Abstract
Taurodontism is a morphological anomaly involving multirooted teeth that is characterized by a vertical shift of the pulp chamber and shortening of the roots. The literature was analyzed to determine the impact of a diagnosis of taurodontism on dental treatment. A total of 85 full-text publications from the years 2005–2021 were analyzed and 20 publications were included in this research. The endodontic treatment of a taurodont tooth is challenging due to the apical displacement of the pulpal chamber floor and the incorrect configuration of the root canal system, or the presence of additional canals. In terms of prosthetics, the use of taurodont teeth as abutments is not recommended as they lack stability due to shorter roots. The extraction of taurodont teeth can be complicated due to an apical shift of the root furcation. In periodontology, taurodont teeth can have a better prognosis as there is less chance of furcation involvement. From an orthodontic point of view, it is important to note that taurodont teeth are not sufficiently embedded in the alveolus and have a greater tendency for root resorption. With regard to genetic diseases, it has been reported that this anomaly can exist as an isolated feature. However, the majority of authors agree that taurodontism is associated with conditions such as Down syndrome, Klinefelter syndrome, cleft lip and palate, hypodontia, amelogenesis imperfecta, and others. From a clinical standpoint, it is very important to diagnose taurodontism before treatment. A diagnosis of taurodontism can be important in the early diagnosis of malformations that commonly occur with this condition.
Key words: genetic diseases, endodontics, dental pulp cavity, tooth cervix
Introduction
Taurodontism is a morphological anomaly involving multirooted teeth. It can affect both deciduous and permanent teeth.1, 2, 3 Taurodontism most commonly affects the permanent molars of the mandible.4 However, some authors contend that this anomaly is found more frequently in the maxilla and second molars, and is less frequently seen in the first molars of the mandible.3 Taurodontism can occur unilaterally or bilaterally.
A taurodont tooth is characterized by an apical displacement of the pulpal floor and shortening of the roots. A lack of constriction at the cementoenamel junction (CEJ) is a characteristic feature.3 On clinical examination, a taurodont tooth is not visibly different from the other teeth, as this anomaly is only detected on radiographic imaging.
The origin of the name “taurodontism” comes from the Latin term “taurus” which means bull and the Greek term “odous” which means tooth.3 Taurodontism was first observed by Henry Pickerill in 1909.3, 5, 6 The name of the condition was coined by Arthur Keith in 1913.2, 3, 4, 5, 6, 7, 8, 9 Since its identification, de Terra has discovered these misshaped teeth in prehistoric humans.8 There are reports stating that the term “taurodontism” was first used by Dragutin Gorjanović-Kramberger who found this anomaly in neanderthal remains in Krapina (Croatia).3 In modern populations, the prevalence of taurodontism varies depending on the population studied. This condition has been observed in 8% of Jordanians, 46% of Chinese, 5% of Israelis, and 10% of the Dutch.10 However, it should be considered that the aforementioned differences may result from the use of different diagnostic criteria.11
The etiology of this condition has not been clearly explained. Many authors assume that the anomaly forms in early fetal life due to the failure of Hertwig’s epithelial sheath diaphragm to invaginate at the proper horizontal level.1, 3, 5, 7, 11, 12, 13, 14 Some authors report that this anomaly may be associated with an aberration of a gene on the X chromosome that is responsible for enamel development,3, 4, 15 or that it may be inherited in an autosomal dominant fashion.4
Objectives
The objective of this study was to analyze the available publications in order to assess the impact of the presence of taurodontism on various aspects of dental treatment (endodontology, prosthetics, surgery, periodontology, and orthodontics) and the association of taurodontism with various malformations.
Material and methods
The PubMed database was searched covering the years 2005–2021, and the keyword “taurodontism” was used. This resulted in identifying 243 publications, of which 158 were rejected after an analysis of the abstracts. The exclusion criteria included a lack of relation to the topic, non-English text and nonavailability of the abstract and article. A total of 85 full-text articles were analyzed. The inclusion criteria consisted of the subject of the article evaluating the impact of taurodontism on endodontic, prosthetics, dental surgery, periodontological and orthodontic treatment, or describing the association of taurodontism with other malformations. Full-text articles were excluded if they were not relevant to the subject of this work. Sixty-five articles were rejected and 20 were included in this research (Figure 1). Particular attention was paid to the clinical relevance of the cases described. The conclusions of the authors were categorized into endodontics, prosthetics, dental surgery, periodontology, and orthodontics. We analyzed the points of view of the authors concerning the coexistence of taurodontism and other genetic diseases and systemic disorders.
