Abstract
Background. Renal steatosis is an abnormal accumulation of fat in the kidney and may cause chronic kidney disease (CKD) or CKD progression.
Objectives. This pilot study aimed to evaluate the quantitative measurability of the parenchymal distribution of lipid deposition in the renal cortex and medulla using chemical shift magnetic resonance imaging (MRI) and investigate its relationship with clinical stages in CKD patients.
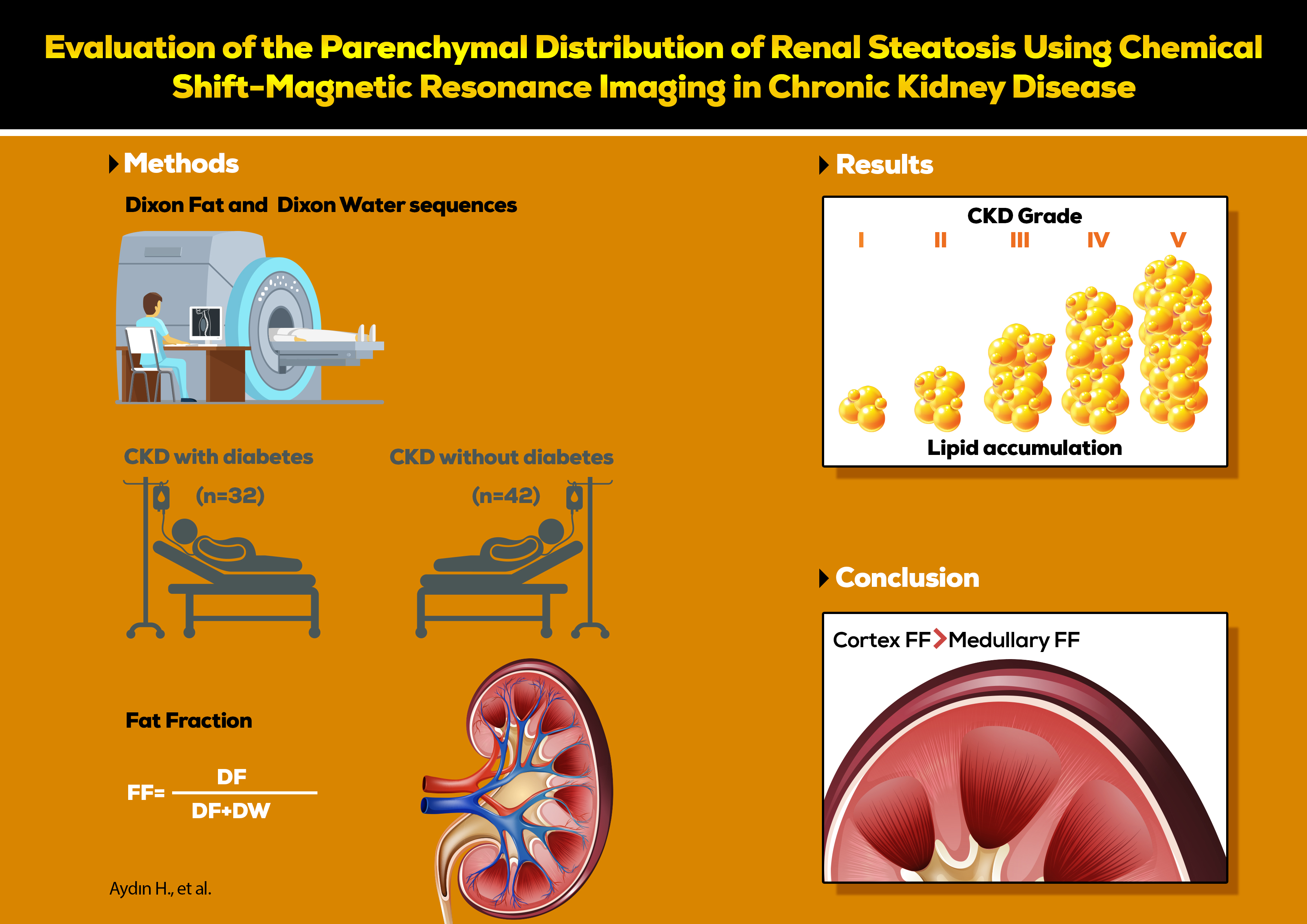
Materials and methods. The study groups included CKD patients with diabetes (CKD-d) (n = 42), CKD patients without diabetes (CKD-nd) (n = 31) and control subjects (n = 15), all of whom underwent a 1.5T MRI of the abdomen using the Dixon two-point method. The fat fraction (FF) values in the renal cortex and medulla were calculated from measurements made on Dixon sequences, and then compared between the groups.
