefrontal dopamine in working memory, with PA linked to heightened cognitive flexibility6, 44, 45 and resilience.15, 46 Physical activity also raises dopamine levels in the midbrain and striatum,47, 48 which encode reward prediction errors and fuel action vigor.49, 50, 51 Using similar and relevant mechanisms,52, 53, 54 PA helps reduce anxiety, a condition commonly co-occurring with depression.55, 56, 57, 58
Physical activity, endorphins, endocannabinoids, and positive emotions
Alongside the aforementioned mechanisms, the body also releases endorphins (a term derived from “endogenous” and “morphine”) and endocannabinoids (an endogenous cannabinoid) during PA. Endorphins facilitate lipid and carbohydrate metabolism, while endocannabinoids promote vasodilation and bronchodilation, enhancing oxygen supply to muscles. These biochemicals augment exercise performance and deliver affective benefits, as captured in the “endorphin hypothesis”59, 60 and the “endocannabinoid hypothesis.”61
The “endorphin hypothesis” was the initial theory to elucidate the phenomenon of “runner’s high” or feelings of euphoria, pleasantness and analgesia after PA. Research has illustrated a strong correlation between changes in β-endorphin plasma concentrations after PA and shifts in feelings of pleasantness (Rho = 0.738, p < 0.001).62 This hypothesis, however, has faced criticism since β-endorphin cannot cross the BBB to activate the μ-opioid receptors responsible for euphoria.63 Despite this, subsequent research implies that PA may directly augment opioid binding in prefrontal/orbitofrontal cortices and the anterior cingulate cortex, thereby eliciting euphoria.64
The “endocannabinoid hypothesis” is an alternative theory that has garnered increasing attention, as peripheral endocannabinoids cross the BBB, activate cannabinoid receptors, and evoke feelings of euphoria and reduced anxiety.65 The PA-induced changes in anandamide, a particular endocannabinoid, correlate with shifts in positive emotions (r = 0.96, p < 0.0001).66 Moreover, genetic ablation of cannabinoid receptors on GABAergic neurons eliminates PA-induced anxiolysis, while pharmacological inhibition of central and peripheral cannabinoid receptors blocks analgesia in mice.67
Conclusions
The complex interactions between PA and the neurobiological mechanisms of affective benefits offer a rich, multifaceted field of study. Our comprehensive overview provides a robust framework for further research, one that may hold the key to developing novel therapeutic approaches for the treatment of emotional disorders and the promotion of emotional wellbeing.