Results
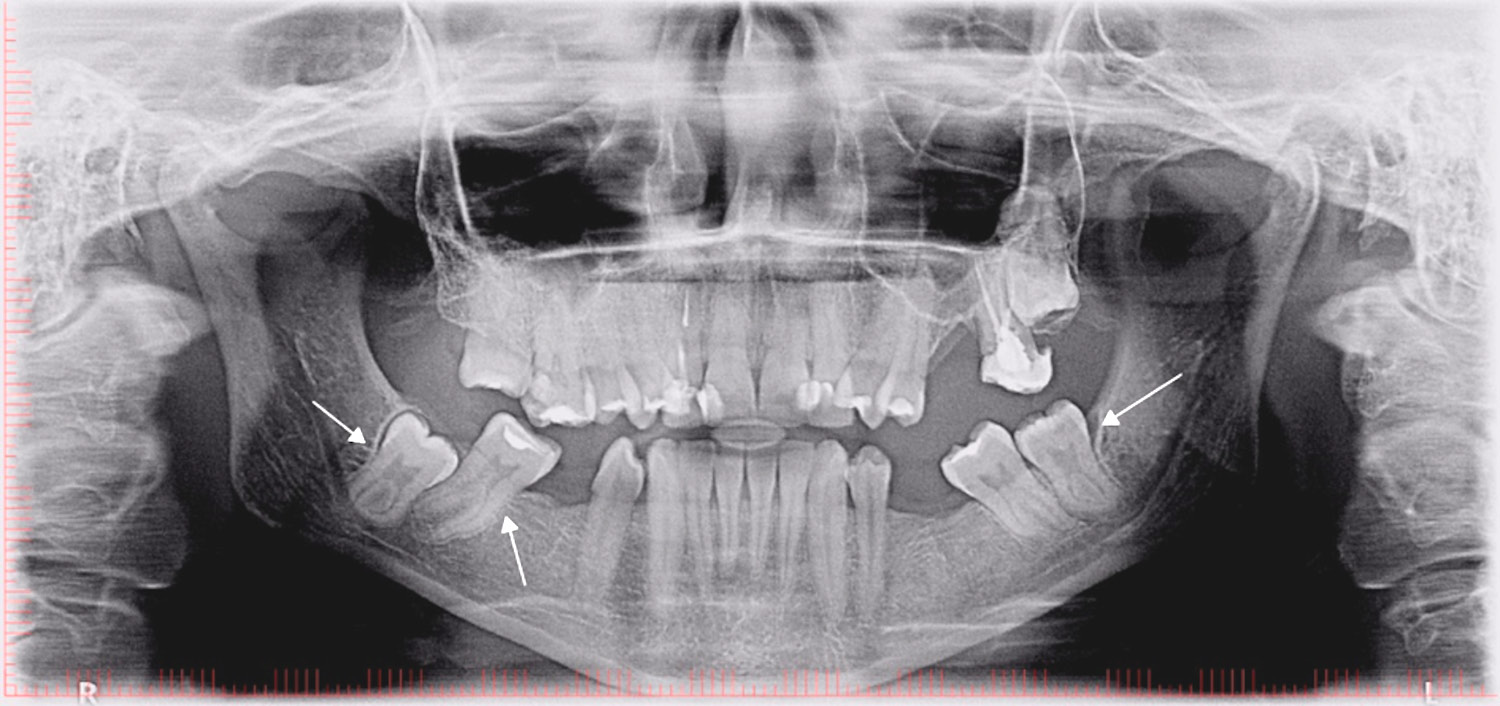
The endodontic treatment of taurodont teeth is complex and difficult because of the apical displacements of the pulpal chamber floor, which makes it harder to find the localization of the root canals.5, 6, 11, 15, 16 Taurodont teeth often have an incorrect configuration of the root canal system and additional canals (Figure 2, Figure 3). Increased bleeding during pulp chamber trepanation may be mistaken for perforation1; however, due to root shortening and the apical displacement of the pulpal chamber, floor perforations can occur.3, 12, 17 The complexity of the root canal system makes its instrumentation almost impossible. Because of this, the authors recommend the use of sodium hypochlorite to dissolve the remaining pulp that cannot be removed with instruments.13, 18 Kulkarni et al. described a case of a patient who underwent root canal irrigation of tooth 37 with 2.5% sodium hypochlorite, 17% aqueous ethylene diamine tetra-acetic acid (EDTA) solution, 2% chlorhexidine gluconate, and saline.4 According to Bharti et al., an irrigation with 5% sodium hypochlorite for 20 min–2 h can completely dissolve the pulp.19 However, Prakash et al. recommended the irrigation with sodium hypochlorite be limited to single-use to minimize the detrimental effects in the periapical tissues.8
From an endodontist’s standpoint, it is very helpful to use an endodontic magnifier and endodontic microscope during the treatment of taurodont teeth.19 By using these modern optical devices, the operating field is better illuminated and the picture becomes deeper and clearer. The endodontic microscope provides up to ×40 magnification of the operating field, which significantly minimizes the risk of complications when finding hard-to-reach root canal orifices. The use of an endodontic microscope also makes it possible to check the dryness, cleanliness and shape of the root canals. An additional challenge during endodontic treatment is the difficult procedure of root canal filling. Mohan et al. proposed a modified technique of root canal filling, based on connecting the side condensation of the apical area with the vertical condensation of the extended pulp chamber.2, 19 As a result of the vertical shift of the pulp chamber, the diagnosis of a taurodont tooth may be difficult, as the pulp viability test may not be conclusive.3
Taurodont teeth are less useful as abutments in prosthetic treatment because the shortened roots do not provide adequate anchorage in the alveolus and, therefore, do not adequately resist lateral forces.3, 5, 16 According to some authors, taurodont teeth are a contraindication for the use of root-crown posts.12
With regard to dental surgery, it should be taken into account that the extraction of a taurodont tooth may be more difficult because of the apical shift of the furcation, the root apical area being shorter and thinner,5, 16 and the roots having a widened dimension in the 1/3 of their length (Figure 2).3, 5, 17 Paradoxically, due to their large crown and short roots, such teeth are less seated in the alveolus, and thus may be easier to extract than their cynodont counterparts.1, 2, 15