Results. The cortical FF value was higher than the medullary FF value in control (0.057 (0.053–0.064) compared to 0.045 (0.039–0.052)), CKD-nd (0.066 (0.059–0.071) compared to 0.063 (0.054–0.071)), and CKD-d (0.081 (0.071–0.091) compared to 0.069 (0.061–0.077)) groups (all p < 0.001). The CKD-d group cortical FF values were higher than those of the CKD-nd group (p < 0.001). The FF values began increasing at CKD stages 2 and 3, and reached statistical significance at stages 4 and 5 in CKD patients (p < 0.001).
Conclusions. Renal parenchymal lipid deposition can be quantified separately in the cortex and medulla using chemical shift MRI. Fat accumulation occurred in cortical and medullary parenchyma in CKD patients, though predominantly in the cortex. This accumulation increased proportionally with the disease stage.
Key words: magnetic resonance imaging, chemical shift imaging, chronic kidney disease, renal steatosis, fatty kidney disease
Background
Renal steatosis is an abnormal accumulation of intracellular triglycerides/lipids in the kidney, which may cause the development and/or progression of chronic kidney disease (CKD).1, 2, 3 Fatty acids accumulate as intracellular droplets and cause the release of toxic cytokines, resulting in interstitial fibrosis and loss of kidney function.4, 5, 6 Inspired by non-alcoholic fatty liver disease (NAFLD), the term “fatty kidney disease (FKD)” has been used recently in the literature.6 In this regard, the effects of intra-abdominal, perirenal and parenchymal fat deposits on the kidneys are evaluated, as well as the relationships between FKD and insulin resistance, type 2 diabetes, obesity, metabolic syndrome, hyperlipidemia, hypertension, NAFLD, and cardiovascular disorders.6, 7, 8
To evaluate renal steatosis, parenchymal lipid accumulation must be quantitatively measured. The gold standard renal steatosis assessment method is a biopsy followed by quantitative enzymatic measurement of triglycerides and qualitative oil red O staining. However, these methods are invasive and can increase the risk of complications.9 Non-invasive lipid measurement is also possible using fatty tissue-sensitive chemical shift magnetic resonance imaging (MRI).10, 11, 12 Chemical shift imaging is an MRI technique for detecting small areas (voxels) that contain water and fat protons. In this technique, the difference in resonance between water and oil protons is used to obtain images, with images taken from the in-phase (IP) and out-of-phase (OP) times of water and fat protons. In voxels containing both water and fat, signal loss occurs in OP images, though voxels containing only fat or water protons have no signal difference between the OP and IP images.13 With the simple addition and subtraction of the 2 images, 1 image containing only water and 1 containing only fat can be obtained. The Dixon technique can be generally used for the suppression or quantification of fat in various types of pulse sequences and allows for the measurement of the fat–water fraction in a precise region of interest (ROI) with higher spatial resolution.14, 15 A few molecular imaging studies have recently evaluated lipid accumulation in the kidneys.7, 11, 12, 15, 16, 17 However, no study has separately evaluated lipid deposition in the cortical and medullary components of the parenchyma.
Objectives
This pilot study evaluated the quantitative measurability of cortical and medullary parenchymal lipid deposition in CKD patients using chemical shift MRI.
Materials and methods
The study was carried out as a retrospective archive search. It was conducted in accordance with the Declaration of Helsinki after obtaining approval from the Clinical Research Local Ethics Committee of the Faculty of Medicine of Suleyman Demirel University (Isparta, Turkey; decision No. 14/210 issues on July 27, 2020).
Study setting and participants
Study subjects were selected randomly from patients registered in the picture archiving and communication system (PACS) of our hospital, who were treated and followed up with a diagnosis of CKD and/or diabetes between 2016 and 2020, and those who had an upper abdominal MRI examination for any reason. In total, 117 CKD patients followed up in the Department of Nephrology were considered eligible for the study. Patients younger than 18 years (n = 2) or with malignancy (n = 2), polycystic or multicystic kidney disease (n = 5), renal transplantation (n = 2), or chronic liver disease (n = 9) were excluded from the study. Patients were also excluded if they had insufficient data in PACS (n = 13) or artifacts on MRI that prevented measurement (n = 11). The remaining 73 CKD patients were divided into 2 subgroups based on the presence or absence of diabetes, including CKD patients with diabetes (CKD-d) (n = 31) and CKD patients without diabetes (CKD-nd) (n = 42). The presence of diabetes was determined using the patient’s history registered in the hospital PACS, the use of oral antidiabetic/insulin, or daily urine albumin level greater than 30 mg.18 The clinical staging of CKD was assigned according to the estimated glomerular filtration rate (eGFR),19 which was calculated using the CKD Epidemiology Collaboration (CKD-EPI) method.20 The control group (n = 15) consisted of patients who underwent upper abdomen MRI for any reason other than kidney disease (such as liver hemangioma and gallbladder pathologies) and who, according to PACS data, did not have urinary disease, diabetes, malignancy, connective tissue disease, or chronic systemic disease. The final evaluation included 176 kidneys of 88 patients – 73 in the CKD group and 15 in the control group. All measurements required for fat fraction (FF) calculation from the renal cortical and medullary parenchyma were performed by a single radiologist (the corresponding author) with 10 years of abdominal MRI experience.