In periodontal treatment, taurodont teeth appear to have a better prognosis than cynodont teeth, as the probability of involvement of the furcation in taurodont teeth is significantly smaller.5, 15, 16 However, if this does occur, then the prognosis becomes questionable.16
A diagnosis of taurodontism is important before making decisions about orthodontic treatment. Due to the reduced surface area of the roots, it may be necessary to reduce the anchorage value of the root in the alveolus.3, 16 From the point of view of an orthodontist, it is very important to know the link between the occurrence of facial and dental malformations. During orthodontic treatment, taurodont teeth may have an excessive tendency for root resorption.14
The opinions of researchers are divided on the question of whether taurodontism coexists with other genetic diseases. Some authors report that taurodontism is an anomaly that may be observed as an isolated feature,15 or as a coexisting feature with other genetic diseases such as tricho-dento-osseus syndrome and Klinefelter syndrome.7, 16, 17, 18 There are reports stating that taurodontism occurs more frequently in people with a cleft lip and palate.3, 7, 10, 11 Also, correlations with disorders such as hypodontia, amelogenesis imperfecta and Down syndrome have been observed.1, 2, 3, 9, 10, 13, 19 The authors agree with the hypothesis that the prevalence of taurodontism increases as the number of X chromosomes increases, indicating that the expression of the defect and the number of X chromosomes may be correlated. Furthermore, it has been suggested that the X chromosomal gene responsible for the development of enamel may also be responsible for the development of taurodontism.15 Puttalingaiah et al. studied patients from central India and were able to prove a correlation between taurodontism and tooth agenesis.20 In the population studied, they noted a prevalence of 7.5% for this association. Chetty et al. investigated and described a relationship between the occurrence of taurodontism and the existence of genetic abnormalities in the bone structure of a South African population.17 They found that out of 23 people with osteogenesis imperfecta (OI) type XI, 43.48% showed signs of taurodontism in their permanent teeth. Contrary to this, a study of the Danish population has shown taurodontism to only occur in persons with mild OI. Taurodontism has also been diagnosed in association with Torg–Winchester syndrome and Pyle disease.17
The prevalence of this dental anomaly reported in the literature is variable due to the use of different study methods. Studies in the literature report values ranging from 0.1% to 55% of the total number of patients examined, including values of 0.1% to 9.9% in patients without known systemic diseases. The proportion of patients with systemic diseases and congenital malformations (Down syndrome, Klinefelter syndrome, oligodontia, or cleft lip and palate) diagnosed with taurodontism was high (from 19.4% to 55%).3
Discussion
Taurodontism is a relatively rare tooth anomaly in modern humans.3, 16 However, there are studies showing that this malformation can occur in 0.25–11.3% of the population.11 Most of the authors of the analyzed publications agree that the occurrence of this defect is related to ethnicity.2, 3, 5, 6, 7, 9, 10, 16 For example, this anomaly has been reported in up to 46% of young Chinese people.3, 10 Even using panoramic radiographs and cone beam computed tomography (CBCT), the occurrence of this anomaly, especially its milder forms (hypotaurodontism), can be overlooked. Therefore, a thorough biometric analysis of the available images is very important.7, 12, 15, 16
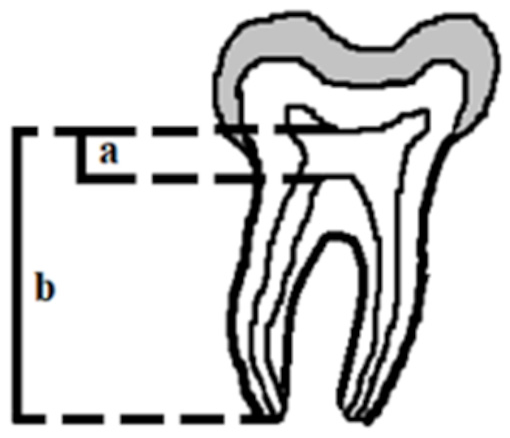
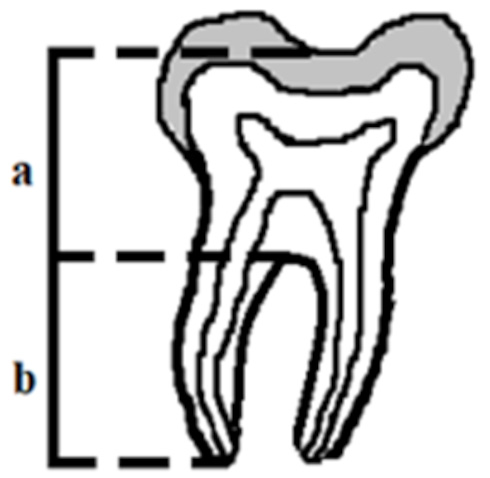
There are several ways to diagnose taurodontism. In 1928, Shaw classified the subtypes of this disease as hypo-, meso- and hypertaurodontism, based on the relative shift of the pulpal floor. This subjective assessment has often led to a misdiagnosis of this anomaly.4 In 1978, Shifman and Chanannel (Figure 4), and later Kim Seow and Lai (Figure 5), developed taurodontal indices in order to determine the occurrence of taurodontism and classify it based on a biometric study, as shown radiographically (Figure 2, Figure 3).3 Determining taurodontism consists of dividing the distance between the lowest point of the pulp chamber roof and the highest point of the pulpal floor by the distance between the lowest point of the pulp chamber roof and the apex, and then multiplying the result by 100. When this value is equal to or greater than 20, the patient is said to have a taurodont tooth. Values from 20 to 29.9 classify the tooth as a hypotaurodont, values from 30 to 39.9 classify it as a mesotaurodont, and values from 40 to 75 identify it as a hypertaurodont. The 2nd index used to identify taurodontism calculates the crown-to-root ratio of the tooth. This is accomplished by measuring the distance from the deeper furrow on the occlusal surface of the furcation and comparing it to the distance from the furcation to the apex. A result from 1.1 to 1.29 indicates hypotaurodontism, from 1.3 to 2.0 indicates mesotaurodontism and above 2.0 indicates hypertaurodontism.3, 13
The ability to diagnose taurodontism is particularly useful in endodontics, especially regarding meso- and hypertaurodont teeth. The treatment of such teeth is very complicated and requires much more commitment from the clinician.11, 18 Due to the considerable elongation of the pulp chamber and consequently, the shortening of the root canals, it is much more difficult to localize and avoid perforation. However, it is possible to observe increased hemorrhaging during trepanation, which can suggest a perforation.13
Conclusions
The literature suggests that from the clinician’s point of view, the diagnosis of taurodontism before treatment is crucial for its success. The complications of endodontic treatment are mostly caused by this defect; however, the possibility of this anomaly should be considered in other areas of dentistry. The diagnosis of taurodontism is important in the early diagnosis of some malformations with which it may be correlated. Therefore, the clinical usefulness of an imaging examination in patients at risk of developing systemic genetic diseases due to medical family history should be emphasized. Genetic testing should be performed in cases where the clinician suspects a genetic disease and where taurodontism has been confirmed, especially in Klinefelter syndrome where it may be asymptomatic at first; however, the risk of tumors development is increased in the case of initially asymptomatic Klineferter syndrome.