MRI examination parameters
Magnetic resonance imaging scans were obtained using a 1.5 Tesla unit (Magnetom Avanto; Siemens Medical Solutions, Erlangen, Germany) and a 16-channel body coil with the patient in supine position without sedation. Images were acquired as axial and coronal plane turbo spin-echo T2-weighted (TSE T2W) without fat saturation and breath-hold, and gradient-echo sequence fat saturated T1 volumetric interpolated breath-hold examination (VIBE), based on the Dixon two-point method and taken as IP and OP to detect intracellular lipid. The version of the VIBE-Dixon sequence applied in this study was a generic version rather than the modified quantitative Dixon sequence, so that IP, OP, water, fat, proton density fat fraction (PDFF), and T2* maps could be calculated. The chemical shift MRI examination parameters are presented in Table 1.
Evaluation of images and measurements
All images were evaluated using OsiriX MD v.10.0.2 software (General Public License (GPL) licensed free to access resource code and commercially licensed with US. Food and Drug Administration (FDA) approval; UCLA, Pixmeo, Bernex, Switzerland) on a MacOS-X radiology workstation (Apple Inc., Cupertino, USA). The measurements were performed by a single radiologist with 10 years of abdominal MRI experience. The intra-observer agreement values for measurements were found to be 0.918 (for cortical FF) and 0.956 (for medullary FF). Slices were evaluated on T2W images to exclude artifacts, space-occupying lesions or vascular pathologies. Measurements in the axial plane were made on Dixon Fat (DF) and Dixon Water (DW) sequences from the most appropriate single slice passing through the renal hilus level without any space-occupying lesions.
The ROI used for measurement in the DW sequence was placed using the copy–paste method in the same parenchymal location of the corresponding slice in the DF sequence so that the measurements were from the same location on both sequences, with the same ROI. Three measurements were taken using a 20-mm2 circular ROI from the areas where the cortex and medulla meet, and then the average was calculated for analysis (Figure 1). Renal FF values were calculated using the formula below13:
FF = [DF/(DF + DW)].
The sample size was found to be sufficient as a result of power analysis performed using the GPower 3.1.9.2 software (Kiel University, Kiel, Germany). The selected test family included F tests and fixed effects one-way analysis of variance (ANOVA). The effect size was calculated as d = 0.80 using the measurements from the pilot study. The Type-I error rate and the power were considered 5% and 0.95, respectively. Therefore, the total sample size was determined as n = 32.
Statistical analyses
The statistical analyses employed IBM Stastistical Package for Social Sciences (SPSS) v. 20.0 (IBM Corp., Armonk, USA) software. The continuous variables were expressed as mean with 95% confidence intervals (95% CIs), and the categorical variables as frequency (percentage (%)). The Shapiro–Wilk test assessed the normality of continuous variables. For comparisons between 2 independent groups, Student’s t-test was applied with Welch robust correction test if the variances were not equal. One-way ANOVA with the Tamhane post hoc test was used for multiple groups since the variances were not homogenous, and the Brown–Forsythe robust correction test was applied to meet the assumptions of homogeneity. The receiver operating characteristic (ROC) analysis was performed, and the diagnostic ratios for sensitivity and specificity for cortical and medullary measurements were calculated. The intra-observer agreement was calculated using interclass correlation (ICC) with two-way mixed and average single-measure methods. There were no missing data in the dataset. A value of p < 0.05 was considered statistically significant.
Results
The evaluations included 176 kidneys of 88 adults (53.3% males, 46.7% females). The mean patient age was 59.28 ±13.05 years in the CKD group and 55.41 ±14.41 years in the control group (p = 0.001). Gender did not affect the FF values (p > 0.05).
The cortical FF values were significantly higher than the medullary FF in all groups (p < 0.001) (Table 2). In the CKD-d patients, a significant increase was observed in the cortical FF values compared to the control subjects (p < 0.001). The medullary FF values in both CKD groups increased, but the values were significantly higher in the CKD-d group than in the control group (p < 0.001). However, in contrast to the CKD-d group, the elevated cortical and medullary FF values in the CKD-nd group had no statistical significance compared to the control group (p > 0.05).
The cortical and medullary FF measurements in the CKD groups, based on the CKD stages, are presented in Figure 2, Figure 3, Figure 4. There was no significant difference between the control group (healthy kidneys) and the CKD groups at stage 1 for cortical and medullary FF values (p > 0.05). When all CKD patients were considered as a single group, there was no significant difference between stage 1 and 2 cortical FF values. A statistically significant difference was determined in the cortical and medullary FF values at stage 2 compared to stage 5 values (cortex, p = 0.021; medulla, p = 0.003). In addition, there was a significant difference between stage 3 and stage 5 for medulla values (p = 0.037) (Figure 2). In the CKD-d group, the cortical and medullary FF values increased with the clinical stage and reached statistical significance between stages 2 and 5 (p = 0.037 and p = 0.041, respectively) (Figure 3). The cortical and medullary FF values in the CKD-nd group were similar to those of the CKD-d group, with statistical significance between stages 2 and 5 (cortex, p = 0.047; medulla, p = 0.040) (Figure 4).
The ROC analysis showed a significant difference between the control and CKD-d patient groups with respect to the area under the curve (AUC) values for both cortical and medullary FF. The cutoff value of 0.076 for cortical FF had a sensitivity of 96.7%, while the cutoff value of 0.056 for medullary FF had better diagnostic ratios, as shown in Table 3.
The results of normality and homogeneity of variance assumptions with related tests are presented in Supplementary Table 1 (https://doi.org/10.5281/zenodo.7961812).
Discussion
This study demonstrated for the first time the separate quantitative evaluation of parenchymal lipid deposition in the cortex and medulla and its relationship with the clinical stages of CKD using a radiological imaging method. We found that fat accumulation occurs in the cortex and medulla in CKD patients, predominantly in the cortex, and is positively correlated with the clinical stages of CKD. The importance of lipid accumulation in the cortex relative to the medulla in the early stages of diabetes demonstrated using MRI was consistent with the biopsy findings, suggesting that this technique is valid for measuring cortical and medullary lipid accumulation in the kidney. Previous histopathological studies have shown that parenchymal intracellular lipid deposition in CKD mainly occurs in the parts of the renal cortex containing the glomerulus and proximal tubules.21, 22 Magnetic resonance imaging studies have demonstrated the presence of very little renal parenchymal lipid in healthy volunteers and an increase in the amount of lipid in the kidney parenchyma (without cortex/medulla distinction) in diabetic patients.11, 17, 23 However, as far as we know, an MRI study on the distribution of parenchymal lipid deposition in the cortex and medullary components in CKD patients, as well as on its relationship with clinical stages, has not yet been performed.
Cortical and medullary lipid depositions differed according to the CKD stage.24, 25 At stage 1 CKD, there was no significant increase in the amount of parenchymal lipid, and the cortical and medullary lipid distributions were similar to those of the control group. In CKD patients, parenchymal lipids increased from stage 2 and reached a statistically significant level at stages 4 and 5. Although there was no statistical significance at stages 2 and 3, the FF increase was greater in the cortex than in the medulla. There was no significant difference between the cortex and medulla in lipid accumulation at stages 4 and 5, which suggests that parenchymal lipid accumulation is diffuse in advanced CKD. The detection of different amounts of lipid accumulation in parenchymal components in different clinical stages suggests that this novel technique presents a new area of research for experimental clinical and drug studies. If the technique proves useful, it can be applied free of charge to patients undergoing MRI for any reason, since chemical shift sequences are routinely obtained during abdominal MRI scans. In this regard, prospective multicenter studies can be conducted with larger patient groups to determine cutoff values according to the clinical stages of CKD and test inter-observer and intra-observer reliability.
Renal lipid accumulation may develop independently of hyperglyceridemia.6 In the CKD-nd group, cortical and medullary FF values increased in parallel with the increase in the clinical stage, but no statistical significance was identified (Table 2). The possible reason for this discrepancy may be the lower number of stage 4 and 5 CKD patients in this group compared to those at stages 1 and 2.
The relationship between diabetes and renal parenchymal lipid accumulation is not clear. Some studies have reported that diabetes does not have a significant relationship with renal lipid accumulation.22, 24 In contrast, other studies have reported a significant increase of renal lipid content in diabetes patients.11, 17, 23 Yokoo et al. conducted a study using 3T MRI, with measurements taken from an ROI through the whole parenchyma, and reported that the renal parenchyma FF rate (2.38%) was high in diabetes patients, independently of serum creatinine, body mass index (BMI) and Hb-A1c, and concluded that steatosis was an independent risk factor.11 In the present study, the increase in FF values in CKD-d group was higher than in the CKD-nd group, and the cortical and medullary FF values increased in parallel with the increasing stage. This finding suggests that diabetes could have a triggering effect on lipid accumulation in patients with CKD. However, it would not be correct to make a conclusion regarding the impact of diabetes on renal steatosis based on the results of the current study. Indeed, this study only focused on measuring FF in the renal cortex and medulla in CKD, and there was no evaluation of other risk factors that may affect renal steatoses, such as diabetes severity and duration, concomitant hypertension, metabolic syndrome, or obesity.
Inspired by the concept of NAFLD, the term FKD has recently been proposed to express the local and systemic effects of ectopic fat accumulation. Within this concept, the renal effects of intra-abdominal, perirenal and parenchymal fat depositions are evaluated (albuminuria, CKD, and podocyte toxicity).7 Thus, as for NAFLD, it has been reported that renal steatosis can be treated as a separate disease or can be a part of a more extended metabolic disorder.6, 7 Such a distinction is important for clinical purposes, and targeting metabolic disorders as a whole may also impact kidney structure and function. In this regard, it is crucial to evaluate if the medications for NAFLD can also decrease kidney lipid accumulation.8 Moreover, it is clinically important to investigate the relative impact of cortical or medullary lipid accumulation. As this pilot study primarily aimed to measure fat accumulation quantitatively in the cortex and medulla but not to investigate the clinical significance of cortical and medullary fat accumulation, future studies are needed to highlight these issues. However, in contrast to NAFLD, in which fat accumulation is clearly evident, lipid accumulation in the kidney is scarce and sensitive techniques may be necessary to evaluate trace amounts of fat deposition, which may be clinically important.
Multiparametric renal MRI biomarkers have been developed and proposed for evaluating renal inflammation, oxidative stress, hypoxia, and fibrosis.26, 27 However, a standard radiological approach that will contribute to the definition of FKD has not yet been developed.7 The present study showed that the addition of quantitative parenchymal FF measurements using chemical shift renal MRI could contribute to FKD understanding and development, though more studies are required to highlight the clinical importance of our findings.
Limitations
This study had several limitations. Selection bias is inherent to the retrospective design of the study. Although biopsy is the gold standard, it was not performed to measure the amount of fat in the renal parenchyma. However, the chemical shift MRI technique, which is accepted for assessing lipids in the liver, was used for the noninvasive measurement of the amount of renal parenchymal lipids. The diagnosis and staging of CKD were defined according to eGFR, though there is an increasing recognition that eGFR alone may not be specific to CKD, and the Kidney Disease: Improving Global Outcomes (KDIGO) recommendations suggest adding proteinuria to the classification.26 Moreover, the study focused on quantifying fat accumulation in the renal cortex and medulla in patients with CKD and evaluating its relationship with the clinical stage. However, it may be interesting to investigate the relationship between renal parenchymal steatosis and parameters such as obesity, hypertension, metabolic syndrome, uric acid, insulin resistance, triglycerides, fasting blood glucose, and hemoglobin A1C (HbA1c) using this method. Also, the reliability of the measurements could not be evaluated, as they were made by a single observer. However, the measurements were reliable since the cortex and medulla are clearly distinguished in Dixon Water images, measurements are made from the same section and region with the cut–copy–paste technique, and the number and size of the measurements are standard.
Conclusions
Results of this study demonstrated that fat accumulation occurred in both the cortex and medulla, predominantly in the cortex of CKD patients, and correlated positively with the clinical stages of CKD. As such, FF measurements using chemical shift MRI could be used as a radiological criterion for developing the FKD concept, since even very small cortical and medullary lipid deposits can be measured quantitatively. However, to validate these findings, there is a need for prospective multicenter trials with larger patient groups to determine cutoff values and test intra-observer and inter-observer reliabilities according to the clinical stages of CKD.
Supplementary data
The supplementary materials are available at https://doi.org/10.5281/zenodo.7961812. The package contains the following files:
Supplementary Table 1. The results of normality and variance homogeneity assumptions.